Abstract
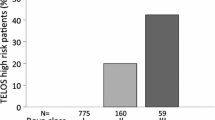
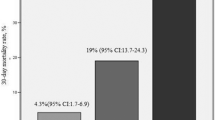
Normotensive patients with acute pulmonary embolism (APE) are accompanied by heterogeneously adverse events. Responding to tissue injury, lipocalin-2 (LCN-2) is elevated in experimental APE model and associated with short-term prognosis. However, the prognostic value of LCN-2 in normotensive patients with APE for long-term major adverse events (MAEs) remains unknown. We evaluated the association of plasma LCN-2 levels with the median 467-day outcome in 170 normotensive patients with APE. We also assessed whether LCN-2 could improve risk stratification. MAEs consisted of mortality or recurrence of venous thromboembolism. During follow-up, 17 (10%) patients suffered from MAEs. These patients had higher LCN-2 levels compared with patients without MAEs (median: 13.97 vs. 8.55 ng/ml, P = 0.01). The proportion of MAEs in the intermediate–low-risk group (14.0%) was higher than that in the intermediate–high-risk group (5.3%). LCN-2 levels independently had prognostic value for MAEs in overall (HR = 3.40, 95% CI 1.46–7.90) and intermediate-risk group (HR = 3.88, 95% CI 1.63–9.23). LCN-2 also showed incremental value in overall (ΔC-index: 0.13, 95% CI 0.02–0.24; category-based NRI = 0.25, 95% CI 0.07–0.42) and intermediate-risk patients (ΔC-index: 0.13, 95% CI 0.05–0.31; category-based NRI = 0.44, 95% CI 0.24–0.65). Adding LCN-2 (cut-off value = 11 ng/ml) to the current risk algorithm improved MAEs of intermediate–risk reclassification (intermediate–high vs. intermediate–low = 25.6% vs. 6.0%, P = 0.002). Elevated plasma LCN-2 levels predict long-term MAEs among normotensive patients with APE. LCN-2 might be a useful biomarker for risk stratification in the intermediate-risk group.






Similar content being viewed by others
References
Konstantinides, S. V., Torbicki, A., Agnelli, G., Danchin, N., Fitzmaurice, D., Galie, N., et al. (2014). 2014 ESC guidelines on the diagnosis and management of acute pulmonary embolism. European Heart Journal. https://doi.org/10.1093/eurheartj/ehu283.
Saar, J. A., & Maack, C. (2015). Diagnosis and management of acute pulmonary embolism. ESC guidelines 2014. Herz,40(8), 1048–1054. https://doi.org/10.1007/s00059-015-4378-0.
Dellas, C., Puls, M., Lankeit, M., Schafer, K., Cuny, M., Berner, M., et al. (2010). Elevated heart-type fatty acid-binding protein levels on admission predict an adverse outcome in normotensive patients with acute pulmonary embolism. Journal of the American College of Cardiology,55(19), 2150–2157. https://doi.org/10.1016/j.jacc.2009.10.078.
Dursunoglu, N., Dursunoglu, D., Yildiz, A. I., & Rota, S. (2016). Evaluation of cardiac biomarkers and right ventricular dysfunction in patients with acute pulmonary embolism. Anatolian Journal of Cardiology,16(4), 276–282. https://doi.org/10.5152/akd.2014.5828.
Bozbay, M., Uyarel, H., Avsar, S., Oz, A., Keskin, M., Murat, A., et al. (2016). Admission glucose level predicts in-hospital mortality in patients with acute pulmonary embolism who were treated with thrombolytic therapy. Lung,194(2), 219–226. https://doi.org/10.1007/s00408-016-9858-3.
Tatlisu, M. A., Kaya, A., Keskin, M., Avsar, S., Bozbay, M., Tatlisu, K., et al. (2017). The association of blood urea nitrogen levels with mortality in acute pulmonary embolism. Journal of Critical Care,39, 248–253. https://doi.org/10.1016/j.jcrc.2016.12.019.
Tanabe, Y., Obayashi, T., Yamamoto, T., Takayama, M., & Nagao, K. (2015). Predictive value of biomarkers for the prognosis of acute pulmonary embolism in Japanese patients: Results of the Tokyo CCU Network registry. Journal of Cardiology,66(6), 460–465. https://doi.org/10.1016/j.jjcc.2015.03.002.
Zagorski, J., Sanapareddy, N., Gellar, M. A., Kline, J. A., & Watts, J. A. (2008). Transcriptional profile of right ventricular tissue during acute pulmonary embolism in rats. Physiological Genomics,34(1), 101–111. https://doi.org/10.1152/physiolgenomics.00261.2007.
