Abstract
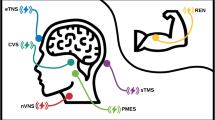
Migraine and other chronic headache disorders are common and if inadequately treated, can lead to significant disability. The effectiveness of medications can be limited by side effects, drug interactions, and comorbid diseases necessitating alternative methods. Technological developments in the past 5 years have made it possible to use non-invasive methods of neuromodulation to treat primary headache disorders. This field includes technologies such as supraorbital transcutaneous stimulation (STS), transcranial magnetic stimulation (TMS), and non-invasive vagal nerve stimulation (nVNS). Existing trials show these modalities are safe and well tolerated and can be combined with standard pharmacotherapy. We review the technologies, biological rationales, and trials involving non-invasive neuromodulation for the treatment of primary headache disorders.
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: •• Of major importance
Lipton R, Stewart W, Diamond S, Diamond M, Reed M. Prevalence and burden of migraine in the United States: data from the American migraine study II. Headache. 2001;41:646–57.
Hepp Z, Dodick D, Varon S, Gillard P, Hansen R, Devine E. Adherence to oral migraine-preventive medications among patients with chronic migraine. Cephalalgia. 2014;35:478–88.
The international classification of headache disorders, 3rd edition (beta version). Cephalagia 2013;33:629-808.
Manack A, Buse D, Lipton R. Chronic migraine: epidemiology and disease burden. Curr Pain Headache Rep. 2011;15:70–8.
Ramadan N. The link between glutamate and migraine. CNS Spectr. 2003;8:446–9.
Ayata C, Jin H, Kudo C, Dalkara T, Moskowitz M. Suppression of cortical spreading depression in migraine prophylaxis. Ann Neurol. 2006;59:652–61.
Schwedt T, Dodick D, Hentz J, Trentman T, Zimmerman R. Occipital nerve stimulation for chronic headache—long-term safety and efficacy. Cephalalgia. 2007;27:153–7.
Saper J, Dodick D, Silberstein S, McCarville S, Sun M, Goadsby P. Occipital nerve stimulation for the treatment of intractable chronic migraine headache: ONSTIM feasibility study. Cephalagia. 2010;31:271–85.
Tsubokawa T, Katayama Y, Yamamoto T, Hirayama T, Koyama S. Chronic motor cortex stimulation in patients with thalamic pain. J Neurosurg. 1993;78:393–401.
Fontaine D, Lazorthes Y, Mertens P, et al. Safety and efficacy of deep brain stimulation in refractory cluster headache: a randomized placebo-controlled double-blind trial followed by a 1-year open extension. J Headache Pain. 2010;11:23–31.
Schoenen J, Clemente LD, vanderheede M, et al. Hypothalamic stimulation in chronic cluster headache: a pilot study of efficacy and mode of action. Brain. 2005;128:940–7.
Coughlin A, Badura A, Fleisher T, Guck T. Multidisciplinary treatment of chronic pain patients: its efficacy in changing patient locus of control. Arch Phys Med Rehabil. 2000;81:739–40.
Lefaucheur J, Andre-Obadia N, Antal A, Ayache S, Baeken C, Benninger D. Evidence-based guidelines on the therapeutic use of repetitive transcranial magnetic stimulation. Clin Neurophys. 2014;125:2150–206.
Narayana S, Papanicolaou A, McGregor A, Boop F, Wheless J. Clinical applications of transcranial magnetic stimulation in pediatric neurology. J Child Neurol. 2014;30:1111–24.
Solomon S, Guglielmo K. Treatment of headache by transcutaneous electrical stimulation. Headache. 1985;25:12–5.
Tayeb Z, Hafeez F, Shafiq Q. Successful treatment of nummular headache with TENS. Cephalalgia. 2008;28:897–8.
Cruccu G, Aziz T, Garcia-Larresa L, et al. EFNS guidelines on neurostimulation therapy for neuropathic pain. Eur J Neurol. 2007;14:952–70.
Sluka K, Judge M, McColley M, Reveiz P, Taylor B. Low frequency TENS is less effective than high frequency TENS at reducing inflammtion-induced hyperalgesia in morphone-tolerant rats. Eur J Pain. 2000;4:185–93.
