Abstract
Purpose of Review
Obstructive sleep apnea syndrome (OSAS) has a high prevalence in western countries. Many papers have been published with the purpose of demonstrating that OSAS acts as an arrhythmia trigger and is responsible for an increase in cardiovascular morbidity and mortality. The aim of this study was to review our knowledge on this topic.
Recent Findings
There is a lot of evidence demonstrating the relationship between OSAS and arrhythmias, but there remains a lack of an interventional randomized trial to demonstrate that by treating OSAS we can reduce arrhythmia burden.
Summary
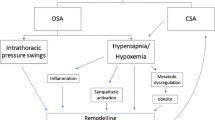
OSAS is a highly prevalent illness in western countries and is clearly related to an increase in cardiovascular mortality and morbidity. Cardiac arrhythmias are triggered by a repetitive hypoxemia, hypercapnia, acidosis, intrathoracic pressure fluctuations, reoxygenation, and arousals during apnea and hypopnea episodes. Early diagnosis and treatment of these patients can reduce further cardiovascular morbidity and mortality.


Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Berry RB, Budhiraja R, Gottlieb DJ, et al. American Academy of Sleep Medicine; Deliberations of the Sleep Apnea Definitions Task Force of the American Academy of Sleep Medicine. Rules for scoring respiratory events in sleep: update of the 2007 AASM Manual for the Scoring of Sleep and Associated Events. J Clin Sleep Med. 2012;8(5):597–619.
Young T, Peppard PE, Gottlieb DJ. Epidemiology of obstructive sleep apnea: a population health perspective. Am J Respir Crit Care Med. 2002;165(9):1217–39.
Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, Hla KM. Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol. 2013;177(9):1006–14.
Ellen RL, Marshall SC, Palayew M, et al. Systematic review of motor vehicle crash risk in persons with sleep apnea. J Clin Sleep Med. 2009;5:573–81.
Marin JM, Agusti A, Villar I, et al. Association between treated and untreated obstructive sleep apnea and the risk of hypertension. JAMA. 2012;307(20):2169–76.
• May AM, Van Wagoner DR, Mehra R. OSA and cardiac arrhythmogenesis. Mechanistic Insights. Contemporary reviews in sleep medicine. Chest. 2017;151(1):225–41. Excellent review of OSA-related electrophysiological mechanisms leading to arrhythmia generation in humans and in animal models.
• Latina JM, Mark Estes NA III, Garlitski A. The Relationship between Obstructive Sleep Apnea and Atrial Fibrillation: A Complex Interplay. Pulmon Med. 2013;(Article ID 621736):11. https://doi.org/10.1155/2013/621736. This paper explores the pathophysiology of OSA which may predispose to AF, clinical implications of stroke risk in this cohort who display overlapping disease processes, and targeted treatment strategies.
Patel N, Donahue C, Shenoy A, et al. Obstructive sleep apnea and arrhythmia: a systemic review. Int J Cardiol. 2017;228:967–70.
Flemons WW, Remmers JE, Gillis AM. Sleep apnea and cardiac arrhythmias: is there a relationship? Am Rev Respir Dis. 1993;148:618–21.
Javaheri S, Parker TJ, Liming JD, Corbett WS, Nishiyama H, Wexler L, et al. Sleep apnea in 81 ambulatory male patients with stable heart failure: types and their prevalences, consequences, and presentations. Circulation. 1997;21:2154–9.
Gami AS, Pressman G, Caples SM, Kanagala R, et al. Association of atrial fibrillation and obstructive sleep apnea. Circulation. 2004;110:364–7.
Gami AS Hodge DO, Herges RM, et al. Obstructive sleep apnea and the risk of incident atrial fibrillation. JACC. 2007;49(5):565–71.
Mehra R, Benjamin EJ, Shahar E, et al. Association of nocturnal arrhythmias with sleep-disordered breathing: The Sleep Heart Health Study. Am J Respir Crit Care Med. 2006;173(8):910–6.
Kanagala R, Murali NS, Friedman PA, et al. Obstructive sleep apnea and the recurrence of atrial fibrillation. Circulation. 2003;107(20):2589–94.
Matiello M, Nadal M, Tamborero D, et al. Low efficacy of atrial fibrillation ablation in severe obstructive sleep Apnoea patients. Europace. 2010;12:1084–9.
Sauer WH, Mckernan ML, Lin D, et al. Clinical predictors and outcomes associated with acute return of pulmonary vein conduction during pulmonary vein isolation for treatment of atrial fibrillation. Heart Rhythm. 2006;3(9):1024–8.
