Abstract
Purpose of Review
To summarize and evaluate evidence available on the effects of yoga on cancer-associated cognitive decline (CACD).
Recent Findings
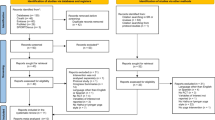
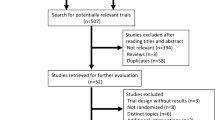
A systematic review was conducted using four databases of articles published before January 1, 2020. Ten articles met the inclusion criteria (six randomized controlled trials, two single-arm studies, one non-randomized controlled trial, and one case series study). Studies were predominantly conducted with breast cancer patients using low-intensity hatha yoga programs. Of the 10 articles, five reported some positive effects on CACD, but significant biases were possible due to design shortcomings. Cohen’s d effect sizes ranged from |0.03| to |0.74|.
Summary
The evidence to date is insufficient to suggest that yoga is beneficial for attenuating CACD. More rigorous trials controlling for non-specific factors are warranted. The field would also benefit from examining self-delivered modes of yoga for treating CACD in various cancer populations to enhance practice sustainability and generalizability.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
National Cancer Institute. Cancer Statistics. 2018; Available at: https://www.cancer.gov/about-cancer/understanding/statistics. Accessed January 14, 2020.
Ono M, Ogilvie JM, Wilson JS, Green HJ, Chambers SK, Ownsworth T, et al. A meta-analysis of cognitive impairment and decline associated with adjuvant chemotherapy in women with breast cancer. Front Oncol. 2015;5:59.
Koppelmans V, Breteler MM, Boogerd W, Seynaeve C, Gundy C, Schagen SB. Neuropsychological performance in survivors of breast cancer more than 20 years after adjuvant chemotherapy. J Clin Oncol. 2012;30(10):1080–6.
Day J, Gillespie DC, Rooney AG, Bulbeck HJ, Zienius K, Boele F, et al. Neurocognitive deficits and neurocognitive rehabilitation in adult brain tumors. Curr Treat Options Neurol. 2016;18(5):22–5.
Padovani L, Andre N, Constine LS, Muracciole X. Neurocognitive function after radiotherapy for paediatric brain tumours. Nat Rev Neurol. 2012;8(10):578–88.
Tsang DS, Edelstein K. Late effects after childhood brain tumor treatment: it’s not just about the radiation. Neuro Oncol. 2019;21(5):565–7.
Ellenberg L, Liu Q, Gioia G, Yasui Y, Packer RJ, Mertens A, et al. Neurocognitive status in long-term survivors of childhood CNS malignancies: a report from the childhood cancer survivor study. Neuropsychology. 2009;23(6):705–17.
Ahles TA, Root JC. Cognitive effects of cancer and cancer treatments. Annu Rev Clin Psychol. 2018;14:425–51.
Ahles TA, Root JC, Ryan EL. Cancer- and cancer treatment-associated cognitive change: an update on the state of the science. J Clin Oncol. 2012;30(30):3675–86.
Janelsins MC, Kesler SR, Ahles TA, Morrow GR. Prevalence, mechanisms, and management of cancer-related cognitive impairment. Int Rev Psychiatry. 2014;26(1):102–13.
Selamat MH, Loh SY, Mackenzie L, Vardy J. Chemobrain experienced by breast cancer survivors: a meta-ethnography study investigating research and care implications. PLoS One. 2014;9(9):e108002.
Von Ah D, Habermann B, Carpenter JS, Schneider BL. Impact of perceived cognitive impairment in breast cancer survivors. Eur J Oncol Nurs. 2013;17(2):236–41.
Denlinger CS, Ligibel JA, Are M, Baker KS, Demark-Wahnefried W, Friedman DL, et al. Survivorship: cognitive function, version 1.2014. J Natl Compr Cancer Netw. 2014;12(7):976–86.
Carlson LE, Zelinski E, Toivonen K, Flynn M, Qureshi M, Piedalue KA, et al. Mind-body therapies in cancer: what is the latest evidence? Curr Oncol Rep. 2017;19(10):67–1.
Bryant E. The yoga sutras of Patanjali: a new edition, translation, and commentary. New York: North Point Press; 2015.
