Abstract
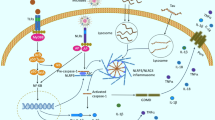
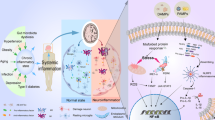
We aim to investigate the mechanisms underlying the beneficial effects of exercise rehabilitation (ER) and/or astragaloside (AST) in counteracting amyloid-beta (Aβ) pathology. Aβ oligomers were microinjected into the bilateral ventricles to induce Aβ neuropathology in rats. Neurobehavioral functions were evaluated. Cortical and hippocampal expressions of both BDNF/TrkB and cathepsin D were determined by the western blotting method. The rat primary cultured cortical neurons were incubated with BDNF and/or AST and ANA12 followed by exposure to aggregated Aβ for 24 h. In vivo results showed that ER and/or AST reversed neurobehavioral disorders, downregulation of cortical and hippocampal expression of both BDNF/TrkB and cathepsin D, neural pathology, Aβ accumulation, and altered microglial polarization caused by Aβ. In vitro studies also confirmed that topical application of BDNF and/or AST reversed the Aβ-induced cytotoxicity, apoptosis, mitochondrial distress, and synaptotoxicity and decreased expression of p-TrkB, p-Akt, p-GSK3β, and β-catenin in rat cortical neurons. The beneficial effects of combined ER (or BDNF) and AST therapy in vivo and in vitro were superior to ER (or BDNF) or AST alone. Furthermore, we observed that any gains from ER (or BDNF) and/or AST could be significantly eliminated by ANA-12, a potent BDNF/TrkB antagonist. These results indicate that whereas ER (or BDNF) and/or AST attenuate Aβ pathology by reversing BDNF/TrkB signaling deficits and mitochondrial dysfunction, combining these two potentiates each other’s therapeutic effects. In particular, AST can be an alternative therapy to replace ER.








Similar content being viewed by others
Availability of Data and Materials
The authors confirm that the data supporting the findings of this study are all available within the article.
Change history
03 May 2022
A Correction to this paper has been published: https://doi.org/10.1007/s12035-022-02842-2
Abbreviations
- Aβ:
-
Amyloid-beta
- p-Akt:
-
Phosphorylated serine/threonine-protein kinase
- T-Akt:
-
Total form serine/threonine-protein kinase
- ANA12:
-
N-[2-[[(Hexahydro-2-oxo-1H-azepin-3-yl)amino]carbonyl]phenyl] benzo[b]thiophene-2-carboxamide
- AST:
-
Astragaloside
- BDNF:
-
Brain-derived neurotrophic factor
- CTSD:
-
Cathepsin D
- DAPI:
-
4′,6-Diamidino-2-phenylindole
- ECL:
-
Enhanced chemiluminescence
- ER:
-
Exercise rehabilitation
- GSK3β:
-
Glycogen synthase kinase-3 beta
- i.c.v.:
-
Intracerebroventricular
- i.p.:
-
Intraperitoneal
- Iba-1:
-
Ionized calcium-binding adaptor molecule 1
- NeuN:
-
Neuronal nuclei
- PBS:
-
Phosphate-buffered saline
- RIPA:
-
Radioimmunoprecipitation assay buffer
- SDS-PAGE:
-
Sodium dodecyl sulfate–polyacrylamide gel electrophoresis
- p-TrkB:
-
Phosphorylated tropomyosin receptor kinase B
- T-TrkB:
-
Total tropomyosin receptor kinase B
- TUNEL:
-
Terminal deoxyribonucleotide transferase-mediated dUTP nick end labeling
References
Choi SH, Bylykbashi E, Chatila ZK, Lee SW, Pulli B, Clemenson GD, Kim E, Rompala A, Oram MK, Asselin C, Aronson J, Zhang C, Miller SJ, Lesinski A, Chen JW, Kim DY, van Praag H, Spiegelman BM, Gage FH, Tanzi RE (2018) Combined adult neurogenesis and BDNF mimic exercise effects on cognition in an Alzheimer’s mouse model. Sci (N Y, NY) 361(6406):eaan8821. https://doi.org/10.1126/science.aan8821
Allen SJ, Watson JJ, Dawbarn D (2011) The neurotrophins and their role in Alzheimer’s disease. Curr Neuropharmacol 9(4):559–573. https://doi.org/10.2174/157015911798376190