Piquet M, Balestra C, Sava S, Schoenen J. Supraorbital transcutaneous neurostimulation has sedative effects in healthy subjects. BMC Neurol. 2011;11:135. This study showed the device to be safe for use in healthy volunteers with verum stimulation leading to mild sedative effects.
Craig A. Spinal and trigeminal lamina I input to the locus coeruleus anterogradely labeled with phaseolus vulgaris leucoagglutinin (PHA-L) in the cat and the monkey. Brain Res. 1992;584:325–8.
Schoenen J, Vandersmissen B, Jeangette S, et al. Migraine prevention with a supraorbital transcutaneous stimulator. Neurology. 2013;80:697–704. Double-blind, RTC, sham-controlled study for STS as a migraine preventive. Significantly reduced headache days at three months of use though did not reduce headache severity.
Magis D, Sava S, D'Elia T, Schoenen J. Safety and patients’ satisfaction of transcutaneous supraorbital neuroStimulation (tSNS) with the Cefaly® device in headache treatment: a survey of 2,313 headache sufferers in the general population. J Headache Pain. 2013;14:95.
Anand S, Hotson J. Transcranial magnetic stimulation: neurophysiological applications and safety. Brain and Cogn. 2002;50:366–86.
Rossini P, Rossi S. Transcranial magnetic stimulation: diagnostic, therapeutic and research potential. Neurology. 2007;68:484–8.
Wasserman E. Risk and safety of repetitive transcranial magnetic stimulation: report and suggested guidelines from the International Workshop on the Safety of Repetitive Transcranial magnetic Stimulation, June 5–7, 1996. Electroencephalogr Clin Neurophysiol. 1997;108:1–16.
Dodick D, Schembri C, Helmuth M, Aurora S. Transcranial magnetic stimulation for migraine: a safety review. Headache. 2010;50:1153–63.
Lipton R, Dodick D, Silberstein S, et al. Single-pulse transcranial magnetic stimulation for acute treatment of migraine with aura: a randomised, double-blind, parallel-group, sham-controlled trial. Lancet Neurology. 2010;9:373–80. Double-blind, RTC, sham-controlled study for TMS as abortive migraine treatment. Treatment group more likely to be pain free at 372 h but no differences seen in abortive medication use.
Almaraz A, Dilli E, Dodick D. The effect of prophylactic medications on TMS for migraine aura. Headache Curr. 2010;50:1630–3.
Bhola R, Kinsella E, Giffin N, et al. Single-pulse transcranial magnetic stimulation (sTMS) for the acute treatment of migraine: evaluation of outcome data for the UK post market pilot program. J Headache Pain. 2015;16:51.
Sadler R, Purdy R, Rahey S. Vagal nerve stimulation aborts migraine in patient with intractable epilepsy. Cephalagia. 2002;22:482–4.
Hord E, Evans M, Mueed S, Adamolekun B, Naritoku D. The effect of vagus nerve stimulation on migraines. J Pain. 2003;4:530–4.
Mauskop A. Vagus nerve stimulation relieves chronic refractory migraine and cluster headaches. Cephalagia. 2005;25:82–6.
Cecchini A, Mea E, Tullo V, et al. Vagus nerve stimulation in drug-resistant daily chronic migraine with depression: preliminary data. Neurol Sci 2009;30.
Kirchner A, Birklein F, Stefan H, Handwerker H. Left vagus nerve stimulation suppresses experimentally induced pain. Neurology. 2000;55:1167–71.
Bohotin C, Scholsem M, Multon S, Martin D, Bohotin V, Schoenen J. Vagus nerve stimulation in awake rats reduces formalin-induced nociceptive behaviour and fos-immunoreactivity in trigeminal nucleus caudalis. Pain. 2003;101:3–12.
Oshinsky M, Murphy A, Hekierski H, Cooper M, Simon B. Non-invasive vagus nerve stimulation as treatment for trigeminal allodynia. Pain. 2014;155:1037–42.
Schachter S, Saper C. Progress in epilepsy research: vagus nerve stimulation. Epilepsia. 1998;39:677–86.
Ferrari GD, Crijns H, Borggrefe M, et al. Chronic vagus nerve stimulation: a new and promising therapeutic approach for chronic heart failure. Eur Heart J. 2011;32:857–5.
