Abstract
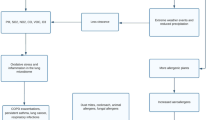
The environment is a major contributor to allergic disease, and great effort is being expended to identify the chemical pollutants and allergens that make a significant impact. Exposure to high levels of ozone, sulfur dioxide, nitrogen dioxide, and diesel exhaust particles is known to reduce lung function. Studies continue to delineate the role of these particles as adjuvants and carriers of allergens into the respiratory system. Current studies also show the exacerbation of allergic disease through fungal spore inhalation and continue to document the role of pollen in allergic rhinitis. Pollen also was recently associated with asthma epidemics, especially after thunderstorms. Forecasting models currently are being developed that predict the trajectories of pollen dispersal and may allow increased avoidance of dangerous outdoor conditions.
Similar content being viewed by others
References and Recommended Reading
Von Mutius E: The environmental predictors of allergic disease. J Allergy Clin Immunol 2000, 105:9–19.This is an outstanding review article that relates environmental pollutants, lifestyle factors, and allergen exposure to the prevalence of allergic disease.
Bjorksten B: The environmental influence on childhood asthma. Allergy 1999, 54:17–23.
Busse WW: Mechanisms and advances in allergic diseases. J Allergy Clin Immunol 2000, 105:S593-S598.
Pearce N, Douwes J, Beasley R: Is allergen exposure the major primary cause of asthma? Thorax 2000, 55:424–431.
Platts-Mills TAE, Rakes G, Heymann PW: The relevance of allergen exposure to the development of asthma in childhood. J Allergy Clin Immunol 2000, 105:S503-S508.
Nelson HS: The importance of allergens in the development of asthma and the persistence of symptoms. J Allergy Clin Immunol 2000, 105:S628-S632.
Nelson HS, Szefler SJ, Jacobs J, et al.: The relationship among environmental allergen sensitization, allergen exposure, pulmonary function, and bronchial hyperresponsivenss in the Childhood Asthma Management Program. J Allergy Clin Immunol 1999, 104:775–785.
Wahn U, Lau S, Bergman R, et al.: Indoor allergen exposure is a risk factor for sensitization during the first three years of life. J Allergy Clin Immunol 1997, 99:763–769.
Woodcock A, Custovic A: Avoiding exposure to indoor allergens. Br Med J 1998, 316:1075–1078.
Weinmann GG, Bowes SM, Gerbase MW, et al.: Response to acute ozone exposure in healthy men: results of a screening procedure. Am J Respir Crit Care Med 1995, 151:33–40.
Horstmann DH, Folinsbee LJ, Ives PJ, et al.: Ozone concentration and pulmonary response relationships for 6.6-hour exposure to 0.12 ppm ozone with moderate exercise. Am Rev Respir Disease 1990, 142:1158–1163.
Aris RM, Christian D, Hearns PQ, et al.: Ozone-induced airway inflammation in human subjects as determined by airway lavage and biopsy. Am Rev Respir Disease 1993, 148:1363–1372.
Kreit JW, Gross KB, Moore TB, et al.: Ozone-induced changes in pulmonary function and bronchial responsiveness in asthmatics. J Appl Physiol 1989, 66:217–222.
Basha MA, Gross KB, Gwizdala CJ, et al.: Bronchoalveolar lavage neutrophilia in asthmatic and healthy volunteers after controlled exposure to ozone and purified air. Chest 1993, 106:1757–1765.
Romieu I, Meneses F, Sienra-Monge JJL, et al.: Effects of urban air pollutants on emergency visits for childhood asthma in Mexico City. Am J Epidemiol 1995, 141:546–553.
White MC, Etzel RA, Wilcox WD, Lloyd C: Exacerbations of childhood asthma and ozone pollution in Atlanta. Environ Res 1994, 65:56–68.
Bates DV, Sitzo R: Relationship between air pollution levels and hospital admissions in southern Ontario. Can J Public Health 1983, 74:117–133.
Kehrl HR, Peden DB, Ball B, et al.: Increased specific airway reactivity of persons with mild allergic asthma after 7.6 hours of exposure to 0.16 ppm ozone. J Allergy Clin Immunol 1999, 104:1198–1204.
Molfino NA, Wright SC, Katz I, et al.: Effect of low concentrations of ozone on inhaled allergen responses in asthmatic subjects. Lancet 1991, 338:199–203.
Kinney PL, Lippmann M: Respiratory effects of seasonal exposures to ozone and particles. Arch Environ Health 2000, 55:210–216.
Koenig JQ: Air pollution and asthma. J Allergy Clin Immunol 1999, 104:717–722.Review article covering the effects of ozone, SO2, NO2, and particulate matter. The author presents a clear description of effects and presents epidemiological results to outline the risk of air pollution to those with allergic disease.