Chang CP, Liu YF, Lin HJ, Hsu CC, Cheng BC, Liu WP, Lin MT, Hsu SF, Chang LS, Lin KC (2016) Beneficial effect of astragaloside on Alzheimer’s disease condition using cultured primary cortical cells under β-amyloid exposure. Mol Neurobiol 53(10):7329–7340. https://doi.org/10.1007/s12035-015-9623-2
Polat E, Bedir E, Perrone A, Piacente S, Alankus-Caliskan O (2010) Triterpenoid saponins from Astragalus wiedemannianus Fischer. Phytochemistry 71(5–6):658–662. https://doi.org/10.1016/j.phytochem.2009.11.013
Li WZ, Wu WY, Huang DK, Yin YY, Kan HW, Wang X, Yao YY, Li WP (2012) Protective effects of astragalosides on dexamethasone and Aβ25-35 induced learning and memory impairments due to decrease amyloid precursor protein expression in 12-month male rats. Food chem toxicol : int j published British Ind Biol Res Assoc 50(6):1883–1890. https://doi.org/10.1016/j.fct.2012.03.064
Tohda C, Tamura T, Matsuyama S, Komatsu K (2006) Promotion of axonal maturation and prevention of memory loss in mice by extracts of Astragalus mongholicus. Br J Pharmacol 149(5):532–541. https://doi.org/10.1038/sj.bjp.0706865
Sun Q, Jia N, Wang W, Jin H, Xu J, Hu H (2014) Protective effects of astragaloside IV against amyloid beta1-42 neurotoxicity by inhibiting the mitochondrial permeability transition pore opening. PLoS ONE 9(6):e98866. https://doi.org/10.1371/journal.pone.0098866
Ye X, Tai W, Zhang D (2012) The early events of Alzheimer’s disease pathology: from mitochondrial dysfunction to BDNF axonal transport deficits. Neurobiol Aging 33(6):1122.e1121–1110. https://doi.org/10.1016/j.neurobiolaging.2011.11.004
Hsu CC, Kuo TW, Liu WP, Chang CP, Lin HJ (2020) Calycosin preserves BDNF/TrkB signaling and reduces post-stroke neurological injury after cerebral ischemia by reducing accumulation of hypertrophic and TNF-α-containing microglia in rats. J neuroimmune pharm: j Soc NeuroImmune Pharm. https://doi.org/10.1007/s11481-019-09903-9
Kilkenny C, Browne WJ, Cuthill IC, Emerson M, Altman DG (2010) Improving bioscience research reporting: the ARRIVE guidelines for reporting animal research. PLoS Biol 8(6):e1000412. https://doi.org/10.1371/journal.pbio.1000412
Du Z, Song Y, Chen X, Zhang W, Zhang G, Li H, Chang L, Wu Y (2021) Knockdown of astrocytic Grin2a aggravates β-amyloid-induced memory and cognitive deficits through regulating nerve growth factor. Aging Cell 20(8):e13437. https://doi.org/10.1111/acel.13437
Kantar Gok D, Hidisoglu E, Ocak GA, Er H, Acun AD, Yargıcoglu P (2018) Protective role of rosmarinic acid on amyloid beta 42-induced echoic memory decline: implication of oxidative stress and cholinergic impairment. Neurochem Int 118:1–13. https://doi.org/10.1016/j.neuint.2018.04.008
Kim BK, Shin MS, Kim CJ, Baek SB, Ko YC, Kim YP (2014) Treadmill exercise improves short-term memory by enhancing neurogenesis in amyloid beta-induced Alzheimer disease rats. Journal of exercise rehabilitation 10(1):2–8. https://doi.org/10.12965/jer.140086
Chio CC, Lin MT, Chang CP, Lin HJ (2016) A positive correlation exists between neurotrauma and TGF-β1-containing microglia in rats. Eur J Clin Invest 46(12):1063–1069. https://doi.org/10.1111/eci.12693
Turégano L, Martínez-Rodríguez R, Alvarez MI, Gragera RR, Gómez de Segura A, De Miguel E, Toledano A (2001) Histochemical study of acute and chronic intraperitoneal nicotine effects on several glycolytic and Krebs cycle dehydrogenase activities in the frontoparietal cortex and subcortical nuclei of the rat brain. J Neurosci Res 64(6):626–635. https://doi.org/10.1002/jnr.1116