American Cancer Society. Can i safely use an alternative or complementary therapy? 2015; Available at: https://www.cancer.org/treatment/treatments-and-side-effects/complementary-and-alternative-medicine/complementary-and-alternative-methods-and-cancer/using-cam-safely.html. Accessed January 14, 2020.
Canadian Cancer Society. Complementary Therapies. 2019; Available at: http://www.cancer.ca/en/cancer-information/diagnosis-and-treatment/complementary-therapies/yoga/?region=on. Accessed January 14, 2020.
Lyman GH, Bohlke K, Cohen L. Integrative therapies during and after breast cancer treatment: ASCO endorsement of the SIO clinical practice guideline summary. J Oncol Pract. 2018;14(8):495–9.
Ross A, Thomas S. The health benefits of yoga and exercise: a review of comparison studies. J Altern Complement Med. 2010;16(1):3–12.
Hillman CH, Erickson KI, Kramer AF. Be smart, exercise your heart: exercise effects on brain and cognition. Nat Rev Neurosci. 2008;9(1):58–65.
Gothe NP, McAuley E. Yoga and cognition: a meta-analysis of chronic and acute effects. Psychosom Med. 2015;77(7):784–97.
Zimmer P, Baumann FT, Oberste M, Wright P, Garthe A, Schenk A, et al. Effects of exercise interventions and physical activity behavior on cancer related cognitive impairments: a systematic review. Biomed Res Int. 2016;2016:1820954.
Rosazza C, Minati L. Resting-state brain networks: literature review and clinical applications. Neurol Sci. 2011;32(5):773–85.
Chiesa A, Calati R, Serretti A. Does mindfulness training improve cognitive abilities? A systematic review of neuropsychological findings. Clin Psychol Rev. 2011;31(3):449–64.
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J Clin Epidemiol. 2009;62(10):1.
National Institutes of Health. NIH Study Quality Assessment Tools. 2014; Available at: https://www.nhlbi.nih.gov/. Accessed January, 1, 2020.
Derry HM, Jaremka LM, Bennett JM, Peng J, Andridge R, Shapiro C, et al. Yoga and self-reported cognitive problems in breast cancer survivors: a randomized controlled trial. Psychooncology. 2015;24(8):958–66.
•• Janelsins MC, Peppone LJ, Heckler CE, Kesler SR, Sprod LK, Atkins J, et al. YOCAS(c)(R) yoga reduces self-reported memory difficulty in cancer survivors in a nationwide randomized clinical trial: investigating relationships between memory and sleep. Integr Cancer Ther. 2016;15(3):263–71 This study randomized 328 cancer patients to receive a combined hatha and restorative yoga program or standard care with the endpoint of memory impairments. The investigators demonstrated memory improvements in patients who received yoga.
Vadiraja HS, Rao MR, Nagarathna R, Nagendra HR, Rekha M, Vanitha N, et al. Effects of yoga program on quality of life and affect in early breast cancer patients undergoing adjuvant radiotherapy: a randomized controlled trial. Complement Ther Med. 2009;17(5–6):274–80.
Culos-Reed SN, Carlson LE, Daroux LM, Hately-Aldous S. A pilot study of yoga for breast cancer survivors: physical and psychological benefits. Psychooncology. 2006;15(10):891–7.
Lotzke D, Wiedemann F, Rodrigues Recchia D, Ostermann T, Sattler D, Ettl J, et al. Iyengar-yoga compared to exercise as a therapeutic intervention during (neo)adjuvant therapy in women with stage I-III breast cancer: health-related quality of life, mindfulness, spirituality, life satisfaction, and cancer-related fatigue. Evid Based Complement Alternat Med. 2016;2016:5931816.
Pasyar N, Barshan Tashnizi N, Mansouri P, Tahmasebi S. Effect of yoga exercise on the quality of life and upper extremity volume among women with breast cancer related lymphedema: a pilot study. Eur J Oncol Nurs. 2019;42:103–9.
Mackenzie MJ, Carlson LE, Paskevich DM, Ekkekakis P, Wurz AJ, Wytsma K, et al. Associations between attention, affect and cardiac activity in a single yoga session for female cancer survivors: an enactive neurophenomenology-based approach. Conscious Cogn. 2014;27:129–46.
