Abstract
Purpose
Given the potential interference between treatment for metastatic colorectal cancer (mCRC) and surgical procedures, we sought to determine the prevalence of major surgery following mCRC diagnosis in clinical practice.
Methods
This cohort study used physician-surveyed data from the LifeLink™ Oncology Analyzer database for mCRC patients in five European countries (France, Germany, Italy, Spain, and the United Kingdom [UK]). All patients aged ≥21 years at mCRC diagnosis and with data collected during 2009 were included. Major surgical procedures were examined descriptively by the purpose and location of surgery.
Results
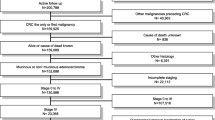
The study sample included 3,249 mCRC patients; 515, 862, 656, 649, and 567 were from France, Germany, Italy, Spain, and the UK, respectively. Following mCRC diagnosis, at least one major surgical procedure for any purpose was seen in 30.5% (UK), 35.2% (Germany), 35.6% (Spain), 36.3% (France), and 38.4% (Italy) of patients, with a mean of 1.3 (UK) to 1.6 (France) procedures. The rate of major surgery for curative purposes was the highest in Italy (13.4%), followed by France (12.8%), Spain (10.3%), and Germany (9.2%); the lowest was in the UK (7.2%). Major surgery performed on the primary tumor (12.4–27.1% of patients, depending on the country) and metastasis (6.4–14.6%) made up the majority of all surgical procedures.
Conclusions
Major surgery is highly prevalent following mCRC diagnosis, suggesting an important role in meeting the goals of mCRC treatment. The role of pharmacological treatment options and their potential to interfere with both surgery use and surgical outcomes should be considered when evaluating mCRC treatment strategies.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
During the last decade, numerous advancements have been made in the treatment of metastatic colorectal cancer (mCRC), including the development of new chemotherapy regimens, the introduction of monoclonal antibodies (mAbs) targeting vascular endothelial growth factor (VEGF) or epidermal growth factor receptor (EGFR), and the optimization of their usage [1–5]. With the exception of the United Kingdom (UK), recent literature has shown that nearly half of patients with mCRC in Europe receive mAb therapy as part of their pharmacological treatment for mCRC [6]. Although mAbs have improved outcomes, they have severe treatment-related toxicities. However, anti-VEGF and anti-EGFR agents have distinct safety profiles [1–5]. Wound-healing complications, a severe adverse event associated with anti-VEGF treatment, interfere with surgical procedures in patients with mCRC [1, 7–10; Avastin SmPC; Avastin PI]. In order to avoid an increased risk of wound-healing complications, the European Society for Medical Oncology (ESMO) clinical guidelines recommend that patients should wait at least 5–8 weeks after cessation of anti-VEGF therapy, specifically bevacizumab, to have surgery and that bevacizumab should not be reinitiated for at least 28 days after surgical operations [10]. Consequently, the potential impact of bevacizumab with regard to wound healing should be considered in all patients undergoing surgical procedures [8].
There are multiple reasons for which patients with mCRC may undergo surgery. Resection with curative intent is possible in some patients with mCRC, of whom approximately 30% remain alive 5 years post-resection [11, 12]. Of particular note is that the ESMO clinical guidelines for advanced CRC indicate that surgical resection should be considered for solitary or confined liver metastases and for resectable lung metastases [10]. As pharmacological therapy may achieve sufficient shrinkage of tumors to allow surgical resection in some patients who were previously considered unresectable (conversion therapy), the National Comprehensive Cancer Network guidelines recommend that eligibility for conversion therapy should be re-evaluated every 2 months [13]. Other cancer-related reasons for surgical procedures also recommended by guidelines include biopsy and surgery in patients with a risk of obstruction or bleeding [13]. While surgery is an important component in the treatment of mCRC, patients with mCRC may also undergo surgical procedures unrelated to their cancer, such as bone fracture repair, and surgery for comorbidities such as heart disease. Given the lack of data quantifying the prevalence of surgery following mCRC diagnosis, this study was designed to evaluate the prevalence of major surgery in patients with mCRC in clinical practice in five European countries.
Methods
Data Source and Elements Extracted
We analyzed data contained within the LifeLink™ Oncology Analyzer™ database from IMS Consulting Group. This database included information on patients with cancer of all types and stages treated by a panel of nearly 2,300 physicians at hospitals, private clinics, and other cancer care centers across Europe, USA, and Japan. Quarterly, physicians were asked to provide case histories for the last five to 25 patients whom they have seen. They were requested not to provide the same patient’s details twice in any 12-month period. The records included full treatment history from diagnosis to current treatment, including all major surgical procedures.