Baluchnejadmojarad T, Mohamadi-Zarch SM, Roghani M (2019) Safranal, an active ingredient of saffron, attenuates cognitive deficits in amyloid β-induced rat model of Alzheimer’s disease: underlying mechanisms. Metab Brain Dis 34(6):1747–1759. https://doi.org/10.1007/s11011-019-00481-6
Ionita R, Postu PA, Beppe GJ, Mihasan M, Petre BA, Hancianu M, Cioanca O, Hritcu L (2017) Cognitive-enhancing and antioxidant activities of the aqueous extract from Markhamia tomentosa (Benth.) K. Schum. stem bark in a rat model of scopolamine. Behav brain funct : BBF 13(1):5. https://doi.org/10.1186/s12993-017-0123-6
Huang TC, Lu KT, Wo YY, Wu YJ, Yang YL (2011) Resveratrol protects rats from Aβ-induced neurotoxicity by the reduction of iNOS expression and lipid peroxidation. PLoS ONE 6(12):e29102. https://doi.org/10.1371/journal.pone.0029102
Honório JE Jr, Vasconcelos GS, Rodrigues FT, Sena Filho JG, Barbosa-Filho JM, Aguiar CC, Leal LK, Soares PM, Woods DJ, Fonteles MM, Vasconcelos SM (2012) Monocrotaline: histological damage and oxidant activity in brain areas of mice. Oxid Med Cell Longev 2012:697541. https://doi.org/10.1155/2012/697541
Liu X, Gu X, Li Z, Li X, Li H, Chang J, Chen P, Jin J, Xi B, Chen D, Lai D, Graham RM, Zhou M (2006) Neuregulin-1/erbB-activation improves cardiac function and survival in models of ischemic, dilated, and viral cardiomyopathy. J Am Coll Cardiol 48(7):1438–1447. https://doi.org/10.1016/j.jacc.2006.05.057
Zhang Z, Obianyo O, Dall E, Du Y, Fu H, Liu X, Kang SS, Song M, Yu SP, Cabrele C, Schubert M, Li X, Wang JZ, Brandstetter H, Ye K (2017) Inhibition of delta-secretase improves cognitive functions in mouse models of Alzheimer’s disease. Nat Commun 8:14740. https://doi.org/10.1038/ncomms14740
Qin L, Crews FT (2012) NADPH oxidase and reactive oxygen species contribute to alcohol-induced microglial activation and neurodegeneration. J Neuroinflammation 9:5. https://doi.org/10.1186/1742-2094-9-5
Shah SA, Yoon GH, Ahmad A, Ullah F, Ul Amin F, Kim MO (2015) Nanoscale-alumina induces oxidative stress and accelerates amyloid beta (Aβ) production in ICR female mice. Nanoscale 7(37):15225–15237. https://doi.org/10.1039/c5nr03598h
Su C, Chen Y, Chen Y, Zhou Y, Li L, Lu Q, Liu H, Luo X, Zhu J (2019) Effect of electroacupuncture at the ST36 and GB39 acupoints on apoptosis by regulating the p53 signaling pathway in adjuvant arthritis rats. Mol Med Rep 20(5):4101–4110. https://doi.org/10.3892/mmr.2019.10674
Wang YL, Lin CH, Chen CC, Chang CP, Lin KC, Su FC, Chou W (2019) Exercise preconditioning attenuates neurological injury by preserving old and newly formed HSP72-containing neurons in focal brain ischemia rats. Int J Med Sci 16(5):675–685. https://doi.org/10.7150/ijms.32962
Chang CK, Chou W, Lin HJ, Huang YC, Tang LY, Lin MT, Chang CP (2014) Exercise preconditioning protects against spinal cord injury in rats by upregulating neuronal and astroglial heat shock protein 72. Int J Mol Sci 15(10):19018–19036. https://doi.org/10.3390/ijms151019018
Chio CC, Lin HJ, Tian YF, Chen YC, Lin MT, Lin CH, Chang CP, Hsu CC (2017) Exercise attenuates neurological deficits by stimulating a critical HSP70/NF-κB/IL-6/synapsin I axis in traumatic brain injury rats. J Neuroinflammation 14(1):90. https://doi.org/10.1186/s12974-017-0867-9
Connor B, Young D, Yan Q, Faull RL, Synek B, Dragunow M (1997) Brain-derived neurotrophic factor is reduced in Alzheimer’s disease. Brain Res Mol Brain Res 49(1–2):71–81. https://doi.org/10.1016/s0169-328x(97)00125-3
