Abstract
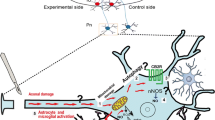
Remote damage is a secondary phenomenon that usually occurs after a primary brain damage in regions that are distant, yet functionally connected, and that is critical for determining the outcomes of several CNS pathologies, including traumatic brain and spinal cord injuries. The understanding of remote damage-associated mechanisms has been mostly achieved in several models of focal brain injury such as the hemicerebellectomy (HCb) experimental paradigm, which helped to identify the involvement of many key players, such as inflammation, oxidative stress, apoptosis and autophagy. Currently, few interventions have been shown to successfully limit the progression of secondary damage events and there is still an unmet need for new therapeutic options. Given the emergence of the novel concept of resolution of inflammation, mediated by the newly identified ω3-derived specialized pro-resolving lipid mediators, such as resolvins, we reported a reduced ability of HCb-injured animals to produce resolvin D1 (RvD1) and an increased expression of its target receptor ALX/FPR2 in remote brain regions. The in vivo administration of RvD1 promoted functional recovery and neuroprotection by reducing the activation of Iba-1+ microglia and GFAP+ astrocytes as well as by impairing inflammatory-induced neuronal cell death in remote regions. These effects were counteracted by intracerebroventricular neutralization of ALX/FPR2, whose activation by RvD1 also down-regulated miR-146b- and miR-219a-1-dependent inflammatory markers. In conclusion, we propose that innovative therapies based on RvD1-ALX/FPR2 axis could be exploited to curtail remote damage and enable neuroprotective effects after acute focal brain damage.





Similar content being viewed by others
Abbreviations
- GFAP:
-
Glial fibrillary acidic protein
- HCb:
-
Hemicerebellectomy
- Rv:
-
Resolvin
- RvD1:
-
Resolvin D1
- SPM:
-
Specialized pro-resolving mediators
References
Tator CH (1995) Update on the pathophysiology and pathology of acute spinal cord injury. Brain Pathol 5(4):407–413. https://doi.org/10.1111/j.1750-3639.1995.tb00619.x
Park E, Velumian AA, Fehlings MG (2004) The role of excitotoxicity in secondary mechanisms of spinal cord injury: a review with an emphasis on the implications for white matter degeneration. J Neurotrauma 21(6):754–774. https://doi.org/10.1089/0897715041269641
Viscomi MT, Molinari M (2014) Remote neurodegeneration: multiple actors for one play. Mol Neurobiol 50(2):368–389. https://doi.org/10.1007/s12035-013-8629-x
Viscomi MT, Florenzano F, Latini L, Amantea D, Bernardi G, Molinari M (2008) Methylprednisolone treatment delays remote cell death after focal brain lesion. Neuroscience 154(4):1267–1282. https://doi.org/10.1016/j.neuroscience.2008.04.024
Viscomi MT, Latini L, Florenzano F, Bernardi G, Molinari M (2008) Minocycline attenuates microglial activation but fails to mitigate degeneration in inferior olive and pontine nuclei after focal cerebellar lesion. Cerebellum 7:401–405
Block F, Dihne M, Loos M (2005) Inflammation in areas of remote changes following focal brain lesion. Prog Neurobiol 75:34–365
Cavallucci V, Bisicchia E, Cencioni MT, Ferri A, Latini L, Nobili A, Biamonte F, Nazio F et al (2014) Acute focal brain damage alters mitochondrial dynamics and autophagy in axotomized neurons. Cell Death Dis 5(11):e1545. https://doi.org/10.1038/cddis.2014.511
Viscomi MT, Latini L, Bisicchia E, Sasso V, Molinari M (2015) Remote degeneration: insights from the hemicerebellectomy model. Cerebellum 14:15–18
Nathan C, Ding A (2010) Nonresolving inflammation. Cell 140(6):871–882. https://doi.org/10.1016/j.cell.2010.02.029
Kotas ME, Medzhitov R (2015) Homeostasis, inflammation, and disease susceptibility. Cell 160(5):816–827. https://doi.org/10.1016/j.cell.2015.02.010
Serhan CN (2014) Pro-resolving lipid mediators are leads for resolution physiology. Nature 510(7503):92–101. https://doi.org/10.1038/nature13479
Basil MC, Levy BD (2016) Specialized pro-resolving mediators: endogenous regulators of infection and inflammation. Nat Rev Immunol 16(1):51–67. https://doi.org/10.1038/nri.2015.4
