Abstract
Background
Previous studies have shown that hyperuricemia is involved in diabetes, obesity, hypertension, chronic kidney disease, and other diseases. At the same time, studies have shown that vitamin D3 levels in the body are linked to the onset of diabetes. However, there is currently no sufficient evidence to prove whether this connection is affected by the uric acid level. Therefore, we attempted to investigate the association between vitamin D3 content and the occurrence of diabetes in populations with different uric acid levels though the data of NHANES database from 2009 to 2018.
Method
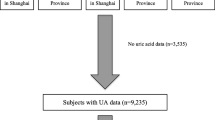
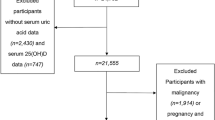
Using the NHANES database, we performed a cross-sectional analysis. The participants were chosen based on stringent inclusion and exclusion requirements. This study finally included a total number of 16,735 individuals. Multivariate logistic regression analysis was used to investigate the association between vitamin D3 and diabetes mellitus in hyperuricemia and non-hyperuricemia patients after complete adjustment, and multivariate linear regression analysis was used to illustrate the association between vitamin D3 and uric acid.
Result
The results showed that the association between vitamin D3 and diabetes was weakened in hyperuricemia patients (OR 0.95 (0.92,0.98)). An independent association was discovered between vitamin D3 and uric acid (β −0.12 (−0.16, −0.07)) in all groups of population.
Conclusions
This study shows that vitamin D3 content is associated with the incidence of diabetes in people with high level of uric acid. This study offers a fresh perspective on the elements that influence the etiology of diabetes in hyperuricemia patients.




Similar content being viewed by others
References
M. Chen-Xu, C. Yokose, S.K. Rai, M.H. Pillinger, H.K. Choi, Contemporary prevalence of gout and hyperuricemia in the United States and Decadal Trends: The National Health and Nutrition Examination Survey, 2007-2016. Arthritis Rheumatol. (Hoboken, N. J.) 71(6), 991–999 (2019)
K.A. Kennel, M.T. Drake, D.L. Hurley, Vitamin D deficiency in adults: when to test and how to treat. Mayo Clin. Proc. 85(8), 752–758 (2010)
P. Song, H. Wang, W. Xia, X. Chang, M. Wang, L. An, Prevalence and correlates of hyperuricemia in the middle-aged and older adults in China. Sci. Rep. 8(1), 4314 (2018)
J. Liu, L. Tao, Z. Zhao, Y. Mu, D. Zou, J. Zhang, X. Guo, Two-year changes in hyperuricemia and risk of diabetes: a five-year prospective cohort study. J. Diabetes Res. 2018, 6905720 (2018)
E. Krishnan, K.S. Akhras, H. Sharma, M. Marynchenko, E.Q. Wu, R. Tawk, J. Liu, L. Shi, Relative and attributable diabetes risk associated with hyperuricemia in US veterans with gout. QJM 106(8), 721–729 (2013)
T. Bardin, P. Richette, Impact of comorbidities on gout and hyperuricaemia: an update on prevalence and treatment options. BMC Med. 15(1), 123 (2017)
N. Katsiki, N. Papanas, V.A. Fonseca, E. Maltezos, D.P. Mikhailidis, Uric acid and diabetes: is there a link? Curr. Pharm. Des. 19(27), 4930–4937 (2013)
D.I. Jalal, Hyperuricemia, the kidneys, and the spectrum of associated diseases: a narrative review. Curr. Med. Res. Opin. 32(11), 1863–1869 (2016)
C. Li, M.C. Hsieh, S.J. Chang, Metabolic syndrome, diabetes, and hyperuricemia. Curr. Opin. Rheumatol. 25(2), 210–216 (2013)
S.B. Woyesa, A.T. Hirigo, T.B. Wube, Hyperuricemia and metabolic syndrome in type 2 diabetes mellitus patients at Hawassa university comprehensive specialized hospital, South West Ethiopia. BMC Endocr. Disord. 17(1), 76 (2017)
C. Borghi, E. Agabiti-Rosei, R.J. Johnson, J.T. Kielstein, E. Lurbe, G. Mancia, J. Redon, A.G. Stack, K.P. Tsioufis, Hyperuricaemia and gout in cardiovascular, metabolic and kidney disease. Eur. J. Intern. Med. 80, 1–11 (2020)
R.J. Johnson, G.L. Bakris, C. Borghi, M.B. Chonchol, D. Feldman, M.A. Lanaspa, T.R. Merriman, O.W. Moe, D.B. Mount, L.G. Sanchez Lozada, E. Stahl, D.E. Weiner, G.M. Chertow, Hyperuricemia, acute and chronic kidney disease, hypertension, and cardiovascular disease: Report of a Scientific Workshop Organized by the National Kidney Foundation. Am. J. Kidney Dis. 71(6), 851–865 (2018)
F.E. García-Arroyo, G. Gonzaga, I. Muñoz-Jiménez, M.G. Blas-Marron, O. Silverio, E. Tapia, V. Soto, N. Ranganathan, P. Ranganathan, U. Vyas, A. Irvin, D. Ir, C.E. Robertson, D.N. Frank, R.J. Johnson, L.G. Sánchez-Lozada, Probiotic supplements prevented oxonic acid-induced hyperuricemia and renal damage. PloS ONE 13(8), e0202901 (2018)
K. Kostka-Jeziorny, K. Widecka, A. Tykarski, Study of epidemiological aspects of hyperuricemia in Poland. Cardiol. J. 26(3), 241–252 (2019)
J.R. Ingelfinger, J.A. Jarcho, Increase in the Incidence of Diabetes and Its Implications. N. Engl. J. Med. 376(15), 1473–1474 (2017). https://doi.org/10.1056/NEJMe1616575
C. Li, M.C. Hsieh, S.J. Chang, Metabolic syndrome, diabetes, and hyperuricemia. Curr. Opin. Rheumatol. 25(2), 210–216 (2013)
F. Baeke, T. Takiishi, H. Korf, C. Gysemans, C. Mathieu, Vitamin D: modulator of the immune system. Curr. Opin. Pharmacol. 10(4), 482–496 (2010). https://doi.org/10.1016/j.coph.2010.04.001
S. Wenclewska, I. Szymczak-Pajor, J. Drzewoski, M. Bunk, A. Śliwińska, Vitamin D supplementation reduces both oxidative DNA damage and insulin resistance in the elderly with metabolic disorders. Int. J. Mol. Sci. 20(12), 2891 (2019).
