Abstract
Purpose of Review
The presence of social support is a major determinant of positive health outcomes among people with cardiovascular disease (CVD); however, little is known about the most effective strategies for enhancing social support among this population. The aim of this scoping review was to describe the effectiveness of interventions seeking to enhance social support among people living with CVD and synthesize the evidence.
Recent Findings
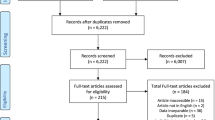
A systematic search for articles that (a) reported on interventions which may enhance social support and (b) included a measure of social support revealed 21 studies. Interventions to enhance social support were diverse and included cognitive behavioural therapy, mindfulness, peer support, and multi-faceted cardiac rehabilitation programmes. Most studies were of fair to good quality according to the PEDro criteria. With the exception of caregiver-oriented interventions, few studies reported significant changes in social support measures.
Summary
Early evidence suggests that caregiver-oriented strategies may offer a promising avenue for enhancing social support; however, more research of higher quality is required to determine the optimal strategies to enhance support among those living with CVD.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Berkman LF. The role of social relations in health promotion. Psychosom Med. 1995;57(3):245–54.
Reifman A. Social relationships, recovery from illness, and survival: a literature review. Ann Behav Med Publ Soc Behav Med. 1995;17(2):124–31.
Cohen, S. Social support measurement and intervention: a guide for health and social scientists [Internet]. Oxford University Press; [cited 2019]. Available from: https://www.oxfordclinicalpsych.com/view/10.1093/med:psych/9780195126709.001.0001/med-9780195126709.
Hogan BE, Linden W, Najarian B. Social support interventions: do they work? Clin Psychol Rev. 2002;22(3):383–442.
Valtorta NK, Kanaan M, Gilbody S, Ronzi S, Hanratty B. Loneliness and social isolation as risk factors for coronary heart disease and stroke: systematic review and meta-analysis of longitudinal observational studies. Heart Br Card Soc. 2016;102(13):1009–16.
Compare A, Zarbo C, Manzoni GM, Castelnuovo G, Baldassari E, Bonardi A, et al. Social support, depression, and heart disease: a ten year literature review. Front Psychol. 2013;4:384.
Uchino BN, Trettevik R, Kent de Grey RG, Cronan S, Hogan J, BRW B. Social support, social integration, and inflammatory cytokines: a meta-analysis. Health Psychol. 2018;37(5):462–71.
Berkman LF, Leo-Summers L, Horwitz RI. Emotional support and survival after myocardial infarction. A prospective, population-based study of the elderly. Ann Intern Med. 1992;117(12):1003–9.
Pfeiffer PN, Heisler M, Piette JD, Rogers MAM, Valenstein M. Efficacy of peer support interventions for depression: a meta-analysis. Gen Hosp Psychiatry. 2011;33(1):29–36.
• Khaledi GH, Mostafavi F, Eslami AA, Rooh Afza H, Mostafavi F, Akbar H. Evaluation of the effect of perceived social support on promoting self-care behaviors of heart failure patients referred to the cardiovascular research center of Isfahan. Iran Red Crescent Med J [Internet]. 2015 [cited 2019 May 31];17(6). Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4552959/. This study, alongside Shahriari et al. (30) demonstrated that a caregiver-only heart failure management education and communication skills program can improve perceived social support among loved-ones with cardiovascular disease.
Dunbar SB, Clark PC, Quinn C, Gary RA, Kaslow NJ. Family influences on heart failure self-care and outcomes. J Cardiovasc Nurs. 2008;23(3):258–65.
Dunbar SB, Clark PC, Deaton C, Smith AL, De AK, O’Brien MC. Family education and support interventions in heart failure: a pilot study. Nurs Res. 2005;54(3):158–66.
Levac D, Colquhoun H, O’Brien KK. Scoping studies: advancing the methodology. Implement Sci. 2010;5(1):69.
Sherrington C, Herbert RD, Maher CG, Moseley AM. PEDro. A database of randomized trials and systematic reviews in physiotherapy. Man Ther. 2000;5(4):223–6.
Foley NC, Bhogal SK, Teasell RW, Bureau Y, Speechley MR. Estimates of quality and reliability with the physiotherapy evidence-based database scale to assess the methodology of randomized controlled trials of pharmacological and nonpharmacological interventions. Phys Ther. 2006;86(6):817–24.