Serhan CN (2017) Treating inflammation and infection in the 21st century: new hints from decoding resolution mediators and mechanisms. FASEB J 31(4):1273–1288. https://doi.org/10.1096/fj.201601222R
Bazan NG (2007) Omega-3 fatty acids, pro-inflammatory signaling and neuroprotection. Curr Opin Clin Nutr Metab Care 10(2):136–141. https://doi.org/10.1097/MCO.0b013e32802b7030
Michael-Titus AT, Priestley JV (2014) Omega-3 fatty acids and traumatic neurological injury: from neuroprotection to neuroplasticity? Trends Neurosci 37(1):30–38. https://doi.org/10.1016/j.tins.2013.10.005
Samaddar R (2016) Effect of docosahexaenoic acid (DHA) on spinal cord injury. Adv Neurobiol 12:27–39. https://doi.org/10.1007/978-3-319-28383-8_2
Bisicchia E, Chiurchiù V, Viscomi MT, Latini L, Fezza F, Battistini L, Maccarrone M, Molinari M (2013) Activation of type-2 cannabinoid receptor inhibits neuroprotective and antiinflammatory actions of glucocorticoid receptor alpha: when one is better than two. Cell Mol Life Sci 70(12):2191–2204. https://doi.org/10.1007/s00018-012-1253-5
Kongsui R, Beynon SB, Johnson SJ, Walker FR (2014) Quantitative assessment of microglial morphology and density reveals remarkable consistency in the distribution and morphology of cells within the healthy prefrontal cortex of the rat. J Neuroinflammation 11(1):182. https://doi.org/10.1186/s12974-014-0182-7
Chiurchiù V, Leuti A, Dalli J, Jacobsson A, Battistini L, Maccarrone M, Serhan CN (2016) Proresolving lipid mediators resolvin D1, resolvin D2, and maresin 1 are critical in modulating T cell responses. Sci Transl Med 8:353ra111
Catanzaro G, Besharat ZM, Garg N, Ronci M, Pieroni L, Miele E, Mastronuzzi A, Carai A et al (2016) MicroRNAs-proteomic networks characterizing human medulloblastoma-SLCs. Stem Cells Int 2016:2683042–2683010. https://doi.org/10.1155/2016/2683042
Betel D, Wilson M, Gabow A, Marks DS, Sander C (2008) The microRNA.org resource: targets and expression. Nucleic Acids Res 36(Database issue):D149–D153. https://doi.org/10.1093/nar/gkm995
Betel D, Koppal A, Agius P, Sander C, Leslie C (2010) Comprehensive modeling of microRNA targets predicts functional non-conserved and non-canonical sites. Genome Biol 11(8):R90. https://doi.org/10.1186/gb-2010-11-8-r90
Recchiuti A, Krishnamoorthy S, Fredman G, Chiang N, Serhan CN (2011) MicroRNAs in resolution of acute inflammation: identification of novel resolvin D1-miRNA circuits. FASEB J 25(2):544–560
Rius B, Titos E, Morán-Salvador E, López-Vicario C, García-Alonso V, González-Périz A, Arroyo V, Clària J (2014) Resolvin D1 primes the resolution process initiated by calorie restriction in obesity-induced steatohepatitis. FASEB J 28(2):836–848. https://doi.org/10.1096/fj.13-235614
Bays HE (2007) Safety considerations with omega-3 fatty acid therapy. Am J Cardiol 99(6A):35C–43C. https://doi.org/10.1016/j.amjcard.2006.11.020
Chiurchiù V, Maccarrone M (2011) Chronic inflammatory disorders and their redox control: from molecular mechanisms to therapeutic opportunities. Antiox Redox Signal 15(9):2605–2641. https://doi.org/10.1089/ars.2010.3547
Hall JC, Priestley JV, Perry VH, Michael-Titus AT (2012) Docosahexaenoic acid, but not eicosapentaenoic acid, reduces the early inflammatory response following compression spinal cord injury in the rat. J Neurochem 121(5):738–750. https://doi.org/10.1111/j.1471-4159.2012.07726.x
Wang X, Zhu M, Hjorth E, Cortés-Toro V, Eyjolfsdottir H, Graff C, Nennesmo I, Palmblad J et al (2015) Resolution of inflammation is altered in Alzheimer’s disease. Alzheimers Dement 11(1):40–50 e41–42
Kong Y, Ruan L, Qian L, Liu X, Le Y (2010) Norepinephrine promotes microglia to uptake and degrade amyloid beta peptide through upregulation of mouse formyl peptide receptor 2 and induction of insulin-degrading enzyme. J Neurosci 30(35):11848–11857. https://doi.org/10.1523/JNEUROSCI.2985-10.2010
Wang G, Zhang L, Chen X, Xue X, Guo Q, Liu M, Zhao J (2016) Formylpeptide receptors promote the migration and differentiation of rat neural stem cells. Sci Rep 6:25946
