Abstract
Background
Tranexamic acid (TXA) reduces blood loss and transfusion after total joint arthroplasty (TJA) but concerns remain that patients with severe medical comorbidities might be at increased risk for thromboembolic complications.
Questions/purposes
Among patients undergoing primary TJA with severe systemic medical disease, (1) was TXA associated with increased symptomatic thromboembolic events; (2) was TXA associated with decreased blood transfusion rates; and (3) were there differences in symptomatic thromboembolism or transfusions in the subset of patients with a history of, or risk factors for; thromboembolic disease?
Methods
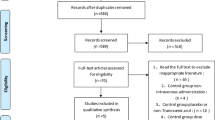
We performed a retrospective review of 1131 primary TJAs in 1002 patients with American Society of Anesthesiologists score III or IV. Of these, 402 had at least one of seven risk factors for thromboembolic events and were designated as high risk; 240 of those patients received TXA. Outcome measures included 30-day postoperative symptomatic thromboembolic events and postoperative transfusion.
Results
There were no differences in symptomatic thromboembolic events within 30 days of surgery between patients who received TXA and those who did not (2.5% versus 2.6%, p = 0.97). Fewer patients treated with TXA received transfusions (11% with versus 41% without; p < 0.0001). In high-risk patients, TXA was not associated with an increase in symptomatic thromboembolic events (6.7% with versus 4.3% without; p = 0.27) and was associated with a decrease in transfusion rates (17% with versus 48% without; p = 0.001).
Conclusions
Although TXA seemed safe and effective in this database review of patients with severe medical comorbidities, a larger prospective trial is warranted to confirm these results.
Level of Evidence
Level III, therapeutic study. See Guidelines for Authors for a complete description of levels of evidence.
Similar content being viewed by others
References
Alvarez JC, Santiveri FX, Ramos I, Vela E, Puig L, Escolano F. Tranexamic acid reduces blood transfusion in total knee arthroplasty even when a blood conservation program is applied. Transfusion. 2008;48:519–525.
Benoni G, Fredin H, Knebel R, Nilsson P. Blood conservation with tranexamic acid in total hip arthroplasty: a randomized, double-blind study in 40 primary operations. Acta Orthop Scand. 2001;72:442–448.
Bierbaum B, Callaghan J, Galante J, Rubash H, Tooms R, Welch R. An analysis of blood management in patients having a total hip or knee arthroplasty. J Bone Joint Surg Am. 1999;81:2–10.
Camarasa MA, Olle G, Serra-Prat M, Martin A, Sanchez M, Ricos P, Perez A, Opisso L. Efficacy of aminocaproic, tranexamic acids in the control of bleeding during total knee replacement: a randomized clinical trial. Br J Anaesth. 2006;96:576–582.
Cid J, Lozano M. Tranexamic acid reduces allogeneic red cell transfusions in patients undergoing total knee arthroplasty: results of a meta-analysis of randomized controlled trials. Transfusion. 2005;45:1302–1307.
DailyMed [Internet]. Bethesda, MD, USA: National Library of Medicine; 2006 [updated February 26, 2013 Feb 26]. Current medication information: Cyklokapraon (tranexamic acid). Available at: http://dailymed.nlm.nih.gov/dailymed/lookup.cfm?setid=6e89a7d9-4da4-42aa-b7f8-c602c24eefe5. Accessed April 25, 2013.
Dunn CJ, Goa KL. Tranexamic acid: a review of its use in surgery and other indications. Drugs. 1999;57:1005–1032.
Engel JM, Hohaus T, Ruwoldt R, Menges T, Jurgensen I, Hempelmann G. Regional hemostatic status and blood requirements after total knee arthroplasty with and without tranexamic acid or aprotinin. Anesth Analg. 2001;92:775–780.
Eubanks JD. Antifibrinolytics in major orthopaedic surgery. J Am Acad Orthop Surg. 2010;18:132–138.
Fergusson DA, Hebert PC, Mazer CD, Fremes S, MacAdams C, Murkin JM, Teoh K, Duke PC, Arellano R, Blajchman MA, Bussieres JS, Cote D, Karski J, Martineau R, Robblee JA, Rodger M, Wells G, Clinch J, Pretorius R. A comparison of aprotinin and lysine analogues in high-risk cardiac surgery. N Engl J Med. 2008;358:2319–2331.
Gill JB, Rosenstein A. The use of antifibrinolytic agents in total hip arthroplasty: a meta-analysis. J Arthroplasty. 2006;21:869–873.
Gillette B, DeSimone L, Trousdale R, Pagnano M, Sierra R. Low risk of thromboembolic complications with tranexamic acid after primary total hip and knee arthroplasty. Clin Orthop Relat Res. 2013;471:150–154.
Henry DA, Carless PA, Moxey AJ, O’Connell D, Stokes BJ, Fergusson DA, Ker K. Anti-fibrinolytic use for minimising perioperative allogeneic blood transfusion. Cochrane Database Syst Rev. 2011;3:CD001886.