Foley NC, Teasell RW, Bhogal SK, Speechley MR. Stroke rehabilitation evidence-based review: methodology. Top Stroke Rehabil. 2003;10(1):1–7.
Blom M, Georgiades A, Janszky I, Alinaghizadeh H, Lindvall B, Ahnve S. Daily stress and social support among women with CAD: results from a 1-year randomized controlled stress management intervention study. Int J Behav Med. 2009;16(3):227–35.
Davidson P, Digiacomo M, Zecchin R, Clarke M, Paul G, Lamb K, et al. A cardiac rehabilitation program to improve psychosocial outcomes of women with heart disease. J Womens Health. 2002. 2008 Jan 1;17:123–34.
Sakakibara BM, Chakrabarti S, Krahn A, Mackay MH, Sedlak T, Singer J, et al. Delivery of peer support through a self-management mHealth intervention (healing circles) in patients with cardiovascular disease: protocol for a randomized controlled trial. JMIR Res Protoc. 2019;8(1):e12322.
Colella TJ, King-Shier K. The effect of a peer support intervention on early recovery outcomes in men recovering from coronary bypass surgery: a randomized controlled trial. Eur J Cardiovasc Nurs J Work Group Cardiovasc Nurs Eur Soc Cardiol. 2018;17(5):408–17.
•• Berkman LF, Blumenthal J, Burg M, Carney RM, Catellier D, Cowan MJ, et al. Effects of treating depression and low perceived social support on clinical events after myocardial infarction: the Enhancing Recovery in Coronary Heart Disease Patients (ENRICHD) randomized trial. JAMA. 2003;289(23):3106–16 This study, while dated, is the largest and most rigorous assessment of an intervention designed to improve perceived social support among those with cardiovascular disease. The cognitive-behavioural therapy intervention led to significant albeit marginal improvements in perceived social support and yielded no changes in cardiovascular outcomes at long term follow up suggesting alternative modalities must be explored.
• Heo S, McSweeney J, Ounpraseuth S, Shaw-Devine A, Fier A, Moser DK. Testing a holistic meditation intervention to address psychosocial distress in patients with heart failure: a pilot study. J Cardiovasc Nurs. 2018;33(2):126–34 Despite being only a pilot, this study indicates that alternate intervention modalities such as group mindfulness meditation-based programs may offer promising avenues to enhance social support among those with cardiovascular disease.
Boese A, Bock S, Kielblock B, Siegmund-Schultze E, Kröner-Herwig B, Herrmann-Lingen C. Randomised controlled trial of a telephone-based peer support intervention to reduce depressive symptoms and improve social support in women with CHD. J Psychosom Res. 2013;74:539.
Zimet GD, Powell SS, Farley GK, Werkman S, Berkoff KA. Psychometric characteristics of the multidimensional scale of perceived social support. J Pers Assess. 1990;55(3–4):610–7.
Berkman LF, Syme SL. Social networks, host resistance, and mortality: a nine-year follow-up study of Alameda County residents. Am J Epidemiol. 1979;109(2):186–204.
Riegel B, Carlson B. Is individual peer support a promising intervention for persons with heart failure? J Cardiovasc Nurs. 2004;19(3):174–83.
Heisler M, Halasyamani L, Cowen ME, Davis MD, Resnicow K, Strawderman RL, et al. Randomized controlled effectiveness trial of reciprocal peer support in heart failure. Circ Heart Fail. 2013;6(2):246–53.
Sakakibara BM, Ross E, Arthur G, Brown-Ganzert L, Petrin S, Sedlak T, et al. Using mobile-health to connect women with cardiovascular disease and improve self-management. Telemed J E-Health Off J Am Telemed Assoc. 2017;23(3):233–9.
Rywik T, Kurjata P, Broda G, Leszek P, Margaret F-L, Targoński R, et al. Level of social support in heart failure patients—effects of caregivers participation in a simple national disease management programme. Eur J Heart Fail. 2013;12:S19.