European data were collected using a paper-based medical record abstraction form which the physician completes for each patient [14]. Information for all patients from France, Germany, Italy, Spain, and the UK with stage IV CRC (mCRC), aged ≥21 years at mCRC diagnosis, and with data collected during the year 2009, were identified from the database. Data relating to demographic characteristics (age, gender, weight, height, and specialty of treating physician), use of chemotherapeutic and monoclonal antibody therapy, and major surgical procedures performed after patients were diagnosed with mCRC were extracted from the database. Major surgical procedures were categorized by the purpose of surgery (curative, palliative, or diagnostic) and also examined by location of surgery (primary tumor, metastases, or other locations). Both prevalence of major surgery and number of surgical procedures were evaluated.
Statistical Analysis
Surgery patterns were analyzed descriptively overall and also by subcategories: major surgery performed for curative, palliative, or diagnostic purposes and major surgery for the primary tumor, metastasis, or at other locations. Mean, standard deviation (SD), and median values were calculated for continuous variables, while numbers and percentages were calculated for categorical variables.
Results
Patient Demographics
The study sample included 3,249 patients with mCRC (61% male, median age category 61–70 years), of whom 515, 862, 656, 649, and 567 were from France, Germany, Italy, Spain, and the UK, respectively (Table 1). Across all countries, most patients were treated by medical oncologists (range 58.7% [UK] to 86.8% [Spain]), although many other specialties were involved in mCRC treatment. In particular, radiologists in the UK were responsible for the treatment of 35.5% of patients, in contrast to all other European countries (range 2–3%). Gastroenterologists treated 22.9% of patients in France and 11.0% of patients in Germany, while general surgeons treated 6.5–11.9% of patients, depending on the country.
Surgical Procedures in Patients with mCRC
Overall Extent of Surgical Procedures
The percentage of patients that underwent at least one major surgical procedure for any purpose as part of treatment for or while being treated for mCRC was 30.5% (UK), 35.2% (Germany), 35.6% (Spain), 36.3% (France), and 38.4% (Italy). Following mCRC diagnosis, patients were subject to a mean of 1.3 major surgical procedures in the UK (SD 0.7) and Spain (SD 0.6), 1.5 in Italy (SD 0.7) and Germany (SD 0.8), and 1.6 in France (SD 0.8).
Surgical Procedures by Purpose
The distribution of patients by major surgical procedure categories in each country is shown in Fig. 1. Between 5.7% (Spain) and 14.1% (UK) of patients (7.3% [Italy], 8.4% [Germany], and 11.5% [France]) received major surgery for diagnostic purposes. The mean number of major surgeries per person for diagnostic purposes was approximately 1.1 across all five European countries (SD range 0.2–0.4). Major surgery for palliative purposes was performed in 10.8% of patients in the UK, 15.7% in France, 19.4% in Italy, and 20.5% in Germany and Spain. Finally, the rate of major surgery for curative purposes was the highest in Italy (13.4%), followed by France (12.8%), Spain (10.3%), and Germany (9.2%); the lowest was in the UK (7.2%). The mean total number of major surgical procedures per patient for curative purposes ranged from 1.3 (Germany and Spain) to 1.6 (France).
Surgical Procedures by Location
The distribution of major surgical procedures categorized by the location of surgery (primary tumors, metastases, and other locations/reasons) in each of the five countries is shown in Fig. 2. Approximately 20% of patients from each country, except the UK (12.4%), had at least one major surgical procedure for primary tumor excision after mCRC diagnosis with a mean of approximately one primary tumor surgery per patient (mean range 1.0–1.1). Italy had the highest number of patients who underwent major surgery for metastasis (14.6%), followed by Spain (9.2%), France (8.9%), and Germany (8.5%); it was lowest in the UK (6.4%). The major surgery for metastasis by the organ site of metastasis was mainly on the liver though some variations existed across countries. Among patients who had major surgery for metastasis, the percentage of patients who had surgery on the liver was 86.1% in the UK, 80.8% in Germany, 76.1% in Italy, 68.3% in Spain, and 58.7% in France. Major surgery at other locations was reported in 4.3% (Spain) to 8.8% (Germany) of patients with a mean of approximately one surgery per patient (mean range 1.0–1.2).
