Abstract
Background
MRI is the gold standard for evaluating the relationship of disc material to soft tissue and neural structures. However, terminologies used to describe lumbar disc herniation and nerve root compression have always been a source of confusion. A clear understanding of lumbar disc terminology among clinicians, radiologists, and researchers is vital for patient care and future research.
Questions/purposes
Through a systematic review of the literature, the purpose of this article is to describe lumbar disc terminology and comment on the reliability of various nomenclature systems and their application to clinical practice.
Methods
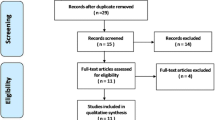
PubMed was used for our literature search using the following MeSH headings: “Magnetic Resonance Imaging and Intervertebral Disc Displacement” and “Lumbar Vertebrae” and terms “nomenclature” or “grading” or “classification”. Ten papers evaluating lumbar disc herniation/nerve root compression using different grading criteria and providing information regarding intraobserver and interobserver agreement were identified.
Results
To date, the Combined Task Force (CTF) and van Rijn classification systems are the most reliable methods for describing lumbar disc herniation and nerve root compression, respectively. van Rijn dichotomized nerve roots from “definitely no root compression, possibly no root compression, indeterminate root compression, possible root compression, and definite root compression” into no root compression (first three categories) and root compression (last two categories). The CTF classification defines lumbar discs as normal, focal protrusion, broad-based protrusion, or extrusion. The CTF classification system excludes “disc bulges,” which is a source of confusion and disagreement among many practitioners. This potentially accounts for its improved reliability compared with other proposed nomenclature systems.
Conclusions
The main issue in the management of patients with lumbar disc disease and nerve root compression is correlation of imaging findings with clinical presentation and symptomatology to guide treatment and intervention. Although it appears that the most commonly supported nomenclatures have strong interobserver reliability, the classification term “disc bulges” is a source of confusion and disagreement among many practitioners. Additional research should focus on the clinical application of the various nomenclatures.
Similar content being viewed by others
References
Arana E, Kovacs FM, Royuela A, Estremera A, Sarasibar H, Amengual G, Galarraga I, Martinez C, Muriel A, Abraira V, Zamora J, Campillo C. Influence of nomenclature in the interpretation of lumbar disk contour on MR imaging: a comparison of the agreement using the combined task force and the nordic nomenclatures. AJNR Am J Neuroradiol. 2011;32:1143–1148.
Brant-Zawadzki MN, Jensen MC, Obuchowski N, Ross JS, Modic MT. Interobserver and intraobserver variability in interpretation of lumbar disc abnormalities. A comparison of two nomenclatures. Spine. 1995;20:1257–1263; discussion 1264.
Brennan TA, Leape LL, Laird NM, Hebert L, Localio AR, Lawthers AG, Newhouse JP, Weiler PC, Hiatt HH. Incidence of adverse events and negligence in hospitalized patients. Results of the Harvard Medical Practice Study I. N Engl J Med. 1991;324:370–376.
Fardon DF. Nomenclature and classification of lumbar disc pathology. Spine. 2001;26:461–462.
Imaad-ur-Rehman, Hamid RS, Akhtar W, Shamim MS, Naqi R, Siddiq HI. Observer variation in MRI evaluation of patients with suspected lumbar disc herniation and nerve root compression: comparison of neuroradiologist and neurosurgeon’s interpretations. J Pak Med Assoc. 2012;62:826–829.
Jarvik JG, Haynor DR, Koepsell TD, Bronstein A, Ashley D, Deyo RA. Interreader reliability for a new classification of lumbar disk disease. Acad Radiol. 1996;3:537–544.
Jensen MC, Brant-Zawadzki MN, Obuchowski N, Modic MT, Malkasian D, Ross JS. Magnetic resonance imaging of the lumbar spine in people without back pain. N Engl J Med. 1994;331:69–73.
Kreiner SD HS, Easa J, Resnick DK, Baisden J, Bess S, Cho CH, DePalma MJ, Dougherty P, Fernand R, Ghiselli G, Hanna AS, Lamer T, Lisi AJ, Mazanec DJ, Meagher RJ, Nucci RC, Patel RD, Sembrano JN, Sharma AK, Summers JT, Taleghani CK, Tontz WL, Toton JF. Clinical guidelines for diagnosis and treatment of lumbar disc herniation with radiculopathy. North American Spine Society; 2012. Available at: www.spine.org/Documents/ResearchClinicalCare/Guidelines/LumbarDiscHerniation.pdf. Accessed November-December 2013.
Lurie JD, Tosteson AN, Tosteson TD, Carragee E, Carrino JA, Kaiser J, Sequeiros RT, Lecomte AR, Grove MR, Blood EA, Pearson LH, Herzog R, Weinstein JN. Reliability of magnetic resonance imaging readings for lumbar disc herniation in the Spine Patient Outcomes Research Trial (SPORT). Spine. 2008;33:991–998.
Mysliwiec LW, Cholewicki J, Winkelpleck MD, Eis GP. MSU classification for herniated lumbar discs on MRI: toward developing objective criteria for surgical selection. Eur Spine J. 2010;19:1087–1093.
Pfirrmann CW, Dora C, Schmid MR, Zanetti M, Hodler J, Boos N. MR image-based grading of lumbar nerve root compromise due to disk herniation: reliability study with surgical correlation. Radiology. 2004;230:583–588.
Solgaard Sorensen J, Kjaer P, Jensen ST, Andersen P. Low-field magnetic resonance imaging of the lumbar spine: reliability of qualitative evaluation of disc and muscle parameters. Acta Radiol. 2006;47:947–953.
Thomas EJ, Studdert DM, Newhouse JP, Zbar BI, Howard KM, Williams EJ, Brennan TA. Costs of medical injuries in Utah and Colorado. Inquiry. 1999;36:255–264.
van Rijn JC, Klemetso N, Reitsma JB, Majoie CB, Hulsmans FJ, Peul WC, Stam J, Bossuyt PM, den Heeten GJ. Observer variation in MRI evaluation of patients suspected of lumbar disk herniation. AJR Am J Roentgenol. 2005;184:299–303.
Acknowledgments
We thank Dr Reitman for the opportunity to contribute to the CORR® symposium on disc herniation as well as our supporting institution, faculty, and staff.
Author information
Authors and Affiliations
Corresponding author
Additional information
Each author certifies that he or she, or a member of his or her immediate family, has no funding or commercial associations (eg, consultancies, stock ownership, equity interest, patent/licensing arrangements, etc) that might pose a conflict of interest in connection with the submitted article.
All ICMJE Conflict of Interest Forms for authors and Clinical Orthopaedics and Related Research ® editors and board members are on file with the publication and can be viewed on request.
Electronic supplementary material
Below is the link to the electronic supplementary material.
About this article
Cite this article
Li, Y., Fredrickson, V. & Resnick, D.K. How Should We Grade Lumbar Disc Herniation and Nerve Root Compression? A Systematic Review. Clin Orthop Relat Res 473, 1896–1902 (2015). https://doi.org/10.1007/s11999-014-3674-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11999-014-3674-y