Abstract
Background
Vasopressor agents are used to correct anesthesia-induced hypotension. We describe the effect of phenylephrine and ephedrine on frontal lobe oxygenation (ScO2) following anesthesia-induced hypotension.
Methods
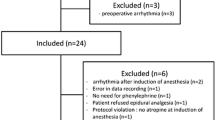
Following induction of anesthesia by fentanyl (0.15 mg kg−1) and propofol (2.0 mg kg−1), 13 patients received phenylephrine (0.1 mg iv) and 12 patients received ephedrine (10 mg iv) to restore mean arterial pressure (MAP). Heart rate (HR), MAP, stroke volume (SV), cardiac output (CO), and frontal lobe oxygenation (ScO2) were registered.
Results
Induction of anesthesia was followed by a decrease in MAP, HR, SV, and CO concomitant with an elevation in ScO2. After administration of phenylephrine, MAP increased (51 ± 12 to 81 ± 13 mmHg; P < 0.001; mean ± SD). However, a 14% (from 70 ± 8% to 60 ± 7%) reduction in ScO2 (P < 0.05) followed with no change in CO (3.7 ± 1.1 to 3.4 ± 0.9 l min−1). The administration of ephedrine led to a similar increase in MAP (53 ± 9 to 79 ± 8 mmHg; P < 0.001), restored CO (3.2 ± 1.2 to 5.0 ± 1.3 l min−1), and preserved ScO2.
Conclusions
The utilization of phenylephrine to correct hypotension induced by anesthesia has a negative impact on ScO2 while ephedrine maintains frontal lobe oxygenation potentially related to an increase in CO.

Similar content being viewed by others
Abbreviations
- CBF:
-
Cerebral blood flow
- CO:
-
Cardiac output
- HR:
-
Heart rate
- MAP:
-
Mean arterial pressure
- NIRS:
-
Near infrared spectroscopy
- ScO2 :
-
Frontal lobe cerebral oxygenation
- SV:
-
Stroke volume
References
Paulson OB, Strandgaard S, Edvinsson L. Cerebral autoregulation. Cerebrovasc Brain Metab Rev. 1990;2:161–92.
Steiner LA, Pfister D, Strebel SP, Radolovich D, Smielewski P, Czosnyka M. Near-infrared spectroscopy can monitor dynamic cerebral autoregulation in adults. Neurocrit Care. 2009;10:122–8.
Nissen P, Pacino H, Frederiksen HJ, Novovic S, Secher NH. Near-infrared spectroscopy for evaluation of cerebral autoregulation during orthotopic liver transplantation. Neurocrit Care. 2009;11:235–41.
Kadoi Y, Saito S, Goto F, Fujita N. Decrease in jugular venous oxygen saturation during normothermic cardiopulmonary bypass predicts short-term postoperative neurologic dysfunction in elderly patients. J Am Coll Cardiol. 2001;38:1450–5.
Yao FS, Tseng CC, Ho CY, Levin SK, Illner P. Cerebral oxygen desaturation is associated with early postoperative neuropsychological dysfunction in patients undergoing cardiac surgery. J Cardiothorac Vasc Anesth. 2004;18:552–8.
Rogers AT, Stump DA, Gravlee GP, Prough DS, Angert KC, Wallenhaupt SL, et al. Response of cerebral blood flow to phenylephrine infusion during hypothermic cardiopulmonary bypass: influence of PaCO2 management. Anesthesiology. 1988;69:547–51.
Mitchell DA, Lambert G, Secher NH, Raven PB, van Lieshout J, Esler MD. Jugular venous overflow of noradrenaline from the brain: a neurochemical indicator of cerebrovascular sympathetic nerve activity in humans. J Physiol 2009; 587:2589–2597
Dinenno FA, Eisenach JH, Dietz NM, Joyner MJ. Post-junctional alpha-adrenoceptors and basal limb vascular tone in healthy men. J Physiol. 2002;540:1103–10.