Ginsberg SD, Alldred MJ, Counts SE, Cataldo AM, Neve RL, Jiang Y, Wuu J, Chao MV, Mufson EJ, Nixon RA, Che S (2010) Microarray analysis of hippocampal CA1 neurons implicates early endosomal dysfunction during Alzheimer’s disease progression. Biol Psychiat 68(10):885–893. https://doi.org/10.1016/j.biopsych.2010.05.030
Michalski B, Fahnestock M (2003) Pro-brain-derived neurotrophic factor is decreased in parietal cortex in Alzheimer’s disease. Brain Res Mol Brain Res 111(1–2):148–154. https://doi.org/10.1016/s0169-328x(03)00003-2
Peng S, Wuu J, Mufson EJ, Fahnestock M (2005) Precursor form of brain-derived neurotrophic factor and mature brain-derived neurotrophic factor are decreased in the pre-clinical stages of Alzheimer’s disease. J Neurochem 93(6):1412–1421. https://doi.org/10.1111/j.1471-4159.2005.03135.x
Devi L, Ohno M (2012) 7,8-dihydroxyflavone, a small-molecule TrkB agonist, reverses memory deficits and BACE1 elevation in a mouse model of Alzheimer’s disease. Neuropsychopharmacol : off publ Am Coll Neuropsychopharmacol 37(2):434–444. https://doi.org/10.1038/npp.2011.191
Peng S, Garzon DJ, Marchese M, Klein W, Ginsberg SD, Francis BM, Mount HT, Mufson EJ, Salehi A, Fahnestock M (2009) Decreased brain-derived neurotrophic factor depends on amyloid aggregation state in transgenic mouse models of Alzheimer’s disease. J neurosci : off j Soc Neurosci 29(29):9321–9329. https://doi.org/10.1523/jneurosci.4736-08.2009
Bemelmans AP, Husson I, Jaquet M, Mallet J, Kosofsky BE, Gressens P (2006) Lentiviral-mediated gene transfer of brain-derived neurotrophic factor is neuroprotective in a mouse model of neonatal excitotoxic challenge. J Neurosci Res 83(1):50–60. https://doi.org/10.1002/jnr.20704
Ma XC, Liu P, Zhang XL, Jiang WH, Jia M, Wang CX, Dong YY, Dang YH, Gao CG (2016) Intranasal delivery of recombinant AAV containing BDNF fused with HA2TAT: a potential promising therapy strategy for major depressive disorder. Sci Rep 6:22404. https://doi.org/10.1038/srep22404
Blurton-Jones M, Kitazawa M, Martinez-Coria H, Castello NA, Müller FJ, Loring JF, Yamasaki TR, Poon WW, Green KN, LaFerla FM (2009) Neural stem cells improve cognition via BDNF in a transgenic model of Alzheimer disease. Proc Natl Acad Sci USA 106(32):13594–13599. https://doi.org/10.1073/pnas.0901402106
Eremenko E, Mittal K, Berner O, Kamenetsky N, Nemirovsky A, Elyahu Y, Monsonego A (2019) BDNF-producing, amyloid β-specific CD4 T cells as targeted drug-delivery vehicles in Alzheimer’s disease. EBioMedicine 43:424–434. https://doi.org/10.1016/j.ebiom.2019.04.019
Makar TK, Trisler D, Eglitis MA, Mouradian MM, Dhib-Jalbut S (2004) Brain-derived neurotrophic factor (BDNF) gene delivery into the CNS using bone marrow cells as vehicles in mice. Neurosci Lett 356(3):215–219. https://doi.org/10.1016/j.neulet.2003.11.045
Mitroshina EV, Yarkov RS, Mishchenko TA, Krut VG, Gavrish MS, Epifanova EA, Babaev AA, Vedunova MV (2020) Brain-derived neurotrophic factor (BDNF) preserves the functional integrity of neural networks in the β-amyloidopathy model in vitro. Front cell dev biol 8:582. https://doi.org/10.3389/fcell.2020.00582
Di Domenico F, Tramutola A, Perluigi M (2016) Cathepsin D as a therapeutic target in Alzheimer’s disease. Expert Opin Ther Targets 20(12):1393–1395. https://doi.org/10.1080/14728222.2016.1252334
Suire CN, Leissring MA (2021) Cathepsin D: a candidate link between amyloid β-protein and tauopathy in Alzheimer disease. J exp neurol 2(1):10–15