Linz D, McEvoy RD, Cowie MR, et al. Associations of obstructive sleep apnea with atrial fibrillation and continuous positive airway pressure treatment. A review. JAMA Cardiol. 2018;3(6):532–40.
•Fein AS, Shvilkin A, Shah D, et al. Treatment of obstructive sleep apnea reduces the risk of atrial fibrillation recurrence after catheter ablation. JACC. 2013;62(4):300–5. Findings from this study suggest that treating with CPAP can reduce atrial fibrillation recurrences after atrial fibrillation ablation.
Abe H, Takahashi M, Yaegashi H, et al. Efficacy of continuous positive airway pressure on arrhythmias in obstructive sleep apnea patients. Heart Vessels. 2010;25:63–9.
Patel D, Mohanty P, Di Biase L, et al. Safety and efficacy of pulmonary vein antral isolation in patients with obstructive sleep apnea: the impact of continuous positive airway pressure. Circ Arrhythm Electrophysiol. 2010;3:445–51.
Dimitri H, Ng M, Brooks AG, et al. Atrial remodeling in obstructive sleep apnea: implications for atrial fibrillation. Heart Rhythm. 2012;9(3):321–7.
Arzt M, Young T, Finn L, Skatrud JB, Bradley TD. Association of sleep-disordered breathing and the occurrence of stroke. Am J Respir Crit Care Med. 2005;172(11):1447–51.
Lau DH, MacKenzie L, Kelly DJ, et al. Hypertension andatrial fibrillation: evidence of progressive atrial remodeling with electrostructural correlate in a conscious chronically instrumentedovine model. Heart Rhythm. 2010;7(9):1282–90.
Otto ME, Belohlavek M, Romero-Corral A, et al. Comparison of cardiac structural and functional changes in obese otherwise healthy adults with versus without obstructive sleep apnea. Am J Cardiol. 2007;99(9):1298–302.
Haïssaguerre M, Jaïs P, Shah DC, et al. Spontaneous initiation of atrial fibrillation by ectopic beats originating in the pulmonary veins. N Engl J Med. 1998;339(10):659–66.
Simantirakis E, Schiza S, Marketou E, Chrysostomakis S, et al. Severe bradyarrhythmias in patients with sleep apnoea: the effect of continuous positive airway pressure treatment—a long-term evaluation using an insertable loop recorder. Eur Heart J. 2004;25:1070–6.
Martí-Almor J, Felez-Flor M, Balcells E, et al. Prevalence of obstructive sleep apnea syndrome in patients with sick sinus syndrome. Rev Esp Cardiol. 2006;59(1):28–32.
Garrigue S, Pépin JL, Defaye P, Murgatroyd F, Poezevara Y, Clémenty J, et al. High prevalence of sleep apnea syndrome in patients with long-term pacing: the European multicenter polysomnographic study. Circulation. 2007;115(13):1703–9.
Velasco A, Hall C, Perez-Verdia A, Nugent K. Association of high-risk scores for obstructive sleep apnea with symptomatic bradyarrhythmias. J Cardiovasc Med. 2014;15(5):407–10.
Netzer NC, Stoohs RA, Netzer CM, Clark K, Strohl KP. Using the Berlin Questionnaire to identify patients at risk for the sleep apnea syndrome. Ann Intern Med. 1999;131:485–91.
Bazan V, Grau N, Valles E, et al. Obstructive sleep apnea in patients with typical atrial flutter. Prevalence and impact on arrhythmia control outcome. Chest. 2013;143(5):1277–83.
Verrier RL, Josephson ME. Impact of sleep on arrhythmogenesis. Circ Arrhythm Electrophysiol. 2009;2:450–9.
Koshino Y, Satoh M, Katayose Y, et al. Association of sleep-disordered breathing and ventricular arrhytmias in patients without heart failure. Am J Cardiol. 2008;101(6):882–6.
Gami AS, Howard DE, Olson EJ, Somers VK. Day-night pattern of sudden death in obstructive sleep apnea. N Engl J Med. 2005;352(12):1206–79.
Gami A, Olson E, Shen W, RWright RS, Ballman K, Hodge D, et al. Obstructive sleep apnea and the risk of sudden cardiac death: a longitudinal study of 10,701 adults. J Am Coll Cardiol. 2013;62(7):610–6.
Garrigue S, Bordier P, Jaïs P, et al. Benefit of atrial pacing in sleep apnea síndrome. N Engl J Med. 2002;346(6):404–12.
