Abstract
Background
Spontaneous intracerebral hemorrhage (sICH) is a major health concern and has high mortality rates up to 52%. Despite a decrease in its incidence, fatality rates remain unchanged; understanding and preventing of factors associated with mortality and treatments for these are needed. Blood pressure variability (BPV) has been shown to be a potential modifiable factor associated with clinical outcomes in patients with traumatic intracerebral hemorrhage and sICH. Few data are available on the effect of intracranial pressure (ICP) variability (ICPV) and outcomes in patients with sICH. The goal of our study was to investigate the association between ICPV and BPV during the first 24 h of intensive care unit (ICU) admission and external ventricular drain (EVD) placement, and mortality in patients with sICH who were monitored with an EVD.
Methods
We conducted a single-center retrospective study of adult patients admitted to an ICU with a diagnosis of sICH who required EVD placement during hospitalization. We excluded patients with ICH secondary to other pathological conditions such as trauma, underlying malignancy, or arteriovenous malformation. Blood pressure and ICP measurements were collected and recorded hourly during the first 24 h of ICU admission and EVD placement, respectively. Measures of variability used were standard deviation (SD) and successive variation (SV). Primary outcome of interest was in-hospital mortality, and secondary outcomes were hematoma expansion and discharge home (a surrogate for good functional outcome at discharge). Descriptive statistics and multivariable logistic regressions were performed.
Results
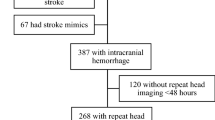
We identified 179 patients with sICH who required EVD placement. Of these, 52 (29%) patients died, 121 (68%) patients had hematoma expansion, and 12 (7%) patients were discharged home. Patient’s mean age (± SD) was 56 (± 14), and 87 (49%) were women. The mean opening ICP (± SD) was 21 (± 8) and median ICH score (interquartile range) was 2 (2–3). Multivariable logistic regression found an association between ICP-SV and ICP-SD and hematoma expansion (odds ratio 1.6 [1.03–2.30], p = 0.035 and odds ratio 0.77 [0.63–0.93] p = 0.009, respectively).
Conclusions
Our study found an association between ICPV and hematoma expansion in patients with sICH monitored with an EVD. Measures of ICPV relating to rapid changes in ICP (ICP-SV) were associated with a higher odds of hematoma expansion, whereas measures relating to tight control of ICP (ICP-SD) were associated with a lower odds of hematoma expansion. One measure of BPV, sytolic blood pressure maximum-minimum (SBP max-min), was found to be weakly associated with discharge home (a surrogate for good functional outcome at hospital discharge). More research is needed to support these findings.

Similar content being viewed by others
References
Qureshi AI, Mendelow AD, Hanley DF. Intracerebral haemorrhage. Lancet Lond Engl. 2009;373(9675):1632–44. https://doi.org/10.1016/S0140-6736(09)60371-8.
Testai FD, Aiyagari V. Acute hemorrhagic stroke pathophysiology and medical interventions: blood pressure control, management of anticoagulant-associated brain hemorrhage and general management principles. Neurol Clin. 2008;26(4):963–85. https://doi.org/10.1016/j.ncl.2008.06.001.
Zahuranec DB, Lisabeth LD, Sanchez BN, et al. Intracerebral hemorrhage mortality is not changing despite declining incidence. Neurology. 2014;82(24):2180–6. https://doi.org/10.1212/WNL.0000000000000519.
Broderick JP, Brott TG, Duldner JE, Tomsick T, Huster G. Volume of intracerebral haemorrhage. A powerful and easy-to-use predictor of 30-day mortality. Stroke. 1993;24(7):987–93. https://doi.org/10.1161/01.STR.24.7.987.
Davis SM, Broderick J, Hennerici M, et al. Hematoma growth is a determinant of mortality and poor outcome after intracerebral hemorrhage. Neurology. 2006;66(8):1175–81. https://doi.org/10.1212/01.wnl.0000208408.98482.99.
Morotti A, Boulouis G, Charidimou A, et al. Hematoma expansion in intracerebral hemorrhage with unclear onset. Neurology. 2021;96(19):e2363–71. https://doi.org/10.1212/WNL.0000000000011895.
Greenberg SM, Ziai WC, Cordonnier C, et al. 2022 guideline for the management of patients with spontaneous intracerebral hemorrhage: a guideline from the American Heart Association/American Stroke Association. Stroke. 2022. https://doi.org/10.1161/STR.0000000000000407.
