Abstract
Purpose of Review
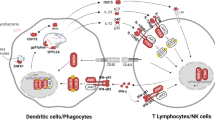
Many genetic conditions predispose affected individuals to opportunistic infections. A number of immunodeficiency diseases, including genetic defects termed Mendelian susceptibility to mycobacterial disease (MSMD), permit infection from many different strains of mycobacteria that would otherwise not cause disease. These include tuberculous and nontuberculous mycobacteria, and bacille Calmette-Guérin vaccine (BCG). Patients may present with infections from other organisms that depend on macrophage function for containment. Defects in multiple genes in the IL-12 and NFKB signaling pathways can cause the MSMD phenotype, some of which include IL12RB1, IL12B, IKBKG, ISG15, IFNGR1, IFNGR2, CYBB, TYK2, IRF8, and STAT1.
Recent Findings
Multiple autosomal recessive and dominant, and 2 X-linked recessive gene defects resulting in the MSMD phenotype have been reported, and others await discovery. This review presents the known gene defects and describes clinical findings that result from the mutations.
Summary
If MSMD is suspected, a careful clinical history and examination and basic immunodeficiency screening tests will narrow the differential diagnosis. A specific diagnosis requires more sophisticated laboratory investigation. Genetic testing permits a definitive diagnosis, permitting genetic counseling. Mild cases respond well to appropriate antibiotic therapy, whereas severe disease may require hematopoietic stem cell transplantation.
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major Importance
Robinson RT, Huppler AR. The Goldilocks model of immune symbiosis with Mycobacteria and Candida colonizers. Cytokine. 2017;97:49–65. https://doi.org/10.1016/j.cyto.2017.05.015.
• Boisson-Dupuis S, Bustamante J, El-Baghdadi J, Camcioglu Y, Parvaneh N, El Azbaoui S, et al. Inherited and acquired immunodeficiencies underlying tuberculosis in childhood. Immunol Rev. 2015;264(1):103–20. https://doi.org/10.1111/imr.12272. This review, not limited to MSMD, focuses on predisposing factors for childhood tuberculosis.
• Louvain de Souza T, de Souza Campos Fernandes RC, Azevedo da Silva J, Gomes Alves Junior V, Gomes Coelho A, Souza Faria AC, et al. Microbial disease spectrum linked to a novel IL-12Rbeta1 N-terminal signal peptide stop-gain homozygous mutation with paradoxical receptor cell-surface expression. Front Microbiol. 2017;8:616. https://doi.org/10.3389/fmicb.2017.00616. This case report describes the clinical presentation of 4 children with MSMD and reviews the features of IL12RB1 inactivation.
•• Bustamante J, Boisson-Dupuis S, Abel L, Casanova JL. Mendelian susceptibility to mycobacterial disease: genetic, immunological, and clinical features of inborn errors of IFN-gamma immunity. Semin Immunol. 2014;26(6):454–70. https://doi.org/10.1016/j.smim.2014.09.008. This is a very detailed review of the causes of MSMD.
• Lee WI, Huang JL, Wu TS, Lee MH, Chen IJ, Yu KH, et al. Patients with inhibitory and neutralizing auto-antibodies to interferon-gamma resemble the sporadic adult-onset phenotype of Mendelian susceptibility to mycobacterial disease (MSMD) lacking Bacille Calmette-Guerin (BCG)-induced diseases. Immunobiology. 2013;218(5):762–71. https://doi.org/10.1016/j.imbio.2012.08.281. Autoantibodies to IFNγ can produce the clinical phenotype of MSMD in adults.
•• Esteve-Sole A, Sologuren I, Martinez-Saavedra MT, Deya-Martinez A, Oleaga-Quintas C, Martinez-Barricarte R, et al. Laboratory evaluation of the IFN-gamma circuit for the molecular diagnosis of Mendelian susceptibility to mycobacterial disease. Crit Rev Clin Lab Sci. 2018;55(3):184–204. https://doi.org/10.1080/10408363.2018.1444580. This article reviews the basic science of the IFNγ circuit in the context of MSMD, and offers detailed advice for laboratory investigation of patients with suspected MSMD.
