Abstract
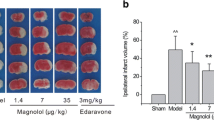
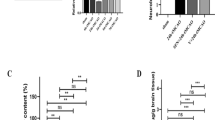
Administration of recombinant human erythropoietin (rhEPO) protects neurons from injury after brain ischemia–reperfusion (I/R), which is in part mediated by ameliorating the blood–brain barrier (BBB) leakage. But the mechanism of rhEPO’s protective effects on BBB remains unclear. This study aims to investigate the effects of rhEPO on BBB integrity and the expressions of tight junctions (TJs) associated proteins of zonula occluden-1 (ZO-1), occludin, and claudin-5 in cerebral I/R rats. These rats underwent 2 h of ischemia and then were reperfused for up to 3 and 72 h. Animals were randomly divided into five groups: sham-operated group, I/R 3 h and I/R 72 h group (2 ml saline was injected intraperitoneally just before the onset of ischemia), rhEPO + I/R 3 h, and rhEPO + I/R 72 h group (5,000 U/kg rhEPO diluted in 2 ml saline solution was injected intraperitoneally just before the onset of ischemia). We verified that rhEPO could decrease the BBB leakage induced by I/R injury detected by Evans blue extravasation. 2, 3, 5-Triphenyltetrazolium chloride staining results showed that rhEPO decreased infarct volume after cerebral I/R. TJ integrity was partly restored by rhEPO observed by transmission electron microscopy. The mRNA and protein expression levels of ZO-1, occludin, and claudin-5 were significantly increased compared with I/R groups at the same reperfusion time point by reverse transcriptase-polymerase chain reaction and Western blot assays. The treatment of rhEPO induced the redistribution of ZO-1, occludin, and claudin-5 in cerebral microvessels observed by immunohistochemical staining. Compared with I/R groups, the mRNA level of tumor necrosis factor-alpha (TNF-α) in cerebral microvessels decreased markedly after rhEPO treatment, accompanied with reduced TNF-α protein level and nuclear factor-кB (NF–кB) p65 activation detected by enzyme-linked immunosorbent assay. These results suggested that the protective mechanism of rhEPO on BBB after cerebral I/R injury was associated with the upregulation of TJ-associated proteins. The downregulated TNF-α levels and NF–кB activation induced by rhEPO might be involved in this process.











Similar content being viewed by others
References
Aslam M, Ahmad N, Srivastava R, Hemmer B (2012) TNF-alpha induced NFκB signaling and p65 (RelA) overexpression repress Cldn5 promoter in mouse brain endothelial cells. Cytokine 57(2):269–275
Bachekapili N, Uzum G, Gokkusu C, Kuru A, Ziylan YZ (2007) The relationship between erythropoietin pretreatment with blood–brain barrier and lipid peroxidation after ischemia/reperfusion in rats. Life Sci 80(14):1245–1251
Bernaudin M, Marti HH, Roussel S, Divoux D, Nouvelot A, MacKenzie ET, Petit E (1999) A potential role for erythropoietin in focal permanent cerebral ischemia in mice. J Cereb Blood Flow Metab 19(6):643–651
Biegel D, Spencer DD, Pachter JS (1995) Isolation and culture of human brain microvessel endothelial cells for the study of blood–brain barrier properties in vitro. Brain Res 692(1–2):183–189
Brines M, Cerami A (2006) Discovering erythropoietin’s extra-hematopoietic functions: biology and clinical promise. Kidney Int 70(2):246–250
Brines ML, Ghezzi P, Keenan S, Agnello D, de Lanerolle NC, Cerami C, Irti LM, Cerami A (2000) Erythropoietin crosses the blood–brain barrier to protect against experimental brain injury. Proc Natl Acad Sci U S A 97(19):10526–10531