Kjeldsen, L., Bainton, D. F., Sengelov, H., & Borregaard, N. (1994). Identification of neutrophil gelatinase-associated lipocalin as a novel matrix protein of specific granules in human neutrophils. Blood,83(3), 799–807.
Xiao, X., Yeoh, B. S., & Vijay-Kumar, M. (2017). Lipocalin 2: An emerging player in iron homeostasis and inflammation. Annual Review of Nutrition,37, 103–130. https://doi.org/10.1146/annurev-nutr-071816-064559.
Glaros, T., Fu, Y., Xing, J., & Li, L. (2012). Molecular mechanism underlying persistent induction of LCN2 by lipopolysaccharide in kidney fibroblasts. PLoS ONE,7(4), e34633. https://doi.org/10.1371/journal.pone.0034633.
Sola, A., Weigert, A., Jung, M., Vinuesa, E., Brecht, K., Weis, N., et al. (2011). Sphingosine-1-phosphate signalling induces the production of Lcn-2 by macrophages to promote kidney regeneration. The Journal of Pathology,225(4), 597–608. https://doi.org/10.1002/path.2982.
Yndestad, A., Landro, L., Ueland, T., Dahl, C. P., Flo, T. H., Vinge, L. E., et al. (2009). Increased systemic and myocardial expression of neutrophil gelatinase-associated lipocalin in clinical and experimental heart failure. European Heart Journal,30(10), 1229–1236. https://doi.org/10.1093/eurheartj/ehp088.
Eilenberg, W., Stojkovic, S., Kaider, A., Kozakowski, N., Domenig, C. M., Burghuber, C., et al. (2017). NGAL and MMP-9/NGAL as biomarkers of plaque vulnerability and targets of statins in patients with carotid atherosclerosis. Clinical Chemistry and Laboratory Medicine,56(1), 147–156. https://doi.org/10.1515/cclm-2017-0156.
Helanova, K., Spinar, J., & Parenica, J. (2014). Diagnostic and prognostic utility of neutrophil gelatinase-associated lipocalin (NGAL) in patients with cardiovascular diseases–review. Kidney & blood pressure research.,39(6), 623–629. https://doi.org/10.1159/000368474.
Mishra, J., Ma, Q., Prada, A., Mitsnefes, M., Zahedi, K., Yang, J., et al. (2003). Identification of neutrophil gelatinase-associated lipocalin as a novel early urinary biomarker for ischemic renal injury. Journal of the American Society of Nephrology: JASN,14(10), 2534–2543.
Maisel, A. S., Mueller, C., Fitzgerald, R., Brikhan, R., Hiestand, B. C., Iqbal, N., et al. (2011). Prognostic utility of plasma neutrophil gelatinase-associated lipocalin in patients with acute heart failure: the NGAL EvaLuation Along with B-type NaTriuretic Peptide in acutely decompensated heart failure (GALLANT) trial. European Journal of Heart Failure,13(8), 846–851. https://doi.org/10.1093/eurjhf/hfr087.
Kostrubiec, M., Labyk, A., Pedowska-Wloszek, J., Dzikowska-Diduch, O., Wojciechowski, A., Garlinska, M., et al. (2012). Neutrophil gelatinase-associated lipocalin, cystatin C and eGFR indicate acute kidney injury and predict prognosis of patients with acute pulmonary embolism. Heart,98(16), 1221–1228. https://doi.org/10.1136/heartjnl-2012-301884.
Polo Friz, H., Corno, V., Orenti, A., Buzzini, C., Crivellari, C., Petri, F., et al. (2017). Comorbidity assessment as predictor of short and long-term mortality in elderly patients with hemodynamically stable acute pulmonary embolism. Journal of Thrombosis and Thrombolysis,44(3), 316–323. https://doi.org/10.1007/s11239-017-1540-y.
Kreit, J. W. (2004). The impact of right ventricular dysfunction on the prognosis and therapy of normotensive patients with pulmonary embolism. Chest,125(4), 1539–1545.
Sydykov, A., Mamazhakypov, A., Petrovic, A., Kosanovic, D., Sarybaev, A. S., Weissmann, N., et al. (2018). Inflammatory mediators drive adverse right ventricular remodeling and dysfunction and serve as potential biomarkers. Frontiers in Physiology,9, 609. https://doi.org/10.3389/fphys.2018.00609.
Dewachter, L., & Dewachter, C. (2018). Inflammation in right ventricular failure: Does It matter? Frontiers in Physiology,9, 1056. https://doi.org/10.3389/fphys.2018.01056.
Campian, M. E., Hardziyenka, M., de Bruin, K., van Eck-Smit, B. L., de Bakker, J. M., Verberne, H. J., et al. (2010). Early inflammatory response during the development of right ventricular heart failure in a rat model. European Journal of Heart Failure,12(7), 653–658. https://doi.org/10.1093/eurjhf/hfq066.