Online Mendelian Inheritance in Man, OMIM® [database on the Internet]. McKusick-Nathans Institute of Genetic Medicine. Available from: https://omim.org. Accessed: 1/3/18.
• Picard C, Gaspar H, Al-Herz W, Bousfiha A, Casanova J-L, Chatila T, et al. International Union of Immunological Societies: 2017 Primary Immunodeficiency Diseases Committee Report on Inborn Errors of Immunity. J Clin Immunol. 2017;38:96–128. https://doi.org/10.1007/s10875-017-0464-9. This is the most recent official list of primary immunodeficiency diseases recognized by the International Union of Immunological Societies. The list, which is frequently updated, has descriptions of the MSMD conditions.
Ogus AC, Yoldas B, Ozdemir T, Uguz A, Olcen S, Keser I, et al. The arg753-to-gln polymorphism of the human Toll-like receptor 2 gene in tuberculosis disease. Europ Resp J. 2004;23:219–23.
• de Beaucoudrey L, Samarina A, Bustamante J, Cobat A, Boisson-Dupuis S, Feinberg J, et al. Revisiting human IL-12Rbeta1 deficiency: a survey of 141 patients from 30 countries. Medicine. 2010;89(6):381–402. https://doi.org/10.1097/MD.0b013e3181fdd832. This somewhat older article is a very large case series describing clinical features of IL12RB1 deficiency.
Arias AA, Perez-Velez CM, Orrego JC, Moncada-Velez M, Rojas JL, Wilches A, et al. Severe enteropathy and hypogammaglobulinemia complicating refractory mycobacterium tuberculosis complex disseminated disease in a child with IL-12Rbeta1 deficiency. J Clin Immunol. 2017;37(7):732–8. https://doi.org/10.1007/s10875-017-0435-1.
IL-12Rβ1 deficiency: mutation update and description of the IL12RB1 variation database [database on the Internet]. LOVD. 2013. Available from: https://grenada.lumc.nl/LOVD2/mendelian_genes/home.php?select_db=IL12RB1. Accessed: April 2018.
• Prando C, Samarina A, Bustamante J, Boisson-Dupuis S, Cobat A, Picard C, et al. Inherited IL-12p40 deficiency: genetic, immunologic, and clinical features of 49 patients from 30 kindreds. Medicine (Baltimore). 2013;92(2):109–22. https://doi.org/10.1097/MD.0b013e31828a01f9. Although IL12B (p40) deficiency is rare, this case series describes features of 49 patients with that disorder.
Fieschi C, Dupuis S, Picard C, Smith CIE, Holland SM, Casanova J-L. High levels of interferon gamma in the plasma of children with complete interferon gamma receptor deficiency. Pediatrics. 2001;107(4):E48.
Janssen R, Van Wengen A, Verhard E, De Boer T, Zomerdijk T, Ottenhoff TH, et al. Divergent role for TNF-alpha in IFN-gamma-induced killing of Toxoplasma gondii and Salmonella typhimurium contributes to selective susceptibility of patients with partial IFN-gamma receptor 1 deficiency. J Immunol. 2002;169(7):3900–7.
Storgaard M, Varming K, Herlin T, Obel N. Novel mutation in the interferon-gamma-receptor gene and susceptibility to mycobacterial infections. Scand J Immunol. 2006;64(2):137–9. https://doi.org/10.1111/j.1365-3083.2006.01775.x.
Dorman SE, Holland SM. Mutation in the signal-transducing chain of the interferon-gamma receptor and susceptibility to mycobacterial infection. J Clin Invest. 1998;101(11):2364–9. https://doi.org/10.1172/JCI2901.
Vogt G, Bustamante J, Chapgier A, Feinberg J, Boisson Dupuis S, Picard C, et al. Complementation of a pathogenic IFNGR2 misfolding mutation with modifiers of N-glycosylation. J Exp Med. 2008;205(8):1729–37. https://doi.org/10.1084/jem.20071987.
Eletto D, Burns SO, Angulo I, Plagnol V, Gilmour KC, Henriquez F, et al. Biallelic JAK1 mutations in immunodeficient patient with mycobacterial infection. Nat Commun. 2016;7:13992. https://doi.org/10.1038/ncomms13992.
