Abstract
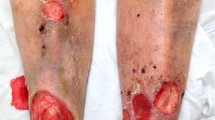
Skin and soft tissue infections (SSTIs) are common illnesses that have a significant impact on health care management. Community-associated, methicillin-resistant Staphylococcus aureus (CA-MRSA) infections have been documented among healthy individuals without predisposing risk factors. The appearance and spread of CA-MRSA represent a new challenge in pediatric medicine and have important clinical implications for therapy of infections caused by S. aureus. This article provides a review of recent changes in the epidemiology of CA-MRSA, pathogenic potential, and therapeutic considerations in the management of SSTIs in children.
Similar content being viewed by others
References and Recommended Reading
Miller LG, Perdreau-Remington F, Rieg G, et al.: Necrotizing fasciitis caused by community-associated methicillinresistant Staphylococcus aureus in Los Angeles. N Engl J Med 2005, 352:1445–1453. A report of 14 cases of CA-MRSA necrotizing fasciitis, an uncommon type of staphylococcal infection.
Saravolatz LD, Markowitz N, Arking L, et al.: Methicillinresistant Staphylococcus aureus. Epidemiologic observations during a community-acquired outbreak. Ann Intern Med 1982, 96:11–16.
Levine DP, Cushing RD, Jui J, Brown WJ: Community-acquired methicillin-resistant Staphylococcus aureus endocarditis in the Detroit Medical Center. Ann Intern Med 1982, 97:330–338.
Herold BC, Immergluck LC, Maranan MC, et al.: Communityacquired methicillin-resistant Staphylococcus aureus in children with no identified predisposing risk. JAMA 1998, 279:593–598.
Fergie JE, Purcell K: Community-acquired methicillinresistant Staphylococcus aureus infections in south Texas children. Pediatr Infect Dis J 2001, 20:860–863.
Gorak EJ, Yamada SM, Brown JD: Community-acquired methicillin-resistant Staphylococcus aureus in hospitalized adults and children without known risk factors. Clin Infect Dis 1999, 29:797–800.
Groom AV, Wolsey DH, Naimi TS, et al.: Community-acquired methicillin-resistant Staphylococcus aureus in a rural American Indian community. JAMA 2001, 286:1201–1205.
Naimi TS, LeDell KH, Boxrud DJ, et al.: Epidemiology and clonality of community-acquired methicillin-resistant Staphylococcus aureus in Minnesota, 1996–1998. Clin Infect Dis 2001, 33:990–996.
Naimi TS, LeDell KH, Como-Sabetti K, et al.: Comparison of community-and health care-associated methicillinresistant Staphylococcus aureus infection. JAMA 2003, 290:2976–2984.
Fey PD, Said-Salim B, Rupp ME, et al.: Comparative molecular analysis of community- or hospital-acquired methicillinresistant Staphylococcus aureus. Antimicrob Agents Chemother 2003, 47:196–203.
Daum RS, Ito T, Hiramatsu K, et al.: A novel methicillinresistance cassette in community-acquired methicillinresistant Staphylococcus aureus isolates of diverse genetic backgrounds. J Infect Dis 2002, 186:1344–1347. The authors show that type IV SCCmec is present in 11 of 12 CA-MRSA isolates with diverse genetic backgrounds as shown by different pulsotypes, ribotypes and coagulase serotypes.
Crawford SE, Daum RS: Epidemic community-associated methicillin-resistant Staphylococcus aureus: modern times for an ancient pathogen. Pediatr Infect Dis 2005, 24:459–460. A recent concise review that describes the molecular characteristic of CA-MRSA isolates.
Ito T, Katayama Y, Asada K, et al.: Structural comparison of the three types of staphylococcal cassette chromosome mec in the chromosome of methicillin-resistant Staphylococcus aureus. Antimicrob Agents Chemother 2001, 45:1323–1336.