Zhang L, Wang G, Chen X, Xue X, Guo Q, Liu M, Zhao J (2017) Formyl peptide receptors promotes neural differentiation in mouse neural stem cells by ROS generation and regulation of PI3K-AKT signaling. Sci Rep 7(1):206
Sofroniew MV, Vinters HV (2010) Astrocytes: biology and pathology. Acta Neuropathol 119(1):7–35. https://doi.org/10.1007/s00401-009-0619-8
Jensen CJ, Massie A, De Keyser J (2013) Immune players in the CNS: the astrocyte. J NeuroImmune Pharmacol 8(4):824–839
Zhu M, Wang X, Hjorth E, Colas RA, Schroeder L, Granholm AC, Serhan CN, Schultzberg M (2016) Pro-resolving lipid mediators improve neuronal survival and increase Abeta42 phagocytosis. Mol Neurobiol 53(4):2733–2749. https://doi.org/10.1007/s12035-015-9544-0
Nayak D, Roth TL, McGavern DB (2014) Microglia development and function. Annu Rev Immunol 32(1):367–402. https://doi.org/10.1146/annurev-immunol-032713-120240
Beynon SB, Walker FR (2012) Microglial activation in the injured and healthy brain: what are we really talking about? Practical and theoretical issues associated with the measurement of changes in microglial morphology. Neuroscience 225:162–171. https://doi.org/10.1016/j.neuroscience.2012.07.029
Xu ZZ, Berta T, Ji RR (2013) Resolvin E1 inhibits neuropathic pain and spinal cord microglial activation following peripheral nerve injury. J NeuroImmune Pharmacol 8(1):37–41. https://doi.org/10.1007/s11481-012-9394-8
Rey C, Nadjar A, Buaud B, Vaysse C, Aubert A, Pallet V, Layé S, Joffre C (2016) Resolvin D1 and E1 promote resolution of inflammation in microglial cells in vitro. Brain Behav Immun 55:249–259. https://doi.org/10.1016/j.bbi.2015.12.013
Li L, Wu Y, Wang Y, Wu J, Song L, Xian W, Yuan S, Pei L et al (2014) Resolvin D1 promotes the interleukin-4-induced alternative activation in BV-2 microglial cells. J Neuroinflammation 11(1):72. https://doi.org/10.1186/1742-2094-11-72
Sheets KG, Jun B, Zhou Y, Zhu M, Petasis NA, Gordon WC, Bazan NG (2013) Microglial ramification and redistribution concomitant with the attenuation of choroidal neovascularization by neuroprotectin D1. Mol Vis 19:1747–1759
Biswas SK, Chittezhath M, Shalova IN, Lim JY (2012) Macrophage polarization and plasticity in health and disease. Immunol Res 53(1-3):11–24. https://doi.org/10.1007/s12026-012-8291-9
Bartel DP (2009) MicroRNAs: target recognition and regulatory functions. Cell 136(2):215–233. https://doi.org/10.1016/j.cell.2009.01.002
Sheedy FJ, O’Neill LAJ (2008) Adding fuel to fire: microRNAs as a new class of mediators of inflammation. Ann Rheum 67:iii50–iii55
O’Neill LA, Sheedy FJ, McCoy CE (2011) MicroRNAs: the fine-tuners of toll-like receptor signalling. Nat Rev Immunol 11(3):163–175. https://doi.org/10.1038/nri2957
Codagnone M, Cianci E, Lamolinara A, Mari VC, Nespoli A, Isopi E, Mattoscio D, Arita M, Bragonzi A, Iezzi M, Romano M, Recchiuti A (2017) Resolvin D1 enhances the resolution of lung inflammation caused by long-term Pseudomonas aeruginosa infection. Mucosal Immunol
Molteni M, Gemma S, Rossetti C (2016) The role of toll-like receptor 4 in infectious and noninfectious inflammation. Mediat Inflamm 2016:6978936. https://doi.org/10.1155/2016/6978936
Caiello I, Minnone G, Holzinger D, Vogl T, Prencipe G, Manzo A, De Benedetti F, Strippoli R (2014) IL-6 amplifies TLR mediated cytokine and chemokine production: implications for the pathogenesis of rheumatic inflammatory diseases. PLoS One 9(10):e107886. https://doi.org/10.1371/journal.pone.0107886
Funding
This work was funded by Fondazione Italiana Sclerosi Multipla (FISM) (grant 2015/R/8 to V.C.) and by the Italian Ministry of Health (Progetto Giovani Ricercatori Project Code GR-2010.2310524 to M.T.V.).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Maria Teresa Viscomi and Valerio Chiurchiù equally senior authors
Rights and permissions
About this article
Cite this article
Bisicchia, E., Sasso, V., Catanzaro, G. et al. Resolvin D1 Halts Remote Neuroinflammation and Improves Functional Recovery after Focal Brain Damage Via ALX/FPR2 Receptor-Regulated MicroRNAs. Mol Neurobiol 55, 6894–6905 (2018). https://doi.org/10.1007/s12035-018-0889-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-018-0889-z