Abstract
Objective
To study the menstrual problems and menstrual hygiene practices of adolescent girls in Thiruvananthapuram City Corporation.
Methods
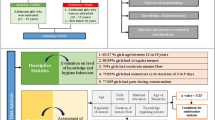
Students of class XI and XII in the age group 15–19 years, belonging to ten Higher Secondary Schools within the Thiruvananthapuram City Corporation area were selected for the study by multistage sampling procedure and screened using a pretested self evaluation questionnaire.
Results
Menstrual disorders were reported in 21.1%. The most frequently reported problem during menstruation was dysmenorrhoea (72.4%) followed by oligomenorrhoea (11.3%). Only 11.5% of the girls who had menstrual problems sought treatment and majority from a gynecologist. Out of 81.5% girls who reported vaginal discharge, only 5.7% had abnormal discharge. Menstrual hygiene was adequate in the majority of girls.
Conclusions
Menstrual disorders are common in adolescence and can have significant consequences on future reproductive health.
Similar content being viewed by others
References
Jacks TH, Obed JY, Agida ET, Petrova GV. Dysmenorrhoea and menstrual abnormalities among postmenarcheal secondary school girls in Maiduguri Nigeria. Afr J Med Med Sci. 2005;34:87–9.
Dutta R, Sengupta S. A profile of adolescent girls with gynecological problems. J Obstet Gynecol India. 2005;55:353–5.
McEvoy M, Chang J, Coupey SM. Common menstrual disorders in adolescence: nursing interventions. Am J Matern Child Nurs. 2004;29:41–9.
Lee LK, Chen PC, Lee KK, Kaur J. Menstruation among adolescent girls in Malaysia: a cross-sectional school survey. Singapore Med J. 2006;47:869–74.
Houston AM, Abraham A, Huang Z, D’Angelo LJ. Knowledge, attitudes, and consequences of menstrual health in urban adolescent females. J Pediatr Adolesc Gynecol. 2006;19:271–5.
Thomas KD, Okonofua FE, Chiboka O. A study of the menstrual patterns of adolescents in Ile-Ife, Nigeria. Int J Gynaecol Obstet. 1990;33:31.
Widhom O, Kantero RL. A statistical analysis of the menstrual patterns of 8,000 Finnish girls and their mothers. Acta Obstet Gynecol Scand Suppl. 1971;14:1–36.
Hickey M, Balen A. Menstrual disorders in adolescence: investigation and management. Hum Reprod Update. 2003;9:493–504.
Minjarez DA, Bradshaw KD. Abnormal uterine bleeding in adolescents. Obstet Gynecol Clin North Am. 2000;27:63–78.
Tscherne G. Menstrual cycle anomalies in young girls--prognosis concerning later fertility. Gynakol Geburtshilfliche Rundsch. 1998;38:47–9 [Article in German].
Agarwal DK, Agarwal KN, Upadhyay SK, Mittal R, Prakash R, Rai S. Physical and sexual growth pattern of affluent Indian children from 5 to 18 years of age. Indian Pediatr. 1992;29:1203–82.
Dzhorbenadze MT, Kristesashvili DI, Chopikashvili NA. Menstrual function in adolescent girls in Tbilisi. Georgian Med News. 2006;130:37–40 [Article in Russian].
van Hooff MHA, Voorhorst FJ, Kaptein MBH, Hirasing RA, Koppenaal C, Schoemaker J. Predictive value of menstrual cycle pattern, body mass index, hormone levels and polycystic ovaries at age 15 years for oligo-amenorrhoea at age 18 years. Hum Reprod. 2004;19:383–92.
Treloar AE, Boynton RE, Behn BG, Brown BW. Variation of the human menstrual cycle through reproductive life. Int J Fertil. 1967;12:77–126.
Mansfield MJ, Emans SJ. Adolescent menstrual irregularity. J Reprod Med. 1984;29:399–410.
American Academy of Pediatrics et al. Committee on adolescent health care menstruation in girls and adolescents: using the menstrual cycle as a vital sign. Pediatrics. 2006;118:2245–50.
Narayan KA, Srinivasa DK, Pelto PJ, Veerammal S. Puberty rituals, reproductive knowledge and health of adolescent schoolgirls in South India. Asia Pac Popul J. 2001;16:225–38.
Nair P, Grover VL, Kannan AT. Awareness and practices of menstruation and pubertal changes amongst unmarried female adolescents in a rural area of East Delhi. Indian J Community Med. 2007;32:156–7.
Sharma P, Malhotra C, Taneja DK, Saha R. Problems related to menstruation amongst adolescent girls. Indian J Pediatr. 2008;75:125–9.
El-Gilany AH, Badawi K, El-Fedawy S. Epidemiology of dysmenorrhoea among adolescent students in Mansoura, Egypt. East Mediterr Health J. 2005;11:155–63.
Joseph GA, Bhattacharji S, Joseph A, Rao PS. General and reproductive health of adolescent girls in rural south India. Indian Pediatr. 1997;34:242–5.
Legro RS, Kunselman AR, Dodson WC, Dunaif A. Prevalence and predictors of risk for type 2 diabetes mellitus and impaired glucose tolerance in polycystic ovary syndrome: a prospective, controlled study in 254 affected women. J Clin Endocrinol Metab. 1999;84:165–9.
Sheehan MT. Polycystic ovarian syndrome: diagnosis and management. Clin Med Res. 2004;2:13–27.
Acknowledgements
The authors gratefully acknowledge the cooperation and support received from Indian Clinical Epidemiology Network (IndiaCLEN), Parents, Principal and Teachers of the participating schools and staff of Child Development Centre, Kerala, specially Dr. G. Suresh Kumar, Registrar; Mr. Binu T, Office Assistant, Mr. Asokan, PA to Director, Suja S, Junior Programmer, CDC; Medical College, Thiruvananthapuram, in conduction of this study.
Conflict of Interest
None.
Role of Funding Source
Indian Clinical Epidemiology Network (IndiaCLEN).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nair, M.K.C., Chacko, D.S., Ranjith Darwin, M. et al. Menstrual Disorders and Menstrual Hygiene Practices in Higher Secondary School Girls. Indian J Pediatr 79 (Suppl 1), 74–78 (2012). https://doi.org/10.1007/s12098-011-0431-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-011-0431-z