Abstract
Background
Intertrochanteric hip fractures pose a significant challenge for the orthopaedic community as optimal surgical treatment continues to be debated. Currently, varus collapse with lag screw cutout is the most common mode of failure. Multiple factors contribute to cutout. From a surgical technique perspective, a tip apex distance less than 25 mm has been suggested to decrease the risk of cutout. We hypothesized that a low-center lag screw position in the femoral head, with a tip apex distance greater than 25 mm will provide equal, if not superior, biomechanical stability compared with a center-center position with a tip apex distance less than 25 mm in an unstable intertrochanteric hip fracture stabilized with a long cephalomedullary nail.
Questions/purposes
We attempted to examine the biomechanical characteristics of intertrochanteric fractures instrumented with long cephalomedullary nails with two separate lag screw positions, center-center and low-center. Our first research purpose was to examine if there was a difference between the center-center and low-center groups in cycles to failure and failure load. Second, we analyzed if there was a difference in fracture translation between the study groups during loading.
Methods
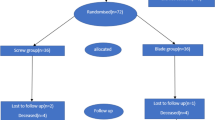
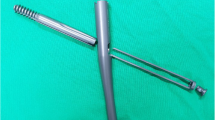
Nine matched pairs of femurs were assigned to one of two treatment groups: low-center lag screw position and center-center lag screw position. Cephalomedullary nails were placed and tip apex distance was measured. A standard unstable four-part intertrochanteric fracture was created in all samples. The femurs were loaded dynamically until failure. Cycles to failure and load and displacement data were recorded, and three-dimensional (3-D) motion was recorded using an Optotrak® motion tracking system.
Results
There were no significant differences between the low-center and center-center treatment groups regarding the mean number of cycles to failure and mean failure load. The 3-D kinematic data showed significantly increased motion in the center-center group compared with the low-center group. At the time of failure, the magnitude of fracture translation was statistically significantly greater in the center-center group (20 ± 2.8 mm) compared with the low-center group (15 ± 3.4 mm; p = 0.004). Additionally, there was statistically significantly increased fracture gap distraction (center-center group, 13 ± 2.8 versus low-center group, 7 ± 4; p < 0.001) and shear fracture gap translation (center-center group, 12 ± 2.3 mm; low-center group, 6 ± 2.7 mm; p < 0.001).
Conclusions
Positioning of the lag screw inferior in the head and neck was found to be at least as biomechanically stable as the center-center group although the tip apex distance was greater than 25 mm.
Clinical Relevance
Our findings challenge previously accepted principles of optimal lag screw placement.





Similar content being viewed by others
References
Baumgaertner MR, Curtin SL, Lindskog DM, Keggi JM. The value of the tip-apex distance in predicting failure of fixation of peritrochanteric fractures of the hip. J Bone Joint Surg Am. 1995;77:1058–1064.
De Bruijn K, den Hartog D, Tuinebreijer W, Roukema G. Reliability of predictors for screw cutout in intertrochanteric hip fractures. J Bone Joint Surg Am. 2012;94:1266–1272.
Haynes RC, Poll RG, Miles AW, Weston RB. An experimental study of the failure modes of the Gamma Locking Nail and AO Dynamic Hip Screw under static loading: a cadaveric study. Med Eng Phys. 1997;19:446–453.
Haynes RC, Poll RG, Miles AW, Weston RB. Failure of femoral head fixation: a cadaveric analysis of lag screw cut-out with the gamma locking nail and AO dynamic hip screw. Injury. 1997;28:337–341.
Jang IG, Kim IY. Computational study of Wolff’s law with trabecular architecture in the human proximal femur using topology optimization. J Biomech. 2008;41:2353–2361.
Kaufer H, Matthews LS, Sonstegard D. Stable fixation of intertrochanteric fractures. J Bone Joint Surg Am. 1974;56:899–907.
Kim WY, Han CH, Park JI, Kim JY. Failure of intertrochanteric fracture fixation with a dynamic hip screw in relation to pre-operative fracture stability and osteoporosis. Int Orthop. 2001;25:360–362.
