Abstract
Purpose
Finding an optimal biomarker for the noninvasive evaluation of acute liver injury (ALI) may be of great value in predicting clinical outcomes and investigating potential treatments. We investigated cell-free DNA (CFD) as a potential biomarker to predict carbon tetrachloride-induced ALI in rats.
Methods
Forty-five Sprague–Dawley rats were randomly assigned to three groups. ALI was induced by carbon tetrachloride via a nasogastric tube at 1, 2.5, or 5 ml/kg of a 50 % solution. Fifteen additional rats underwent a sham procedure. Blood samples were drawn at time t which was 0 (baseline), 3, 6, 12, 24, 48, 72, 96, and 120 h for the measurements of CFD, glutamate–pyruvate transaminase (GPT), glutamate–oxaloacetate transaminase (GOT), and total bilirubin. Prothrombin time and histology were examined at 24 and 120 h following injection of 5 ml/kg carbon tetrachloride in 18 additional rats and in 10 control rats.
Results
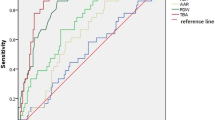
CFD levels in rats subjected to carbon tetrachloride-induced ALI were significantly increased in all blood samples starting at 12 h after the induction of ALI (p < 0.001), reaching peak levels at 24 h. Blood GOT, GPT, and total bilirubin were elevated in all blood samples starting at 3 h after the induction of ALI (p < 0.0001), reaching peak levels by 48 h. A positive correlation was demonstrated between CFD levels and GOT (R 2 = 0.92), GPT (R 2 = 0.92), and total bilirubin (R 2 = 0.76). CFD levels correlated with liver damage seen on histological examination, as well as predicted liver damage, at 24 h after ALI.
Conclusions
CFD may be a useful biomarker for the prediction and measurement of ALI. There is no evidence to suggest that CFD is superior to other available noninvasive biomarkers.




Similar content being viewed by others
References
Bernuau J, Rueff B, Benhamou JP. Fulminant and subfulminant liver failure: definitions and causes. Semin Liver Dis 1986;6(2):97–106
Riordan SM, Williams R. Treatment of hepatic encephalopathy. N Engl J Med 1997;337(7):473–479
Auzinger G, Wendon J. Intensive care management of acute liver failure. Curr Opin Crit Care 2008;14(2):179–188
Lidofsky SD. Liver transplantation for fulminant hepatic failure. Gastroenterol Clin North Am 1993;22(2):257–269
Rakela J, Lange SM, Ludwig J, Baldus WP. Fulminant hepatitis: mayo clinic experience with 34 cases. Mayo Clin Proc 1985;60(5):289–292
Hoofnagle JH, Carithers RL Jr, Shapiro C, Ascher N. Fulminant hepatic failure: summary of a workshop. Hepatology 1995;21(1):240–252
Grigorescu M. Noninvasive biochemical markers of liver fibrosis. J Gastrointestin Liver Dis 2006;15(2):149–159
Rutherford AE, Hynan LS, Borges CB, et al. Serum apoptosis markers in acute liver failure: a pilot study. Clin Gastroenterol Hepatol 2007;5(12):1477–1483
Tagami A, Ohnishi H, Hughes RD. Increased serum soluble Fas in patients with acute liver failure due to paracetamol overdose. Hepatogastroenterology 2003;50(51):742–745
Singhal S, Chakravarty A, Das BC, Kar P. Tumour necrosis factor-alpha and soluble Fas ligand as biomarkers in non-acetaminophen-induced acute liver failure. Biomarkers 2009;14(5):347–353
Ozer J, Ratner M, Shaw M, Bailey W, Schomaker S. The current state of serum biomarkers of hepatotoxicity. Toxicology 2008;245(3):194–205
Ohayon S, Boyko M, Saad A, et al. Cell-free DNA as a marker for prediction of brain damage in traumatic brain injury in rats. J Neurotrauma 2012;29(2):261–267
Boyko M, Ohayon S, Goldsmith T, et al. Cell-free DNA—a marker to predict ischemic brain damage in a rat stroke experimental model. J Neurosurg Anesthesiol 2011;23(3):222–228
Swarup V, Rajeswari MR. Circulating (cell-free) nucleic acids—a promising, non-invasive tool for early detection of several human diseases. FEBS Lett 2007;581(5):795–799
Shimony A, Zahger D, Gilutz H, et al. Cell free DNA detected by a novel method in acute ST-elevation myocardial infarction patients. Acute Card Care 2010;12(3):109–111
Wu Q, Gong D, Tian N, et al. Protection of regenerating liver after partial hepatectomy from carbon tetrachloride hepatotoxicity in rats: roles of mitochondrial uncoupling protein 2 and ATP stores. Dig Dis Sci 2009;54(9):1918–1925
Tunon MJ, Alvarez M, Culebras JM, Gonzalez-Gallego J. An overview of animal models for investigating the pathogenesis and therapeutic strategies in acute hepatic failure. World J Gastroenterol 2009;15(25):3086–3098
van de Kerkhove MP, Hoekstra R, van Gulik TM, Chamuleau RAFM. Large animal models of fulminant hepatic failure in artificial and bioartificial liver support research. Biomaterials 2004;25(9):1613–1625