Meraro D, Gleit-Kielmanowicz M, Hauser H, Levi BZ. IFN-stimulated gene 15 is synergistically activated through interactions between the myelocyte/lymphocyte-specific transcription factors, PU.1, IFN regulatory factor-8/IFN consensus sequence binding protein, and IFN regulatory factor-4: characterization of a new subtype of IFN-stimulated response element. J Immunol. 2002;168(12):6224–31. https://doi.org/10.4049/jimmunol.168.12.6224.
Bogunovic D, Byun M, Durfee LA, Abhyankar A, Sanal O, Mansouri D, et al. Mycobacterial disease and impaired IFN-gamma immunity in humans with inherited ISG15 deficiency. Science. 2012;337(6102):1684–8. https://doi.org/10.1126/science.1224026.
Zhang X, Bogunovic D, Payelle-Brogard B, Francois-Newton V, Speer SD, Yuan C, et al. Human intracellular ISG15 prevents interferon-alpha/beta over-amplification and auto-inflammation. Nature. 2015;517:89–93.
Okada S, Markle JG, Deenick EK, Mele F, Averbuch D, Lagos M, et al. Impairment of immunity to Candida and Mycobacterium in humans with bi-allelic RORC mutations. Science. 2015;349(6248):606–13. https://doi.org/10.1126/science.aaa4282.
Vinh DC, Patel SY, Uzel G, Anderson VL, Freeman AF, Olivier KN, et al. Autosomal dominant and sporadic monocytopenia with susceptibility to mycobacteria, fungi, papillomaviruses, and myelodysplasia. Blood. 2010;115(8):1519–29. https://doi.org/10.1182/blood-2009-03-208629.
Calvo KR, Vinh DC, Maric I, Wang W, Noel P, Stetler-Stevenson M, et al. Myelodysplasia in autosomal dominant and sporadic monocytopenia immunodeficiency syndrome: diagnostic features and clinical implications. Haematologica. 2011;96(8):1221–5. https://doi.org/10.3324/haematol.2011.041152.
Hsu AP, Sampaio EP, Khan J, Calvo KR, Lemieux JE, Patel SY, et al. Mutations in GATA2 are associated with the autosomal dominant and sporadic monocytopenia and mycobacterial infection (MonoMAC) syndrome. Blood. 2011;118(10):2653–5. https://doi.org/10.1182/blood-2011-05-356352.
Dickinson RE, Griffin H, Bigley V, Reynard LN, Hussain R, Haniffa M, et al. Exome sequencing identifies GATA-2 mutation as the cause of dendritic cell, monocyte, B and NK lymphoid deficiency. Blood. 2011;118(10):2656–8. https://doi.org/10.1182/blood-2011-06-360313.
Shaw M-A, Clayton D, Atkinson SE, Williams H, Miller N, Sibthorpe D, et al. Linkage of rheumatoid arthritis to the candidate gene NRAMP1 on 2q35. J Med Genet. 1996;33:672–7.
Holtschke T, Lohler J, Kanno Y, Fehr T, Giese N, Rosenbauer F, et al. Immunodeficiency and chronic myelogenous leukemia-like syndrome in mice with a targeted mutation of the ICSBP gene. Cell. 1996;87(2):307–17.
Driggers PH, Elenbaas BA, An JB, Lee IJ, Ozato K. Two upstream elements activate transcription of a major histocompatibility complex class I gene in vitro. Nucleic Acids Res. 1992;20(10):2533–40.
Hambleton S, Salem S, Bustamante J, Bigley V, Boisson-Dupuis S, Azevedo J, et al. IRF8 mutations and human dendritic-cell immunodeficiency. N Engl J Med. 2011;365(2):127–38. https://doi.org/10.1056/NEJMoa1100066.
Ragimbeau J, Dondi E, Alcover A, Eid P, Uze G, Pellegrini S. The tyrosine kinase Tyk2 controls IFNAR1 cell surface expression. EMBO J. 2003;22(3):537–47. https://doi.org/10.1093/emboj/cdg038.