Kouvidis GK, Sommers MB, Giannoudis PV, Katonis PG, Bottlang M. Comparison of migration behavior between single and dual lag screw implants for intertrochanteric fracture fixation. J Orthop Surg Res. 2009;4:16.
Kubiak EN, Bong M, Park SS, Kummer F, Egol K, Koval KJ. Intramedullary fixation of unstable intertrochanteric hip fractures: one or two lag screws. J Orthop Trauma. 2004;18:12–17.
Kuzyk PR, Zdero R, Shah S, Olsen M, Waddell JP, Schemitsch EH. Femoral head lag screw position for cephalomedullary nails: a biomechanical analysis. J Orthop Trauma. 2012; 26:414–421.
Laskin RS, Gruber MA, Zimmerman AJ. Intertrochanteric fractures of the hip in the elderly: a retrospective analysis of 236 cases. Clin Orthop Relat Res. 1979;141:188–195.
12 Lenz M, Perren SM, Gueorguiev B, Richards RG, Hofmann GO, Fernandez dell’Oca A, Hontzsch D, Windolf M. A biomechanical study on proximal plate fixation techniques in periprosthetic femur fractures. Injury. 2014; 45(suppl 1):S71–75.
Lorich DG, Geller DS, Nielson JH. Osteoporotic pertrochanteric hip fractures: management and current controversies. Instr Course Lect. 2004;53:441–454.
Parker MJ. Trochanteric hip fractures: fixation failure commoner with femoral medialization, a comparison of 101 cases. Acta Orthop Scand. 1996;67:329–332.
Simpson AH, Varty K, Dodd CA. Sliding hip screws: modes of failure. Injury. 1989;20:227–231.
Strauss E, Frank J, Lee J, Kummer FJ, Tejwani N. Helical blade versus sliding hip screw for treatment of unstable intertrochanteric hip fractures: a biomechanical evaluation. Injury. 2006;37:984–989.
Topp T, Muller T, Huss S, Kann PH, Weihe E, Ruchholtz S, Zettl RP. Embalmed and fresh frozen human bones in orthopedic cadaveric studies: which bone is authentic and feasible? Acta Orthop. 2012;83:543–547.
Wu CC, Shih CH, Lee MY, Tai CL. Biomechanical analysis of location of lag screw of a dynamic hip screw in treatment of unstable intertrochanteric fracture. J Trauma. 1996;41:699–702.
Acknowledgments
The research was supported by [RIH Orthopaedic Foundation] and the National Institutes of Health [P20-GM104937 (COBRE Bioengineering Core)].
Author information
Authors and Affiliations
Corresponding author
Additional information
One of the authors (CB) certifies that he, or a member of his immediate family, has or may receive payments or benefits, during the study period, an amount of USD 10,000–USD 100,000 from Stryker Orthopaedics (Mahwah, NJ, USA); one author (CB) has stock in BioIntraface (North Kingston, RI, USA) and IlluminOss (Riverside, RI, USA).
Intramedullary nails and instrumentation equipment were provided by Stryker.
All ICMJE Conflict of Interest Forms for authors and Clinical Orthopaedics and Related Research editors and board members are on file with the publication and can be viewed on request.
Clinical Orthopaedics and Related Research neither advocates nor endorses the use of any treatment, drug, or device. Readers are encouraged to always seek additional information, including FDA-approval status, of any drug or device prior to clinical use.
Each author certifies that his or her institution approved the human protocol for this investigation, that all investigations were conducted in conformity with ethical principles of research, and that informed consent for participation in the study was obtained.
This work was performed at RIH Orthopaedic Foundation, Inc, Providence, RI, USA.
About this article
Cite this article
Kane, P., Vopat, B., Heard, W. et al. Is Tip Apex Distance As Important As We Think? A Biomechanical Study Examining Optimal Lag Screw Placement. Clin Orthop Relat Res 472, 2492–2498 (2014). https://doi.org/10.1007/s11999-014-3594-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11999-014-3594-x