Abstract
Background
The Basic Arthroscopic Knee Skill Scoring System (BAKSSS) has construct validity as an objective measure of arthroscopic proficiency when used to assess the task of performing arthroscopic meniscectomies on cadaver knees. The reliability of this instrument is unknown.
Questions/purpose
We asked whether (1) a simple modification of the BAKSSS would show construct validity similar to that in the initial BAKSSS study, (2) this assessment would be reliable, and (3) this assessment could be used as a high-stakes pass or fail test.
Methods
Twenty-three orthopaedic residents performed diagnostic knee arthroscopies on cadaveric knee specimens. Their competency was assessed by three live raters using the modified BAKSSS. Interrater reliability was assessed by comparing the scores given by each rater to each subject.
Results
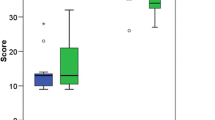
The modified BAKSSS showed construct validity with junior residents achieving lower scores (mean score, 20) than senior residents (mean score, 33). The modified BAKSSS had an interrater reliability of kappa = 0.685–0.852. The modified BAKSSS had a kappa = 0.543 when used as a proficiency test for diagnostic arthroscopy.
Conclusions
The modified BAKSSS is useful for assessing diagnostic knee arthroscopy proficiency. Future scoring systems should be designed to be generalizable so they can be applied to multiple procedures without the need for modification, allow for video-based assessment, and must be rigorously tested for reliability and other types of validity (eg, face validity, content validity, and criterion-related validity).
Clinical Relevance
Having a valid and reliable assessment of basic arthroscopic procedures may allow educators to more adequately evaluate individual residents and the effectiveness of various training modalities.



Similar content being viewed by others
References
Alvand A, Auplish S, Gill H, Rees J. Innate arthroscopic skills in medical students and variation in learning curves. J Bone Joint Surg Am. 2011;93:e115(111–119).
Atesok K, Mabrey JD, Jazrawi LM, Egol KA. Surgical simulation in orthopaedic skills training. J Am Acad Orthop Surg. 2012;20:410–422.
Ceponis PJ, Chan D, Boorman RS, Hutchison C, Mohtadi NG. A randomized pilot validation of educational measures in teaching shoulder arthroscopy to surgical residents. Can J Surg. 2007;50:387–393.
Doyle JD, Webber EM, Sidhu RS. A universal global rating scale for the evaluation of technical skills in the operating room. Am J Surg. 2007;193:551–555; discussion 555.
Gumbs AA, Hogle NJ, Fowler DL. Evaluation of resident laparoscopic performance using global operative assessment of laparoscopic skills. J Am Coll Surg. 2007;204:308–313.
Howells NR, Gill HS, Carr AJ, Price AJ, Rees JL. Transferring simulated arthroscopic skills to the operating theatre: a randomised blinded study. J Bone Joint Surg Br. 2008;90:494–499.
Hoyle AC, Whelton C, Umaar R, Funk L. Validation of a global rating scale for shoulder arthroscopy: a pilot study. Shoulder Elbow. 2012;4:16–21.
Insel A, Carofino B, Leger R, Arciero R, Mazzocca AD. The development of an objective model to assess arthroscopic performance. J Bone Joint Surg Am. 2009;91:2287–2295.
Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics. 1977;33:159–174.
Martin JA, Regehr G, Reznick R, MacRae H, Murnaghan J, Hutchison C, Brown M. Objective structured assessment of technical skill (OSATS) for surgical residents. Br J Surg. 1997;84:273–278.
Mitchell EL, Arora S, Moneta GL. Ensuring vascular surgical training is on the right track. J Vasc Surg. 2011;53:517–525.
Pedowitz RA, Marsh JL. Motor skills training in orthopaedic surgery: a paradigm shift toward a simulation-based educational curriculum. J Am Acad Orthop Surg. 2012;20:407–409.
Reznick R, Regehr G, MacRae H, Martin J, McCulloch W. Testing technical skill via an innovative “bench station” examination. Am J Surg. 1997;173:226–230.
Sonnadara RR, Van Vliet A, Safir O, Alman B, Ferguson P, Kraemer W, Reznick R. Orthopedic boot camp: examining the effectiveness of an intensive surgical skills course. Surgery. 2011;149:745–749.
Tashiro Y, Miura H, Nakanishi Y, Okazaki K, Iwamoto Y. Evaluation of skills in arthroscopic training based on trajectory and force data. Clin Orthop Relat Res. 2009;467:546–552.
Van Heest A, Putnam M, Agel J, Shanedling J, McPherson S, Schmitz C. Assessment of technical skills of orthopaedic surgery residents performing open carpal tunnel release surgery. J Bone Joint Surg Am. 2009;91:2811–2817.