Minegishi Y, Saito M, Morio T, Watanabe K, Agematsu K, Tsuchiya S, et al. Human tyrosine kinase 2 deficiency reveals its requisite roles in multiple cytokine signals involved in innate and acquired immunity. Immunity. 2006;25(5):745–55. https://doi.org/10.1016/j.immuni.2006.09.009.
Jacobs MD, Harrison SC. Structure of an IkappaBalpha/NF-kappaB complex. Cell. 1998;95(6):749–58.
Staples E, Morillo-Gutierrez B, Davies J, Petersheim D, Massaad M, Slatter M, et al. Disseminated Mycobacterium malmoense and Salmonella infections associated with a novel variant in NFKBIA. J Clin Immunol. 2017;37(5):415–8. https://doi.org/10.1007/s10875-017-0390-x.
Lee AJ, Moncada-Vélez M, Picard C, Llanora G, Huang C, Abel L, et al. Severe mycobacterial diseases in a patient with GOF IκBα mutation without EDA. J Clin Immunol. 2016;36:12–5.
Yoshioka T, Nishikomori R, Hara J, Okada K, Hashii Y, Okafuji I, et al. Autosomal dominant anhidrotic ectodermal dysplasia with immunodeficiency caused by a novel NFKBIA mutation, p.Ser36Tyr, presents with mild ectodermal dysplasia and non-infectious systemic inflammation. J Clin Immunol. 2013;33(7):1165–74. https://doi.org/10.1007/s10875-013-9924-z.
Burns SO, Plagnol V, Gutierrez BM, Al Zahrani D, Curtis J, Gaspar M, et al. Immunodeficiency and disseminated mycobacterial infection associated with homozygous nonsense mutation of IKKbeta. J Allergy Clin Immunol. 2014;134(1):215–8. https://doi.org/10.1016/j.jaci.2013.12.1093.
Nielsen C, Jakobsen MA, Larsen MJ, Muller AC, Hansen S, Lillevang ST, et al. Immunodeficiency associated with a nonsense mutation of IKBKB. J Clin Immunol. 2014;34(8):916–21. https://doi.org/10.1007/s10875-014-0097-1.
Zonana J, Elder ME, Schneider LC, Orlow SJ, Moss C, Golabi M, et al. A novel X-linked disorder of immune deficiency and hypohidrotic ectodermal dysplasia is allelic to incontinentia pigmenti and due to mutations in IKK-gamma (NEMO). Am J Hum Genet. 2000;67(6):1555–62. https://doi.org/10.1086/316914.
Filipe-Santos O, Bustamante J, Haverkamp MH, Vinolo E, Ku CL, Puel A, et al. X-linked susceptibility to mycobacteria is caused by mutations in NEMO impairing CD40-dependent IL-12 production. J Exp Med. 2006;203(7):1745–59.
Wang Y, Ma CS, Ling Y, Bousfiha A, Camcioglu Y, Jacquot S, et al. Dual T cell- and B cell-intrinsic deficiency in humans with biallelic RLTPR mutations. J Exp Med. 2016;213(11):2413–35. https://doi.org/10.1084/jem.20160576.
Bustamante J, Arias A, Vogt G, Picard C, Galicia L, Prando C, et al. Germline CYBB mutations that selectively affect macrophages in kindreds with X-linked predisposition to tuberculous mycobacterial disease. Nat Immunol. 2011;12(3):213–21.
• Haverkamp MH, van de Vosse E, van Dissel JT. Nontuberculous mycobacterial infections in children with inborn errors of the immune system. J Inf Secur. 2014;68(Suppl 1):S134–50. https://doi.org/10.1016/j.jinf.2013.09.024. An illustrated review of the basic science of IL-12, IFNγ, and IFNα signaling pathways with a detailed discussion of individual defects causing MSMD.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Drs. Reed and Dolen declare no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Pediatric Allergy and Immunology
Rights and permissions
About this article
Cite this article
Reed, B., Dolen, W.K. The Child with Recurrent Mycobacterial Disease. Curr Allergy Asthma Rep 18, 44 (2018). https://doi.org/10.1007/s11882-018-0797-3
Published:
DOI: https://doi.org/10.1007/s11882-018-0797-3