L. Lu, Q. Lu, W. Chen, J. Li, C. Li, Z. Zheng, Vitamin D3 protects against diabetic retinopathy by inhibiting high-glucose-induced activation of the ROS/TXNIP/NLRP3 inflammasome pathway. J. Diabetes Res. 2018, 8193523 (2018). https://doi.org/10.1155/2018/8193523
D. Caccamo, S. Ricca, M. Currò, R. Ientile, Health risks of hypovitaminosis D: a review of new molecular insights. Int. J. Mol. Sci. 19(3), 892 (2018)
P. Pozzilli, S. Manfrini, A. Crinò, A. Picardi, C. Leomanni, V. Cherubini, L. Valente, M. Khazrai, N. Visalli,IMDIAB group, Low levels of 25-hydroxyvitamin D3 and 1,25-dihydroxyvitamin D3 in patients with newly diagnosed type 1 diabetes. Horm. Metab. Res. 37(11), 680–683 (2005).
Del Pinto, R., Viazzi, F., Pontremoli, R., Ferri, C., Carubbi, F., & Russo, E. The Urrah study. Panminerva Med. https://doi.org/10.23736/S0031-0808.21.04357-3 (2021).
B. Han, N. Wang, Y. Chen, Q. Li, C. Zhu, Y. Chen, Y. Lu, Prevalence of hyperuricaemia in an Eastern Chinese population: a cross-sectional study. BMJ Open 10(5), e035614 (2020)
T. Cederholm, I. Bosaeus, R. Barazzoni, J. Bauer, A. Van Gossum, S. Klek, M. Muscaritoli, I. Nyulasi, J. Ockenga, S.M. Schneider, M.A. de van der Schueren, P. Singer, Diagnostic criteria for malnutrition—an ESPEN Consensus Statement. Clin. Nutr. (Edinb., Scotl.) 34(3), 335–340 (2015)
WHO Expert Consultation, Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. Lancet (Lond., Engl.) 363(9403), 157–163 (2004)
L.A. Lotta, A. Abbasi, S.J. Sharp, A.S. Sahlqvist, D. Waterworth, J.M. Brosnan, R.A. Scott, C. Langenberg, N.J. Wareham, Definitions of metabolic health and risk of future type 2 diabetes in BMI categories: a systematic review and network meta-analysis. Diabetes Care 38(11), 2177–2187 (2015)
American Diabetes Association, (2) Classification and diagnosis of diabetes. Diabetes Care 38(Suppl), S8–S16 (2015)
G.E. White, C. Mair, G.A. Richardson, A.P. Courcoulas, W.C. King, Alcohol Use Among U.S. adults by weight status and weight loss attempt: NHANES, 2011-2016. Am. J. Prevent. Med. 57(2), 220–230 (2019)
W.J. Elliott, Systemic hypertension. Curr. Probl. Cardiol. 32(4), 201–259 (2007)
C. Ricci, A.E. Schutte, R. Schutte, C.M. Smuts, M. Pieters, Trends in alcohol consumption in relation to cause-specific and all-cause mortality in the United States: a report from the NHANES linked to the US mortality registry. Am. J. Clin. Nutr. 111(3), 580–589 (2020)
K.M. Flegal, D. Kruszon-Moran, M.D. Carroll, C.D. Fryar, C.L. Ogden, Trends in obesity among adults in the United States, 2005 to 2014. J. Am. Med. Assoc. USA 315(21), 2284–2291 (2016)
I. Mortada, Hyperuricemia, type 2 diabetes mellitus, and hypertension: an emerging association. Curr. Hypertens. Rep. 19(9), 69 2017). https://doi.org/10.1007/s11906-017-0770-x
A. Stadlmayr, E. Aigner, U. Huber-Schönauer, D. Niederseer, J. Zwerina, E. Husar-Memmer, F. Hohla, G. Schett, W. Patsch, C. Datz, Relations of vitamin D status, gender and type 2 diabetes in middle-aged Caucasians. Acta Diabetol. 52(1), 39–46 (2015). https://doi.org/10.1007/s00592-014-0596-9
K. Łach, K. Krajewski-Siuda, Witamina D3 w prewencji chorób u dorosłych-przeglad systematyczny [Vitamin D3 in prevention of diseases in adults-a systematic review]. Wiadomosci Lekarskie (Warsaw, Poland: 1960) 63, 316–330 (2010)
B. de Courten, A. Mousa, N. Naderpoor, H. Teede, M.P. de Courten, R. Scragg, Vitamin D supplementation for the prevention of type 2 diabetes in overweight adults: study protocol for a randomized controlled trial. Trials 16, 335 2015). https://doi.org/10.1186/s13063-015-0851-6