Sung, H. K., Chan, Y. K., Han, M., Jahng, J. W. S., Song, E., Danielson, E., et al. (2017). Lipocalin-2 (NGAL) attenuates autophagy to exacerbate cardiac apoptosis induced by myocardial ischemia. Journal of Cellular Physiology,232(8), 2125–2134. https://doi.org/10.1002/jcp.25672.
Chan, Y. K., Sung, H. K., Jahng, J. W., Kim, G. H., Han, M., & Sweeney, G. (2016). Lipocalin-2 inhibits autophagy and induces insulin resistance in H9c2 cells. Molecular and Cellular Endocrinology,430, 68–76. https://doi.org/10.1016/j.mce.2016.04.006.
Marques, F. Z., Prestes, P. R., Byars, S. G., Ritchie, S. C., Wurtz, P., Patel, S. K., et al. (2017). Experimental and human evidence for Lipocalin-2 (Neutrophil gelatinase-associated lipocalin [NGAL]) in the development of cardiac hypertrophy and heart failure. Journal of the American Heart Association. https://doi.org/10.1161/JAHA.117.005971.
Tarjus, A., Martinez-Martinez, E., Amador, C., Latouche, C., El Moghrabi, S., Berger, T., et al. (2015). Neutrophil gelatinase-associated lipocalin, a novel mineralocorticoid biotarget, mediates vascular profibrotic effects of mineralocorticoids. Hypertension,66(1), 158–166. https://doi.org/10.1161/HYPERTENSIONAHA.115.05431.
Becattini, C., Agnelli, G., Lankeit, M., Masotti, L., Pruszczyk, P., Casazza, F., et al. (2016). Acute pulmonary embolism: mortality prediction by the 2014 European Society of Cardiology risk stratification model. European Respiratory Journal,48(3), 780–786. https://doi.org/10.1183/13993003.00024-2016.
Zhou, X. Y., Ben, S. Q., Chen, H. L., & Ni, S. S. (2012). The prognostic value of pulmonary embolism severity index in acute pulmonary embolism: a meta-analysis. Respiratory Research,13, 111. https://doi.org/10.1186/1465-9921-13-111.
Vinson, D. R., Ballard, D. W., Mark, D. G., Huang, J., Reed, M. E., Rauchwerger, A. S., et al. (2016). Risk stratifying emergency department patients with acute pulmonary embolism: Does the simplified Pulmonary Embolism Severity Index perform as well as the original? Thrombosis Research,148, 1–8. https://doi.org/10.1016/j.thromres.2016.09.023.
Gussoni, G., Frasson, S., La Regina, M., Di Micco, P., & Monreal, M. (2013). Three-month mortality rate and clinical predictors in patients with venous thromboembolism and cancer. Findings from the RIETE registry. Thrombosis Research,131(1), 24–30. https://doi.org/10.1016/j.thromres.2012.10.007.
Alotaibi, G., Wu, C., Senthilselvan, A., & McMurtry, M. S. (2018). Short- and long-term mortality after pulmonary embolism in patients with and without cancer. Vascular Medicine (London, England),23(3), 261–266. https://doi.org/10.1177/1358863x18754692.
Liu, X., Chang, S., Fu, C., Huo, Z., Zhou, J., Liu, C., et al. (2017). Predictors of mid-term prognosis and adverse factors in acute pulmonary embolism. Therapeutic Advances in Respiratory Disease,11(8), 293–300. https://doi.org/10.1177/1753465817717168.
Wicki, J., Perrier, A., Perneger, T. V., Bounameaux, H., & Junod, A. F. (2000). Predicting adverse outcome in patients with acute pulmonary embolism: a risk score. Thrombosis and Haemostasis,84(4), 548–552.
Acknowledgements
This study was supported by the National Natural Science Foundation of China (Grant No. 81790622), Beijing Municipal Science & Technology Commission (Grant No. Z171100000417002), Chinese Academy of Medical Sciences Innovation Fund for Medical Sciences (Grant No. 2017-I2 M-3-003), and Capital Clinical Characteristic Application Program (Grant No. 2018-BKJ01). We thank Ellen Knapp, PhD, from Liwen Bianji, Edanz Group China (www.liwenbianji.cn/ac), for editing the English text of a draft of this manuscript.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Handling Editor: Y. James Kang.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Yu, H., Liu, Z., Lu, J. et al. Lipocalin-2 Predicts Long-Term Outcome of Normotensive Patients with Acute Pulmonary Embolism. Cardiovasc Toxicol 20, 101–110 (2020). https://doi.org/10.1007/s12012-019-09525-w
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12012-019-09525-w