Abstract
Background
Dysfunctional cerebral autoregulation often precedes delayed cerebral ischemia (DCI). Currently, there are no data-driven techniques that leverage this information to predict DCI in real time. Our hypothesis is that information using continuous updated analyses of multimodal neuromonitoring and cerebral autoregulation can be deployed to predict DCI.
Methods
Time series values of intracranial pressure, brain tissue oxygenation, cerebral perfusion pressure (CPP), optimal CPP (CPPOpt), ΔCPP (CPP − CPPOpt), mean arterial pressure, and pressure reactivity index were combined and summarized as vectors. A validated temporal signal angle measurement was modified into a classification algorithm that incorporates hourly data. The time-varying temporal signal angle measurement (TTSAM) algorithm classifies DCI at varying time points by vectorizing and computing the angle between the test and reference time signals. The patient is classified as DCI+ if the error between the time-varying test vector and DCI+ reference vector is smaller than that between the time-varying test vector and DCI− reference vector. Finally, prediction at time point t is calculated as the majority voting over all the available signals. The leave-one-patient-out cross-validation technique was used to train and report the performance of the algorithms. The TTSAM and classifier performance was determined by balanced accuracy, F1 score, true positive, true negative, false positive, and false negative over time.
Results
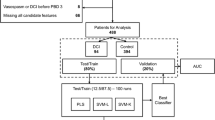
One hundred thirty-one patients with aneurysmal subarachnoid hemorrhage who underwent multimodal neuromonitoring were identified from two centers (Columbia University: 52 [39.7%], Aachen University: 79 [60.3%]) and included in the analysis. Sixty-four (48.5%) patients had DCI, and DCI was diagnosed 7.2 ± 3.3 days after hemorrhage. The TTSAM algorithm achieved a balanced accuracy of 67.3% and an F1 score of 0.68 at 165 h (6.9 days) from bleed day with a true positive of 0.83, false positive of 0.16, true negative of 0.51, and false negative of 0.49.
Conclusions
A TTSAM algorithm using multimodal neuromonitoring and cerebral autoregulation calculations shows promise to classify DCI in real time.


Similar content being viewed by others
References
Dorsch NW. Therapeutic approaches to vasospasm in subarachnoid hemorrhage. Curr Opin Crit Care. 2002;8(2):128–33.
Suarez JI. Diagnosis and management of subarachnoid hemorrhage. Continuum (Minneap Minn). 2015;21:1263–87. https://doi.org/10.1212/CON.0000000000000217.
Rowland MJ, Hadjipavlou G, Kelly M, Westbrook J, Pattinson KT. Delayed cerebral ischaemia after subarachnoid haemorrhage: looking beyond vasospasm. Br J Anaesth. 2012;109(3):315–29. https://doi.org/10.1093/bja/aes264.
Francoeur CL, Mayer SA. Management of delayed cerebral ischemia after subarachnoid hemorrhage. Crit Care. 2016;20(1):277. https://doi.org/10.1186/s13054-016-1447-6.
Lai X, Zhang W, Ye M, Liu X, Luo X. Development and validation of a predictive model for the prognosis in aneurysmal subarachnoid hemorrhage. J Clin Lab Anal. e23542.
Claassen J, Hirsch LJ, Kreiter KT, et al. Quantitative continuous EEG for detecting delayed cerebral ischemia in patients with poor-grade subarachnoid hemorrhage. Clin Neurophysiol. 2004;115(12):2699–710. https://doi.org/10.1016/j.clinph.2004.06.017.
Roederer A, Holmes JH, Smith MJ, Lee I, Park S. Prediction of significant vasospasm in aneurysmal subarachnoid hemorrhage using automated data. Neurocrit Care. 2014;21(3):444–50. https://doi.org/10.1007/s12028-014-9976-9.
Park S, Megjhani M, Frey HP, et al. Predicting delayed cerebral ischemia after subarachnoid hemorrhage using physiological time series data. J Clin Monit Comput. 2018. https://doi.org/10.1007/s10877-018-0132-5.
Megjhani M, Terilli K, Frey HP, et al. Incorporating high-frequency physiologic data using computational dictionary learning improves prediction of delayed cerebral ischemia compared to existing methods. Front Neurol. 2018;9:122. https://doi.org/10.3389/fneur.2018.00122.
Schmidt JM, Sow D, Crimmins M, et al. Heart rate variability for preclinical detection of secondary complications after subarachnoid hemorrhage. Neurocrit Care. 2014;20(3):382–9. https://doi.org/10.1007/s12028-014-9966-y.
Ramos LA, van der Steen WE, Sales Barros R, et al. Machine learning improves prediction of delayed cerebral ischemia in patients with subarachnoid hemorrhage. J Neurointerv Surg. 2018. https://doi.org/10.1136/neurintsurg-2018-014258.
Megjhani M, Terilli K, Weiss M, et al. Dynamic detection of delayed cerebral ischemia: a study in 3 centers. Stroke. 2021;52(4):1370–9.
Veldeman M, Albanna W, Weiss M, et al. Invasive multimodal neuromonitoring in aneurysmal subarachnoid hemorrhage: a systematic review. Stroke. 2021;52(11):3624–32.
Budohoski KP, Czosnyka M, Smielewski P, et al. Impairment of cerebral autoregulation predicts delayed cerebral ischemia after subarachnoid hemorrhage: a prospective observational study. Stroke. 2012;43(12):3230–7. https://doi.org/10.1161/strokeaha.112.669788.
