Abstract
Background and aims
Lysyl oxidase-like-1 (LOXL1), a vital cross-linking enzyme in extracellular matrix (ECM) maintenance, promotes fibrosis via enhancement of ECM stability. However, the potential role of LOXL1 in the pathogenesis of nonalcoholic steatohepatitis (NASH) has not been previously studied.
Methods
We generated Loxl1fl/fl mice to selectively delete LOXL1 in hepatic stellate cells (HSCs) (Loxl1fl/flGfapcre; Loxl1fl/fl as littermate controls) and then examined liver pathology and metabolic profiles in Loxl1fl/flGfapcre fed with either a choline-deficient L-amino acid-defined (CDAA) diet or an isocaloric control diet for 16 weeks. Thereafter, the findings from the animal model were confirmed in 23 patients with biopsy-proven non-alcoholic fatty liver disease (NAFLD).
Results
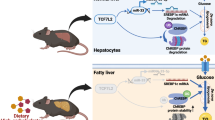
LOXL1 was significantly increased in CDAA induced non-obese NASH compared with the control diet, and LOXL1 deficient in HSCs ameliorated CDAA-induced inflammation and fibrosis, with reduced expression of pro-inflammation and pro-fibrogenic genes in the HSCs-specific LOXL1 knockout mice model. Interestingly, LOXL1 deficient in HSCs could attenuate hepatic steatosis and reverse the metabolic disorder by restoring adipose tissue function without altering the effect of hepatic lipogenesis gene expression in non-obese NASH model. More importantly, analyses of serum LOXL1 and leptin levels from NAFLD patients revealed that LOXL1 was positively correlated with histological fibrosis progression, whereas it was inversely correlated with leptin levels, especially in non-obese NAFLD patients.
Conclusion
LOXL1 may contribute to fibrosis progression in non-obese NAFLD, and HSCs-specific knockout of LOXL1 attenuated liver steatosis, inflammation, fibrosis, , and improved lipid metabolic abnormalities. Hence, LOXL1 inhibition may serve as a new therapeutic strategy for NASH.







Similar content being viewed by others
References
Younossi Z, Anstee QM, Marietti M, Hardy T, Henry L, Eslam M, George J, et al. Global burden of NAFLD and NASH: trends, predictions, risk factors and prevention. Nat Rev Gastroenterol Hepatol 2018;15:11–20
Schuppan D, Surabattula R, Wang XY. Determinants of fibrosis progression and regression in NASH. J Hepatol 2018;68:238–250
Schuppan D, Ashfaq-Khan M, Yang AT, Kim YO. Liver fibrosis: direct antifibrotic agents and targeted therapies. Matrix Biol 2018;68–69:435–451
Chen W, Yang A, Jia J, Popov YV, Schuppan D, You H. Lysyl Oxidase (LOX) Family Members: rationale and their potential as therapeutic targets for liver fibrosis. Hepatology 2020;72:729–741
Zhao W, Yang A, Chen W, Wang P, Liu T, Cong M, Xu A, et al. Inhibition of lysyl oxidase-like 1 (LOXL1) expression arrests liver fibrosis progression in cirrhosis by reducing elastin crosslinking. Biochim Biophys Acta Mol Basis Dis 2018;1864:1129–1137
Romani P, Valcarcel-Jimenez L, Frezza C, Dupont S. Crosstalk between mechanotransduction and metabolism. Nat Rev Mol Cell Biol 2021;22:22–38
Romani P, Brian I, Santinon G, Pocaterra A, Audano M, Pedretti S, Mathieu S, et al. Extracellular matrix mechanical cues regulate lipid metabolism through Lipin-1 and SREBP. Nat Cell Biol 2019;21:338–347
Dongiovanni P, Meroni M, Baselli GA, Bassani GA, Rametta R, Pietrelli A, Maggioni M, et al. Insulin resistance promotes Lysyl Oxidase Like 2 induction and fibrosis accumulation in non-alcoholic fatty liver disease. Clin Sci (Lond) 2017;131:1301–1315
Kleiner DE, Brunt EM, Van Natta M, Behling C, Contos MJ, Cummings OW, Ferrell LD, et al. Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology 2005;41:1313–1321
Nevzorova YA, Boyer-Diaz Z, Cubero FJ, Gracia-Sancho J. Animal models for liver disease —a practical approach for translational research. J Hepatol 2020;73:423–440
Wang H, Xu PF, Li JY, Liu XJ, Wu XY, Xu F, Xie BC, et al. Adipose tissue transplantation ameliorates lipodystrophy-associated metabolic disorders in seipin-deficient mice. Am J Physiol Endocrinol Metab 2019;316:E54–E62
