Abstract
Background
Metastasis to the oral soft tissues and jawbones is rare and frequently associated with wide spread disease and dismal prognosis. Herein, we report the clinicopathologic characteristics of 40 intraoral metastatic neoplasms and perform a comprehensive review of the pertinent literature.
Methods
Criteria for inclusion included: (a) archived cases from the UMN Oral Pathology laboratory with available tissue blocks and/or H&E-stained preparations diagnosed between 2003 and 2021, (b) proper documentation of the clinico-radiographic characteristics of oral metastasis along with confirmed history of primary malignancy, or (c) microscopic findings consistent with metastatic disease with or without discovery of the primary site.
Results
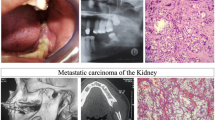
Intraoral metastases comprised 0.03% of all accessioned cases; 22 (55%) occurred in men and 18 (45%) in women (median age = 66.5; range = 18–94 years). Eighteen cases (45%) involved the gingiva, 16 (40%) the gingiva and jawbones, 5 (12.5%) were exclusively intraosseous, and 1 affected (2.5%) the tongue. The lung was the two most frequent primary site in both men (n = 6, 27.3%) and women (n = 5, 27.7%), followed by the colon (n = 4, 18.2%) and kidney (n = 3, 13.7%) in men, and colon (n = 4, 22.2%) and breast (n = 3, 16.6%) in women. Analysis of 1,084 metastatic cases from the literature (male-to-female ratio = 1.2; mean = 52.3; range = 0.6–90 years) indicated strong preference for the jawbones (69.5%) and significant site-specific predilection of certain primary malignancies.
Conclusions
Oral and gnathic metastases are rare but demonstrate a clear predilection for the gingiva and mandible. Clinicians should remain cognizant of such lesions since they frequently mimic inflammatory, reactive or benign neoplastic processes and, in certain cases, are the first indication of occult disease.




Similar content being viewed by others
Data Availability
The data and material presented in this study are available upon request.
Code Availability
Not applicable.
References
Kaplan I, Raiser V, Shuster A, Shlomi B, Rosenfeld E, Greenberg A, et al. Metastatic tumors in oral mucosa and jawbones: unusual primary origins and unusual oral locations. Acta Histochem. 2019;121:151448.
Hirshberg A, Leibovich P, Buchner A. Metastatic tumors to the jawbones: analysis of 390 cases. J Oral Pathol Med. 1994;23:337–41.
Hirshberg A, Shnaiderman-Shapiro A, Kaplan I, Berger R. Metastatic tumours to the oral cavity—pathogenesis and analysis of 673 cases. Oral Oncol. 2008;44:743–52.
Kumar G, Manjunatha B. Metastatic tumors to the jaws and oral cavity. J Oral Maxillofac Pathol. 2013;17:71–5.
Hirshberg A, Berger R, Allon I, Kaplan I. Metastatic tumors to the jaws and mouth. Head Neck Pathol. 2014;8:463–74.
Meyer I, Shklar G. Malignant tumors metastatic to mouth and jaws. Oral Surg Oral Med Oral Pathol. 1965;20:350–62.
Neville B, Allen C, Damm D, Chi A. Oral and maxillofacial pathology. Fourth. Amsterdam: Elselvier; 2016.
Seoane J, Van der Waal I, Van der Waal RI, Cameselle-Teijeiro J, Antón I, Tardio A, et al. Metastatic tumours to the oral cavity: a survival study with a special focus on gingival metastases. J Clin Periodontol. 2009;36:488–92.
Ayranci F, Omezli MM, Torul D, Ay M. Metastatic prostate adenocarcinoma of the mandible diagnosed with oral manifestations. J Craniofac Surg. 2020;31:e220–2.
D’Silva NJ, Summerlin DJ, Cordell KG, Abdelsayed RA, Tomich CE, Hanks CT, et al. Metastatic tumors in the jaws: a retrospective study of 114 cases. J Am Dent Assoc. 2006;137:1667–72.
Hirshberg A, Leibovich P, Buchner A. Metastases to the oral mucosa: analysis of 157 cases. J Oral Pathol Med. 1993;22:385–90.