VanHeest A, Kuzel B, Agel J, Putnam M, Kalliainen L, Fletcher J. Objective structured assessment of technical skill in upper extremity surgery. J Hand Surg Am. 2012;37:332–337 337.e4.
Van Nortwick SS, Lendvay TS, Jensen AR, Wright AS, Horvath KD, Kim S. Methodologies for establishing validity in surgical simulation studies. Surgery. 2010;147:622–630.
Vassiliou MC, Feldman LS, Andrew CG, Bergman S, Leffondre K, Stanbridge D, Fried GM. A global assessment tool for evaluation of intraoperative laparoscopic skills. Am J Surg. 2005;190:107–113.
Vassiliou MC, Feldman LS, Fraser SA, Charlebois P, Chaudhury P, Stanbridge DD, Fried GM. Evaluating intraoperative laparoscopic skill: direct observation versus blinded videotaped performances. Surg Innov. 2007;14:211–216.
Vassiliou MC, Kaneva PA, Poulose BK, Dunkin BJ, Marks JM, Sadik R, Sroka G, Anvari M, Thaler K, Adrales GL, Hazey JW, Lightdale JR, Velanovich V, Swanstrom LL, Mellinger JD, Fried GM. Global Assessment of Gastrointestinal Endoscopic Skills (GAGES): a valid measurement tool for technical skills in flexible endoscopy. Surg Endosc. 2010;24:1834–1841.
Acknowledgments
We thank Rachel Johnston for assistance in formatting this manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
Each author certifies that he or she has no commercial associations (eg, consultancies, stock ownership, equity interest, patent/licensing arrangements, etc) that might pose a conflict of interest in connection with the submitted article.
All ICMJE Conflict of Interest Forms for authors and Clinical Orthopaedics and Related Research editors and board members are on file with the publication and can be viewed on request.
Clinical Orthopaedics and Related Research neither advocates nor endorses the use of any treatment, drug, or device. Readers are encouraged to always seek additional information, including FDA-approval status, of any drug or device prior to clinical use.
Each author certifies that his or her institution approved the human protocol for this investigation, that all investigations were conducted in conformity with ethical principles of research, and that informed consent for participation in the study was obtained.
Appendix 1: Modified BAKSSS Global Rating Scale
Appendix 1: Modified BAKSSS Global Rating Scale
Instrument handling
-
1- Repeatedly makes tentative or awkward movements with instruments
-
2-
-
3- Competent use of instruments, although occasionally appeared stiff or awkward
-
4-
-
5- Fluid moves with instruments and no awkwardness
Depth perception
-
1- Constantly overshoots target, slow to correct
-
2-
-
3- Some overshooting or missing of target
-
4-
-
5- Accurately directs instruments in the correct plane to target
Bimanual dexterity
-
1- Noticeably awkward with nondominant hand, poor coordination between hands
-
2-
-
3- Uses both hands but does not maximize interaction between hands
-
4-
-
5- Expertly uses both hands in complementary manner to provide optimum performance
Flow of operation and forward planning
-
1- Frequently stopped operating or needed to discuss next move
-
2-
-
3- Demonstrated ability for forward planning with steady progression of operative procedure
-
4-
-
5- Obviously planned course of operation with effortless flow from one move to the next
Knowledge of instruments
-
1- Frequently asked for the wrong instrument or used inappropriate instrument
-
2-
-
3- Knew the names of most instruments and used appropriate instrument for the task
-
4-
-
5- Obviously familiar with the instruments required and their names
Efficiency
-
1- Many unnecessary, inefficient movements, constantly changing focus or persisting without progress
-
2-
-
3- Slow but planned movements are reasonably organized with few unnecessary or repetitive movements
-
4-
-
5- Confident, clear economy of movement and maximum efficiency.
Knowledge of specific procedure
-
1- Deficient knowledge, needed specific instruction at most operative steps
-
2-
-
3- Knew all important aspects of the operation
-
4-
-
5- Demonstrated familiarity with all aspects of the operation
Autonomy
-
1- Unable to complete entire task, even with verbal guidance
-
2-
-
3- Able to complete task safely with moderation guidance
-
4-
-
5- Able to complete task independently without prompting
Quality
-
1- Very poor
-
2-
-
3- Competent
-
4-
-
5- Clearly superior
About this article
Cite this article
Olson, T., Koehler, R., Butler, A. et al. Is there a Valid and Reliable Assessment of Diagnostic Knee Arthroscopy Skill?. Clin Orthop Relat Res 471, 1670–1676 (2013). https://doi.org/10.1007/s11999-012-2744-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11999-012-2744-2