Abstract
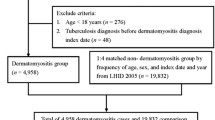
We investigated the relationship between dermatomyositis/polymyositis (DM/PM) and the risk of subsequent osteoporosis development. A population-based retrospective cohort analysis was conducted using the National Health Insurance Research Database and the Catastrophic Illness Patients Database of Taiwan. We included 1179 patients and 4716 patients from 1999 to 2008 as the DM/PM cohort and the comparison cohort, respectively, and calculated the incidence rates of newly diagnosed osteoporosis. We used Cox proportional hazards models stratified on matched pair to assess the effect of DM/PM. The Kaplan–Meier method was applied to estimate the cumulative osteoporosis incidence curves. Patients with DM/PM were 2.99 times more likely to experience osteoporosis than those without DM/PM. The risk for osteoporosis in DM/PM patients was higher than comparisons in different propensity score quartiles. DM/PM cohort, no matter treated with or without corticosteroids and immunosuppressant, had a higher risk than the comparison cohort. The incidence of osteoporosis in Taiwan is associated with a priori DM/PM history. This risk was independent of the corticosteroids and immunosuppressant treatment.

Similar content being viewed by others
Abbreviations
- BMD:
-
Bone mineral density
- BNHI:
-
Bureau of National Health Insurance
- CIPD:
-
Catastrophic Illness Patients Database
- COPD:
-
Chronic obstructive pulmonary disease
- DM:
-
Dermatomyositis
- DXA:
-
Dual energy X-ray absorptiometry
- IHD:
-
Ischemic heart disease
- IIMs:
-
Idiopathic inflammatory myopathies
- LHID:
-
Longitudinal Health Insurance Database
- NHIRD:
-
National Health Insurance Research Database
- OPD:
-
Outpatient department
- PM:
-
Polymyositis
References
M.C. Dalakas, R. Hohlfeld, Polymyositis and dermatomyositis. Lancet 362, 971–982 (2003)
A.E. Hak, B. de Paepe, J.L. de Bleecker, P.P. Tak, M. de Visser, Dermatomyositis and polymyositis: new treatment targets on the horizon. Neth. J. Med. 69, 410–421 (2011)
I. Marie, Morbidity and mortality in adult polymyositis and dermatomyositis. Curr. Rheumatol. Rep. 14, 275–285 (2012)
T.D. Rachner, S. Khosla, L.C. Hofbauer, Osteoporosis: now and the future. Lancet 377, 1276–1287 (2011)
A. Leboime, C.B. Confavreux, N. Mehsen, J. Paccou, C. David, C. Roux, Osteoporosis and mortality. Joint Bone Spine 77, S107–S112 (2010)
W.A. Stewart, P.D. Acott, S.R. Salisbury, B.A. Lang, Bone mineral density in juvenile dermatomyositis: assessment using dual X-ray absorptiometry. Arthritis Rheum. 48, 2294–2298 (2003)
K.A. Alsufyani, O. Ortiz-Alvarez, D.A. Cabral, L.B. Tucker, R.E. Petty, H. Nadel, P.N. Malleson, Bone mineral density in children and adolescents with systemic lupus erythematosus, juvenile dermatomyositis, and systemic vasculitis: relationship to disease duration, cumulative corticosteroid dose, calcium intake, and exercise. J. Rheumatol. 32, 729–733 (2005)
T.C. Castro, M.T. Terreri, V.L. Szejnfeld, C. Len, A.S. Fonseca, M.O. Hilario, Bone mineral density of Brazilian girls with juvenile dermatomyositis. Braz. J. Med. Biol. Res. 38, 309–313 (2005)
D.C. de Andrade, S.C. de Magalhaes Souza, J.F. de Carvalho, L. Takayama, C.T. Borges, J.M. Aldrighi, R.M. Pereira, High frequency of osteoporosis and fractures in women with dermatomyositis/polymyositis. Rheumatol. Int. 32, 1549–1553 (2012)
R.A. Santiago, C.A. Silva, V.F. Caparbo, A.M. Sallum, R.M. Pereira, Bone mineral apparent density in juvenile dermatomyositis: the role of lean body mass and glucocorticoid use. Scand. J. Rheumatol. 37, 40–47 (2008)
T.P. van Staa, H.G. Leufkens, C. Cooper, The epidemiology of corticosteroid-induced osteoporosis: a meta-analysis. Osteoporos. Int. 13, 777–787 (2002)
R.B. Mazess, G.D. Whedon, Immobilization and bone. Calcif. Tissue Int. 35, 265–267 (1983)
