Abstract
Background/Objective
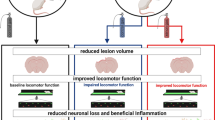
In recent years, the noble gas argon (Ar) has been extensively studied for its organ protection properties. While mounting in vitro and in vivo evidence indicates that argon provides neuroprotection in ischemic brain injury, its neuroprotective potential in traumatic brain injury (TBI) has not been evaluated in vivo. We tested the hypothesis that prolonged inhalation of 70% or 79% argon for 24 h after closed-head injury (CHI) improves neurologic outcome and overall recovery at 36 days post-injury. We also compared effects of the 30% or 21% residual oxygen on argon’s potential neuroprotective capacity.
Methods
Adult male C57/black mice (n = 240) were subjected to closed-head traumatic brain injury, followed by inhalation of 70% argon or nitrogen (30% oxygen), or 79% argon or nitrogen (21% oxygen) for 24 h. Neurologic outcome (rotarod, neuroscore, and Morris water maze) was evaluated for up to 36 days post-injury. Histologic parameters of neurologic degeneration (Fluoro-Jade staining) and inflammation (F4/80 microglia immunostaining) were assessed in subgroups at 24 h and on post-injury day 7.
Results
Our CHI protocol consistently resulted in significant brain injury. After argon inhalation for 24 h at either concentration, mice did not show significant improvement with regard to neuroscores, rotarod performance, Morris water maze performance, or overall recovery (body weight), compared to nitrogen controls, up to 36 days. At 7 days post-injury, histologic markers of neurodegeneration and inflammation, particularly in the hippocampus, consistently demonstrated significant injury. Notably, recovery was reduced in mice treated with the higher oxygen concentration (30%) after CHI compared to 21%.
Conclusions
Prolonged argon treatment did not improve neurologic outcome, overall recovery (weight), nor markers of neurodegeneration or neuroinflammation after significant CHI compared to nitrogen. While neuroprotective in predominately ischemic injury, argon did not provide protection after TBI in this model, highlighting the crucial importance of assessing argon’s strengths and weaknesses in preclinical models to fully understand its organ protective potential in different pathologies and gas mixtures.






Similar content being viewed by others
References
Faul M, Coronado V. Epidemiology of traumatic brain injury. Handb Clin Neurol. 2015;127:3–13.
Corps KN, Roth TL, McGavern DB. Inflammation and neuroprotection in traumatic brain injury. JAMA Neurol. 2015;72(3):355–62.
Dixon KJ. Pathophysiology of traumatic brain injury. Phys Med Rehabil Clin N Am. 2017;28(2):215–25.
McGinn MJ, Povlishock JT. Pathophysiology of traumatic brain injury. Neurosurg Clin N Am. 2016;27(4):397–407.
Nespoli F, Redaelli S, Ruggeri L, et al. A complete review of preclinical and clinical uses of the noble gas argon: Evidence of safety and protection. Ann Card Anaesth. 2019;22(2):122–35.
Grune F, Kazmaier S, Hoeks SE, et al. Argon does not affect cerebral circulation or metabolism in male humans. PLoS ONE. 2017;12(2):e0171962.
Lemoine S, Blanchart K, Souplis M, et al. Argon exposure induces postconditioning in myocardial ischemia-reperfusion. J Cardiovasc Pharmacol Ther. 2017;22(6):564–73.
Zhao H, Mitchell S, Koumpa S, et al. Heme oxygenase-1 mediates neuroprotection conferred by argon in combination with hypothermia in neonatal hypoxia-ischemia brain injury. Anesthesiology. 2016;125:180–92.
Zhao H, Mitchell S, Ciechanowicz S, et al. Argon protects against hypoxic-ischemic brain injury in neonatal rats through activation of nuclear factor (erythroid-derived 2)-like 2. Oncotarget. 2016;7:25640.
Hollig A, Weinandy A, Liu J, et al. beneficial properties of argon after experimental subarachnoid hemorrhage: early treatment reduces mortality and influences hippocampal protein expression. Crit Care Med. 2016;44(7):e520–e529529.
Brucken A, Kurnaz P, Bleilevens C, et al. Delayed argon administration provides robust protection against cardiac arrest-induced neurological damage. Neurocrit Care. 2015;22(1):112–20.
