Abstract
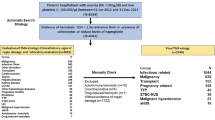
A second questionnaire survey of Japanese patients with thrombotic microangiopathy (TMA) was carried out to investigate the frequency, laboratory abnormalities and outcome in 2004 and 2005. The first and second surveys evaluated 397 patients including 19 with familial TMA and 378 with acquired TMA. The patients with acquired TMA included 165 with Escherichia coli O-157 infection-related TMA (O-157 TMA), 70 with ADAMTS13-related TMA (ADAMTS13 TMA) and 38 with other types of TMA (other TMA). The rate of ADAMTS13 TMA was significantly higher in patients with collagen diseases than in patients with all other underlying diseases (p < 0.001). The treatment of acquired TMA included plasma exchange (PE), steroids, antiplatelet agents, and anticoagulants, PE was carried out in 91.4% of patients with ADAMTS13 TMA, 68.4% of patients with other TMA and 12.7% of patients with O-157 TMA. The efficacy of PE and steroid therapy tended to be higher in patients with ADAMTS13 TMA than in those with other TMA. The complete remission rate was the highest and the mortality rate was the lowest in the patients with O-157 TMA. The mortality rate tended to be lower in patients with ADAMTS13 TMA than in those with other TMA. However, not all of the patients in our study were examined for ADAMTS13 at the time that this questionnaire survey was conducted.

Similar content being viewed by others
References
Moake JL. Thrombotic microangiopathies. N Engl J Med. 2002;347:589–600.
George JN, Vessely SK, Terrell DR. The Oklahoma thrombotic thrombocytopenic purpura—Hemolytic Uremic Syndrome (TTP-HUS) Registry: a community perspective of patients with clinically diagnosed TTP-HUS. Semin Hematol. 2004;41:60–7.
Amorosi EL, Ultman JE. Thrombotic thrombocytopenic purpura: report of the 16 cases and review of the literature. Medicine. 1966;45:139–59.
Matsumoto M, Yagi H, Ishizashi H, Wada H, Fujimura Y. The Japanese Experience with thrombotic thrombocytopenic purpura—hemolytic uremic syndrome. Semin Hematol. 2004;41:68–74.
Pereira A, Mazzara R, Monteagudo J, Sanz C, Puig L, Martínez A, Ordinas A, Castillo R. Thrombotic thrombocytopenic purpura/hemolytic uremic syndrome: a multivariate analysis of factors predicting the response to plasma exchange. Ann Hematol. 1995;70:319–23.
Moake JL, Rudy CK, Troll JH, Weinstein MJ, Colannino NM, Azocar J, Seder RH, Hong SL, Deykin D. Unusually large plasma factor VIII: von Willebrand factor multimers in chronic relapsing thrombotic thrombocytopenic purpura. N Engl J Med. 1982;307:1432–5.
Chow TW, Turner NA, Chintagumpala M, McPherson PD, Nolasco LH, Rice L, Hellums JD, Moake JL. Increased von Willebrand factor binding to platelets in single episode and recurrent types of thrombotic thrombocytopenic purpura. Am J Hematol. 1998;57:293–302.
Asada Y, Sumiyoshi A, Hayashi T, Suzumiya J, Kaketani K. Immunohistochemistry of vascular lesion in thrombotic thrombocytopenic purpura, with special reference to factor VIII related antigen. Thromb Res. 1985;38:469–79.
Soejima K, Mimura N, Hirashima M, Maeda H, Hamamoto T, Nakagaki T, Nozaki C. A novel human metalloprotease synthesized in the liver and secreted into the blood: possibly, the von Willebrand factor-cleaving protease? J Biochem. 2001;130:475–80.
Levy GG, Nichols WC, Lian EC, Foroud T, McClintick JN, McGee BM, Yang AY, Siemieniak DR, Stark KR, Gruppo R, Sarode R, Shurin SB, Chandrasekaran V, Stabler SP, Sabio H, Bouhassira EE, Upshaw JD Jr, Ginsburg D, Tsai HM. Mutations in a member of the ADAMTS gene family cause thrombotic thrombocytopenic purpura. Nature. 2001;413:488–94.
Zheng X, Chung D, Takayama TK, Majerus EM, Sadler JE, Fujikawa K. Structure of von Willebrand factor-cleaving protease (ADAMTS13), a metalloprotease involved in thrombotic thrombocytopenic purpura. J Biol Chem. 2001;276:41059–63.
Furlan M, Robles R, Lamie B. Partial purification and characterization of a protease from human plasma cleaving von Willebrand factor to fragments produced by in vivo proteolysis. Blood. 1996;87:4223–34.
Tsai H-M. Physiologic cleavage of von Willebrand factor by a plasma protease is depend on its conformation and requires calcium ion. Blood. 1996;87:4235–44.