Discussion
This study assessed the extent to which patients with mCRC underwent major surgical procedures following diagnosis of mCRC in clinical practice in five European countries. Our analyses indicate that major surgery occurs frequently, with 30–38% of patients undergoing at least one major surgical procedure following diagnosis of mCRC. Although there were substantial differences among countries, major surgery for curative, palliative, and diagnostic purposes were common across all five European countries. Major surgery performed on the primary tumor and at sites of metastasis made up the majority of all surgical procedures, implying that surgery played a considerable role in the treatment of mCRC.
The country-specific differences in major surgery rates may be explained, at least in part, by the availability of advanced treatment options and difference in clinicians’ attitudes and approaches to surgery for mCRC. Additionally, national guidelines for the treatment of mCRC, developed and based on treatment options available in the country, exist in France, Germany, Italy, and the UK [15–18], which may provide differing recommendations regarding the use of surgery, leading to subsequent differences in the number and types of surgical procedures reported. Surgery rates may be influenced by the availability of appropriately trained surgeons. Additionally, country-specific differences may be attributable to differences in access to newer treatment options. For example, the UK National Institute for Health and Clinical Excellence (NICE) does not recommend the use of bevacizumab in mCRC and cetuximab has only recently been recommended for restricted use in the UK [19–21]. Since there is some evidence that adding an mAb to cytotoxic chemotherapy may increase resection rates compared with the use of cytotoxic chemotherapy alone [22], this may partially explain the relatively lower rates of surgical procedures for metastases and curative purposes in the UK.
The ESMO guidelines for treatment of advanced CRC recommend that resection of metastases should be performed as soon as the metastases become resectable, since unnecessary prolonged administration of chemotherapy may lead to higher postoperative morbidity [10]. The potential requirement for surgery should therefore be an important consideration when selecting treatment for mCRC. With advances in systemic therapy and surgical techniques, it is likely that the number of surgical procedures will increase further during treatment of mCRC.
There are some limitations to our analyses. As survey data were used in this study, sample selection bias could occur. However, the survey contains a random sample of oncology patients, which should reduce the chance for selection bias. The study also used data from five European countries and the findings may not be generalizable to other countries. Finally, the observation period after mCRC diagnosis might be truncated before death, especially for newly diagnosed patients; thus, the prevalence of major surgeries from this study could be underestimated.
In summary, this study showed that major surgery is highly prevalent following mCRC diagnosis, suggesting that surgery plays an important role in meeting the goals of mCRC treatment. The role of pharmacological treatment options and their potential to interfere with both surgery use and surgical outcomes should be considered when evaluating mCRC treatment strategies.
References
Hurwitz H, Fehrenbacher L, Novotny W, et al. Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N Engl J Med. 2004;350:2335–42.
Saltz LB, Clarke S, Diaz-Rubio E, et al. Bevacizumab in combination with oxaliplatin-based chemotherapy as first-line therapy in metastatic colorectal cancer: a randomized phase III study. J Clin Oncol. 2008;26:2013–9.
Van Cutsem E, Kohne CH, Hitre E, et al. Cetuximab and chemotherapy as initial treatment for metastatic colorectal cancer. N Engl J Med. 2009;360:1408–17.
Douillard JY, Siena S, Cassidy J, et al. Randomized, phase III trial of panitumumab with infusional fluorouracil, leucovorin, and oxaliplatin (FOLFOX4) versus FOLFOX4 alone as first-line treatment in patients with previously untreated metastatic colorectal cancer: the PRIME study. J Clin Oncol. 2010;28:4697–705.
Peeters M, Price TJ, Cervantes A, et al. Randomized phase III study of panitumumab with fluorouracil, leucovorin, and irinotecan (FOLFIRI) compared with FOLFIRI alone as second-line treatment in patients with metastatic colorectal cancer. J Clin Oncol. 2010;28:4706–13.
Zhao Z, Pelletier E, Barber B et al. Current chemotherapy and monoclonal antibody use patterns in metastatic colorectal cancer in western Europe. The 35th ESMO Congress, 8–12 October 2010, Milan, Italy. Poster number 611
Adenis A, Vanseymortier L, Foissey D, et al. Bevacizumab and postponed suture leakages after surgery for ulcerative colitis and rectal cancer. Gut. 2007;56:734.