Chin K, Yu X, Beleslin-Cokic B, Liu C, Shen K, Mohrenweiser HW, Noguchi CT (2000) Production and processing of erythropoietin receptor transcripts in brain. Brain Res Mol Brain Res 81(1–2):29–42
Correale J, Villa A (2009) Cellular elements of the blood–brain barrier. Neurochem Res 34(12):2067–2077
del Zoppo GJ (1994) Microvascular changes during cerebral ischemia and reperfusion. Cerebrovasc Brain Metab Rev 6(1):47–96
Hacke W, Schwab S, Horn M, Spranger M, De Georgia M, von Kummer R (1996) Malignant middle cerebral artery territory infarction: clinical course and prognostic signs. Arch Neurol 53(4):309–315
Hasselblatt M, Ehrenreich H, Siren AL (2006) The brain erythropoietin system and its potential for therapeutic exploitation in brain disease. J Neurosurg Anesthesiol 18(2):132–138
Hossmann KA (1993) Ischemia-mediated neuronal injury. Resuscitation 26(3):225–235
Huang ZG, Xue D, Preston E, Karbalai H, Buchan AM (1999) Biphasic opening of the blood–brain barrier following transient focal ischemia: effects of hypothermia. Can J Neurol Sci 26(4):298–304
Jelkmann W (2007) Erythropoietin after a century of research: younger than ever. Eur J Haematol 78(3):183–205
Jiao HX, Wang ZH, Liu YH, Wang P, Xue YX (2011) Specific role of tight junction proteins claudin-5, occludin, and ZO-1 of the blood–brain barrier in a focal cerebral ischemic insult. J Mol Neurosci 44(2):130–139
Kawakami M, Sekiguchi M, Sato K, Kozak S, Takahashi M (2001) Erythropoietin receptor-mediated inhibition of exocytotic glutamate release confers neuroprotection during chemical ischemia. J Biol Chem 276(42):39469–39475
Kumral A, Genc S, Ozer E, Yilmaz O, Gokmen N, Koroglu TF, Duman N, Genc K, Ozkan H (2006) Erythropoietin downregulates bax and DP5 proapoptotic gene expression in neonatal hypoxic-ischemic brain injury. Biol Neonate 89(3):205–210
Kuribayashi M, Wang J, Fujiwara O, Doi Y, Nabae K, Tamano S, Ogiso T, Asamoto M, Shirai T (2005) Lack of effects of 1439 MHz electromagnetic near field exposure on the blood–brain barrier in immature and young rats. Bioelectromagnetics 26(7):578–588
Kuroiwa T, Ting P, Martinez H, Klatzo I (1985) The biphasic opening of the blood-brain barrier to proteins following temporary middle cerebral artery occlusion. Acta Neuropathol 68(2):122–129
Li Y, Lu Z, Keogh CL, Yu SP, Wei L (2007) Erythropoietin-induced neurovascular protection, angiogenesis, and cerebral blood flow restoration after focal ischemia in mice. J Cereb Blood Flow Metab 27(5):1043–1054
Li Y, Ogle ME, Wallace GC 4th, Lu ZY, Yu SP, Wei L (2008) Erythropoietin attenuates intracerebral hemorrhage by diminishing matrix metalloproteinases and maintaining blood–brain barrier integrity in mice. Acta Neurochir Suppl 105:105–112
Longa EZ, Weinstein PR, Carlson S, Cummins R (1989) Reversible middle cerebral artery occlusion without craniectomy in rats. Stroke 20(1):84–91
Ma TY, Iwamoto GK, Hoa NT, Akotia V, Pedram A, Boivin MA, Said HM (2004) TNF-alpha-induced increase in intestinal epithelial tight junction permeability requires NF-kappa B activation. Am J Physiol Gastrointest Liver Physiol 286(3):G367–G376
Marti HH (2004) Erythropoietin and the hypoxic brain. Exp Biol 207(pt 18):3233–3242
Martínez-Estrada OM, Rodríguez-Millán E, González-De Vicente E, Reina M, Vilaró S, Fabre M (2003) Erythropoietin protects the in vitro blood–brain barrier against VEGF-induced permeability. Eur J Neurosci 18(9):2538–2544
