Abstract
Urinary tract infection (UTI) is a common infection in infants and children. During infancy, boys are more commonly affected than girls and thereafter, female preponderance is found. Presentation varies among different age groups. Clinical features in neonates and young infants are non-specific, manifest as septicemia where a high index of suspicion is needed. Older children typically present as simple or complicated UTI. Rapid diagnosis, institution of early treatment and further evaluation by imaging modalities are of utmost importance. The prevention of recurrent UTI and detection of congenital anomalies of kidney and urinary tract are major objectives in the management. Use of ultrasound is required to detect underlying congenital abnormalities, whereas voiding cystourethrogram and dimercaptosuccinic acid (DMSA) scan are useful in the diagnosis of obstructive uropathy and vesicoureteric reflux and renal scar, respectively. The children requiring surgical interventions are to be recognised early to prevent recurrent UTI. The treatment of vesicoureteric reflux by chemoprophylaxis in lower grades and surgical treatment in higher grades are important consideration in prevention of recurrent UTI. This is required to prevent renal parenchymal damage and scarring that can cause hypertension and progressive renal insufficiency in later life.

Similar content being viewed by others
References
National Institute for Health and Clinical Excellence (NICE). Urinary tract infection in children: diagnosis, treatment and long-term management. National Collaborating Centre for Women’s and Children’s Health. Clinical guideline 2007. www.nice.org.uk/CG054.
Chang SL, Shortliffe LD. Pediatric urinary tract infections. Pediatr Clin North Am. 2006;53:379–400.
Elder JS. Urinary tract infections. In: Kliegman RM, Stanton BF, St. Geme JW, Schor NF, Behrman RE, eds. Nelson Textbook of Pediatrics. Philadelphia: Elsevier Saunders; 2011. pp. 1829–934.
Conway PH, Cnaan A, Zaoutis T, Henry BV, Grundmeier RW, Keren R. Recurrent urinary tract infections in children: Risk factors and association with prophylactic antimicrobials. JAMA. 2007;298:179–86.
Dai B, Liu Y, Jia J, Mei C. Long-term antibiotics for the prevention of recurrent urinary tract infection in children: A systematic review and meta-analysis. Arch Dis Child. 2010;95:499–508.
Saadeh SA, Mattoo TK. Managing urinary tract infections. Pediatr Nephrol. 2011;26:1967–76.
Bell LE, Mattoo TK. Update on childhood urinary tract infection and vesicoureteral reflux. Semin Nephrol. 2009;29:349–59.
Bensman A, Dunand O, Ulinski T. Urinary tract infections. In: Avner ED, Harmon WE, Niaudet P, Yoshikawa N, eds. Pediatric Nephrology. Berlin: Springer-Verlag; 2009. pp. 1299–310.
Panaretto K, Craig J, Knight J, Howman-Giles R, Sureshkumar P, Roy L. Risk factors for recurrent urinary tract infection in preschool children. J Paediatr Child Health. 1999;35:454–9.
Williams GJ, Macaskill P, Chan SF, Turner RM, Hodson E, Craig JC. Absolute and relative accuracy of rapid urine tests for urinary tract infection in children: A meta-analysis. Lancet Infect Dis. 2010;10:240–50.
Indian Society of Pediatric Nephrology, Vijayakumar M, Kanitkar M, Nammalwar BR, Bagga A. Revised statement on management of urinary tract infections. Indian Pediatr. 2011;48:709–17.
Williams G, Craig JC. Diagnosis and management of urinary tract infections. In: Geary DF, Schaefer F, eds. Comprehensive Pediatric Nephrology. Philadelphia: Mosby Elsevier; 2008. pp. 539–48.
American Academy of Pediatrics, Committee on Quality Improvement, Subcommittee on Urinary Tract Infections. Practice parameters: the diagnosis, treatment and evaluation of the initial urinary tract infections in febrile infants and young children. Pediatrics. 1999;103:843–52.
Lebowitz RL, Olbing H, Parkkulainen KV, Smellie JM, Tamminen-Mobius TE. International system of radiographic grading of vesicoureteric reflux. International reflux study in children. Pediatr Radiol. 1985;15:105–9.
American Academy of Pediatrics, Subcommittee on urinary tract infection, steering committee on quality improvement and management. Urinary tract infection: Clinical practice guideline for the diagnosis and management of the initial UTI in febrile infants and children 2 to 24 months. Pediatrics. 2011;128:595–610.
Ditchfield MR, Summerville D, Grimwood K, Cook DJ, Powell HR, Sloane R, et al. Time course of transient cortical scintigraphic defects associated with acute pyelonephritis. Pediatr Radiol. 2002;32:849–52.
Singh-Grewal D, Macdessi J, Craig J. Circumcision for the prevention of urinary tract infection in boys: A systematic review of randomized trials and observational studies. Arch Dis Child. 2005;90:853–8.
Yohannes P, Hanna M. Current trend in the management of posterior urethral valves in the pediatric population. Urology. 2002;60:947–53.
Hodson EM, Wheeler DM, Smith GH, Craig JC, Vimalachandra D. Interventions for primary vesicoureteric reflux. Cochrane Database Syst Rev. 2007;3:CD001532.
Greenbaum LA, Mesrobian HGO. Vesicoureteral reflux. Pediatr Clin North Am. 2006;53:413–27.
Molitierno JA, Scherz HC, Kirsch AJ. Endoscopic treatment of vesicoureteral reflux using dextranomer hyaluronic acid copolymer. J Pediatr Urol. 2008;4:221–8.
Acknowledgments
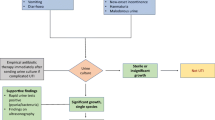
Authors are thankful to Prof. Piyush Gupta, Editor-in Chief, Indian Pediatrics for his permission to quote algorithm for evaluation of children after first episode of UTI from Ref. [11].
Conflict of Interest
None.
Role of Funding Source
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
Guest Editor: Bhim S. Pandhi
Rights and permissions
About this article
Cite this article
Mishra, O.P., Abhinay, A. & Prasad, R. Urinary Infections in Children. Indian J Pediatr 80, 838–843 (2013). https://doi.org/10.1007/s12098-013-1118-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-013-1118-4