Ito T, Ma XX, Takeuchi F, et al.: Novel type V staphylococcal cassette chromosome mec driven by a novel cassette chromosome recombinase, ccrC. Antimicrob Agents Chemother 2004, 48:2637–2651. The authors describe the identification and genetic characterization of the novel type V SCCmec found in CA-MRSA isolate.
Centers for Disease Control and Prevention: Outbreaks of community-associated methicillin-resistant Staphylococcus aureus skin infections. http:/www.cdc.gov/mmwr/preview/ mmwrhtm/mm5205a4. htm.
Purcell K, Fergie J: Epidemic of community-acquired MRSA infections: a 13-year study at Driscoll Children’s Hospital. Paper presented at the Annual Meeting of the Infectious Diseases Society of America [abstract 484]. Boston, MA; September 30-October 3, 2004.
Baba T, Takeuchi F, Kuroda M, et al.: Genome and virulence determinants of high-virulence community-acquired MRSA. Lancet 2002, 359:1819–1827. The complete genome sequence of MW2, a CA-MRSA isolate, which caused fatal septicemia and septic arthritis in a 16-month-old girl without risk factors associated with healthcare was described.
LadhaniS: Recent developments in staphylococcal scalded skin syndrome. Clin Microbiol Infect 2001, 7:301–307.
Dinges MM, Orwin PM, Schlievert PM: Exotoxins of Staphylococcus aureus. Clin Microbiol Rev 2000, 13:16–34.
Lina G, Piemont Y, Godail-Gamot F, et al.: Involvement of Panton-Valentine leukocidin-producing Staphylococcus aureus in primary skin infections and pneumonia. Clin Infect Dis 1999, 29:1128–1132.
Supersac G, Prevost G, Piemont Y: Sequencing of leucocidin R from Staphylococcus aureus P83 suggests that staphylococcal leucocidins and gamma-hemolysin are members of a single, two-component family of toxins. Infect Immun 1993, 61:580–587.
Konig B, Prevost G, Piemont Y, Konig W: Effects of Staphylococcus aureus leukocidins on inflammatory mediator release from human granulocytes. J Infect Dis 1995, 171:607–613.
Prevost G, Couppie P, Prevost P, et al.: Epidemiological data on Staphylococcus aureus strains producing synergohymenotropic toxins. J Med Microbiol 1995, 42:237–245.
Gillet Y, Issartel B, Vanhems P, et al.: Association between Staphylococcus aureus strains carrying gene for Panton-Valentine leukocidin and highly lethal necrotizing pneumonia in young immunocompetent patients. Lancet 2002, 359:753–759.
Vandenesch F, Naimi T, Enright MC, et al.: Communityacquired methicillin-resistant Staphylococcus aureus carrying Panton-Valentine leukocidin genes: worldwide emergence. Emerg Infect Dis 2003, 9:978–984.
Baggett HC, Hennessy TW, Rudolph K, et al.: Community-onset methicillin-resistant Staphylococcus aureus associated with antibiotic use and the cytotoxin Panton-Valentine leukocidin during a furunculosis outbreak in rural Alaska. J Infect Dis 2004, 189:1565–1573. One of a number of recent reports about CA-MRSA skin and soft tissue infections and the association between those isolates and Panton-Valentine leukocidin.
Mongkolrattanothai K, Boyle S, Kahana MD, Daum RS: Severe Staphylococcus aureus infections caused by clonally related community-acquired methicillin-susceptible and methicillinresistant isolates. Clin Infect Dis 2003, 37:1050–1058.
Martinez-Aguilar G, Avalos-Mishann A, Hulten K, et al.: Community-acquired methicillin-resistant and methicillinsusceptible Staphylococcus aureus musculoskeletal infection in children. Pediatr Infect Dis J 2004, 23:701–706.
Lee MC, Rios AM, Aten MF, et al.: Management and outcome of children with skin and soft tissue abscesses caused by community-acquired methicillin-resistant Staphylococcus aureus. Pediatr Infect Dis J 2004, 23:123–127.