Ulbrich F, Schallner N, Coburn M, et al. Argon inhalation attenuates retinal apoptosis after ischemia/reperfusion injury in a time- and dose-dependent manner in rats. PLoS ONE. 2014;9(12):e115984.
Ma S, Chu D, Li L, et al. Argon inhalation for 24 h after onset of permanent focal cerebral ischemia in rats provides neuroprotection and improves neurologic outcome. Crit Care Med. 2019;47(8):e693–e699699.
Donati G, Kapetanios A, Dubois-Dauphin M, Pournaras CJ. Caspase-related apoptosis in chronic ischaemic microangiopathy following experimental vein occlusion in mini-pigs. Acta Ophthalmol. 2008;86(3):302–6.
Haelewyn B, David HN, Colloc'h N, et al. Interactions between nitrous oxide and tissue plasminogen activator in a rat model of thromboembolic stroke. Anesthesiology. 2011;115(5):1044–53.
Rizvi M, Jawad N, Li Y, et al. Effect of noble gases on oxygen and glucose deprived injury in human tubular kidney cells. Exp Biol Med (Maywood). 2010;235(7):886–91.
Hafner C, Qi H, Soto-Gonzalez L, et al. argon preconditioning protects airway epithelial cells against hydrogen peroxide-induced oxidative stress. Eur Surg Res. 2016;57(3–4):252–62.
Faure A, Bruzzese L, Steinberg JG, et al. Effectiveness of pure argon for renal transplant preservation in a preclinical pig model of heterotopic autotransplantation. J Transl Med. 2016;14:40.
Loetscher PD, Rossaint J, Rossaint R, et al. Argon: neuroprotection in in vitro models of cerebral ischemia and traumatic brain injury. Crit Care. 2009;13(6):R206.
Harris K, Armstrong SP, Campos-Pires R, et al. Neuroprotection against traumatic brain injury by xenon, but not argon, is mediated by inhibition at the N-methyl-D-aspartate receptor glycine site. Anesthesiology. 2013;119(5):1137–48.
Grüßer L, Blaumeiser-Debarry R, Krings M, et al. Argon attenuates the emergence of secondary injury after traumatic brain injury within a 2-hour incubation period compared to desflurane: an in vitro study. Med Gas Res. 2017;7(2):93–100.
Lamade AM, Anthonymuthu TS, Hier ZE, et al. Mitochondrial damage & lipid signaling in traumatic brain injury. Exp Neurol. 2020;329:113307.
da Silva Meirelles L, Simon D, Regner A. Neurotrauma: the crosstalk between neurotrophins and inflammation in the acutely injured brain. Int J Mol Sci. 2017;18(5):1082.
Abdul-Muneer PM, Pfister BJ, Haorah J, Chandra N. Role of matrix metalloproteinases in the pathogenesis of traumatic brain injury. Mol Neurobiol. 2016;53(9):6106–23.
Wang H, Gao J, Lassiter TF, et al. Levetiracetam is neuroprotective in murine models of closed head injury and subarachnoid hemorrhage. Neurocrit Care. 2006;5(1):71–8.
Lynch JR, Wang H, McGirt MJ, et al. Simvastatin reduces vasospasm after aneurysmal subarachnoid hemorrhage: results of a pilot randomized clinical trial. Stroke J Cereb circ. 2005;36(9):2024–6.
Wang H, Lynch JR, Song P, et al. Simvastatin and atorvastatin improve behavioral outcome, reduce hippocampal degeneration, and improve cerebral blood flow after experimental traumatic brain injury. Exp Neurol. 2007;206(1):59–69.
Wang H, Durham L, Dawson H, et al. An apolipoprotein E-based therapeutic improves outcome and reduces Alzheimer's disease pathology following closed head injury: evidence of pharmacogenomic interaction. Neuroscience. 2007;144(4):1324–33.
Tsenter J, Beni-Adani L, Assaf Y, et al. Dynamic changes in the recovery after traumatic brain injury in mice: effect of injury severity on T2-weighted MRI abnormalities, and motor and cognitive functions. J Neurotrauma. 2008;25(4):324–33.
Schmued LC, Hopkins KJ. Fluoro-Jade B: a high affinity fluorescent marker for the localization of neuronal degeneration. Brain Res. 2000;874(2):123–30.
