Abstract
Purpose
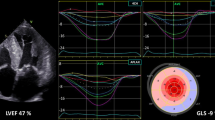
Left ventricular ejection fraction may remain normal or even higher despite significant impairment of contractility in cases of mitral regurgitation. The aim of this study is to evaluate the changes in left ventricular function after mitral valve replacement and to study the role of global longitudinal strain in detecting early left ventricular dysfunction using speckle tracking.
Method
Study involved 31 patients who underwent mitral valve replacement for mitral regurgitation. Patient’s preoperative and postoperative echocardiography (conventional parameters and global longitudinal strain) and other parameters like functional status, radiological findings, and electrocardiogram were recorded to evaluate left ventricular function.
Results
All patients presented in advanced stage with New York heart association class III (67.7%) and IV (32.3%). There was significant decline in left ventricular ejection fraction (with the mean value from 64.58 to 40.13%) and global longitudinal strain (− 15.57 ± 4.98to − 8.97) in the immediate postoperative period (~ 7 days). However, there was a rise in both left ventricular ejection fraction (mean 52.48%) and in global longitudinal strain (mean − 14.44 ± 3.67) at 3 months. Left ventricular and atrial size decreased significantly immediately after surgery, which further declined at 3 months. We also found that patients who attained a left ventricular ejection fraction of > 50% in postoperative period had better left ventricular ejection fraction and global longitudinal strain preoperatively. In addition, they had smaller cardiac size and milder pulmonary hypertension comparatively.
Conclusions
Mitral valve replacement in mitral regurgitation results in decline in left ventricular function immediately after surgery. In patients with chronic mitral regurgitation, left ventricular ejection fraction is fallacious and global longitudinal strain can be an important tool to assess left ventricular ejection fraction.


Similar content being viewed by others
References
Nishimura RA, Otto CM, Bonow RO, et al. 2017 AHA/ACC focused update of the 2014 AHA/ACC guideline for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol. 2017;70:252–89.
Quintana E, Suri RM, Thalji NM, et al. Left ventricular dysfunction after mitral valve repair—the fallacy of “normal” preoperative myocardial function. J Thorac Cardiovasc Surg. 2014;148:2752–62.
Suri RM, Schaff HV, Dearani JA, et al. Determinants of early decline in ejection fraction after surgical correction of mitral regurgitation. J Thorac Cardiovasc Surg. 2008;136:442–7.
Manjunath CN, Srinivas P, Ravindranath KS, Dhanalakshmi C. Incidence and patterns of valvular heart disease in a tertiary care high-volume cardiac center: a single center experience. Indian Heart J. 2014;66:320–6.
Shafii AE, Gillinov AM, Mihaljevic T, Stewart W, Batizy LH, Blackstone EH. Changes in left ventricular morphology and function after mitral valve surgery. Am J Cardiol. 2012;110:403–8.
Miller JD, Suri RM. Left ventricular dysfunction after degenerative mitral valve repair: A question of better molecular targets or better surgical timing? J Thorac Cardiovasc Surg. 2016;152:1071–4.
Dupuis M, Mahjoub H, Clavel MA, et al. Forward left ventricular ejection fraction: a simple risk marker in patients with primary mitral regurgitation. J Am Heart Assoc. 2017;6:pii. e006309.
Dilip D, Chandra A, Rajashekhar D, Padmanbhan M. Early beneficial effect of preservation of papillo-annular continuity in mitral valve replacement on left ventricular function. J Heart Valve Dis. 2001;10:294–300.
Coutinho GF, Bihun V, Correia PE, Antunes PE, Antunes MJ. Preservation of the subvalvular apparatus during mitral valve replacement of rheumatic valves does not affect long-term survival. Eur J Cardiothorac Surg. 2015;48:861–7.
Mazine A, Friedrich JO, Nedadur R, et al. Systematic review and meta-analysis of chordal replacement versus leaflet resection for posterior mitral leaflet prolapse. J Thorac Cardiovasc Surg. 2018;155:120–8.
Pandis D, Grapsa J, Athanasiou T, Punjabi P, Nihoyannopoulos P. Left ventricular remodeling and mitral valve surgery: Prospective study with real-time 3-dimensional echocardiography and speckle tracking. J Thorac Cardiovasc Surg. 2011;142:641–9.
Gaasch WH, Meyer TE. Left ventricular response to mitral regurgitation implications for management. Circulation. 2008;118:2298–303.
Chipeta P, Shim CY, Hong GR, et al. Time course of left atrial reverse remodelling after mitral valve surgery and the impact of left ventricular global longitudinal strain in patients with chronic severe mitral regurgitation. Interact Cardiovasc Thorac Surg. 2016;23:876–82.
Antonini-Canterin F, Beladan CC, Popescu BA, et al. Left atrial remodelling early after mitral valve repair for degenerative mitral regurgitation. Heart. 2008;94:759–64.
Witkowski TG, Thomas JD, Delgado V, et al. Changes in left ventricular function after mitral valve repair for severe organic mitral regurgitation. Ann Thorac Surg. 2012;93:754–60.
Tribouilloy C, Rusinaru D, Szymanski C, et al. Predicting left ventricular dysfunction after valve repair for mitral regurgitation due to leaflet prolapse: additive value of left ventricular end-systolic dimension to ejection fraction. Eur J Echocardiogr. 2011;12:702–10.
Witkowski TG, Thomas JD, Debonnaire PJ, et al. Global longitudinal strain predicts left ventricular dysfunction after mitral valve repair. Eur Heart J Cardiovasc Imaging. 2013;14:69–76.
Funding
None
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Statement of human rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of King George’s Medical University, U.P. Institutional ethical committee, (Ref. code: 89 ECM IIB-thesis /P51) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Statement on the welfare of animals
This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Singh, V., Kumar, S., Bhandari, M. et al. Global longitudinal strain: is it a superior assessment method for left ventricular function in patients with chronic mitral regurgitation undergoing mitral valve replacement?. Indian J Thorac Cardiovasc Surg 36, 119–126 (2020). https://doi.org/10.1007/s12055-019-00854-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12055-019-00854-7