Brassard P, Seifert T, Secher NH. Is cerebral oxygenation negatively affected by infusion of norepinephrine in healthy subjects? Br J Anaesth. 2009;102:800–5.
Pfister D, Strebel SP, Steiner LA. Effects of catecholamines on cerebral blood vessels in patients with traumatic brain injury. Eur J Anaesthesiol Suppl. 2008;42:98–103.
Madsen PL, Skak C, Rasmussen A, Secher NH. Interference of cerebral near-infrared oximetry in patients with icterus. Anesth Analg. 2000;90:489–93.
Jenstrup M, Ejlersen E, Mogensen T, Secher NH. A maximal central venous oxygen saturation (SvO2max) for the surgical patient. Acta Anaesthesiol Scand Suppl. 1995;107:29–32.
Greif R, Akca O, Horn EP, Kurz A, Sessler DI. Supplemental perioperative oxygen to reduce the incidence of surgical-wound infection. Outcomes Research Group. N Engl J Med. 2000;342:161–7.
Wesseling KH, Jansen JR, Settels JJ, Schreuder JJ. Computation of aortic flow from pressure in humans using a nonlinear, three-element model. J Appl Physiol. 1993;74:2566–73.
Harms MP, Wesseling KH, Pott F, Jenstrup M, Van GJ, Secher NH, et al. Continuous stroke volume monitoring by modelling flow from non-invasive measurement of arterial pressure in humans under orthostatic stress. Clin Sci (Lond). 1999;97:291–301.
Jansen JR, Schreuder JJ, Mulier JP, Smith NT, Settels JJ, Wesseling KH. A comparison of cardiac output derived from the arterial pressure wave against thermodilution in cardiac surgery patients. Br J Anaesth. 2001;87:212–22.
Nissen P, van Lieshout JJ, Novovic S, Bundgaard-Nielsen M, Secher NH. Techniques of cardiac output measurement during liver transplantation: arterial pulse wave versus thermodilution. Liver Transpl. 2009;15:287–91.
Bogert LW, van Lieshout JJ. Non-invasive pulsatile arterial pressure and stroke volume changes from the human finger. Exp Physiol. 2005;90:437–46.
Skak C, Rasmussen A, Kirkegaard P, Secher NH. Cerebral oxygen saturation and blood flow during liver transplantation. Anesth Analg. 1997;84:730–3.
Plachky J, Hofer S, Volkmann M, Martin E, Bardenheuer HJ, Weigand MA. Regional cerebral oxygen saturation is a sensitive marker of cerebral hypoperfusion during orthotopic liver transplantation. Anesth Analg. 2004;99:344–9.
Grubhofer G, Lassnigg A, Manlik F, Marx E, Trubel W, Hiesmayr M. The contribution of extracranial blood oxygenation on near-infrared spectroscopy during carotid thrombendarterectomy. Anaesthesia. 1997;52:116–20.
Vatner SF, Braunwald E. Cardiovascular control mechanisms in the conscious state. N Engl J Med. 1975;293:970–6.
Nissen P, Nielsen HB, van Lieshout JJ, Secher NH. Frontal lobe oxygenation is maintained during hypotension following propofol-phentanyl anesthesia. AANA J. 2009;77:271–6.
Madsen P, Pott F, Olsen SB, Nielsen HB, Burcev I, Secher NH. Near-infrared spectrophotometry determined brain oxygenation during fainting. Acta Physiol Scand. 1998;162:501–7.
Madsen PL, Secher NH. Near-infrared oximetry of the brain. Prog Neurobiol. 1999;58:541–60.
Harms MP, Colier WN, Wieling W, Lenders JW, Secher NH, van Lieshout JJ. Orthostatic tolerance, cerebral oxygenation, and blood velocity in humans with sympathetic failure. Stroke. 2000;31:1608–14.
Njemanze PC. Critical limits of pressure-flow relation in the human brain. Stroke. 1992;23:1743–7.