Martinez-Aguilar G, Hammerman WA, Mason EO Jr, Kaplan SL: Clindamycin treatment of invasive infections caused by community-acquired, methicillin-resistant and methicillinsusceptible Staphylococcus aureus in children. Pediatr Infect Dis J 2003, 22:593–598.
Kaplan SL, Hulten KG, Gonzalez BE, et al.: Three-year surveillance of community-acquired Staphylococcus aureus infections in children. Clin Infect Dis 2005, 40:1785–1791. A recent study of CA-MRSA infections at Texas Children’s Hospital that showed an alarming increase in the number of infections and hospitalizations caused by CA-MRSA isolates.
LeclercqR: Mechanisms of resistance to macrolides and lincosamides: nature of the resistance elements and their clinical implications. Clin Infect Dis 2002, 34:482–492. This paper provides an extensive and complete review about the mechanism of resistance to macrolides and lincosamides which is important reading to understand the complexicity in the therapy caused by S. aureus.
Siberry GK, Tekle T, Carroll K, Dick J: Failure of clindamycin treatment of methicillin-resistant Staphylococcus aureus expressing inducible clindamycin resistance in vitro. Clin Infect Dis 2003, 37:1257–1260.
Sattler CA, Mason EO Jr, Kaplan SL: Prospective comparison of risk factors and demographic and clinical characteristics of community-acquired, methicillin-resistant versus methicillin-susceptible Staphylococcus aureus infection in children. Pediatr Infect Dis J 2002, 21:910–917.
Clinical Laboratory Standards Institute (CLSI/ NCCLS):Approved Standards. 15th informational supplement. Wayne: CLSI/NCCLS; 2004.
Baker CJ, Frenck RW: Guidelines for management of skin and soft tissue infections. AAP news 2004, 25:110–117.
Iyer S, Jones DH: Community-acquired methicillin-resistant Staphylococcus aureus skin infection: a retrospective analysis of clinical presentation and treatment of a local outbreak. J Am Acad Dermatol 2004, 50:854–858.
Markowitz N, Quinn EL, Saravolatz LD: Trimethoprim-sulfamethoxazole compared with vancomycin for the treatment of Staphylococcus aureus infection. Ann Intern Med 1992, 117:390–398.
Masters PA, O’Bryan TA, Zurlo J, et al.: Trimethoprim-sulfamethoxazole revisited. Arch Intern Med 2003, 163:402–410.
Standiford HC: Tetracycline and chloramphenicol. Principles and Practice of Infectious Diseases. Edited by Mandell GL, Bennett JE, Dolin R. New York: Churchill Livingstone; 2000:336–348.
Ruhe JJ, Monson T, Bradsher RW, Menon A: Use of long-acting tetracyclines for methicillin-resistant Staphylococcus aureus infections: case series and review of the literature. Clin Infect Dis 2005, 40:1429–1434.
Barna JC, Williams DH: The structure and mode of action of glycopeptide antibiotics of the vancomycin group. Annu Rev Microbiol 1984, 38:339–357.
Fridkin SK, Hageman J, McDougal LK, et al.: Epidemiological and microbiological characterization of infections caused by Staphylococcus aureus with reduced susceptibility to vancomycin, United States, 1997–2001. Clin Infect Dis 2003, 36:429–439.
Centers for Disease Control:Staphylococcus aureus resistant to vancomycin—United States 2002. MMWR Morb Mortal Wkly Rep 2002, 51:565–567.
Ford CW, Zurenko GE, Barbachyn MR: The discovery of linezolid, the first oxazolidinone antibacterial agents. Curr Drug Targets Infect Disord 2001, 1:181–199.
Kaplan SL, Deville JG, Yogev R, et al.: Linezolid Pediatric Study Group. Linezolid versus vancomycin for treatment of resistant Gram-positive infections in children. Pediatr Infect Dis J 2003, 22:677–686.