Cherry JD, Olschowka JA, O’Banion MK (2014) Neuroinflammation and M2 microglia: the good, the bad, and the inflamed. J Neuroinflammation 11:98. https://doi.org/10.1186/1742-2094-11-98
Seira O, Del Río JA (2014) Glycogen synthase kinase 3 beta (GSK3β) at the tip of neuronal development and regeneration. Mol Neurobiol 49(2):931–944. https://doi.org/10.1007/s12035-013-8571-y
Beurel E, Grieco SF, Jope RS (2015) Glycogen synthase kinase-3 (GSK3): regulation, actions, and diseases. Pharmacol Ther 148:114–131. https://doi.org/10.1016/j.pharmthera.2014.11.016
Reddy PH (2013) Amyloid beta-induced glycogen synthase kinase 3β phosphorylated VDAC1 in Alzheimer’s disease: implications for synaptic dysfunction and neuronal damage. Biochem Biophys Acta 1832(12):1913–1921. https://doi.org/10.1016/j.bbadis.2013.06.012
Salcedo-Tello P, Ortiz-Matamoros A, Arias C (2011) GSK3 function in the brain during development, neuronal plasticity, and neurodegeneration. Int j Alzheimer’s dis 2011:189728. https://doi.org/10.4061/2011/189728
Li Z, Tan F, Thiele CJ (2007) Inactivation of glycogen synthase kinase-3beta contributes to brain-derived neutrophic factor/TrkB-induced resistance to chemotherapy in neuroblastoma cells. Mol Cancer Ther 6(12 Pt 1):3113–3121. https://doi.org/10.1158/1535-7163.Mct-07-0133
Zhao S, Fu J, Liu X, Wang T, Zhang J, Zhao Y (2012) Activation of Akt/GSK-3beta/beta-catenin signaling pathway is involved in survival of neurons after traumatic brain injury in rats. Neurol Res 34(4):400–407. https://doi.org/10.1179/1743132812y.0000000025
Swerdlow RH, Burns JM, Khan SM (2010) The Alzheimer’s disease mitochondrial cascade hypothesis. Journal of Alzheimer's disease : JAD 20 Suppl 2 (Suppl 2):S265–279. https://doi.org/10.3233/jad-2010-100339
Chen HH, Zhang N, Li WY, Fang MR, Zhang H, Fang YS, Ding MX, Fu XY (2015) Overexpression of brain-derived neurotrophic factor in the hippocampus protects against post-stroke depression. Neural Regen Res 10(9):1427–1432. https://doi.org/10.4103/1673-5374.165510
Acknowledgements
We acknowledge Ms. Meng-Tsung Ho for her excellent editorial assistance in manuscript preparation.
Funding
This study was supported by the Taiwan Ministry of Science and Technology (MOST) (grant no. MOST109-2314-B-384–002-MY3, MOST106-2314-B-384 -001 -MY3, MOST 105–2314-B-384 -001 -MY3) and Chi Mei Medical Center (Taiwan) grant CMFHT10802. The funders had no role in the study design, data collection, and analysis, the decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
Study concept and design: WYL, SCK, CCC; acquisition of data: CHY, JTM, WPL; analysis and interpretation of data: WYL, SCK, CHY; drafting of the manuscript: CCC, CPC, KCL; critical revision of the manuscript for important intellectual content: SCK, CCC, MTL; statistical analysis: WYL, JTM, WPL; material support: CCC, CPC, MTL; obtained funding: CCC, CPC, KCL. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics Approval and Consent to Participate
All animal experiments were approved and carried out in accordance with the Institutional Animal Care and Use Committee at the Chi Mei Medical Center, Tainan, Taiwan (approved no. 108120110).
Consent for Publication
Not applicable.
Conflicts of Interest
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Wang, YL., Chio, CC., Kuo, SC. et al. Exercise Rehabilitation and/or Astragaloside Attenuate Amyloid-beta Pathology by Reversing BDNF/TrkB Signaling Deficits and Mitochondrial Dysfunction. Mol Neurobiol 59, 3091–3109 (2022). https://doi.org/10.1007/s12035-022-02728-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-022-02728-3