Abstract
Thyroid paraganglioma is an extremely rare tumor and frequently mistaken for other thyroid neoplasms. Increased awareness of its potential presentation in thyroid and its characteristic features is essential for avoiding diagnostic and therapeutic pitfalls. We describe here three additional cases of primary thyroid paraganglioma and analyze their clinical findings and pathological characteristics. Patients included two women and one man presenting with asymptomatic thyroid nodules. Radiological examinations were nonspecific and none had been diagnosed correctly before surgery. On intraoperative frozen section consultation they were all misdiagnosed as carcinomas, either primary or metastatic. However, the permanent sections showed features consistent with paraganglioma. Of note, two cases displayed extension into adjacent thyroid tissues, one of which exhibited increased mitotic activity, confluent tumor necrosis and vascular invasion. Immunohistochemically, the neoplastic chief cells expressed chromogranin, synaptophysin, neuron-specific enolase and CD56, whereas the sustentacular cells were highlighted by S100 protein. All three patients were well with normal hormone secretion, without local recurrence or distant metastasis at last follow-up (range 10–47 months). We further reviewed the literature to summarize the characteristics of this distinctive entity. Albeit being very rare, paraganglioma should be included in the differential diagnosis of hypervascular thyroidal neoplasms. Accurate diagnosis relies on the histopathogical findings and adjunctive immunohistochemcial studies. To date, all the reported cases have pursued a benign course. Although atypical features seem to have no association with clinical behavior, long time postoperative surveillance with biochemical screening of hormone secretion, cervical ultrasonography and whole-body CT scan is recommended.




Similar content being viewed by others
References
Zantour B, Guilhaume B, Tissier F, et al. A thyroid nodule revealing a paraganglioma in a patient with a new germline mutation in the succinate dehydrogenase B gene. Eur J Endocrinol. 2004;151:433–8.
Ferri E, Manconi R, Armato E, Ianniello F. Primary paraganglioma of thyroid gland: a clinicopathologic and immunohistochemical study with review of the literature. Acta Otorhinolaryngol Ital. 2009;29:97–102.
Haegert DG, Wang NS, Farrer PA, et al. Non-chromaffin paragangliomatosis manifesting as a cold thyroid nodule. Am J Clin Pathol. 1974;61:561–70.
Schmit GD, Gorman B, van Heerden JA, Gharib H. Inferior laryngeal paraganglioma mimicking a primary thyroid tumor. Endocr Pract. 2006;12:432–5.
Erem C, Kocak M, Nuhoglu İ, et al. Primary thyroid paraganglioma presenting with double thyroid nodule: a case report. Endocrine. 2009;36:368–71.
Cayot F, Bastien H, Justrabo E, et al. Multiple paragangliomas of the neck localized in the thyroid region. Papillary thyroid cancer associated with parathyroid adenoma. Sem Hop. 1982;58:2004–7.
Kronz JD, Argani P, Udelsman R, et al. Paraganglioma of the thyroid: two cases that clarify and expand the clinical spectrum. Head Neck. 2000;22:621–5.
Yano Y, Nagahama M, Sugino K, et al. Paraganglioma of the thyroid: report of a male case with ultrasonographic imagings, cytologic, histologic, and immunohistochemical features. Thyroid. 2007;17:575–8.
Tiong HY, White SA, Roop L, et al. Paraganglioma-an unusual solitary nodule of the thyroid. Eur J Surg Oncol. 2000;26:720–1.
Foppiani L, Marugo A, Del Monte P, et al. Thyroid paraganglioma manifesting as hot toxic nodule. J Endocrinol Invest. 2005;28:479–80.
Phitayakorn R, Faquin W, Wei N, et al. Thyroid-associated paragangliomas. Thyroid. 2011;21:725–33.
Evankovich J, Dedhia RC, Mastaki JM, et al. Primary sclerosing paraganglioma of the thyroid gland: a case report. Ann Otol Rhinol Laryngol. 2012;121:510–5.
Corrado S, Montanini V, De Gaetani C, et al. Primary paraganglioma of the thyroid gland. J Endocrinol Invest. 2004;27:788–92.
Bockhorn M, Sheu SY, Frilling A, et al. Paraganglioma-like medullary thyroid carcinoma: a rare entity. Thyroid. 2005;15:1363–7.
