Opinion statement
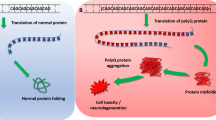
Spinal muscular atrophy is caused by mutations in the survival motor neuron 1 (SMN1) gene, leading to the reduction of SMN protein. The loss of alpha motor neurons in the ventral horn of the spinal cord results in progressive paralysis and premature death. There is no current treatment other than symptomatic and supportive care, although over the past decade, there has been an outstanding advancement in understanding the genetics and molecular mechanisms underlying the physiopathology of SMA. The most promising approach, from current trials, is the use of antisense oligonucleotide (ASOs) to redirect SMN2 translation and increase exon 7 inclusion in the majority of the RNA transcript, to increase the production of fully functional SMN protein. Recently, ISIS Pharmaceuticals Inc. (2855 Gazelle Court, Carlsbad CA 92010) reported an interim analysis from a multiple dose study in children with SMA between 2 and 14 years of age, using ASO therapy. The results indicated good tolerability at all dose levels, increases in muscle function in children treated with multiple doses of ISIS-SMNRx, and increase in SMN protein levels in cerebrospinal fluid (CSF) from both single and multiple dose studies. Studies in infants are ongoing in a few centers; soon other institutions may begin enrollment. Infants are fragile and their disease process may differ from the older SMA population. It is not known whether effective drug would best be given to SMA infants or older children. Other promising therapies are still in preclinical phases or early clinical phases. Gene therapy appears to be efficient in improving survival in a severe mouse model of SMA, though a better definition of the route of administration and of the safety profile of the viral vectors is needed before clinical administration is possible.
Similar content being viewed by others
References and Recommended Reading
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Werdnig G. Zwei frühinfantile hereditäre Fälle von progressive Muskelatrophie unter dem Bilde der Dystrophie, aber auf neurotischer Grundlage [Two early infantile hereditary cases of progressive muscular atrophy simulating dystrophy, but on a neural basis; in German]. Arch Psychiatr Nervenkr. 1891;22:437–80.
Hoffmann J. U” ber chronische spinale Muskelatrophie im Kindesalter, auf familiärer Basis [On chronic spinal muscular atrophy in childhood, with a familial basis; in German]. Dtsch Z Nervenheilkd. 1893;3:427–70.
Byers RK, Banker BQ. Infantile muscular atrophy: en eleven-year experience. Trans Am Neurol Assoc. 1960;85:10–4.
Ogino S, Leonard DG, Rennert H, Ewens WJ, Wilson RB. Genetic risk assessment in carrier testing for spinal muscular atrophy. Am J Med Genet. 2002;110:301–7.
Zaldivar T, Montejo Y, Acevedo AM, Guerra R, Vargas J, Garofalo N, et al. Evidence of reduced frequency of spinal muscular atrophy type I in the Cuban population. Neurology. 2005;65:636–8.
Wang CH, Finkel RS, Bertini ES, Schroth M, Simonds A, Wong B, et al. Consensus Statement for Standard of Care in Spinal Muscular Atrophy. J Child Neurol. 2007;22:1027.
Mercuri E, Bertini E, Iannaccone ST. Childhood spinal muscular atrophy: controversies and challenges. Lancet Neurol. 2012;11:443–52. A brief communication bringing the reader up to date for standard of care for children with SMA. The authors who are well known for their expertise in the care of SMA patients include a discussion of new and emerging therapies in pre-clinical or clnical testing.
Willig TN, Paulus J, Lacau-Saint-Guily J, et al. Swallowing problems in neuromuscular disorders. Arch Phys Med Rehabil. 1994;75:1175–81.
Tilton AH, Miller MD, Khoshoo V. Nutrition and swallowing in pediatric neuromuscular patients. Semin Pediatr Neurol. 1998;5:106–15.
Ito T, Jensen RT. Association of long-term proton pump inhibitor therapy with bone fractures and effects on absorption of calcium, vitamin B12, iron, and magnesium. Curr Gastroenterol Rep. 2010;12:448–57.
Jones M, Campbell KA, Duggan C, et al. Multiple micronutrient deficiencies in a child fed an elemental formula. J Pediatr Gastroenterol Nutr. 2001;33:602–5.
Van den Engel-Hoek L, Erasmus C. Dysphagia in spinal muscular atrophy type II. Neurology. 2009;73:1787–91.
Messina S, Pane M, et al. Feeding problems and malnutrition in spinal muscular atrophy type I. Neuromuscul Disord. 2008;18:389–93.
Chng S, Wong Y, Hui J, et al. Pulmonary function and scoliosis in children with spinal muscular atrophy types II and III. J Paediatr Child Health. 2003;39:673–6.
Zanetta C, Riboldi G, Nizzardo M, Simone C, Faravelli I, Bresolin N, et al. Molecular, genetic and stem cell-mediated therapeutic strategies for spinal muscular atrophy (SMA). J Cell Mol Med. 2014;18:187–96. This is an in depth review of new therapeutic strategies for childhood SMA. The authors are prominent Italian clinician scientists and they provide and excellent summary of the mechanism of action for each of the approaches with many references.
Zanetta C, Nizzardo M, Simone C, Monguzzi E, Bresolin N, Comi GP, et al. Molecular therapeutic strategies for spinal muscular atrophies: current and future clinical trials. Clin Ther. 2014;36:128–40. These authors are the same as for #15, but this article presents an up to date summary of actual clinical trials either recently completed or still in process for SMA. there is description of mechanism of action for the investigational product as well as summary of the protocol for each study.
Yee J-K, Lin R-J. Antisense Oligonucleotides Shed new light on the pathogenesis and treatment of Spinal Muscular Atrophy. Mol Ther. 2012;20:8–10.
Braun S. Gene-based therapies of neuromuscular disorders: an update and the pivotal role of patient organizations in their discovery and implementation. J Gene Med. 2013;15:397–413. This is an interesting review/comment on the role that patient/volunteer disease-specific organizations have played in drug development for neuromuscular disorders. Such organizations have become increasingly important for the field in the past 15 years. Changes in the way clinical research is done for neuromuscular patients have been historic, very much like the influence the AIDS community had on clinical drug development in the 1980s.
Singh P, Liew WKM, Darras BT. Current advances in drug development in spinal muscular atrophy. Curr Opin Pediatr. 2013;25:682–8.
Compliance with Ethics Guidelines
Conflict of Interest
Susan T. Iannaccone declares that she is a principle investigator for ISIS Pharmaceutical studies in SMA patients. Diana Castro declares that she is a co-principle investigator for ISIS Pharmaceutical studies in SMA patients.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Pediatric Neurology
Rights and permissions
About this article
Cite this article
Castro, D., Iannaccone, S.T. Spinal Muscular Atrophy: Therapeutic Strategies. Curr Treat Options Neurol 16, 316 (2014). https://doi.org/10.1007/s11940-014-0316-3
Published:
DOI: https://doi.org/10.1007/s11940-014-0316-3