Aliabad HO, Vafaeinasab M, Morowatisharifabad MA, Afshani SA, Firoozabadi MG, Forouzannia SK. Maintenance of physical activity and exercise capacity after rehabilitation in coronary heart disease: a randomized controlled trial. Glob J Health Sci. 2014;6(6):198–208.
Safabakhsh L, Jahantigh M, Nosratzehi S, Navabi S. The effect of health promoting programs on patient’s life style after coronary artery bypass graft-hospitalized in Shiraz hospitals. Glob J Health Sci. 2015;8(5):154–9.
Shahriari M, Alimohammadi N, Ahmadi M. Effects of a family centered program on perceived social support in patients with congestive heart failure: an interventional study. J Educ Health Promot. 2016;5:6.
Aldana SG, Greenlaw R, Thomas D, Salberg A, DeMordaunt T, Fellingham GW, et al. The influence of an intense cardiovascular disease risk factor modification program. Prev Cardiol. 2004;7(1):19–25.
Aldana SG, Whitmer WR, Greenlaw R, Avins AL, Thomas D, Salberg A, et al. Effect of intense lifestyle modification and cardiac rehabilitation on psychosocial cardiovascular disease risk factors and quality of life. Behav Modif. 2006;30(4):507–25.
Pischke CR, Scherwitz L, Weidner G, Ornish D. Long-term effects of lifestyle changes on well-being and cardiac variables among coronary heart disease patients. Health Psychol Off J Div Health Psychol Am Psychol Assoc. 2008;27(5):584–92.
Carlson JJ, Norman GJ, Feltz DL, Franklin BA, Johnson JA, Locke SK. Self-efficacy, psychosocial factors, and exercise behavior in traditional versus modified cardiac rehabilitation. J Cardpulm Rehabil. 2001;21(6):363–73.
Younge JO, Wery MF, Gotink RA, Utens EMWJ, Michels M, Rizopoulos D, et al. Web-based mindfulness intervention in heart disease: a randomized controlled trial. PLoS One. 2015;10(12):e0143843.
Gotink RA, Younge JO, Wery MF, Utens EMWJ, Michels M, Rizopoulos D, et al. Online mindfulness as a promising method to improve exercise capacity in heart disease: 12-month follow-up of a randomized controlled trial. PLoS One. 2017;12(5):e0175923.
Bakan G, Akyol AD. Theory-guided interventions for adaptation to heart failure. J Adv Nurs. 2008;61(6):596–608.
Niebauer J, editor. Cardiac rehabilitation manual [Internet]. 2nd ed. Springer International Publishing; 2017 [cited 2019 Jun 8]. Available from: https://www.springer.com/gp/book/9783319477374
Ades PA, Savage PD, Tischler MD, Poehlman ET, Dee J, Niggel J. Determinants of disability in older coronary patients. Am Heart J. 2002;143(1):151–6.
Pinto BM, Goldstein MG, Papandonatos GD, Farrell N, Tilkemeier P, Marcus BH, et al. Maintenance of exercise after phase II cardiac rehabilitation: a randomized controlled trial. Am J Prev Med. 2011;41(3):274–83.
Welstand J, Carson A, Rutherford P. Living with heart failure: an integrative review. Int J Nurs Stud. 2009;46(10):1374–85.
Parry M, Watt-Watson J. Peer support intervention trials for individuals with heart disease: a systematic review. Eur J Cardiovasc Nurs J Work Group Cardiovasc Nurs Eur Soc Cardiol. 2010;9(1):57–67.
Dale JR, Williams SM, Bowyer V. What is the effect of peer support on diabetes outcomes in adults? A systematic review. Diabet Med J Br Diabet Assoc. 2012;29(11):1361–77.
Baig AA, Benitez A, Quinn MT, Burnet DL. Family interventions to improve diabetes outcomes for adults. Ann N Y Acad Sci. 2015;1353(1):89–112.
Dale J, Caramlau I, Sturt J, Friede T, Walker R. Telephone peer-delivered intervention for diabetes motivation and support: the telecare exploratory RCT. Patient Educ Couns. 2009;75(1):91–8.
Heisler M, Vijan S, Makki F, Piette JD. Diabetes control with reciprocal peer support versus nurse care management: a randomized trial. Ann Intern Med. 2010;153(8):507–15.