Rock G. The management of thrombotic thrombocytopenic purpura in 2005. Semin Thromb Hemost. 2005;31:709–16.
Ozkalemkas F, Ali R, Ozkocaman V, Ozcelik T, Ozkan A, Tunali A. Therapeutic plasma exchange plus corticosteroid for the treatment of the thrombotic thrombocytopenic purpura: a single institutional experience in the southern Marmara region of Turkey. Transfus Apher Sci. 2007;36:109–15.
Brunskill SJ, Tusold A, Benjamin S, Stanworth SJ, Murphy MF. A systematic review of randomized controlled trials for plasma exchange in the treatment of thrombotic thrombocytopenic purpura. Transfus Med. 2007;17:17–35.
Allford SL, Hunt BJ, Rose P, Machin SJ. Haemostasis and Thrombosis Task Force, British Committee for Standards in Haematology: Guidelines on the diagnosis and management of the thrombotic microangiopathic haemolytic anaemias. Br J Haematol. 2003;120:556–73.
Sugita M, Izumo T, Tamakoshi A, Nagai M, Inaba Y, Kurosawa M, Ikeda Y, Murata M, Fujimura Y, Miyata T, Wada H. Nationwide epidemiological survey of patients with thrombotic thrombocytopenic purpura (TTP) and hemolytic uremic syndrome (HUS). In: Nagai M, editor. 2006 Annual Report of Research on Measures for Intractable Diseases. Japan: The Ministry of Health, Labour and Welfare of Japan; 2007.
Ito N, Wada H, Matsumoto M, Fujimura Y, Murata M, Izuno T, Sugita M, Ikeda Y. National questionnaire survey of TMA. Int J Hematol. 2009;90:328–35.
Kokame K, Nobe Y, Kokubo Y, Okayama A, Miyata T. FRETS-VWF73, a first fluorogenic substrate for ADAMTS13 assay. Br J Haematol. 2005;129:93–100.
Kato S, Matsumoto M, Matsuyama T, Isonishi A, Hiura H, Fujimura Y. Novel monoclonal antibody-based enzyme immunoassay for determining plasma levels of ADAMTS13 activity. Transfusion. 2006;46(8):1444–52.
Rock GA. Management of thrombocytopenic purpura. Br J Haematol. 2000;109:496–507.
Lian EC. Pathogenesis of thrombotic thrombocytopenic purpura: ADAMTS13 deficiency and beyond. Semin Thromb Hemost. 2005;31:625–32.
Thompson CE, Damon LE, Ries CA, Linker CA. Thrombotic microangiopathies in the 1980s: clinical features, response to treatment, and the impact of the human immunodeficiency virus epidemic. Blood. 1992;80:1890–5.
Coppo P, Bengoufa D, Veyradier A, Wolf M, Bussel A, Millot GA, Malot S, Heshmati F, Mira JP, Boulanger E, Galicier L, Durey-Dragon MA, Fremeaux-Bacchi V, Ramakers M, Pruna A, Bordessoule D, Gouilleux V, Scrobohaci ML, Vernant JP, Moreau D, Azoulay E, Schlemmer B, Guillevin L, Lassoued K. Severe ADAMTS13 deficiency in adult idiopathic thrombotic microangiopathies defines a subset of patients characterized by various autoimmune manifestations, lower platelet count, and mild renal involvement. Medicine (Baltimore). 2004;83:233–44.
Rock GA, Shumak KH, Buskard NA, Blanchette VS, Kelton JG, Nair RC, Spasoff RA. Comparison of plasma exchange with plasma infusion in the treatment of thrombotic thrombocytopenic purpura. Canadian Apheresis Study Group. N Engl J Med. 1991;325:393–7.
Hattori A, Tatewaki W, Japan TTP Research Group. Treatment of TTP—retrospective analysis on Japanese patients and review. Jpn J Clin Med. 1993;51:178–83.
Verbeke L, Delforge M, Dierickx D. Current insight into thrombotic thrombocytopenic purpura. Blood Coagul Fibrinolysis. 2009 [Epub ahead of print].
Mori Y, Wada H, Tamaki S, Minami N, Shiku H, Ihara T, Omine M, Kakisita E. Outcome of thrombotic thrombocytopenic purpura and hemolytic uremic syndrome in Japan. Clin Appl Thromb Hemost. 1999;5:110–2.
Acknowledgments
This work was supported in part by a Grant-in-Aid for Blood Coagulation Abnormalities from the Ministry of Health, Labor and Welfare of Japan.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Ito-Habe, N., Wada, H., Matsumoto, M. et al. A second national questionnaire survey of TMA. Int J Hematol 92, 68–75 (2010). https://doi.org/10.1007/s12185-010-0599-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12185-010-0599-4