Castelblanco E, Gallel P, Ros S, et al. Thyroid paraganglioma. Report of 3 cases and description of an immunohistochemical profile useful in the differential diagnosis with medullary thyroid carcinoma, based on complementary DNA array results. Hum Pathol. 2012;43:1103–12.
Vodovnik A. Fine needle aspiration cytology of primary thyroid paraganglioma. Report of a case with cytologic, histologic and immunohistochemical features and differential diagnostic considerations. Acta Cytol. 2002;46:1133–7.
Mitsudo SM, Grajower MD, Balbi H, Silver C. Malignant paraganglioma of the thyroid gland. Arch Pathol Lab Med. 1987;111:378–80.
de Vries EJ, Watson CG. Paraganglioma of the thyroid. Head Neck. 1989;11:462–5.
Armstrong MJ, Chiosea SI, Carty SE, et al. Thyroid paragangliomas are locally aggressive. Thyroid. 2012;22:88–93.
Brownlee RE, Shockley WW. Thyroid paraganglioma. Ann Otol Rhinol Laryngol. 1992;101:293–9.
Banner B, Morecki R, Eviatar A. Chemodectoma in the mid-thyroid region. J Otolaryngol. 1979;8:271–3.
Buss DH, Marshall RB, Baird FG, Myers RT. Paraganglioma of the thyroid gland. Am J Surg Pathol. 1980;4:589–93.
Hughes JH, El-Mofty S, Sessions D, Liapis H. Primary intrathyroidal paraganglioma with metachronous carotid body tumor: report of a case and review of the literature. Pathol Res Pract. 1997; 193: 791–6; discussion 797–9.
Napolitano L, Francomano F, Angelucci D, Napolitano AM. Thyroid paraganglioma: report of a case and review of the literature. Ann Ital Chir. 2000; 71:511–3; discussion 513–4.
Skiadas PK, Kakavoulis TN, Gikonti IJ. Normalisation of blood pressure and heart rate after excision of a thyroid paraganglioma. Eur J Surg. 2001;167:392–4.
González Poggioli N, López Amado M, Pimentel MT. Paraganglioma of the thyroid gland: a rare entity. Endocr Pathol. 2009;20:62–5.
Mun KS, Pailoor J, Chan KS, Pillay B. Extra-adrenal paraganglioma: presentation in three uncommon locations. Malays J Pathol. 2009;31:57–61.
Basu S, Viswanathan S. Primary paraganglioma of thyroid presenting as solitary thyroid mass. J Cancer Res Ther. 2011;7:385–7.
LaGuette J, Matias-Guiu X, Rosai J. Thyroid paraganglioma: a clinicopathologic and immunohistochemical study of three cases. Am J Surg Pathol. 1997;21:748–53.
Massaioli N, Balbo G, Fausone G, Negro D. Endothyroid (non-chromaffin) branchiomeric paraganglioma. Description of a clinical case. Minerva Chir. 1979;34:867–74.
Van Duinen N, Steenvoorden D, Kema IP, Jansen JC, Vriends AHJT, Bayley JP, Smit JWA, Romijn JA, Corssmitt EPM. Increased urinary excretion of 3-methoxytyramine in patients with head and neck paragangliomas. J Clin Endocrinol Metab. 2010;95:209–14.
Fishbein L, Nathanson KL. Pheochromocytoma and paraganglioma: understanding the complexities of the genetic background. Cancer Genet. 2012;205:1–11.
Acknowledgments
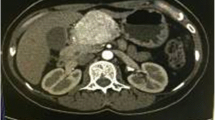
The authors are very grateful to Dr. Bai-Zhou Li (Department of Pathology, the 2nd Affiliated Hospital of Zhejiang University, Medical College, Hangzhou, China) for kindly providing the ultrasound image and CT scan figure of case 1.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yu, BH., Sheng, WQ. & Wang, J. Primary Paraganglioma of Thyroid Gland: A Clinicopathologic and Immunohistochemical Analysis of Three Cases with a Review of the Literature. Head and Neck Pathol 7, 373–380 (2013). https://doi.org/10.1007/s12105-013-0467-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12105-013-0467-7