Abstract
Objective
The purpose of this study is to identify factors which predict adherence in stroke survivors.
Design
This is a longitudinal study where 180 stroke survivors were assessed 1 year after their first ischaemic stroke. The relationship between adherence and illness and medication beliefs was tested at baseline (time 1) and again 5–6 weeks later (time 2).
Main Outcome Measures
The main outcome measures used in this study are Medication Adherence Report Scale and urinary salicylate levels.
Results
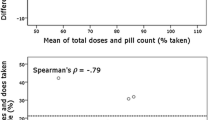
Four variables predicted time 1 poor adherence: (1) younger age, (2) increased specific concerns about medications, (3) reduced cognitive functioning and (4) low perceived benefit of medication. Three out of these four variables were again predictive of time 2 adherence and accounted for 24% of the variance: (1) younger age, (2) increased specific concerns about medications and (3) low perceived benefit of medication. The urinary salicylate assay failed to differentiate between patients taking and not taking aspirin.
Conclusion
Interventions to improve adherence should target patients’ beliefs about their medication.
Similar content being viewed by others
References
World Health Organisation. Adherence to long-term therapies: Evidence for action. Geneva: WHO; 2003.
Haynes RB, Ackloo E, Sahota N, McDonald HP, Yao X. Interventions for enhancing medication adherence (Review). The Cochrane Collaboration, 4; 2008.
National Institute for Clinical Excellence, UK. Medicines adherence, Clinical Guideline, 76; 2009.
Scottish Intercollegiate Guidelines Network. Management of patients with stroke or TIA: assessment, investigation, immediate management and secondary prevention—A national guideline. Guideline 108. Edinburgh: SIGN; 2008
Stephenson J. Noncompliance may cause half of antihypertensive drug "failures". JAMA. 1999; 282[4]: 313-314.
Hayes TL, Larimer N, Adami A, Kaye JA. Medication adherence in healthy elders: small cognitive changes make a big difference. J Aging Health. 2009; 21[4]: 567-580.
Fischer B, Lehrl S, Weber E, Gundert-Remy U, Fischer, U. [Cerebrovascular insufficiency and compliance with drug therapy]. Z Gerontol. 1981; 14[2]: 145-152.
Leventhal H, Diefenbach M. Illness cognition: using common sense to understand treatment adherence and affect cognition interactions. Cognit Ther and Res. 1992; 16[2]: 143-163.
Meyer D, Leventhal H, Gutmann M. Common-sense models of illness: the example of hypertension. Health Psychol. 1985; 4: 5-135.
Brewer NT, Chapman GB, Brownlee S, Leventhal EA. Cholesterol control medication adherence and illness cognition. Br J Health Psychol. 2002; 7(Part 4): 433-447.
Horne R. Measuring adherence: the case for self-report. Intl J Behavioral Med. 2004; 11:75.
Trewby PN, Reddy AV, Trewby CS, Ashton VJ, Brennan G, Inglis J. Are preventive drugs preventive enough? A study of patients' expectation of benefit from preventive drugs. Clin Med. 2002; 2[6]: 527-533.
Enderby PM, Wood VA, Wade DT, Hewer RL. The Frenchay Aphasia Screening Test: a short simple test for aphasia appropriate for non-specialists. Int Rehabil Med. 1987; 8[4]: 166-170.
Baxter GJ, Lawrence JR, Graham AB, Wiles D, Paterson JR. Identification and determination of salicylic acid and salicyluric acid in urine of people not taking salicylate drugs. Ann Clin Biochem. 2002; 39(Pt 1): 50-55.
Hays RD, Corporation TR. A five-item measure of socially desirable response set. Educ Psychol Meas. 1989; 49: 629-636.
Bartels H, Bohmer M, Heierli C. Serum creatinine determination without protein precipitation. Clin Chim Acta. 1972; 37: 193-197.
McLoone P. Carstairs scores for Scottish Postcode Sectors from the 2001 census. MRC Social and Public Health Sciences Unit. Glasgow: MRC; 2004
Folstein MF, Folstein SE, McHugh PR. Mini-Mental State: a practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975; 12: 189-198.
Wilson B, Cockburn J, Baddeley AD. Rivermead Behavioural Memory Test, Titchfield, Fareham: Thames Valley Test Co; 1985.
O'Carroll RE, McGregor LM, Swanson V, Masterton G, Hayes PC. Adherence to medication after liver transplantation in Scotland: a pilot study. Liver Transpl. 2006; 12[12]: 1862-1868.
Moss-Morris R, Weinman J, Petrie KJ, Horne R, Cameron LD, Buick D. The Revised Illness Perception Questionnaire (IPQ-R). Psychol Health. 2002; 16: 1-15.
Horne R, Weinman J, Hankins M. The beliefs about medicines questionnaire: the development and evaluation of a new method for assessing the cognitive representation of medication. Psychol Health. 1999; 14: 1-24.
Zigmond AS, Snaith RP. The Hospital Anxiety and Depression Scale. Acta Psychiatr Scand. 1983; 67:361-370.
Field A. Discovering statistics using SPSS (2nd ed). London: Sage; 2005.
Tabachnick BG, Fidell LS. Using multivariate statistics (4th ed). Needham Heights, MA: Allyn Bacon; 2001.
Leventhal H, Weinman J, Leventhal EA, Phillips LA. Health psychology: The search for pathways between behavior and health. Annu Rev Psychol. 2008; 59: 477-505.
O'Carroll RE, Dennis M, Johnston M, Sudlow C. Improving adherence to medication in stroke survivors (IAMSS): A randomised controlled trial: Study protocol BMC Neurol. 2010; 10:15.
Acknowledgements
We would also like to thank Dr. Julie Chambers, Dr Carolyn Choudhary and three anonymous reviewers for their helpful comments on a previous version of this paper.
We would also like to thank the patients and partners for their participation. Finally, we acknowledge the grant support provided by the Chief Scientist Office-Scotland, Health Services Research Committee, grant reference CZH/4/297.
Conflict of Interest Statement
The authors have no conflict of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
O’Carroll, R., Whittaker, J., Hamilton, B. et al. Predictors of Adherence to Secondary Preventive Medication in Stroke Patients. ann. behav. med. 41, 383–390 (2011). https://doi.org/10.1007/s12160-010-9257-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12160-010-9257-6