JL JP, Defaye P, Garrigue S, Poezevara Y, Levy P. Overdrive atrial pacing does not improve obstructive sleep apnoea syndrome. Eur Respir J. 2005;25(2)):343–7.
Simantirakis E, Shciza S, Chrysostomakis S, et al. Atrial overdrive pacing for the obstructive sleep apnea–hypopnea syndrome. N Engl J Med. 2005;353:2568–77.
Lamba J, Simpson CS, Redfearn DP, et al. Cardiac Resynchronization therapy for the treatment of sleep apnoea: a meta-analysis. Europace. 2011;13(8):1174–9.
Defaye P, de la Cruz I, Marti-Almor J, et al. A pacemaker transthoracic impedance sensor with an advanced algorithm to identify severe sleep apnea: The DREAM European study. Heart Rhythm. 2014;11(5):842–8.
• Marti-Almor J, Marques P, Jesel L, et al. Incidence of sleep apnea and association with atrial fibrillation in an unselected pacemaker population: results of the observational RESPIRE study. Heart Rhythm. 2020;17(2):195–202. Findings from this study showed the usefulness of sleep apnea monitoring sensor in the pacemaker to detect OSA, and the increase in the incidence of atrial fibrillation in the severe OSA group compared with the non severe OSA group.
Tilkian AG, Guilleminault C, Schroeder JS, et al. Sleep inducedapnea syndrome. Prevalence of cardiac arrhythmiasand their reversal after tracheostomy. Am J Med. 1977;63:348–58.
Guilleminault C, Connolly SJ, Winkle RA. Cardiac arrhythmia and conduction disturbances during sleep in 400 patients with sleep apnea syndrome. Am J Cardiol. 1983;52:490–4.
HF Becker UK, Stammnitz A, Peter JH. Heart block in patients with sleep apnoea. Thorax. 1998;53(suppl 3):S29–32.
Benjamin EJ, Wolf PA, D’Agostino RB, Silbershatz H, Kannel WB, Levy D. Impact of atrial fibrillation on the risk of death: the Framingham Heart Study. Circulation. 1998;98(10):946–52.
Roden DM, Iansmith DH. Effects of low potassium or magnesium concentrations on isolated cardiac tissue. Am J Med. 1987;82(3A):18–23.
Antzelevitch C, Burashnikov A. Overview of basic mechanisms of cardiac arrhythmia. Card Electrophysiol Clin. 2011;3(1):23–45.
Gupta P, Patel C, Patel H, et al. T(p-e)/QT ratio as an index of arrhythmogenesis. J Electrocardiol. 2008;41(6):567–74.
Panikkath R, Reinier K, Uy-Evanado A, et al. Prolonged Tpeak to-tend interval on the resting ECG is associated with increased risk of sudden cardiac death. Circ Arrhythm Electrophysiol. 2011;4(4):441–7.
Yamaguchi M, Shimizu M, Ino H, et al. T wave peak-to-end interval and QT dispersion in acquired long QT syndrome: a new index for arrhythmogenicity. Clin Sci. 2003;105(6):671–6.
Roche F, Barthélémy JC, Garet M, Duverney D, Pichot V, Sforza E. Continuous positive airway pressure treatment improves the QT rate dependence adaptation of obstructive sleep apnea patients. Pacing Clin Electrophysiol. 2005;28(8):819–25.
Gillis AM, Stoohs R, Guilleminault C. Changes in the QT interval during obstructive sleep apnea. Sleep. 1991;14(4):346–50.
Linz D, Schotten U, Neuberger HR, Böhm M, Wirth K. Combined blockade of early and late activated atrial potassium currents suppresses atrial fibrillation in a pig model of obstructive apnea. Heart Rhythm Off J Heart Rhythm Soc. 2011;8(12):1933–9.
Schlatzer C, Schwarz EI, Sievi NA. Intrathoracic pressure swings induced by simulated obstructive sleep apnoea promote arrhythmias in paroxysmal atrial fibrillation. Europace. 2016;18:64–70.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with animal subjects performed by any of the authors. All the studies on humans beings performed by the authors follow the Helsinki criteria and all of them were done after signing informed consent approved by the local ethical committee.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Invasive Electrophysiology and Pacing
Rights and permissions
About this article
Cite this article
Martí-Almor, J., Jiménez-López, J., Casteigt, B. et al. Obstructive Sleep Apnea Syndrome as a Trigger of Cardiac Arrhythmias. Curr Cardiol Rep 23, 20 (2021). https://doi.org/10.1007/s11886-021-01445-y
Accepted:
Published:
DOI: https://doi.org/10.1007/s11886-021-01445-y