Abstract
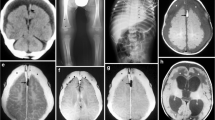
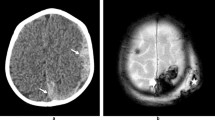
The diagnostic process for evaluating suspected abusive head trauma in infants and children has evolved with technological advances in neuroimaging. Since Caffey first described a series of children with chronic subdural hematomas and multiple long bone fractures, radiologists have played an important role, along with pediatricians and pathologists, in evaluating abused children. Neuroimaging modalities include ultrasound, CT scans, and MRI technology. Each has distinct clinical applications, as well as practical uses in the clinical diagnostic process of AHT. Importantly, neuroimaging assists in the process of differential diagnosis of other conditions which may mimic AHT. Collaboration between neuroradiologists, clinicians, and pathologists remains critical to making the appropriate diagnosis. Careful history, physical examination, and investigation by legal authorities form the components that result in accurate assessment of any case. This paper reviews pertinent neuroimaging modalities currently utilized in the diagnosis of AHT, describing clinical indications and a collaborative approach to this process.















Similar content being viewed by others
References
Frasier LD. Abusive head trauma in infants and young children: a unique contributor to developmental disabilities. Pediatr Clin North Am. 2008;55(6):1269–85. vii.
Caffey J. Multiple fractures in the long bones of infants suffering from chronic subdural hematoma. Am J Roentgen. 1946;56(1):163–73.
Caffey J. The whiplash shaken infant syndrome: manual shaking by the extremities with whiplash-induced intracranial and intraocular bleedings, linked with residual permanent brain damage and mental retardation. Pediatrics. 1974;54(4):396–403.
Jenny C, Hymel KP, Ritzen A, Reinert SE, Hay TC. Analysis of missed cases of abusive head trauma. JAMA. 1999;281(7):621–6.
Vellody K, Freeto JP, Gage SL, Collins N, Gershan WM. Clues that aid in the diagnosis of nonaccidental trauma presenting as an apparent life-threatening event. Clin Pediatr (Phila). 2008;47(9):912–8.
Waseem M, Pinkert H. Apparent life-threatening event or child abuse? Pediatr Emerg Care. 2006;22(4):245–6.
Altman RL, Brand DA, Forman S, et al. Abusive head injury as a cause of apparent life-threatening events in infancy. Arch Pediatr Adolesc Med. 2003;157(10):1011–5.
Demaerel P, Casteels I, Wilms G. Cranial imaging in child abuse. Eur Radiol. 2002;12(4):849–57.
Foerster BR, Petrou M, Lin D, et al. Neuroimaging evaluation of non-accidental head trauma with correlation to clinical outcomes: a review of 57 cases. J Pediatr. 2009;154(4):573–7.
Kemp AM, Rajaram S, Mann M, et al. What neuroimaging should be performed in children in whom inflicted brain injury (iBI) is suspected? A systematic review. Clin Radiol. 2009;64(5):473–83.
Tung GA, Kumar M, Richardson RC, Jenny C, Brown WD. Comparison of accidental and nonaccidental traumatic head injury in children on noncontrast computed tomography. Pediatrics. 2006;118(2):626–33.
Fujiwara T, Okuyama M, Miyasaka M. Characteristics that distinguish abusive from nonabusive head trauma among young children who underwent head computed tomography in Japan. Pediatrics. 2008;122(4):e841–7.
Ashwal S, Holshouser BA, Tong KA. Use of advanced neuroimaging techniques in the evaluation of pediatric traumatic brain injury. Dev Neurosci. 2006;28(4–5):309–26.
Sehgal V, Delproposto Z, Haddar D, et al. Susceptibility-weighted imaging to visualize blood products and improve tumor contrast in the study of brain masses. J Magn Reson Imaging. 2006;24(1):41–51.
Tong KA, Ashwal S, Holshouser BA, et al. Hemorrhagic shearing lesions in children and adolescents with posttraumatic diffuse axonal injury: improved detection and initial results. Radiology. 2003;227(2):332–9.
Babikian T, Freier MC, Ashwal S, Riggs ML, Burley T, Holshouser BA. MR spectroscopy: predicting long-term neuropsychological outcome following pediatric TBI. J Magn Reson Imaging. 2006;24(4):801–11.
Holshouser BA, Tong KA, Ashwal S, et al. Prospective longitudinal proton magnetic resonance spectroscopic imaging in adult traumatic brain injury. J Magn Reson Imaging. 2006;24(1):33–40.