Deville JG, Adler S, Azimi PH, et al.: Linezolid versus vancomycin in the treatment of known or suspected resistant gram-positive infections in neonates. Pediatr Infect Dis J 2003, 22(Suppl 9):S158-S163.
Yogev R, Patterson LE, Kaplan SL, et al.: Linezolid for the treatment of complicated skin and skin structure infections in children. Pediatr Infect Dis J 2003, 22(Suppl 9):S172-S177.
Jungbluth GL, Welshman IR, Hopkins NK: Linezolid pharmacokinetics in pediatric patients: an overview. Pediatr Infect Dis J 2003, 22(Suppl 9):S153-S157.
Wigen CL, Goetz MB: Serotonin syndrome and linezolid. Clin Infect Dis 2002, 34:1651–1652.
Pankey GA, Sabath LD: Clinical relevance of bacteriostatic versus bactericidal mechanism of action in the treatment of gram positive bacterial infection. Clin Infec Dis 2004, 38:864–870.
Ruiz ME, Guerrero IC, Tuazon CU: Endocarditis caused by methicillin-resistant Staphylococcus aureus: treatment failure with linezolid. Clin Infect Dis 2002, 35:1018–1020.
French G: Safety and tolerability of linezolid. J Antimicrob Chemother 2003, 51(Suppl 2):ii45-ii53.
Allington DR, Rivey MP: Quinupristin/dalfopristin: a therapeutic review. Clin Ther 2001, 23:24–44.
Nichols RL, Graham DR, Barriere SL, et al.: Treatment of hospitalized patients with complicated gram-positive skin and skin structure infections: two randomized, multicentre studies of quinupristin/dalfopristin versus cefazolin, oxacillin or vancomycin. Synercid Skin and Skin Structure Infection Group. J Antimicrob Chemother 1999, 44:263–273.
Rubinstein E, Prokocimer P, Talbot GH: Safety and tolerability of quinupristin/dalfopristin: administration guidelines. J Antimicrob Chemother 1999, 44(Suppl A):37–46.
Olsen KM, Rebuck JA, Rupp ME: Arthralgias and myalgias related to quinupritin-dalfopristin administration. Clin Infect Dis 2001, 32:e83–86.
Lakey JH, Ptak M: Fluorescence indicates a calcium-dependent interaction between the lipopeptide antibiotic LY146032 and phopholipid membranes. Biochemistry 1988, 27:4639–4645.
Critchley IA, Blosser-Middleton RS, Jones ME, et al.: In vitro activities of daptomycin against gram-positive pathogens isolated in the United States in 2000–2001. Antimicrob Agents Chemother 2003, 47:1689–1693.
Tally FP, De Bruin MF: Development of daptomycin for grampositive infections. J Antimicrob Chemother 2000, 46:523–526.
Arbeit RD, Maki D, Tally FP, et al.: Daptomycin 98-01 and 99-01 Investigators. The safety and efficacy of daptomycin for the treatment of complicated skin and skin-structure infections. Clin Infect Dis 2004, 38:1673–1681.
Silverman JA, Mortin LI, VanPraagh AD, et al.: Inhibition of Daptomycin by Pulmonary Surfactant: In Vitro Modeling and Clinical Impact. J Infect Dis 2005, 191:2149–2152.
Cubicin (daptomycin for injection) [package insert]. Lexington, MA: Cubist Pharmaceuticals; 2003.
Oleson FB Jr, Berman CL, Kirkpatrick JB, et al.: Once daily dosing in dogs optimizes daptomycin safety. Antimicrob Agents Chemother 2000, 44:2948–2953.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Mongkolrattanothai, K., Daum, R.S. Impact of community-associated, methicillin-resistant Staphylococcus aureus on management of the skin and soft tissue infections in children. Curr Infect Dis Rep 7, 381–389 (2005). https://doi.org/10.1007/s11908-005-0013-1
Issue Date:
DOI: https://doi.org/10.1007/s11908-005-0013-1