Kurihara K, Kikukawa A, Kobayashi A, Nakadate T. Frontal cortical oxygenation changes during gravity-induced loss of consciousness in humans: a near-infrared spatially resolved spectroscopic study. J Appl Physiol. 2007;103:1326–31.
Suzuki K, Asahina M, Suzuki A, Hattori T. Cerebral oxygenation monitoring for detecting critical cerebral hypoperfusion in patients with multiple system atrophy during the head-up tilt test. Intern Med. 2008;47:1681–7.
Hunt K, Tachtsidis I, Bleasdale-Barr K, Elwell C, Mathias C, Smith M. Changes in cerebral oxygenation and haemodynamics during postural blood pressure changes in patients with autonomic failure. Physiol Meas. 2006;27:777–85.
Erkinaro T, Makikallio K, Acharya G, Pakkila M, Kavasmaa T, Huhta JC, et al. Divergent effects of ephedrine and phenylephrine on cardiovascular hemodynamics of near-term fetal sheep exposed to hypoxemia and maternal hypotension. Acta Anaesthesiol Scand. 2007;51:922–8.
Dunaway S, Yu Q, Larson DF. Effect of acute alpha adrenergic stimulation on cardiac function. Perfusion. 2007;22:289–92.
Pawelczyk JA, Hanel B, Pawelczyk RA, Warberg J, Secher NH. Leg vasoconstriction during dynamic exercise with reduced cardiac output. J Appl Physiol. 1992;73:1838–46.
Larsen TS, Rasmussen P, Overgaard M, Secher NH, Nielsen HB. Non-selective beta-adrenergic blockade prevents reduction of the cerebral metabolic ratio during exhaustive exercise in humans. J Physiol. 2008;586:2807–15.
Ogoh S, Brothers RM, Barnes Q, Eubank WL, Hawkins MN, Purkayastha S, et al. The effect of changes in cardiac output on middle cerebral artery mean blood velocity at rest and during exercise. J Physiol. 2005;569:697–704.
Ide K, Gullov AL, Pott F, van Lieshout JJ, Koefoed BG, Petersen P, et al. Middle cerebral artery blood velocity during exercise in patients with atrial fibrillation. Clin Physiol. 1999;19:284–9.
Secher NH, Seifert T, van Lieshout JJ. Cerebral blood flow and metabolism during exercise: implications for fatigue. J Appl Physiol. 2008;104:306–14.
Lavi S, Egbarya R, Lavi R, Jacob G. Role of nitric oxide in the regulation of cerebral blood flow in humans: chemoregulation versus mechanoregulation. Circulation. 2003;107:1901–5.
Schleien CL, Koehler RC, Gervais H, Berkowitz ID, Dean JM, Michael JR, et al. Organ blood flow and somatosensory-evoked potentials during and after cardiopulmonary resuscitation with epinephrine or phenylephrine. Circulation. 1989;79:1332–42.
Schwartz AE, Minanov O, Stone JG, Adams DC, Sandhu AA, Pearson ME, et al. Phenylephrine increases cerebral blood flow during low-flow hypothermic cardiopulmonary bypass in baboons. Anesthesiology. 1996;85:380–4.
Strebel SP, Kindler C, Bissonnette B, Tschaler G, Deanovic D. The impact of systemic vasoconstrictors on the cerebral circulation of anesthetized patients. Anesthesiology. 1998;89:67–72.
Ide K, Horn A, Secher NH. Cerebral metabolic response to submaximal exercise. J Appl Physiol. 1999;87:1604–8.
Schaller B. Physiology of cerebral venous blood flow: from experimental data in animals to normal function in humans. Brain Res Rev. 2004;46:243–60.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nissen, P., Brassard, P., Jørgensen, T.B. et al. Phenylephrine but not Ephedrine Reduces Frontal Lobe Oxygenation Following Anesthesia-Induced Hypotension. Neurocrit Care 12, 17–23 (2010). https://doi.org/10.1007/s12028-009-9313-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-009-9313-x