D.L. Kamen, J.D. Alele, Skeletal manifestations of systemic autoimmune diseases. Curr. Opin. Endocrinol. Diabetes Obes. 17, 540–545 (2010)
D. Kamen, C. Aranow, Vitamin D in systemic lupus erythematosus. Curr. Opin. Rheumatol. 20, 532–537 (2008)
S.A. Stechschulte, R.S. Kirsner, D.G. Federman, Vitamin D: bone and beyond, rationale and recommendations for supplementation. Am. J. Med. 122, 793–802 (2009)
J.M. Grossman, R. Gordon, V.K. Ranganath, C. Deal, L. Caplan, W. Chen, J.R. Curtis, D.E. Furst, M. McMahon, N.M. Patkar, E. Volkmann, K.G. Saag, American College of Rheumatology 2010, Recommendations for the prevention and treatment of glucocorticoid-induced osteoporosis. Arthritis. Care Res. (Hoboken) 62, 1515–1526 (2010)
D. Liu, A. Ahmet, L. Ward, P. Krishnamoorthy, E.D. Mandelcorn, R. Leigh, J.P. Brown, A. Cohen, H. Kim, A practical guide to the monitoring and management of the complications of systemic corticosteroid therapy. Allergy Asthma Clin. Immunol. 9, 30 (2013)
J.M. Quinn, H. Saleh, Modulation of osteoclast function in bone by the immune system. Mol. Cell. Endocrinol. 310, 40–51 (2009)
S. Kotake, N. Udagawa, M. Hakoda, M. Mogi, K. Yano, E. Tsuda, K. Takahashi, T. Furuya, S. Ishiyama, K.J. Kim, S. Saito, T. Nishikawa, N. Takahashi, A. Togari, T. Tomatsu, T. Suda, N. Kamatani, Activated human T cells directly induce osteoclastogenesis from human monocytes: possible role of T cells in bone destruction in rheumatoid arthritis patients. Arthritis. Rheum. 44, 1003–1012 (2001)
K. Sato, A. Suematsu, K. Okamoto, A. Yamaguchi, Y. Morishita, Y. Kadono, S. Tanaka, T. Kodama, S. Akira, Y. Iwakura, D.J. Cua, H. Takayanagi, Th17 functions as an osteoclastogenic helper T cell subset that links T cell activation and bone destruction. J. Exp. Med. 203, 2673–2682 (2006)
C.L. Cheng, Y.H. Kao, S.J. Lin, C.H. Lee, M.L. Lai, Validation of the National Health Insurance Research Database with ischemic stroke cases in Taiwan. Pharmacoepidemiol. Drug Saf. 20, 236–242 (2011)
W.Q. Gan, S.F. Man, A. Senthilselvan, D.D. Sin, Association between chronic obstructive pulmonary disease and systemic inflammation: a systematic review and a meta-analysis. Thorax 59, 574–580 (2004)
Acknowledgments
This study is supported in part by Taiwan Ministry of Health and Welfare Clinical Trial and Research Center of Excellence (MOHW104-TDU-B-212-113002); China Medical University Hospital, Academia Sinica Taiwan Biobank, Stroke Biosignature Project (BM104010092); NRPB Stroke Clinical Trial Consortium (MOST 103-2325-B-039 -006); Tseng-Lien Lin Foundation, Taichung, Taiwan; Taiwan Brain Disease Foundation, Taipei, Taiwan; Katsuzo and Kiyo Aoshima Memorial Funds, Japan; and CMU under the Aim for Top University Plan of the Ministry of Education, Taiwan.
Author contributions
The individual contributions of the authors are listed as follows. Conception and design: Cynthia Wei-Sheng Lee and Chia-Hung Kao. Administrative support: Chih-Hsin Muo and Fung-Chang Sung. Data collection and assembly: Cynthia Wei-Sheng Lee, Ji-An Liang, and Chia-Hung Kao. Data analysis and interpretation: Cynthia Wei-Sheng Lee and Chia-Hung Kao. Manuscript writing and final approval of the manuscript: All authors. The guarantor of the paper assumes responsibility for the integrity of the work as a whole: Chia-Hung Kao.
Funding
The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript. No additional external funding was received for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure statement
All authors state that they have no conflicts of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Lee, C.WS., Muo, CH., Liang, JA. et al. Increased osteoporosis risk in dermatomyositis or polymyositis independent of the treatments: a population-based cohort study with propensity score. Endocrine 52, 86–92 (2016). https://doi.org/10.1007/s12020-015-0756-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-015-0756-x