Abstract
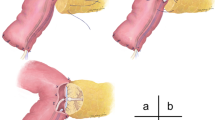
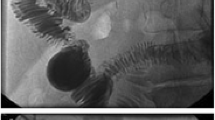
This study’s objective was to test the new drainage apparatus called enclosed passive infraversion lavage–drainage system (EPILDS) in the treatment of bile leakage and pancreatic fistula Post Pancreatoduodenectomys. The EPILDS device has a design of a siphon. The inlet bag that contains the rinse liquid is put lower than the abdominal lacuna to be washed but higher than the outlet bag. The hydrostatic pressure difference between the inlet and outlet bags constitutes the driving force of the flow. The three-way cock valves are installed in the inlet and outlet tubes to facilitate the washing of occluded tubes. Two side by side Penrose drainage tubes were placed during the operation. One tube passed through the posterior side of pancreatico-jejunal and biliary-jejunal anastomoses, right paracolic gutter, and exited through an opening made in the right lower abdomen. Second tube came from the smaller sac, went through the anterior side of pancreatico-jejunal and biliary-jejunal anastomoses, and exited through an opening made in the left upper abdomen. Using this system, we successfully treated two patients. Both inlet and outlet volumes were observed to verify that the outlet exceeds the inlet volume. In conclusion, EPILDS has a simple and practical design. It changes the active washing process into a passive one, in which the input is controlled by the exiting fluid. This is the effective and safe system for treatment of severe bile leakage and pancreatic fistula at the early postoperative stage.



Similar content being viewed by others
References
Yeo, C. J., Cameron, J. L., Sohn, T. A., Lillemoe, K. D., Pitt, H. A., Talamini, M. A., et al. (1997). Six hundred fifty consecutive pancreaticoduodenectomies in the 1990s: pathology, complications, and outcomes. Annals of Surgery, 226, 248–257.
Bartoli, F. G., Arnone, G. B., Ravera, G., & Bachi, V. (1991). Pancreatic fistula and relative mortality in malignant disease after pancreaticoduodenectomy. Review and statistical meta-analysis regarding 15 years of literature. Anticancer Research, 11, 1831–1848.
Yeo, C. J., Cameron, J. L., Maher, M. M., Sauter, P. K., Zahurak, M. L., Talamini, M. A., et al. (1995). A prospective randomized trial of pancreaticogastrostomy versus pancreaticojejunostomy after pancreaticoduodenectomy. Annals of Surgery, 222, 580–588.
van Berge Henegouwen, M. I., Allema, J. H., van Gulik, T. M., Verbeek, P. C., Obertop, H., & Gouma, D. J. (1995). Delayed massive haemorrhage after pancreatic and biliary surgery. British Journal of Surgery, 1995(82), 1527–1531.
Shankar, R., & Russel, R. C. G. (1995). Hemorrhage in pancreatic disease. British Journal of Surgery, 1995, 1527–1531.
Brodsky, J. T., & Turnbull, A. D. (1991). Arterial hemorrhage after pancreatoduodenectomy. The ‘sentinel bleed’. Archives of Surgery, 126, 1037–1040.
Stojadinovic, A., Brooks, A., Hoos, A., Jaques, D. P., Conlon, K. C., & Brennan, M. F. (2003). An evidence-based approach to the surgical management of resectable pancreatic adenocarcinoma. Journal of the American College of Surgeons, 196, 954–964.
Buchler, M. W., Wagner, M., Schmied, B. M., Uhl, W., Friess, H., & Z’graggen, K. (2003). Changes in morbidity after pancreatic resection: toward the end of completion pancreatectomy. Archives of Surgery, 138, 1310–1314.
Halloran, C. M., Ghaneh, P., Bosonnet, L., Hartley, M. N., Sutton, R., & Neoptolemos, J. P. (2002). Complications of pancreatic cancer resection. Digestive Surgery, 19, 138–146.
Berberat, P. O., Friess, H., Kleeff, J., Uhl, W., & Buchler, M. W. (1999). Prevention and treatment of complications in pancreatic cancer surgery. Digestive Surgery, 16, 327–336.
Ho, C. K., Kleeff, J., Friess, H., & Buchler, M. W. (2005). Complications of pancreatic surgery. HPB (Oxford), 7, 99–108.
Wente, M. N., Veit, J. A., Bassi, C., Dervenis, C., Fingerhut, A., Gouma, D. J., et al. (2007). Postpancreatectomy hemorrhage (PPH): an International Study Group of Pancreatic Surgery (ISGPS) definition. Surgery, 142, 20–25.
Koch, M., Garden, O. J., Padbury, R., Rahbari, N. N., Adam, R., Capussotti, L., et al. (2011). Bile leakage after hepatobiliary and pancreatic surgery: a definition and grading of severity by the International Study Group of Liver Surgery. Surgery, 149, 680–688.
Bassi, C., Dervenis, C., Butturini, G., Fingerhut, A., Yeo, C., Izbicki, J., et al. (2005). Postoperative pancreatic fistula: an international study group (ISGPF) definition. Surgery, 138, 8–13.
Cullen, J. J., Sarr, M. G., & Ilstrup, D. M. (1994). Pancreatic anastomotic leak after pancreaticoduodenectomy: incidence, significance, and management. American Journal of Surgery, 168, 295–298.
Trede, M., Saeger, H. D., Schwall, G., & Rumstadt, B. (1998). Resection of pancreatic cancer-surgical achievements. Langenbecks Archives of Surgery, 383, 121–128.
Suzuki, Y., Fujino, Y., Tanioka, Y., Hiraoka, K., Takada, M., Ajiki, T., et al. (2002). Selection of pancreaticojejunostomy techniques according to pancreatic texture and duct size. Archives of Surgery, 137, 1044–1047.
Bassi, C., Falconi, M., Salvia, R., Mascetta, G., Molinari, E., & Pederzoli, P. (2001). Management of complications after pancreaticoduodenectomy in a high volume centre: results on 150 consecutive patients. Digestive Surgery, 18, 453–457.
Bradley, E. L, III. (2002). Pancreatoduodenectomy for pancreatic adenocarcinoma: triumph, triumphalism, or transition? Archives of Surgery, 137, 771–773.
Author information
Authors and Affiliations
Corresponding author
Additional information
Kai Jiang and Wenzhi Zhang have contributed equally to this study and should be considered co-first authors.
Rights and permissions
About this article
Cite this article
Jiang, K., Zhang, W., Feng, Y. et al. Enclosed Passive Infraversion Lavage–Drainage System (EPILDS): A Novel Safe Technique for Local Management of Early Stage Bile Leakage and Pancreatic Fistula Post Pancreatoduodenectomy. Cell Biochem Biophys 68, 541–546 (2014). https://doi.org/10.1007/s12013-013-9735-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12013-013-9735-0