Shen ML, Kang J, Wen YL, Ying WM, Yi J, Hua CG, et al. Metastatic tumors to the oral and maxillofacial region: a retrospective study of 19 cases in West China and review of the Chinese and English literature. J Oral Maxillofac Surg. 2009;67:718–37.
Jham BC, Salama AR, McClure SA, Ord RA. Metastatic tumors to the oral cavity: a clinical study of 18 cases. Head Neck Pathol. 2011;5:355–8.
Murillo J, Bagan JV, Hens E, Diaz JM, Leopoldo M. Tumors metastasizing to the oral cavity: a study of 16 cases. J Oral Maxillofac Surg. 2013;71:1545–51.
McClure SA, Movahed R, Salama A, Ord RA. Maxillofacial metastases: a retrospective review of one institution’s 15-year experience. J Oral Maxillofac Surg. 2013;71:178–88.
Maschino F, Guillet J, Curien R, Dolivet G, Bravetti P. Oral metastasis: a report of 23 cases. Int J Oral Maxillofac Surg. 2013;42:164–8.
Bodner L, Sion-Vardy N, Geffen DB, Nash M. Metastatic tumors to the jaws: a report of eight new cases. Med Oral Patol Oral Cir Bucal. 2006;11:E132–5.
Owosho AA, Xu B, Kadempour A, Yom SK, Randazzo J, Ghossein RA, et al. Metastatic solid tumors to the jaw and oral soft tissue: a retrospective clinical analysis of 44 patients from a single institution. J Craniomaxillofac Surg. 2016;44:1047–53.
Sánchez Aniceto G, García Peñín A, de la Mata PR, Montalvo Moreno JJ. Tumors metastatic to the mandible: analysis of nine cases and review of the literature. J Oral Maxillofac Surg. 1990;48:246–51.
Shimono H, Hirai H, Oikawa Y, Mochizuki Y, Kuroshima T, Tomioka H, et al. Metastatic tumors in the oral region: a retrospective chart review of clinical characteristics and prognosis. Oral Surg Oral Med Oral Pathol Oral Radiol. 2021;132:648–52.
Lee YH, Lee JI. Metastatic carcinoma of the oral region: An analysis of 21 cases. Med Oral Patol Oral Cir Bucal. 2017;22:e359–65.
Hanahan D, Weinberg RA. Hallmarks of cancer: the next generation. Cell. 2011;144:646–74.
Nguyen DX, Bos PD, Massagué J. Metastasis: from dissemination to organ-specific colonization. Nat Rev Cancer. 2009;9:274–84.
Talmadge JE, Fidler IJ. AACR centennial series: the biology of cancer metastasis: historical perspective. Cancer Res. 2010;70:5649–69.
Polyak K, Weinberg RA. Transitions between epithelial and mesenchymal states: acquisition of malignant and stem cell traits. Nat Rev Cancer. 2009;9:265–73.
Koutlas IG, Dolan M, Lingen MW, Argyris PP. Plasmacytoid cells in salivary pleomorphic adenoma: an alternative interpretation of their immunohistochemical characteristics highlights function and capability for epithelial-mesenchymal transition. Oral Surg Oral Med Oral Pathol Oral Radiol. 2019;128:515–29.
Lamouille S, Xu J, Derynck R. Molecular mechanisms of epithelial-mesenchymal transition. Nat Rev Mol Cell Biol. 2014;15:178–96.
Thiery JP, Acloque H, Huang RY, Nieto MA. Epithelial-mesenchymal transitions in development and disease. Cell. 2009;139:871–90.
Acloque H, Adams MS, Fishwick K, Bronner-Fraser M, Nieto MA. Epithelial-mesenchymal transitions: the importance of changing cell state in development and disease. J Clin Invest. 2009;119:1438–49.
Naumov GN, Bender E, Zurakowski D, Kang SY, Sampson D, Flynn E, et al. A model of human tumor dormancy: an angiogenic switch from the nonangiogenic phenotype. J Natl Cancer Inst. 2006;98:316–25.
Bishop-Bailey D. Tumour vascularisation: a druggable target. Curr Opin Pharmacol. 2009;9:96–101.
Christofori G. New signals from the invasive front. Nature. 2006;441:444–50.
Pugh CW, Ratcliffe PJ. Regulation of angiogenesis by hypoxia: role of the HIF system. Nat Med. 2003;9:677–84.