Younossi ZM, Koenig AB, Abdelatif D, Fazel Y, Henry L, Wymer M. Global epidemiology of nonalcoholic fatty liver disease-Meta-analytic assessment of prevalence, incidence, and outcomes. Hepatology 2016;64:73–84
Estes C, Anstee QM, Arias-Loste MT, Bantel H, Bellentani S, Caballeria J, Colombo M, et al. Modeling NAFLD disease burden in China, France, Germany, Italy, Japan, Spain, United Kingdom, and United States for the period 2016–2030. J Hepatol 2018;69:896–904
Sheka AC, Adeyi O, Thompson J, Hameed B, Crawford PA, Ikramuddin S. Nonalcoholic steatohepatitis: a review. JAMA 2020;323:1175–1183
Bellaye PS, Shimbori C, Upagupta C, Sato S, Shi W, Gauldie J, Ask K, et al. Lysyl oxidase-like 1 protein deficiency protects mice from adenoviral transforming growth factor-β1-induced pulmonary fibrosis. Am J Respir Cell Mol Biol 2018;58:461–470
Martinez-Martinez E, Rodriguez C, Galan M, Miana M, Jurado-Lopez R, Bartolome MV, Luaces M, et al. The lysyl oxidase inhibitor (β-aminopropionitrile) reduces leptin profibrotic effects and ameliorates cardiovascular remodeling in diet-induced obesity in rats. J Mol Cell Cardiol 2016;92:96–104
Murawaki Y, Kusakabe Y, Hirayama C. Serum lysyl oxidase activity in chronic liver disease in comparison with serum levels of prolyl hydroxylase and laminin. Hepatology 1991;14:1167–1173
Bertolio R, Napoletano F, Mano M, Maurer-Stroh S, Fantuz M, Zannini A, Bicciato S, et al. Sterol regulatory element binding protein 1 couples mechanical cues and lipid metabolism. Nat Commun 2019;10:1326
Huang W, Dedousis N, Bandi A, Lopaschuk GD, O’Doherty RM. Liver triglyceride secretion and lipid oxidative metabolism are rapidly altered by leptin in vivo. Endocrinology 2006;147:1480–1487
Hackl MT, Furnsinn C, Schuh CM, Krssak M, Carli F, Guerra S, Freudenthaler A, et al. Brain leptin reduces liver lipids by increasing hepatic triglyceride secretion and lowering lipogenesis. Nat Commun 2019;10:2717
Shi Y, Wang Q, Sun Y, Zhao X, Kong Y, Ou X, Jia J, et al. The prevalence of lean/nonobese nonalcoholic fatty liver disease: a systematic review and meta-analysis. J Clin Gastroenterol 2020;54:378–387
Dobie R, Wilson-Kanamori JR, Henderson BEP, Smith JR, Matchett KP, Portman JR, Wallenborg K, et al. Single-cell transcriptomics uncovers zonation of function in the mesenchyme during liver fibrosis. Cell Rep 2019;29:1832–1847 (e1838)
Funding
This study was supported by the National Natural Science Foundation of China (81970524 and 81500456).
Author information
Authors and Affiliations
Contributions
AY, and HY conceived the study. AY, XY, XF, YS, TH, WL, WC, JJ, and HY performed experiments or analyzed the data. AY drafted the manuscript, and all authors read or revised the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors Aiting Yang, Xuzhen Yan, Xu Fan, Yiwen Shi, Tao Huang, Weiyu Li, Wei Chen, Jidong Jia and Hong You declared that they have no conflict of interest.
Animal research
This study was approved by the Institutional Animal Care and Usage Committee of the Beijing Friendship Hospital, Capital Medical University (No.:20-2002).
Consent to participate
The study was conducted in accordance with the principles enshrined in the Declaration of Helsinki and the Good Clinical Practices. The Ethics Committee of Beijing Friendship Hospital, Capital Medical University approved study (No.: 2018-P2-228-02).
Consent to publish
All authors had access to the study data and reviewed and approved the final manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Yang, A., Yan, X., Fan, X. et al. Hepatic stellate cells-specific LOXL1 deficiency abrogates hepatic inflammation, fibrosis, and corrects lipid metabolic abnormalities in non-obese NASH mice. Hepatol Int 15, 1122–1135 (2021). https://doi.org/10.1007/s12072-021-10210-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12072-021-10210-w