Zhang BH, Gong DZ, Mei MH. Protection of regenerating liver after partial hepatectomy from carbon tetrachloride hepatotoxicity in rats: role of hepatic stimulator substance. J Gastroenterol Hepatol 1999;14(10):1010–1017
Ugazio G, Danni O, Milillo P, Burdino E, Congiu AM. Mechanism of protection against carbon tetrachloride toxicity. I. Prevention of lethal effects by partial surgical hepatectomy. Drug Chem Toxicol 1982;5(2):115–124
Taniguchi M, Takeuchi T, Nakatsuka R, Watanabe T, Sato K. Molecular process in acute liver injury and regeneration induced by carbon tetrachloride. Life Sci 2004;75(13):1539–1549
Goldshtein H, Hausmann MJ, Douvdevani A. A rapid direct fluorescent assay for cell-free DNA quantification in biological fluids. Ann Clin Biochem 2009;46(Pt 6):488–494
Shimony A, Zahger D, Gilutz H, et al. Cell free DNA detected by a novel method in acute ST-elevation myocardial infarction patients. Acute Card Care 2010;12(3):109–111
Wills PJ, Asha W. Protective effect of Lygodium flexuosum (L.) Sw. extract against carbon tetrachloride-induced acute liver injury in rats. J Ethnopharmacol 2006;108(3):320–326
Ye X, Feng Y, Tong Y, et al. Hepatoprotective effects of Coptidis rhizoma aqueous extract on carbon tetrachloride-induced acute liver hepatotoxicity in rats. J Ethnopharmacol 2009;124(1):130–136
Wang T, Sun NL, Zhang WD, et al. Protective effects of dehydrocavidine on carbon tetrachloride-induced acute hepatotoxicity in rats. J Ethnopharmacol 2008;117(2):300–308
Lo YM, Rainer TH, Chan LY, Hjelm NM, Cocks RA. Plasma DNA as a prognostic marker in trauma patients. Clin Chem 2000;46(3):319–323
Zachariah RR, Schmid S, Buerki N, et al. Levels of circulating cell-free nuclear and mitochondrial DNA in benign and malignant ovarian tumors. Obstet Gynecol 2008;112(4):843–850
Gormally E, Caboux E, Vineis P, Hainaut P. Circulating free DNA in plasma or serum as biomarker of carcinogenesis: practical aspects and biological significance. Mutat Res 2007;635(2–3):105–117
Zhong XY, Ladewig A, Schmid S, et al. Elevated level of cell-free plasma DNA is associated with breast cancer. Arch Gynecol Obstet 2007;276(4):327–331
Kamat AA, Baldwin M, Urbauer D, et al. Plasma cell-free DNA in ovarian cancer: an independent prognostic biomarker. Cancer 2010;116(8):1918–1925
Chang CP, Chia RH, Wu TL, et al. Elevated cell-free serum DNA detected in patients with myocardial infarction. Clin Chim Acta 2003;327(1–2):95–101
Grill S, Rusterholz C, Zanetti-Dallenbach R, et al. Potential markers of preeclampsia—a review. Reprod Biol Endocrinol 2009;7:70–84
Farina A, LeShane ES, Romero R, et al. High levels of fetal cell-free DNA in maternal serum: a risk factor for spontaneous preterm delivery. Am J Obstet Gynecol 2005;193(2):421–425
Saukkonen K, Lakkisto P, Varpula M, et al. Association of cell-free plasma DNA with hospital mortality and organ dysfunction in intensive care unit patients. Intensive Care Med 2007;33(9):1624–1627
Rhodes A, Wort SJ, Thomas H, Collinson P, Bennett ED. Plasma DNA concentration as a predictor of mortality and sepsis in critically ill patients. Crit Care 2006;10(2):R60
Saukkonen K, Lakkisto P, Pettila V, et al. Cell-free plasma DNA as a predictor of outcome in severe sepsis and septic shock. Clin Chem. 2008;54(6):1000–1007
Lam NY, Rainer TH, Wong LK, Lam W, Lo YM. Plasma DNA as a prognostic marker for stroke patients with negative neuroimaging within the first 24 h of symptom onset. Resuscitation 2006;68(1):71–78
Rainer TH, Wong LK, Lam W, et al. Prognostic use of circulating plasma nucleic acid concentrations in patients with acute stroke. Clin Chem 2003;49(4):562–569
Gaffey MJ, Boyd JC, Traweek ST, et al. Predictive value of intraoperative biopsies and liver function tests for preservation injury in orthotopic liver transplantation. Hepatology 1997;25(1):184–189
Janßen H, Lange R, Erhard J, et al. Serum bile acids in liver transplantation—early indicator for acute rejection and monitor for antirejection therapy. Transpl Int 2001;14(6):429–437
Klin Y, Zlotnik A, Boyko M, et al. Distribution of radiolabeled l-glutamate and d-aspartate from blood into peripheral tissues in naive rats: significance for brain neuroprotection. Biochem Biophys Res Commun 2010;399(4):694–698
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gruenbaum, B.F., Boyko, M., Delgado, B. et al. Cell-free DNA as a potential marker to predict carbon tetrachloride-induced acute liver injury in rats. Hepatol Int 7, 721–727 (2013). https://doi.org/10.1007/s12072-012-9414-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12072-012-9414-z