Reymond N, d’Água BB, Ridley AJ. Crossing the endothelial barrier during metastasis. Nat Rev Cancer. 2013;13:858–70.
Psaila B, Lyden D. The metastatic niche: adapting the foreign soil. Nat Rev Cancer. 2009;9:285–93.
Wells A, Griffith L, Wells JZ, Taylor DP. The dormancy dilemma: quiescence versus balanced proliferation. Cancer Res. 2013;73:3811–6.
Batson OV. The function of the vertebral veins and their role in the spread of metastases. Ann Surg. 1940;112:138–49.
Tezal M, Sullivan MA, Hyland A, Marshall JR, Stoler D, Reid ME, et al. Chronic periodontitis and the incidence of head and neck squamous cell carcinoma. Cancer Epidemiol Biomark Prev. 2009;18:2406–12.
Allon I, Pessing A, Kaplan I, Allon DM, Hirshberg A. Metastatic tumors to the gingiva and the presence of teeth as a contributing factor: a literature analysis. J Periodontol. 2014;85:132–9.
Wells A, Grahovac J, Wheeler S, Ma B, Lauffenburger D. Targeting tumor cell motility as a strategy against invasion and metastasis. Trends Pharmacol Sci. 2013;34:283–9.
Coleman RE. Clinical features of metastatic bone disease and risk of skeletal morbidity. Clin Cancer Res. 2006;12:6243s-s6249.
Barnes L. Metastases to the head and neck: an overview. Head Neck Pathol. 2009;3:217–24.
National Cancer Institute S, Epidemiology, and End Results Program. Cancer stat facts: kidney and renal pelvis cancer. https://seer.cancer.gov/statfacts/html/kidrp.html. Accessed 17 Jan 2022.
Lim SY, Kim SA, Ahn SG, Kim HK, Kim SG, Hwang HK, et al. Metastatic tumours to the jaws and oral soft tissues: a retrospective analysis of 41 Korean patients. Int J Oral Maxillofac Surg. 2006;35:412–5.
Pavlidis N, Pentheroudakis G. Cancer of unknown primary site. Lancet. 2012;379:1428–35.
Cígerová V, Adamkov M, Drahošová S, Grendár M. Immunohistochemical expression and significance of SATB2 protein in colorectal cancer. Ann Diagn Pathol. 2021;52:51.
Gurel B, Ali TZ, Montgomery EA, Begum S, Hicks J, Goggins M, et al. NKX3.1 as a marker of prostatic origin in metastatic tumors. Am J Surg Pathol. 2010;34:1097–105.
Liliac L, Carcangiu ML, Canevari S, Căruntu ID, Ciobanu Apostol DG, Danciu M, et al. The value of PAX8 and WT1 molecules in ovarian cancer diagnosis. Rom J Morphol Embryol. 2013;54:17–27.
Nonaka D, Chiriboga L, Soslow RA. Expression of pax8 as a useful marker in distinguishing ovarian carcinomas from mammary carcinomas. Am J Surg Pathol. 2008;32:1566–71.
Monzon FA, Koen TJ. Diagnosis of metastatic neoplasms: molecular approaches for identification of tissue of origin. Arch Pathol Lab Med. 2010;134:216–24.
Pesis M, Taicher S, Greenberg G, Hirshberg A. Metastasis to the jaws as a first manifestation of hepatocellular carcinoma: report of a case and analysis of 41 cases. J Craniomaxillofac Surg. 2014;42:1997–2001.
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
Conceptualization and design of the study was performed by RG and PPA. Material preparation, data collection and analysis were performed by DPH, PEW, RG and PPA. Statistical analyses were performed by RIV. The first draft of the manuscript was written by DPH and PPA. All authors commented on previous versions of the manuscript and have read and approved the final submitted version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest to disclose.
Ethical Approval
This retrospective cohort is exempt from institutional IRB approval.
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ho, D.P., Wilkinson, P.E., Vogel, R.I. et al. Metastatic Tumors to the Oral Soft Tissues and Jawbones: A Retrospective Analysis of 40 Cases and Review of the Literature. Head and Neck Pathol 16, 802–813 (2022). https://doi.org/10.1007/s12105-022-01451-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12105-022-01451-8