Bonnier C, Marique P, Van Hout A, Potelle D. Neurodevelopmental outcome after severe traumatic brain injury in very young children: role for subcortical lesions. J Child Neurol. 2007;22(5):519–29.
Koumellis P, McConachie NS, Jaspan T. Spinal subdural haematomas in children with non-accidental head injury. Arch Dis Child. 2009;94(3):216–9.
Sato Y, Yuh WT, Smith WL, Alexander RC, Kao SC, Ellerbroek CJ. Head injury in child abuse: evaluation with MR imaging. Radiology. 1989;173(3):653–7.
Levin AV, Magnusson MR, Rafto SE, Zimmerman RA. Shaken baby syndrome diagnosed by magnetic resonance imaging. Pediatr Emerg Care. 1989;5(3):181–6.
Sert A. Cranial ultrasound as a non-invasive diagnostic technique in the diagnosis of subdural haemorrhage. Arch Dis Child. 2007;92(5):468.
Zenger MN, Kabatas S, Zenger S, Cakmakci H. The value of power Doppler ultrasonography in the differential diagnosis of intracranial extraaxial fluid collections. Diagn Interv Radiol. 2007;13(2):61–3.
Looney CB, Smith JK, Merck LH, et al. Intracranial hemorrhage in asymptomatic neonates: prevalence on MR images and relationship to obstetric and neonatal risk factors. Radiology. 2007;242(2):535–41.
Whitby EH, Griffiths PD, Rutter S, et al. Frequency and natural history of subdural haemorrhages in babies and relation to obstetric factors. Lancet. 2004;363(9412):846–51.
Towner D, Castro MA, Eby-Wilkens E, Gilbert WM. Effect of mode of delivery in nulliparous women on neonatal intracranial injury. N Engl J Med. 1999;341(23):1709–14.
Rooks VJ, Eaton JP, Ruess L, Petermann GW, Keck-Wherley J, Pedersen RC. Prevalence and evolution of intracranial hemorrhage in asymptomatic term infants. AJNR Am J Neuroradiol. 2008;29(6):1082–9.
Hellbusch LC. Benign extracerebral fluid collections in infancy: clinical presentation and long-term follow-up. J Neurosurg. 2007;107(2 suppl):119–25.
Aoki N. Extracerebral fluid collections in infancy: role of magnetic resonance imaging in differentiation between subdural effusion and subarachnoid space enlargement. J Neurosurg. 1994;81(1):20–3.
Pittman T. Significance of a subdural hematoma in a child with external hydrocephalus. Pediatr Neurosurg. 2003;39(2):57–9.
Raul JS, Roth S, Ludes B, Willinger R. Influence of the benign enlargement of the subarachnoid space on the bridging veins strain during a shaking event: a finite element study. Int J Legal Med. 2008;122(4):337–40.
McNeely PD, Atkinson JD, Saigal G, O’Gorman AM, Farmer JP. Subdural hematomas in infants with benign enlargement of the subarachnoid spaces are not pathognomonic for child abuse. AJNR Am J Neuroradiol. 2006;27(8):1725–8.
Hubbard D, Tobias JD. Intracerebral hemorrhage due to hemorrhagic disease of the newborn and failure to administer vitamin K at birth. South Med J. 2006;99(11):1216–20.
Per H, Kumandas S, Ozdemir MA, Gumus H, Karakukcu M. Intracranial hemorrhage due to late hemorrhagic disease in two siblings. J Emerg Med. 2006;31(1):49–52.
Feldman KW, Bethel R, Shugerman RP, Grossman DC, Grady MS, Ellenbogen RG. The cause of infant and toddler subdural hemorrhage: a prospective study. Pediatrics. 2001;108(3):636–46.
Trenchs V, Curcoy AI, Navarro R, Pou J. Subdural haematomas and physical abuse in the first two years of life. Pediatr Neurosurg. 2007;43(5):352–7.
Twomey EL, Naughten ER, Donoghue VB, Ryan S. Neuroimaging findings in glutaric aciduria type 1. Pediatr Radiol. 2003;33(12):823–30.
Frasier LD, Rauth-Farley K, Alexander R, Parrish R, editors. Abusive head trauma in infants and children: a medical, legal, and forensic reference. 1st ed. St. Louis: GW Medical Publishing Inc; 2006.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hedlund, G.L., Frasier, L.D. Neuroimaging of abusive head trauma. Forensic Sci Med Pathol 5, 280–290 (2009). https://doi.org/10.1007/s12024-009-9132-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12024-009-9132-6