T.C. Friedman, Vitamin D supplementation to prevent the progression of prediabetes to diabetes: getting closer to a recommendation. Transl. Res. 158(5), 273–275 (2011). https://doi.org/10.1016/j.trsl.2011.06.007
C. Gagnon, R.M. Daly, A. Carpentier, Z.X. Lu, C. Shore-Lorenti, K. Sikaris, S. Jean, P.R. Ebeling, Effects of combined calcium and vitamin D supplementation on insulin secretion, insulin sensitivity and β-cell function in multi-ethnic vitamin D-deficient adults at risk for type 2 diabetes: a pilot randomized, placebo-controlled trial. PLoS ONE 9(10), e109607 (2014). https://doi.org/10.1371/journal.pone.0109607
P.S. George, E.R. Pearson, M.D. Witham, Effect of vitamin D supplementation on glycaemic control and insulin resistance: a systematic review and meta-analysis. Diabet. Med. 29(8), e142–e150 (2012). https://doi.org/10.1111/j.1464-5491.2012.03672.x
Berridge M. J. Vitamin D deficiency and diabetes. Biochem. J. 474(8), 1321–1332 (2017)
P. Lips, M. Eekhoff, N. van Schoor, M. Oosterwerff, R. de Jongh, Y. Krul-Poel, S. Simsek, Vitamin D and type 2 diabetes. J. Steroid Biochem. Mol. Biol. 173, 280–285 (2017)
G.E. Fagundes, T.P. Macan, P. Rohr, A.P. Damiani, F.R. Da Rocha, M. Pereira, L.M. Longaretti, T.C. Vilela, L.B. Ceretta, C. Mendes, P. Silveira, J. Teixeira, V.M. de Andrade, Vitamin D3 as adjuvant in the treatment of type 2 diabetes mellitus: modulation of genomic and biochemical instability. Mutagenesis 34(2), 135–145 (2019)
P. Yu, H. Song, J. Gao, B. Li, Y. Liu, Y. Wang, Vitamin D (1,25-(OH)2D3) regulates the gene expression through competing endogenous RNAs networks in high glucose-treated endothelial progenitor cells. J. Steroid Biochem. Mol. Biol. 193, 105425 (2019). https://doi.org/10.1016/j.jsbmb.2019.105425
K. Chaudhary, K. Malhotra, J. Sowers, A. Aroor, Uric acid—key ingredient in the recipe for cardiorenal metabolic syndrome. Cardiorenal Med. 3(3), 208–220 (2013).
T. Matsuoka, Y. Kajimoto, H. Watada, H. Kaneto, M. Kishimoto, Y. Umayahara, Y. Fujitani, T. Kamada, R. Kawamori, Y. Yamasaki, Glycation-dependent, reactive oxygen species-mediated suppression of the insulin gene promoter activity in HIT cells. J. Clin. Investig. 99(1), 144–150 (1997).
G. Shen, J.Y. Huang, Y.Q. Huang, Y.Q. Feng, The relationship between telomere length and cancer mortality: data from the 1999-2002 National Healthy and Nutrition Examination Survey (NHANES). J. Nutr. Health Aging 24(1), 9–15 (2020)
Author contributions
R. G. and X. W. conceived the idea; R. G. and Z. X. wrote the paper; Z. X. and R. G. collected and read the literature and revised the article; X. W. read through and corrected the paper. All authors read and approved the final paper. R. G. is the first author. Z. X. is the co-first author. X. W. is the corresponding author of this paper.
Funding
This work was Supported by Grants from National Natural Science Foundation of China (81860370), CAS “Light of West China” Program (2019) and the Open Project of State Key Laboratory of Plateau Ecology and Agriculture, Qinghai University (2017-ZZ-15).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethical approval and consent to participate
All participants provided written informed consent, and the study was approved by the NCHS Research Ethics Review Board (https://wwwn.cdc.gov/nchs/nhanes/default.aspx).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gong, R., Xu, Z. & Wei, X. The association between vitamin D3 and diabetes in both hyperuricemia and non-hyperuricemia populations. Endocrine 74, 90–99 (2021). https://doi.org/10.1007/s12020-021-02778-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-021-02778-y