Hibbard MR, Cantor J, Charatz H, Rosenthal R, Ashman T, Gundersen N, et al. Peer support in the community: initial findings of a mentoring program for individuals with traumatic brain injury and their families. J Head Trauma Rehabil. 2002;17(2):112–31.
Ashbury FD, Cameron C, Mercer SL, Fitch M, Nielsen E. One-on-one peer support and quality of life for breast cancer patients. Patient Educ Couns. 1998;35(2):89–100.
Hofmann SG, Sawyer AT, Witt AA, Oh D. The effect of mindfulness-based therapy on anxiety and depression: a meta-analytic review. J Consult Clin Psychol. 2010;78(2):169–83.
Zeidan F, Johnson SK, Gordon NS, Goolkasian P. Effects of brief and sham mindfulness meditation on mood and cardiovascular variables. J Altern Complement Med N Y N. 2010;16(8):867–73.
Ospina MB, Bond K, Karkhaneh M, Tjosvold L, Vandermeer B, Liang Y, et al. Meditation practices for health: state of the research. Evid ReportTechnology Assess. 2007;155:1–263.
Olivo EL, Dodson-Lavelle B, Wren A, Fang Y, Oz MC. Feasibility and effectiveness of a brief meditation-based stress management intervention for patients diagnosed with or at risk for coronary heart disease: a pilot study. Psychol Health Med. 2009;14(5):513–23.
Barnes S, Brown KW, Krusemark E, Campbell WK, Rogge RD. The role of mindfulness in romantic relationship satisfaction and responses to relationship stress. J Marital Fam Ther. 2007;33(4):482–500.
Wachs K, Cordova JV. Mindful relating: exploring mindfulness and emotion repertoires in intimate relationships. J Marital Fam Ther. 2007;33(4):464–81.
Dekeyser M, Raes F, Leijssen M, Leysen S, Dewulf D. Mindfulness skills and interpersonal behaviour. Personal Individ Differ. 2008;44(5):1235–45.
Schellekens MPJ, Tamagawa R, Labelle LE, Speca M, Stephen J, Drysdale E, et al. Mindfulness-based cancer recovery (MBCR) versus supportive expressive group therapy (SET) for distressed breast cancer survivors: evaluating mindfulness and social support as mediators. J Behav Med. 2017;40(3):414–22.
Kleine A-K, Hallensleben N, Mehnert A, Hönig K, Ernst J. Psychological interventions targeting partners of cancer patients: a systematic review. Crit Rev Oncol Hematol. 2019;140:52–66.
Robinson BC. Validation of a caregiver strain index. J Gerontol. 1983;38(3):344–8.
Pinquart M, Sörensen S. Correlates of physical health of informal caregivers: a meta-analysis. J Gerontol B Psychol Sci Soc Sci. 2007;62(2):126–37.
Aggarwal B, Mosca L. Heart disease risk for female cardiac caregivers. Female Patient. 2009;34(2):42–5.
Aggarwal B, Liao M, Christian A, Mosca L. Influence of caregiving on lifestyle and psychosocial risk factors among family members of patients hospitalized with cardiovascular disease. J Gen Intern Med. 2009;24(1):93–8.
Feeney BC, Collins NL. New look at social support: a theoretical perspective on thriving through relationships. Personal Soc Psychol Rev Off J Soc Personal Soc Psychol Inc. 2015;19(2):113–47.
Uchino BN, Bowen K, Carlisle M, Birmingham W. Psychological pathways linking social support to health outcomes: a visit with the “ghosts” of research past, present, and future. Soc Sci Med. 1982. 2012 Apr;74(7):949–57.
Funding
B.M Sakakibara is supported by a Michael Smith Foundation for Health Research Scholar Award.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
C.T. Clayton, C. Motley, and B.M. Sakakibara declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Psychological Aspects of Cardiovascular Diseases
Appendix
Appendix
Rights and permissions
About this article
Cite this article
Clayton, C., Motley, C. & Sakakibara, B. Enhancing Social Support Among People with Cardiovascular Disease: a Systematic Scoping Review. Curr Cardiol Rep 21, 123 (2019). https://doi.org/10.1007/s11886-019-1216-7
Published:
DOI: https://doi.org/10.1007/s11886-019-1216-7