Abstract
Background
Adolescents with type 1 diabetes experience stress related to treatment management, feeling different from peers, and deciding to tell others about their diabetes.
Purpose
This study examined the relationship of stress reactivity and coping with self-management, quality of life, and metabolic control in an ethnically diverse sample of adolescents with type 1 diabetes.
Methods
Adolescents (n = 327) completed measures of coping and stress reactivity, self-management, and quality of life. Glycosylated hemoglobin data were collected from medical records.
Results
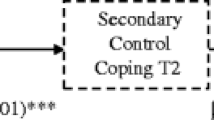
Low-income and minority status were related to lower levels of primary control coping (e.g., problem solving) and secondary control coping (e.g., acceptance), and higher levels of disengagement coping (e.g., avoidance). Self-management mediated the relationship between coping and stress reactivity with quality of life and metabolic control. Race/ethnicity and income moderated the relationship between coping and self-management goals.
Conclusions
Results indicate differences in coping related to income and race/ethnicity and demonstrate the impact of coping on self-management and health outcomes in adolescents with type 1 diabetes.

Similar content being viewed by others
References
Liese AD. The burden of diabetes mellitus among US youth: Prevalence estimates from the SEARCH for Diabetes in Youth Study. Pediatrics. 2006; 118:1510–8.
ADA. Standards of medical care in diabetes - 2010. Diabetes Care. 2010; 33:S11–S61.
Greening L, Stoppelbein L, Konishi C, Jordan SS, Moll G. Child routines and youths’ adherence to treatment for type 1 diabetes. J Pediatr Psychol. 2007; 32:437–47.
Davidson M, Penney EA, Muller B, Grey M. Stressors and self-care challenges faced by adolescents living with type 1 diabetes. Appl Nurs Res. 2004; 17:72–80.
Malik JA, Koot HM. Explaining the adjustment of adolescents with type 1 diabetes: Role of diabetes-specific and psychosocial factors. Diabetes Care. 2009; 32:774–9.
Hanson CL, Henggeler SW, Burghen GA. Social competence and parental support as mediators of the link between stress and metabolic control in adolescents with insulin-dependent diabetes mellitus. J Consult Clin Psych. 1987; 55:529–33.
Compas BE, Connor-Smith JK, Saltzman H, Thomsen AH, Wadsworth ME. Coping with stress during childhood and adolescence: Progress, problems, and potential in theory and research. Psychol Bull. 2001; 127:87–127.
Graue M, Wentzel-Larsen T, Bru E, Hanestad BR, Sovik O. The coping styles of adolescents with type 1 diabetes are associated with degree of metabolic control. Diabetes Care. 2004; 27:1313–7.
Jacobson AM, Hauser ST, Lavori P, Wofsdorf JI, Herskowitz RD, Milley JE, et al. Adherence among children with insulin-dependent diabetes mellitus over a four-year longitudinal follow-up: I. The influence of patient coping and adjustment. J Pediatr Psychol. 1990; 15:511–26.
Delamater AM, Kurtz SM, Bubb J, White NH, Santiago JV. Stress and coping in relation to metabolic control of adolescents with type 1 diabetes. J Dev Behav Pediatr. 1987; 8:136–40.
Grey M, Cameron ME, Thurber FW. Coping and adaptation in children with diabetes. Nurs Res. 1991; 40:144–9.
Reid GJ, Dubow EF, Carey TC. Developmental and situational differences in coping among children and adolescents with diabetes. J Appl Dev Psychol. 1995; 16:529–54.
Reid GJ, Dubow EF, Carey TC, Dura JR. Contribution of coping to medical adjustment and treatment responsibility among children and adolescents wtih diabetes. Dev Behav Pediatr. 1994; 15:327–35.
Band EB, Weisz JR. Developmental differences in primary and secondary control coping and adjustment to juvenile diabetes. J Clin Child Psychol. 1990; 19:150–8.
Hanson CL, Cigrang JA, Harris MA, Carle DL, Relyea G, Burghen GA. Coping styles in youth with insulin-dependent diabetes mellitus. J Consult Clin Psychol. 1989; 57:644–51.
Wiebe DJ, Berg CA, Korbel C, Palmer DL, Beveridge RM, Upchurch R, et al. Children’s appraisals of maternal involvement in coping with diabetes: Enhancing our understanding of adherence, metabolic control, and quality of life across adolescence. J Pediatr Psychol. 2005; 30:167–78.
