Abstract
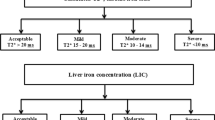
In the present study, we sought to determine the prevalence of iron overload in patients with non-transfusion-dependent thalassemia (NTDT) and its association with genotype and other clinical risk factors, and to evaluate the correlation between serum ferritin (SF) and liver iron concentration (LIC). Myocardial and liver iron concentration was measured by MRI using a T2* gradient multi-echo sequence in NTDT patients, aged 10–50 years. Of 91 patients, 54 (59 %) had hepatic iron overload. None had cardiac iron overload. The clinical risk factors for hepatic iron overload were age >20 years (adjusted OR 30.2, 95 % CI 4.5–203, p < 0.001), hemoglobin level <7 g/dL (adjusted OR 6.3, 95 % CI 1.01–39.5, p = 0.049), and cumulative RBC transfusion >10 units (adjusted OR 53.6, 95 % CI 3.2–884, p = 0.005). Beta-thalassemia genotype was associated with higher risk of iron overload by univariate analysis, but the association was not significant when adjusted for other clinical factors. The correlation coefficient between SF and LIC was 0.60 (p < 0.001). In conclusion, the prevalence of hepatic iron overload is high in NTDT. Older age, lower hemoglobin level, and higher cumulative RBC transfusion are significant risk factors. SF and LIC show a significant positive correlation.

Similar content being viewed by others
References
Weatherall DJ. The definition and epidemiology of non-transfusion-dependent thalassemia. Blood Rev. 2012;26(Suppl 1):S3–6.
Taher A, Vichinsky E, Musallam K, Cappellini MD. Viprakasit V. In: Weatherall D, editor. Guidelines for the management of non transfusion dependent thalassaemia (NTDT). Nicosia: Team up Creations; 2013.
Taher AT, Musallam KM, Karimi M, El-Beshlawy A, Belhoul K, Daar S, Saned MS, El-Chafic AH, Fasulo MR, Cappellini MD. Overview on practices in thalassemia intermedia management aiming for lowering complication rates across a region of endemicity: the OPTIMAL CARE study. Blood. 2010;115:1886–92.
Musallam KM, Cappellini MD, Wood JC, Taher AT. Iron overload in non-transfusion-dependent thalassemia: a clinical perspective. Blood Rev. 2012;26(Suppl 1):S16–9.
Taher AT, Viprakasit V, Musallam KM, Cappellini MD. Treating iron overload in patients with non-transfusion-dependent thalassemia. Am J Hematol. 2013;88:409–15.
Taher AT, Musallam KM, Cappellini MD, Weatherall DJ. Optimal management of beta thalassaemia intermedia. Br J Haematol. 2011;152:512–23.
Tanno T, Miller JL. Iron loading and overloading due to ineffective erythropoiesis. Adv Hematol. 2010;2010:358283. doi:10.1155/2010/358283.
Origa R, Galanello R, Ganz T, Giagu N, Maccioni L, Faa G, Nemeth E. Liver iron concentrations and urinary hepcidin in beta-thalassemia. Haematologica. 2007;92:583–8.
Lemmens-Zygulska M, Eigel A, Helbig B, Sanguansermsri T, Horst J, Flatz G. Prevalence of alpha-thalassemias in northern Thailand. Hum Genet. 1996;98:345–7.
Teawtrakul N, Ungprasert P, Pussadhamma B, Prayalaw P, Fucharoen S, Jetsrisuparb A, et al. Effect of genotype on pulmonary hypertension risk in patients with thalassemia. Eur J Haematol. 2014;92:429–34.
Angelucci E, Brittenham GM, McLaren CE, Ripalti M, Baronciani D, Giardini C, Polchi P, Lucarelli G. Hepatic iron concentration and total body iron stores in thalassemia major. N Engl J Med. 2000;343:327–31.
Taher AT, Porter JB, Viprakasit V, Kattamis A, Chuncharunee S, Sutcharitchan P, et al. Defining serum ferritin thresholds to predict clinically relevant liver iron concentrations for guiding deferasirox therapy when MRI is unavailable in patients with non-transfusion-dependent thalassaemia. Br J Haematol. 2015;168:284–90.
Taher A, El Rassi F, Isma’eel H, Koussa S, Inati A, Cappellini MD. Correlation of liver iron concentration determined by R2 magnetic resonance imaging with serum ferritin in patients with thalassemia intermedia. Haematologica. 2008;93:1584–6.