Gordon CR, Rojavin Y, Patel M, et al. A review on bevacizumab and surgical wound healing: an important warning to all surgeons. Ann Plast Surg. 2009;62:707–9.
Kabbinavar F, Hurwitz HI, Fehrenbacher L, et al. Phase II, randomized trial comparing bevacizumab plus fluorouracil (FU)/leucovorin (LV) with FU/LV alone in patients with metastatic colorectal cancer. J Clin Oncol. 2003;21:60–5.
Van Cutsem E, Nordlinger B, Cervantes A. Advanced colorectal cancer: ESMO clinical practice guidelines for treatment. Ann Oncol. 2010;21 Suppl 5:v93–7.
Simmonds PC, Primrose JN, Colquitt JL, et al. Surgical resection of hepatic metastases from colorectal cancer: a systematic review of published studies. Br J Cancer. 2006;94:982–99.
National Comprehensive Cancer Network Guidelines (2010) Colon cancer guidelines version 2.2011. Available at http://www.nccn.org/professionals/physician_gls/PDF/colon.pdf. Accessed Oct 2010.
Nordlinger B, Van Cutsem E, Gruenberger T, et al. European colorectal metastases treatment group; Sixth International Colorectal Liver Metastases Workshop. Combination of surgery and chemotherapy and the role of targeted agents in the treatment of patients with colorectal liver metastases: recommendations from an expert panel. Ann Oncol. 2009;20:985–92.
Inoue Y, Toiyama Y, Tanaka K, et al. A comprehensive comparative study on the characteristics of colorectal cancer chemotherapy. Jpn J Clin Oncol. 2009;39:367–75.
Beretta G, Carnaghi C, Cosimelli M et al. Linee guida, tumori del colon-retto, 2009. Available at http://www.aiom.it/. Accessed Oct 2010
Schmiegel W, Pox C, Reinacher-Schick A, et al. S3 guidelines for colorectal carcinoma: results of an evidence-based consensus conference on February 6/7, 2004 and June 8/9, 2007 (for the topics IV, VI and VII). Z Gastroenterol. 2010;48:65–136.
Haute Autorité de Santé/Institut National du Cancer (2008) Tumeur maligne, affection maligne du tissue lymphatique ou hématopoïétique: cancer colorectal. Available at http://www.e-cancer.fr/soins/recommandations/cancers-digestifs. Accessed Oct 2010
Association of Coloproctology of Great Britain and Ireland (2007) Guidelines for the management of colorectal cancer, 3 rd edition. Available at http://www.acpgbi.org.uk/assets/documents/COLO_guides.pdf. Accessed Oct 2010.
NICE (2007) TA118 Colorectal cancer (metastatic)—bevacizumab & cetuximab: full guidance. Available at http://guidance.nice.org.uk/TA118/Guidance/pdf/English. Accessed Oct 2010.
NICE (2010) Final appraisal determination (FAD)—bevacizumab in combination with oxaliplatin and either fluorouracil plus folinic acid or capecitabine for the treatment of metastatic colorectal cancer. Available at http://www.nice.org.uk/nicemedia/live/12098/51510/51510.pdf. Accessed Oct 2010.
NICE (2009) TA176 colorectal cancer (first line)—cetuximab: full guidance. Available at http://guidance.nice.org.uk/TA176/Guidance/pdf/English. Accessed Oct 2010.
Nasti G, Ottaiano A, Berretta M, et al. Pre-operative chemotherapy for colorectal cancer liver metastases: an update of recent clinical trials. Cancer Chemother Pharmacol. 2010;66:209–18.
Acknowledgments
The study was funded by Amgen Inc. Medical writing assistance was provided by ApotheCom ScopeMedical Ltd, funded by Amgen, Inc.
Conflicts of Interest
Zhongyun Zhao, Beth Barber, Song Wang, and Sue Gao are employees and stockholders of Amgen Inc. Elise Pelletier, Monali Bhosle, and David Klingman are employees of the IMS Consulting Group and received funding from Amgen Inc to perform the analyses reported in this manuscript.
Open Access
This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License (https://creativecommons.org/licenses/by-nc/2.0), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Zhao, Z., Pelletier, E., Barber, B. et al. Major Surgery in Patients with Metastatic Colorectal Cancer in Western Europe. J Gastrointest Canc 43, 456–461 (2012). https://doi.org/10.1007/s12029-011-9349-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12029-011-9349-y