Hood KK, Peterson CM, Rohan JM, Drotar D. Association between adherence and glycemic control in pediatric type 1 diabetes: A meta-analysis. Pediatrics. 2010; 124:1171–9.
Gallegos-Macias AR, Macias SR, Kaufman E, Skipper B, Kalishman N. Relationship between glycemic control, ethnicity and socioeconomic status in Hispanic and white non-Hispanic youths with type 1 diabetes mellitus. Pediatr Diabetes. 2003; 4:19–23.
Delamater AM, Shaw KH, Applegate EB, Pratt IA, Eidson M, Lancelotta GX, et al. Risk for metabolic control problems in minority youth with diabetes. Diabetes Care. 1999; 22:700–5.
Wadsworth ME, Compas BE. Coping with family conflict and economic strain: The adolescent perspective. J Res Adolescence. 2002; 12:243–74.
Connor-Smith JK, Compas BE, Wadsworth ME, Thomsen AH, Saltzman H. Responses to stress in adolescence: Measurement of coping and involuntary stress responses. J Consult Clin Psychol. 2000; 68:976–92.
Compas BE, Boyer MC, Stanger C, Colletti RB, Thomsen AH, Dufton LM, et al. Latent variable analysis of coping, anxiety/depression, and somatic symptoms in adolescents with chronic pain. J Consult Clin Psychol. 2006; 56:1132–42.
Kline RB. Principles and Practice of Structural Equation Modeling. 3 rd Ed. Guilford Press, New York, NY, 2011.
Vitaliano PP, Maiuro RD, Russo J, Becker J. Raw versus relative scores in the assessment of coping strategies. J Behav Med. 1987; 10:1–18.
Schilling LS, Dixon JK, Knafl KA, Lynn MR, Murphy K, Dumser S, et al. A new self-report measure of self-management of type 1 diabetes for adolescents. Nurs Res. 2009; 58:228–36.
Varni JW, Seid M, Kurtin PS. Pediatric health-related quality of life measurement technology: A guide for health care decision makers. J Clin Outcomes Manage. 1999; 6:33–40.
Browne MW, Cudeck R. Alternative ways of assessing model fit. In: Bollen KA, Long JS, (eds). Testing structural equation models. Sage, Newbury Park, CA, 1993, pp. 136–62.
Faulkner MS, Fritschi C, Quinn L, Hepworth JT. Cardiovascular risks in adolescents with diabetes from vulnerable populations. Home Health Care Manage Prac. 22:123–30.
Skinner EA, Zimmer-Gembeck MJ. The development of coping. Annu Rev Psychol. 2007; 58:119–44.
Whittemore R, Jaser SS, Guo J, Grey M. A conceptual model of adaptation to type 1 diabetes. Nurs Outlook. 2010; 58:242–51.
Wadsworth ME, Raviv T, Santiago CD, Etter EM. Testing the adaptation to poverty-related stress model: Predicting psychopathology symptoms in families facing economic hardship. J Clin Child Adolesc Psychol. 2011; 40:646–57.
Luyckx K, Seiffge-Krenke I, Hampson S. Glycemic control, coping, and internalizing and externalizing symptoms in adolescents with type 1 diabetes: A cross-lagged, longitudinal approach Diabetes Care. 2010; 33:1424–9.
Skinner EA, Edge K, Altman J, Sherwood H. Searching for the structure of coping: A review and critique of the category systems for classifying ways of coping. Psychol Bull. 2003; 129:216–69.
Garcia C. Conceptualization and measurement of coping during adolescence: A review of the literature. J Nurs Scholarship. 2010; 42:166–85.
Acknowledgments
This research was supported by grant number R01-NR04009 from the National Institute of Nursing Research (PIs: Grey and Whittemore). Author Sarah S. Jaser was supported by awards from the National Institute of Diabetes and Digestive and Kidney Diseases (K23 NK088454) and the National Center for Research Resources (UL1 RR024139). The contents of this manuscript are solely the responsibility of the authors and do not necessarily represent the official view of NIH. Clinical Trial Registry number: NCT00684658
Conflict of Interest Statement
The authors have no conflict of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Jaser, S.S., Faulkner, M.S., Whittemore, R. et al. Coping, Self-Management, and Adaptation in Adolescents with Type 1 Diabetes. ann. behav. med. 43, 311–319 (2012). https://doi.org/10.1007/s12160-012-9343-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12160-012-9343-z