Pakbaz Z, Fischer R, Fung E, Nielsen P, Harmatz P, Vichinsky E. Serum ferritin underestimates liver iron concentration in transfusion independent thalassemia patients as compared to regularly transfused thalassemia and sickle cell patients. Pediatr Blood Cancer. 2007;49:329–32.
Inthawong K, Charoenkwan P, Silvilairat S, Tantiworawit A, Phrommintikul A, Choeyprasert W, Natesirinilkul R, Siwasomboon C, Visrutaratna P, Srichairatanakool S, Chattipakorn N, Sanguansermsri T. Pulmonary hypertension in non-transfusion-dependent thalassemia: correlation with clinical parameters, liver iron concentration, and non-transferrin-bound iron. Hematology. 2015;20:610–7.
Taher AT, Porter J, Viprakasit V, Kattamis A, Chuncharunee S, Sutcharitchan P, et al. Deferasirox reduces iron overload significantly in nontransfusion-dependent thalassemia: 1-year results from a prospective, randomized, double-blind, placebo-controlled study. Blood. 2012;120:970–7.
Musallam KM, Cappellini MD, Wood JC, Motta I, Graziadei G, Tamim H, Taher AT. Elevated liver iron concentration is a marker of increased morbidity in patients with β thalassemia intermedia. Haematologica. 2011;96:1605–12.
Mavrogeni S, Gotsis E, Ladis V, Berdousis E, Verganelakis D, Toulas P, Cokkinos DV. Magnetic resonance evaluation of liver and myocardial iron deposition in thalassemia intermedia and b-thalassemia major. Int J Cardiovasc Imaging. 2008;24:849–54.
Taher AT, Musallam KM, Wood JC, Cappellini MD. Magnetic resonance evaluation of hepatic and myocardial iron deposition in transfusion-independent thalassemia intermedia compared to regularly transfused thalassemia major patients. Am J Hematol. 2010;85:288–90.
Chen FE, Ooi C, Ha SY, Cheung BM, Todd D, Liang R, Chan TK, Chan V. Genetic and clinical features of hemoglobin H disease in Chinese patients. N Engl J Med. 2000;343:544–50.
Taher AT, Musallam KM, El-Beshlawy A, Karimi M, Daar S, Belhoul K, Saned MS, Graziadei G, Cappellini MD. Age-related complications in treatment-naive patients with thalassaemia intermedia. Br J Haematol. 2010;150:486–9.
Mishra AK, Tiwari A. Iron overload in beta thalassaemia major and intermedia patients. Maedica (Buchar). 2013;8:328–32.
Musallam KM, Taher AT, Duca L, Cesaretti C, Halawi R, Cappellini MD. Levels of growth differentiation factor-15 are high and correlate with clinical severity in transfusion-independent patients with beta thalassemia intermedia. Blood Cells Mol Dis. 2011;47:232–4.
Fiorelli G, Fargion S, Piperno A, Battafarano N, Cappellini MD. Iron metabolism in thalassemia intermedia. Haematologica. 1990;75(Suppl 5):89–95.
Musallam KM, Rivella S, Vichinsky E, Rachmilewitz EA. Non-transfusion-dependent thalassemias. Haematologica. 2013;98:833–44.
Adamkiewicz TV, Abboud MR, Paley C, Olivieri N, Kirby-Allen M, Vichinsky E, et al. Serum ferritin level changes in children with sickle cell disease on chronic blood transfusion are nonlinear and are associated with iron load and liver injury. Blood. 2009;114:4632–8.
Acknowledgments
This work was supported by Diamond Research Grant, Faculty of Medicine, Chiang Mai University, Chiang Mai, Thailand (DM 2555). The authors are grateful to Ms Antika Wongthanee, Bio-statistician, for her assistance with statistical analysis, and Ms Suwakon Wongjaikam for her technical assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This work was supported by a Diamond Research Grant, Faculty of Medicine, Chiang Mai University, Chiang Mai, Thailand (DM 2555).
Conflict of interest
The authors report no conflict of interest.
About this article
Cite this article
Tantiworawit, A., Charoenkwan, P., Hantrakool, S. et al. Iron overload in non-transfusion-dependent thalassemia: association with genotype and clinical risk factors. Int J Hematol 103, 643–648 (2016). https://doi.org/10.1007/s12185-016-1991-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12185-016-1991-5