Abstract
Background
Open débridement with polyethylene liner exchange (ODPE) remains a relatively low morbidity option in acute infection of total knee arthroplasty (TKA), but concerns regarding control of infection exist. We sought to identify factors that would predict control of infection after ODPE.
Methods
We identified 44 patients (44 knees) with culture-positive periprosthetic infection who underwent ODPE. Failure was defined as any reoperation performed for control of infection or the need for lifetime antibiotic suppression. Patients had been followed prospectively for a minimum of 1 year (mean, 5 years; range, 1–9 years).
Results
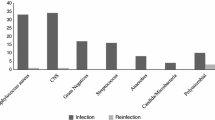
Twenty-five of the 44 patients (57%) failed ODPE. Of these 25 patients, two had one additional procedure, 21 had more than one additional procedure, and two required lifetime antibiotic suppression. Failure rates tended to differ based on primary organism: 71% of Staphylococcus aureus periprosthetic infection failed versus 29% of Staphylococcus epidermidis, although with the limited numbers theses differences were not significant. Age, gender, or measures of comorbidity did not influence the risk of failure. There was no difference in failure rate (58% versus 50%) when the ODPE was performed greater than 4 weeks after index TKA. After a failed ODPE, 19 of the 25 failures went on to an attempted two-stage revision procedure. In only 11 of these 19 cases was the two-stage revision ultimately successful.
Conclusions
Eradication of infection with ODPE in acute TKA infections is unpredictable; certain factors trend toward increased success but no firm algorithm can be offered. The success of two-stage revision for infection may be diminished after a failed ODPE.
Level of Evidence
Level III, retrospective comparative study. See Guidelines for Authors for a complete description of levels of evidence.

Similar content being viewed by others
References
Bozic KJ, Kurtz SM, Lau E, Ong K, Chiu V, Vail TP, Rubash HE, Berry DJ. The epidemiology of revision total knee arthroplasty in the United States. Clin Orthop Relat Res. 2009;468:45–51.
Brandt CM, Sistrunk WW, Duffy MC, Hanssen AD, Steckelberg JM, Ilstrup DM, Osmon DR. Staphylococcus aureus prosthetic joint infection treated with débridement and prosthesis retention. Clin Infect Dis. 1997;24:914–919.
Burger RR, Basch T, Hopson CN. Implant salvage in infected total knee arthroplasty. Clin Orthop Relat Res. 1991;273:105–112.
Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: Development and Validation. J Chronic Dis. 1987;40:373–383.
Deirmengian C, Greenbaum J, Stern J, Braffman M, Lotke PA, Booth RE, Lonner JH. Open débridement of acute Gram-positive infections after total knee arthroplasty. Clin Orthop Relat Res. 2003;416:129–134.
Dripps RD. New classification of physical status. Anesthesiology. 1963;24:111.
Gioe TJ, Killeen KK, Mehle S, Grimm K. Implementation and application of a community total joint registry: a twelve year history. J Bone Joint Surg Am. 2006;88:1399–1404.
Goldman RT, Scuderi GR, Insall JN. Two-stage reimplantation for infected total knee replacement. Clin Orthop Relat Res. 1996;331:118–124.
Haleem AA, Berry DJ, Hanssen AD. Mid-term to long-term followup of two-stage reimplantation for infected total knee arthroplasty. Clin Orthop Relat Res. 2004;428:35–39.
Hartman MB, Fehring TK, Jordan L, Norton HJ. Periprosthetic knee sepsis: the role of irrigation and débridement. Clin Orthop Relat Res. 1991;273:113–118.
Insall JN, Thompson FM, Brause BD. Two-stage reimplantation for the salvage of infected total knee arthroplasty. J Bone Joint Surg Am. 1983;65:1087–1098.
Kurtz SM, Ong KL, Lau E, Bozick KJ, Berry D, Parvizi J. Prosthetic joint infection risk following TKA in the Medicare population. Clin Orthop Relat Res. 2009;468:52–56.
Leone JM, Hanssen AD. Management of infection at the site of a total knee arthroplasty. J Bone Joint Surg Am. 2005;87:2335–2348.
Marculescu CE, Berbari EF, Hanssen AD, Steckelberg JM, Harmsen SW, Mandrekar JN, Osmon DR. Outcome of prosthetic joint infections treated with débridement and retention of components. Clin Infect Dis. 2006;42:471–478.
Mont MA, Waldman B, Banerjee C, Pacheco IH, Hungerford DS. Multiple irrigation, débridement, and retention of components in infected total knee arthroplasty. J Arthroplasty. 1997;12:426–433.
Schoifet SD, Morrey BF. Treatment of infection after total knee arthroplasty by débridement with retention of the components. J Bone Joint Surg Am. 1990;72:1383–1390.
Segawa H, Tysukama D, Kyle RF, Becker DA, Gustilo RB. Infection after total knee arthroplasty. A retrospective study of the treatment of eighty-one infections. J Bone Joint Surg Am. 1999;81:1434–1445.
Tattevin P, Cremieux AC, Pottier P, Huten D, Carbon C. prosthetic joint infection: when can prosthesis salvage be considered? Clin Infect Dis. 1999;29:292–295.
Teeny SM, Dorr L, Murata G, Conaty P. Treatment of infected total knee arthroplasty. Irrigation and débridement versus two-stage reimplantation. J Arthroplasty. 1990;5:35–39.
Windsor RE, Insall JN, Urs WK, Miller DV, Brause BD. Two-stage reimplantation for the salvage of total knee arthroplasty complicated by infection. J Bone Joint Surg Am. 1990;72:272–278.
Author information
Authors and Affiliations
Corresponding author
Additional information
Each author certifies that he or she has no commercial associations (eg, consultancies, stock ownership, equity interest, patent/licensing arrangements, etc) that might pose a conflict of interest in connection with the submitted article.
Each author certifies that his or her institution approved the human protocol for this investigation, that all investigations were conducted in conformity with ethical principles of research, and that informed consent for participation in the study was obtained.
This work was performed at the Minneapolis Veterans Administration Medical Center and the HealthEast Hospitals, St Paul, MN, USA.
About this article
Cite this article
Gardner, J., Gioe, T.J. & Tatman, P. Can This Prosthesis Be Saved?: Implant Salvage Attempts in Infected Primary TKA. Clin Orthop Relat Res 469, 970–976 (2011). https://doi.org/10.1007/s11999-010-1417-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11999-010-1417-2