Chung PW, Kim JT, Sanossian N, et al. Association between hyperacute stage blood pressure variability and outcome in patients with spontaneous intracerebral hemorrhage. Stroke. 2018;49(2):348–54. https://doi.org/10.1161/STROKEAHA.117.017701.
Manning L, Hirakawa Y, Arima H, et al. Blood pressure variability and outcome after acute intracerebral haemorrhage: a post-hoc analysis of INTERACT2, a randomised controlled trial. Lancet Neurol. 2014;13(4):364–73. https://doi.org/10.1016/S1474-4422(14)70018-3.
Tanaka E, Koga M, Kobayashi J, et al. Blood pressure variability on antihypertensive therapy in acute intracerebral hemorrhage: the stroke acute management with urgent risk-factor assessment and improvement-intracerebral hemorrhage study. Stroke. 2014;45(8):2275–9. https://doi.org/10.1161/STROKEAHA.114.005420.
Gurshawn T, Jackson M, Barr J, et al. Transportation management affecting outcomes of patients with spontaneous intracranial hemorrhage. Air Med J. 2020;39(3):189–95. https://doi.org/10.1016/j.amj.2019.12.001.
Treggiari MM, Schutz N, Yanez ND, Romand JA. Role of intracranial pressure values and patterns in predicting outcome in traumatic brain injury: a systematic review. Neurocrit Care. 2007;6(2):104–12. https://doi.org/10.1007/s12028-007-0012-1.
Kalita J, Misra UK, Vajpeyee A, Phadke RV, Handique A, Salwani V. Brain herniations in patients with intracerebral hemorrhage. Acta Neurol Scand. 2009;119(4):254–60. https://doi.org/10.1111/j.1600-0404.2008.01095.x.
Svedung Wettervik T, Howells T, Enblad P, Lewén A. Intracranial pressure variability: relation to clinical outcome, intracranial pressure–volume index, cerebrovascular reactivity and blood pressure variability. J Clin Monit Comput. 2020;34(4):733–41. https://doi.org/10.1007/s10877-019-00387-9.
Svedung Wettervik T, Howells T, Hånell A, Ronne-Engström E, Lewén A, Enblad P. Low intracranial pressure variability is associated with delayed cerebral ischemia and unfavorable outcome in aneurysmal subarachnoid hemorrhage. J Clin Monit Comput. 2022;36(2):569–78. https://doi.org/10.1007/s10877-021-00688-y.
Kirkness CJ, Burr RL, Mitchell PH. Intracranial and blood pressure variability and long-term outcome after aneurysmal sub-arachnoid hemorrhage. Am J Crit Care. 2009;18(3):241–51. https://doi.org/10.4037/ajcc2009743.
Tian Y, Wang Z, Jia Y, et al. Intracranial pressure variability predicts short-term outcome after intracerebral hemorrhage: a retrospective study. J Neurol Sci. 2013;330(1–2):38–44. https://doi.org/10.1016/j.jns.2013.04.001.
Tran C, Frederick H, Baqai H, et al. Traumatic brain injury and intraparenchymal hemorrhage progression: blood pressure variability matters. Am J Emerg Med. 2022;52:119–27. https://doi.org/10.1016/j.ajem.2021.12.005.
Tiffany L, Haase DJ, Boswell K, et al. Care intensity of spontaneous intracranial hemorrhage: effectiveness of the critical care resuscitation unit. Am J Emerg Med. 2021;46:437–44. https://doi.org/10.1016/j.ajem.2020.10.044.
Ajam K, Gold LS, Beck SS, Damon S, Phelps R, Rea TD. Reliability of the cerebral performance category to classify neurological status among survivors of ventricular fibrillation arrest: a cohort study. Scand J Trauma Resusc Emerg Med. 2011;19(1):38. https://doi.org/10.1186/1757-7241-19-38.
Grossestreuer AV, Abella BS, Sheak KR, et al. Inter-rater reliability of post-arrest cerebral performance category (CPC) scores. Resuscitation. 2016;109:21–4. https://doi.org/10.1016/j.resuscitation.2016.09.006.
Quinn TJ, Dawson J, Walters MR, Lees KR. Exploring the reliability of the modified Rankin Scale. Stroke. 2009;40(3):762–6. https://doi.org/10.1161/STROKEAHA.108.522516.