West MJ, Slomianka L, Gundersen HJ. Unbiased stereological estimation of the total number of neurons in thesubdivisions of the rat hippocampus using the optical fractionator. Anat Rec. 1991;231(4):482–97.
Ryang YM, Fahlenkamp AV, Rossaint R, et al. Neuroprotective effects of argon in an in vivo model of transient middle cerebral artery occlusion in rats. Crit Care Med. 2011;39(6):1448–533.
Bhowmick S, D'Mello V, Abdul-Muneer PM. Synergistic inhibition of ERK1/2 and JNK, Not p38, phosphorylation ameliorates neuronal damages after traumatic brain injury. Mol Neurobiol. 2019;56(2):1124–36.
Abdul-Muneer PM, Long M, Conte AA, Santhakumar V, Pfister BJ. High Ca(2+) influx during traumatic brain injury leads to caspase-1-dependent neuroinflammation and cell death. Mol Neurobiol. 2017;54(6):3964–75.
Abdul-Muneer PM, Conte AA, Haldar D, et al. Traumatic brain injury induced matrix metalloproteinase2 cleaves CXCL12alpha (stromal cell derived factor 1alpha) and causes neurodegeneration. Brain Behav Immun. 2017;59:190–9.
Shi H, Hua X, Kong D, Stein D, Hua F. Role of Toll-like receptor mediated signaling in traumatic brain injury. Neuropharmacology. 2019;145(Pt B):259–67.
Ulbrich F, Kaufmann K, Roesslein M, et al. Argon mediates anti-apoptotic signaling and neuroprotection via inhibition of toll-like receptor 2 and 4. PLoS ONE. 2015;10(12):e0143887.
Ulbrich F, Lerach T, Biermann J, et al. Argon mediates protection by interleukin-8 suppression via a TLR2/TLR4/STAT3/NF-kappaB pathway in a model of apoptosis in neuroblastoma cells in vitro and following ischemia-reperfusion injury in rat retina in vivo. J Neurochem. 2016;138(6):859–73.
Fahlenkamp AV, Rossaint R, Haase H, et al. The noble gas argon modifies extracellular signal-regulated kinase 1/2 signaling in neurons and glial cells. Eur J Pharmacol. 2012;674(2–3):104–11.
Abdul-Muneer PM, Chandra N, Haorah J. Interactions of oxidative stress and neurovascular inflammation in the pathogenesis of traumatic brain injury. Mol Neurobiol. 2015;51(3):966–79.
Wu X, Yu T, Xu H, et al. Morphological and functional changes of microglia cultured under different oxygen concentrations and the analysis of related mechanisms. Exp Ther Med. 2018;15(2):2015–9.
Fumagalli S, Perego C, Pischiutta F, Zanier ERD, Simoni MG. The ischemic environment drives microglia and macrophage function. Front Neurol. 2015;6:81.
Thorek DL, Weisshaar CL, Czupryna JC, Winkelstein BA, Tsourkas A. Superparamagnetic iron oxide-enhanced magnetic resonance imaging of neuroinflammation in a rat model of radicular pain. Mol Imaging. 2011;10(3):206–14.
Terrando N, Eriksson LI, Ryu JK, et al. Resolving postoperative neuroinflammation and cognitive decline. Ann Neurol. 2011;70(6):986–95.
Acknowledgements
Special thanks go to Kathy Gage for her support and scientific editing of our work.
Funding
DREAM Award, Duke Anesthesiology to UH; Donald B. Sanders Fund for Residents and Fellows, Duke University to JC.
Author information
Authors and Affiliations
Contributions
The experiments were conceived and designed by JC, UH, DTL. The experiments were performed by JC, UH, VCR, BHY, SM, DC, HW. The data were analyzed by JC, UH, DTL. The paper was written by JC, DAT, UH.
Corresponding author
Ethics declarations
Conflict of interest
There are no competing financial interests.
Ethical Approval
Ethical approvals (IACUC Duke University) were obtained before the study.
Human and Animal Rights
Animal studies followed and adhered to the ARRIVE Guidelines.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Creed, J., Cantillana-Riquelme, V., Yan, B.H. et al. Argon Inhalation for 24 h After Closed-Head Injury Does not Improve Recovery, Neuroinflammation, or Neurologic Outcome in Mice. Neurocrit Care 34, 833–843 (2021). https://doi.org/10.1007/s12028-020-01104-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-020-01104-0