Nagai A, Nakagawa E, Choi HB, Hatori K, Kobayashi S, Kim SU (2001) Erythropoietin and erythropoietin receptors in human CNS neurons, astrocytes, microglia, and oligodendrocytes grown in culture. J Neuropathol Exp Neurol 60(4):386–392
Nishimura Y, Ito T, Saavedra JM (2000) Angiotensin II AT (1) blockade normalizes cerebrovascular autoregulation and reduces cerebral ischemia in spontaneously hypertensive rats. Stroke 31(10):2478–2486
Ohtsuki S, Sato S, Yamaguchi H, Kamio M, Asashima T, Terasaki T (2007) Exogenous expression of claudin-5 induces barrier properties in cultured rat brain capillary endothelial cells. J Cell Physiol 210(1):81–86
Sandoval KE, Witt KA (2008) Blood–brain barrier tight junction permeability and ischemic stroke. Neurobiol Dis 32(2):200–219
Sawada N, Murata M, Kikuchi K, Osanai M, Tobioka H, Kojima T, Chiba H (2003) Tight junctions and human diseases. Med Electron Microsc 36(3):147–156
Schreibelt G, Kooij G, Reijerkerk A, van Doorn R, Gringhuis SL, van der Pol S, Weksler BB, Romero LA, Couraud PO, Piontek J, Blasig IE, Dijkstra CD, Ronken E, de Vries HE (2007) Reactive oxygen species alter brain endothelial tight junction dynamics via RhoA, PI3 kinase, and PKB signaling. FASEB J 21(13):3666–3676
Sheth P, Basuroy S, Li C, Naren AP, Rao RK (2003) Role of phosphatidylinositol 3-kinase in oxidative stress-induced disruption of tight junctions. J Biol Chem 278(49):49239–49245
Shimakura A, Kamanaka Y, Ikeda Y, Kondo K, Suzuki Y, Umemura K (2000) Neutrophil elastase inhibition reduces cerebral ischemia damage in the middle cerebral artery occlusion. Brain Res 858(1):55–60
Siren AL, Knerlich F, Poser W, Gleiter CH, Bruck W, Ehrenreich H (2001) Erythropoietin and erythropoietin receptor in human ischemic/hypoxic brain. Acta Neuropathol 101(3):271–276
Song HL, Lv S, Liu P (2009) The roles of tumor necrosis factor-alpha in colon tight junction protein expression and intestinal mucosa structure in a mouse model of acute liver failure. BMC Gastroenterol 9:70
Takagi K, Ginsberg MD, Globus MY, Dietrich WD, Martinez E, Kraydieh S, Busto R (1993) Changes in amino acid neurotransmitters and cerebral blood flow in the ischemia penumbral region following middle cerebral artery occlusion in the rat: correlation with histopathology. J Cereb Blood Flow Metab 13(4):575–585
Wolburg H, Lippoldt A (2002) Tight junctions of the blood–brain barrier: development, composition and regulation. Vascul Pharmacol 38(6):323–337
Acknowledgements
This work is supported by grants from the Natural Science Foundation of China (nos. 81171131, 81172197, 30973079, 81072056, and 81100893), the special fund for Scientific Research of Doctor-degree Subjects in Colleges and Universities (nos. 20092104110015 and 20102104110009), the Natural Science Foundation of Liaoning Province in China (no. 201102300), Liaoning Science and Technology Plan Projects (no. 2011225020), and Shenyang Science and Technology Plan Projects (nos. F-10-205-1-22 and F-10-205-1-37).
Author information
Authors and Affiliations
Corresponding author
Additional information
Kun Liu, Tao Sun, and Ping Wang contributed equally to this work.
Rights and permissions
About this article
Cite this article
Liu, K., Sun, T., Wang, P. et al. Effects of Erythropoietin on Blood–Brain Barrier Tight Junctions in Ischemia–Reperfusion Rats. J Mol Neurosci 49, 369–379 (2013). https://doi.org/10.1007/s12031-012-9883-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12031-012-9883-5