Komatsu H, Yagasaki K, Yamauchi H, Yamauchi T, Takebayashi T. A self-directed home yoga programme for women with breast cancer during chemotherapy: a feasibility study. Int J Nurs Pract. 2016;22(3):258–66.
• Bragard I, Etienne A, Faymonville M, Coucke P, Lifrange E, Schroeder H, et al. A nonrandomized comparison study of self-hypnosis, yoga, and cognitive-behavioral therapy to reduce emotional distress in breast cancer patients. Int J Clin Exp Hypn. 2017;65(2):189–209 This study included assignment to active comparison groups (self-hypnosis versus yoga versus cognitive-behavioral therapy). This comparative approach is of particular importance because it can provide guidance on whether yoga is superior to other potential treatments for cancer-associated cognitive decline with regard to cost and effectiveness.
Galantino ML, Greene L, Daniels L, Dooley B, Muscatello L, O'Donnell L. Longitudinal impact of yoga on chemotherapy-related cognitive impairment and quality of life in women with early stage breast cancer: a case series. Explore (NY). 2012;8(2):127–35.
Hutchinson AD, Hosking JR, Kichenadasse G, Mattiske JK, Wilson C. Objective and subjective cognitive impairment following chemotherapy for cancer: a systematic review. Cancer Treat Rev. 2012;38(7):926–34.
Wefel JS, Vardy J, Ahles T, Schagen SB. International cognition and cancer task force recommendations to harmonise studies of cognitive function in patients with cancer. Lancet Oncol. 2011;12(7):703–8.
Compen F, Bisseling E, Schellekens M, Donders R, Carlson L, van der Lee M, et al. Face-to-face and internet-based mindfulness-based cognitive therapy compared with treatment as usual in reducing psychological distress in patients with Cancer: a multicenter randomized controlled trial. J Clin Oncol. 2018;36(23):2413–21.
Carlson LE. Mindfulness-based interventions for physical conditions: a narrative review evaluating levels of evidence. ISRN Psychiatry. 2012;2012:651583.
Cifu G, Power MC, Shomstein S, Arem H. Mindfulness-based interventions and cognitive function among breast cancer survivors: a systematic review. BMC Cancer. 2018;18(1):1163.
Baydoun M, Barton DL, Peterson M, Wallner LP, Visovatti MA, Arslanian-Engoren C, et al. Yoga for cancer-related fatigue in survivors of hematopoietic cell transplantation: a feasibility study. J Pain Symptom Manag. 2020;59(3):702–708. https://doi.org/10.1016/j.jpainsymman.2019.11.012.
Oh B, Butow PN, Mullan BA, Clarke SJ, Beale PJ, Pavlakis N, et al. Effect of medical qigong on cognitive function, quality of life, and a biomarker of inflammation in cancer patients: a randomized controlled trial. Support Care Cancer. 2012;20(6):1235–42.
Funding
MB, DO, CM, and MF are supported by the Training in Research and Clinical Trials in Integrative Oncology (TRACTION) fellowship from the University of Calgary. DO is supported by a joint Cumming School of Medicine-Charbonneau Cancer Institute Postdoctoral Fellowship. CM and MF are supported by the Alberta Innovates Support for Patient-Oriented Research (SPOR) Graduate Studentships. CM is supported by an award from the Fonds de la recherche en santé du Québec (FRQS). MF is supported by the Queen Elizabeth II Doctoral Scholarship from the province of Alberta. LEC holds the Enbridge Research Chair in Psychosocial Oncology, co-funded by the Canadian Cancer Society Alberta/NWT Division and the Alberta Cancer Foundation, as well as a Canadian Institutes of Health Research Mentorship Chair in Innovative Clinical Trials.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Integrative Care
Rights and permissions
About this article
Cite this article
Baydoun, M., Oberoi, D., Flynn, M. et al. Effects of Yoga-Based Interventions on Cancer-Associated Cognitive Decline: a Systematic Review. Curr Oncol Rep 22, 100 (2020). https://doi.org/10.1007/s11912-020-00960-5
Published:
DOI: https://doi.org/10.1007/s11912-020-00960-5