Weiss Miriam, Walid A, Catharina C, et al. Optimal cerebral perfusion pressure during delayed cerebral ischemia after aneurysmal subarachnoid hemorrhage. Crit Care Med (in press). 2022
Lipton ZC, Kale DC, Elkan C, Wetzell R. Learning to Diagnose with LSTM Recurrent Neural Networks. ArXiv e-prints. 2015;1511. Accessed November 1, 2015. http://adsabs.harvard.edu/abs/2015arXiv151103677L
Xiao C, Choi E, Sun J. Opportunities and challenges in developing deep learning models using electronic health records data: a systematic review. J Am Med Inform Assoc. 2018;25(10):1419–28.
Wang F, Casalino LP, Khullar D. Deep learning in medicine: promise, progress, and challenges. JAMA Intern Med. 2019;179(3):293–4.
Kwon SB, Park J-H, Kwon C, Kong HJ, Hwang JY, Kim HC. An energy-efficient algorithm for classification of fall types using a wearable sensor. IEEE Access. 2019;7:31321–9.
Connolly ES Jr, Rabinstein AA, Carhuapoma JR, et al. Guidelines for the management of aneurysmal subarachnoid hemorrhage: a guideline for healthcare professionals from the American Heart Association/american Stroke Association. Stroke. 2012;43(6):1711–37. https://doi.org/10.1161/STR.0b013e3182587839.
Steiner T, Juvela S, Unterberg A, et al. European Stroke Organization guidelines for the management of intracranial aneurysms and subarachnoid haemorrhage. Cerebrovasc Dis. 2013;35(2):93–112. https://doi.org/10.1159/000346087.
Stuart RM, Schmidt M, Kurtz P, et al. Intracranial multimodal monitoring for acute brain injury: A single institution review of current practices. Neurocrit Care. 2010;12(2):188–98. https://doi.org/10.1007/s12028-010-9330-9.
Komotar RJ, Schmidt JM, Starke RM, et al. Resuscitation and critical care of poor-grade subarachnoid hemorrhage. Neurosurgery. 2009;64(3):397–410. https://doi.org/10.1227/01.NEU.0000338946.42939.C7.
Le-Roux P, Menon DK, Citerio G, et al. The International multidisciplinary consensus conference on multimodality monitoring in neurocritical Care: a list of recommendations and additional conclusions: a statement for healthcare professionals from the Neurocritical Care Society and the European Society of Intensive Care Medicine. Neurocrit Care. 2014;21(Suppl2):282–96. https://doi.org/10.1007/s12028-014-0077-6.
Le Roux P, Menon DK, Citerio G, et al. Consensus summary statement of the international multidisciplinary consensus conference on multimodality monitoring in neurocritical care: a statement for healthcare professionals from the neurocritical care society and the european society of intensive care medicine. Intensive Care Med. 2014;40(9):1189–209. https://doi.org/10.1007/s00134-014-3369-6.
Vergouwen MD, Vermeulen M, van Gijn J, et al. Definition of delayed cerebral ischemia after aneurysmal subarachnoid hemorrhage as an outcome event in clinical trials and observational studies: proposal of a multidisciplinary research group. Stroke. 2010;41(10):2391–5. https://doi.org/10.1161/strokeaha.110.589275.
Megjhani M, Terilli K, Martin A, et al. Deriving PRx and CPPopt from 0.2 Hz data: establishing generalizability to bedmaster users. Acta Neurochir Suppl. 2017; Proceedings of Intracranial Pressure & Neuromonitoring XVI.
Zweifel C, Lavinio A, Steiner LA, et al. Continuous monitoring of cerebrovascular pressure reactivity in patients with head injury. Neurosurg Focus. 2008;25(4):E2. https://doi.org/10.3171/FOC.2008.25.10.E2.
Czosnyka M, Smielewski P, Kirkpatrick P, Laing RJ, Menon D, Pickard JD. Continuous assessment of the cerebral vasomotor reactivity in head injury. Neurosurgery. 1997;41(1):11–9. https://doi.org/10.1097/00006123-199707000-00005.
Johnson AE, Ghassemi MM, Nemati S, Niehaus KE, Clifton DA, Clifford GD. Machine learning and decision support in critical care. Proc IEEE Inst Electr Electron Eng. 2016;104(2):444–66. https://doi.org/10.1109/jproc.2015.2501978.
Funding
This study was funded by the National Institutes of Health [Grants R21NS113055 (SP), K01-ES026833 (SP)] and the American Heart Association [Grant 20POST35210653 (MM)].
Author information
Authors and Affiliations
Contributions
Data collection: MW, JF, DN, NK, HF, AV, DR, SA, ESC, JC, GS, analysis: MM, MW, SK GS, SP, writing: MM, SP, MW, editing: all.
Corresponding author
Ethics declarations
Conflict of interest
Please confirm the authors declare no conflicts of interest.
Ethical Approval
The study was approved by the institutional review boards at the respective centers.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Megjhani, M., Weiss, M., Kwon, S.B. et al. Vector Angle Analysis of Multimodal Neuromonitoring Data for Continuous Prediction of Delayed Cerebral Ischemia. Neurocrit Care 37 (Suppl 2), 230–236 (2022). https://doi.org/10.1007/s12028-022-01481-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-022-01481-8