Hiippala ST, Strid LJ, Wennerstrand MI, V Arvela JV, Niemala HM, Mantyla SK, Kuisma RP, Ylienen JE. Tranexamic acid radically decreases blood loss and transfusions associated with total knee arthroplasty. Anesth Analg. 1997;84:839–844.
Ho KM, Ismail H. Use of intravenous tranexamic acid to reduce allogeneic blood transfusion in total hip and knee arthroplasty: a meta-analysis. Anaesth Intensive Care. 2003;31:529–537.
Hutton B, Joseph L, Fergusson D, Mazer CD, Shapiro S, Tinmouth A. Risks of harms using antifibrinolytics in cardiac surgery: systematic review and network meta-analysis of randomised and observational studies. Br Med J. 2012; 345:e5798.
Hynes M, Calder P, Scott G. The use of tranexamic acid to reduce blood loss during total knee arthroplasty. Knee. 2003;10:375–377.
Kagoma YK, Crowther MA, Douketis J, Bhandari M, Eikelboom J, Lim W. Use of antifibrinolytic therapy to reduce transfusion in patients undergoing orthopedic surgery: a systematic review of randomized trials. Thromb Res. 2009;123:687–696.
Lee GC, Hawes T, Cushner FD, Scott WN. Current trends in blood conservation in total knee arthroplasty. Clin Orthop Relat Res. 2005;440:170–174.
Lemay E, Guay J, Cote C, Roy A. Tranexamic acid reduces the need for allogenic red blood cell transfusions in patients undergoing total hip replacement. Can J Anaesth. 2004;51:31–37.
Murkin JM, Haig GM, Beer KJ, Cicutti N, McCutchen J, Comunale ME, Hall R, Ruzicka BB. Aprotinin decreases exposure to allogeneic blood during primary unilateral total hip replacement. J Bone Joint Surg Am. 2000;82:675–684.
Sehat K, Evans R, Newman J. Hidden blood loss following hip and knee arthroplasty. J Bone Joint Surg Br. 2004;86:561–565.
Shiga T, Wajima Z, Inoue T, Sakamoto A. Aprotinin in major orthopedic surgery: a systematic review of randomized controlled trials. Anesth Analg. 2005;101:1602–1607.
Slaughter TF, Greenberg CS. Antifibrinolytic drugs and perioperative hemostasis. Am J Hematol. 1997;56:32–36.
Veien M, Sorensen JV, Madsen F, Juelsgaard P. Tranexamic acid given intraoperatively reduces blood loss after total knee replacement: a randomized, controlled study. Acta Anaesthesiol Scand. 2002;46:1206–1211.
Yamasaki S, Masuhara K, Fuji T. Tranexamic acid reduces postoperative blood loss in cementless total hip arthroplasty. J Bone Joint Surg Am. 2005;87:766–770.
Yang Z, Chen W, Wu L. Effectiveness and safety of tranexamic acid in reducing blood loss in total knee arthroplasty: a meta-analysis. J Bone Joint Surg Am. 2012;94:1153–1159.
Zohar E, Fredman B, Ellis MH, Ifrach N, Stern A, Jedeikin R. A comparative study of the postoperative allogeneic blood-sparing effects of tranexamic acid and of desmopressin after total knee replacement. Transfusion. 2001;41:1285–1289.
Acknowledgments
We thank Robert T. Trousdale MD, for his assistance with this research and the following for their assistance in data analysis and verification: Christina Wood-Wentz MS, and Jordan Rosedahl BA, of the Division of Biomedical Statistics and Informatics as well as the staff of the Department of Transfusion Medicine.
Author information
Authors and Affiliations
Corresponding author
Additional information
One of the authors (MWP) certifies that he has or may receive payments or benefits, in any one year, an amount in excess of USD 100,000 from DePuy (Warsaw, IN, USA), MAKO Surgical Corp (Ft Lauderdale, FL, USA), and Stryker Orthopaedics (Mahwah, NJ, USA). One or more of the authors (RJS) certifies that he has or may receive payments or benefits, in any one year, an amount in excess of USD 10,000 from Biomet Inc (Warsaw, IN, USA).
All ICMJE Conflict of Interest Forms for authors and Clinical Orthopaedics and Related Research editors and board members are on file with the publication and can be viewed on request.
Each author certifies that his or her institution approved the human protocol for this investigation, that all investigations were conducted in conformity with ethical principles of research, and that informed consent for participation in the study was obtained.
About this article
Cite this article
Whiting, D.R., Gillette, B.P., Duncan, C. et al. Preliminary Results Suggest Tranexamic Acid is Safe and Effective in Arthroplasty Patients with Severe Comorbidities. Clin Orthop Relat Res 472, 66–72 (2014). https://doi.org/10.1007/s11999-013-3134-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11999-013-3134-0