Sjogren M, Hellstrom P, Jonsson M, Runngerstam M, Silander H, Ben-Menachem E. Cognition-enhancing effect of vagus nerve stimulation in patients with Alzheimer’s disease: a pilot study. J Clin Psych. 2002;63:972–80.
Silberstein S. Non-invasive vagus nerve stimulation in the treatment of migraine headache. Presented at the 4th European Headache and Migraine Trust International Congress; September 20, 2014; Copenhagen, Denmark.
Silberstein S, Silva AD, Calhoun A, Grosberg B, Lipton R, Cady R. Non-invasive vagus nerve stimulation for chronic migraine prevention in a prospective, randomized, sham-controlled pilot study (the EVENT Study): report from the double-blind phase. Presented at the 56th Annual Scientific Meeting of the American Headache Society; June 2014; Los Angeles, California. Double-blind, RTC, sham-controlled study for nVNS as migraine preventive. Reduced number of migraine days with more benefits seen after multiple months of use.
Silberstein S, Silva AD, Calhoun A, Grosberg B, Lipton R, Cady R. Non-invasive vagus nerve stimulation for chronic migraine prevention in a prospective, randomized, sham-controlled pilot Study (the EVENT Study): report from the open-label phase. Presented at the 56th Annual Scientific Meeting of the American Headache Society; June 2014; Los Angeles, California.
Gaul C, Diener H, Solbach K, et al. Non-invasive vagus nerve stimulation using gammaCore® for the prevention and acute treatment of chronic cluster headache: report from the randomised phase of the PREVA study. Presented at the 4th European Headache and Migraine Trust International Congress; September 18–21, 2014; Copenhagen, Denmark. RCT, open-label study for nVNS as abortive and preventive in chronic cluster. Cluster preventive and abortive. Reduced number of headache days after 2 weeks.
Gaul C, Diener H, Solbach K, et al. Non-invasive vagus nerve stimulation using gammaCore for the prevention and acute treatment of chronic cluster headache: report from the open-label phase of the PREVA study. Presented at the 4th European Headache and Migraine Trust International Congress; September 18–21, 2014; Copenhagen, Denmark.
Silberstein S, Mechtler L, Kudrow D, et al. Efficacy and safety outcomes of non-invasive vagus nerve stimulation for the acute treatment (ACT1) of cluster headache study. Presented at the 57th Annual Scientific Meeting of the American Headache Society; Jun 18–21, 2015; Washington DC.
Nesbitt A, Martin J, Tompkins E, Ruttledge M, Goadsby P. Initial use of a novel noninvasive vagus nerve stimulator for cluster headache treatment. Neurology. 2015;84:1249–53.
Grazzi L, Padovan A, Barbanti P. Role of neurostimulation in migraine. Neurol Sci. 2015;36 Suppl 1:S121–3.
Goadsby P, Grosberg B, Mauskop A, Cady R, Simmons K. Effect of noninvasive vagus nerve stimulation on acute migraine: an open label pilot study. Cephalagia. 2014;34:986–93.
Rainero I, Martino PD, Rubino E, Vaula G, Gentile S, Pinessi L. Non-invasive vagal nerve stimulation for the treatment of headache attacks in patients with chronic migraine and medication-overuse headache. Neurology 2014;82:P1.262.
Keskin E, Onur O, Keskin H, Gamus I, Kafali H, Turhan N. Transcutaneous electrical nerve stimulation improves low back pain during pregnancy. Gynecol Obstet Investig. 2012;74:76–83.
Husain M, Stegman D, Trevino K. Pregnancy and delivery while receiving vagus nerve stimulation for the treatment of major depression: a case report. Ann Gen Psych. 2005;4:1–7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Shuhan Zhu declares no potential conflicts of interest.
Michael J. Marmura reports grants from eNeura and Teva.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Headache
Rights and permissions
About this article
Cite this article
Zhu, S., Marmura, M.J. Non-Invasive Neuromodulation for Headache Disorders. Curr Neurol Neurosci Rep 16, 11 (2016). https://doi.org/10.1007/s11910-015-0620-7
Published:
DOI: https://doi.org/10.1007/s11910-015-0620-7