Tuteja G, Uppal A, Strong J, et al. Interventions affecting blood pressure variability and outcomes after intubating patients with spontaneous intracranial hemorrhage. Am J Emerg Med. 2019;37(9):1665–71. https://doi.org/10.1016/j.ajem.2018.11.041.
Dodd WS, Laurent D, Dumont AS, et al. Pathophysiology of delayed cerebral ischemia after subarachnoid hemorrhage: a review. J Am Heart Assoc. 2021;10(15):e021845. https://doi.org/10.1161/JAHA.121.021845.
Connolly ES, Rabinstein AA, Carhuapoma JR, et al. Guidelines for the management of aneurysmal subarachnoid hemorrhage: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2012;43(6):1711–37. https://doi.org/10.1161/STR.0b013e3182587839.
Tran Q, Najafali D, et al. Effect of blood pressure variability on outcomes in emergency patients with intracranial hemorrhage. West J Emerg Med. 2021. https://doi.org/10.5811/westjem.2020.9.48072.
Manning LS, Mistri AK, Potter J, Rothwell PM, Robinson TG. Short-term blood pressure variability in acute stroke: post hoc analysis of the controlling hypertension and hypotension immediately post stroke and continue or stop post-stroke antihypertensives collaborative study trials. Stroke. 2015;46(6):1518–24. https://doi.org/10.1161/STROKEAHA.115.009078.
Bzhilyanskaya V, Najafali D, Torre OM, et al. Emergency department and transport predictors of neurological deterioration in patients with spontaneous intracranial hemorrhage. Am J Emerg Med. 2022;53:154–60. https://doi.org/10.1016/j.ajem.2022.01.002.
Li Q, Warren AD, Qureshi AI, et al. Ultra-early blood pressure reduction attenuates hematoma growth and improves outcome in intracerebral hemorrhage. Ann Neurol. 2020;88(2):388–95. https://doi.org/10.1002/ana.25793.
Wang X, Arima H, Heeley E, et al. Magnitude of blood pressure reduction and clinical outcomes in acute intracerebral hemorrhage: intensive blood pressure reduction in acute cerebral hemorrhage trial study. Hypertension. 2015;65(5):1026–32. https://doi.org/10.1161/HYPERTENSIONAHA.114.05044.
Saulle M, Schambra H. Recovery and rehabilitation after intracerebral hemorrhage. Semin Neurol. 2016;36(03):306–12. https://doi.org/10.1055/s-0036-1581995.
Kitago T, Ratan RR. Rehabilitation following hemorrhagic stroke: building the case for stroke-subtype specific recovery therapies. F1000Research. 2017;6:2044. https://doi.org/10.12688/f1000research.11913.1.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
SC: Conceptualization, data curation, formal analysis, investigation, project administration, visualization, writing—original draft, writing–review and editing. HB: Conceptualization, data curation, formal analysis, investigation, visualization, writing—original draft, writing—review and editing. FM: Conceptualization, data curation, formal analysis, investigation, visualization, writing—original draft, writing—review and editing. AA: Conceptualization, data curation, formal analysis, investigation, visualization, writing—original draft, writing—review and editing. JS: Conceptualization, data curation, formal analysis, investigation, visualization, writing—original draft, writing—review and editing. HF: Conceptualization, data curation, formal analysis, investigation, visualization, writing—original draft, writing—review and editing. NS: Conceptualization, data curation, formal analysis, investigation, visualization, writing—original draft, writing—review and editing. JO: Conceptualization, data curation, formal analysis, investigation, visualization, writing—original draft, writing—review and editing. JAS: Conceptualization, data curation, formal analysis, investigation, visualization, writing—original draft, writing—review and editing. AS: Conceptualization, data curation, formal analysis, investigation, visualization, writing—original draft, writing—review and editing. MBP: Conceptualization, data curation, formal analysis, investigation, visualization, writing—original draft, writing—review and editing. QKT: Conceptualization, data curation, formal analysis, investigation, visualization, writing—original draft, writing—review and editing. The authors approve of the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no conflicts of interest to disclose.
Ethical approval/informed consent
This study was exempted by the institutional review board number HP-00094744.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix 1
Appendix 1
See Table 4.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cardona, S., Baqai, H., Mikdashi, F. et al. Intracranial and Blood Pressure Variability and In-Hospital Outcomes in Intracranial Device-Monitored Patients with Spontaneous Intracerebral Hemorrhage. Neurocrit Care 39, 357–367 (2023). https://doi.org/10.1007/s12028-023-01677-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-023-01677-6