Devalia JL, Bayram H, Rusznak C, et al.: Mechanisms of pollution- induced airway disease: in vitro studies in the upper and lower airways. Allergy 1997, 52:45–51.This article presents a biological overview of the effects that diesel exhaust particles have upon the respiratory system at the cellular level.
Wang J, DeValia JL, Duddle JM, et al.: The effect of exposure for six hours to nitrogen dioxide (NO2) on early phase nasal response to allergen challenge in patients with a history of seasonal allergic rhinitis. J Allergy Clin Immunol 1995, 96:669–676.
Atkinson RW, Anderson HR, Strachan DP, et al.: Short-term associations between outdoor air pollution and visits to accident and emergency departments in London for respiratory complaints. Eur Respir J 1999, 13:257–265.
Yamane K, Chikahisa T, Murayama T, Miyamoto N: Measurement of particulate and unburnt hydrocarbon emissions from diesel engines. Soc. Automotive Engineers, Tech. Paper Series 1988, 880343:1–10.
Takenaka H, Zhang K, Diaz-Sanchez D, et al.: Enhanced human IgE results from exposure to the aromatic hydrocarbons in diesel exhaust: direct effects on B cells IgE production. J Allergy Clin Immunol 1995, 95:103–115.
Diaz-Sanchez D, Zhang K, Nutman TB, Saxon A: Differential regulation of alternative 3’ splicing of human epsilon mRNA variants. J Immunol 1995, 155:1930–1941.
Nel AE, Diaz-Sanchez D, Ng D, et al.: Enhancement of allergic inflammation by the interaction between diesel exhaust particles and the immune system. J Allergy Clin Immunol 1998, 102:539–554.
Diaz-Sanchez D, Tsien A, Fleming J, Saxon A: Combined diesel exhaust particulate and ragweed allergen challenge markedly enhanced in vivo nasal ragweed-specific IgE and skews cytokine production to a TH2-type pattern. J Immunol 1997, 158:2406–2413.
Knox RB, Suphioglu C, Taylor P, et al.: Major grass pollen allergen Lol p 1 binds to diesel exhaust particles: implications for asthma and air pollution. Clin Exp Allergy 1997, 27:246–251.
Ormstad H, Johansen BV, Gaarder PI: Airborne house dust particles and diesel exhaust particles as allergen carriers. Clin Exper Allergy 1998, 28:702–708.
Schwartz J, Slater D, Larson TV, et al.: Particulate air pollution and hospital emergency room visits for asthma in Seattle. Am Rev Respir Disease 1993, 147:826–831.
Targonski PV, Persky VW, Ramekrishnan V: Effect of environmental molds on risk of death from asthma during the pollen season. J Allergy Clin Immunol 1995, 95:955–961.
O’Hollaren MT, Yunginger JW, Offord KP, et al.: Exposure to an aeroallergen as a possible precipitating factor in respiratory arrest in young patients with asthma. N Engl J Med 1991, 324:359–363.
Neukirch C, Henry C, Leynaert B, et al.: Is sensitization to Alternaria alternata a risk factor for severe asthma? A population- based study. J Allergy Clin Immunol 1999, 103:709–711.
Delfino RJ, Coate BD, Zieger RS, et al.: Daily asthma severity in relation to personal ozone exposure and outdoor fungal spores. Am J Respir Crit Care Med 1996, 154:633–641.
Delfino RJ, Zieger RS, Seltzer JM, et al.: The effect of outdoor fungal spore concentrations on daily asthma severity. Environ Health Perspect 1997, 105:622–635.This study correlated self-reported asthma symptoms and peak flow readings with outdoor allergen concentrations and also personal ozone levels. Investigators found that fungal spore levels were associated with all outcomes.
Lehrer SB, Hughes JM, Altman LC, et al.: Prevalence of basidiomycete allergy in the USA and Europe and its relationship to allergic respiratory symptoms. Allergy 1994, 49:460–465.
Horner WE, Hughes JM, Lopez M, Lehrer SB: Basidiomycete skin test reactivity is a risk factor for asthma. Pediatr Asthma Allergy Immunol 2000, 14:69–74.
Epton MJ, Martin IR, Graham P, et al.: Climate and aeroallergen levels in asthma: a 12 month prospective study. Thorax 1997, 52:528–534.
Rosas I, McCartney HA, Payne RW, et al.: Analysis of the relationships between environmental factors (aeroallergens, air pollution, and weather) and asthma emergency admissions to a hospital in Mexico City. Allergy 1998, 53:394–401.
Suphioglu C, Singh MB, Taylor P, et al.: Mechanism of grasspollen- induced asthma. Lancet 1992, 339:569–572.
Venables KM, Allitt U, Collier CG, et al.: Thunderstorm-related asthma—the epidemic of 24/25 June 1994. Clin Exper Allergy 1997, 27:725–736.
Grote M, Vrtala S, Niederberger V, et al.: Expulsion of allergencontaining materials from hydrated rye grass (Lolium perenne) pollen revealed by using immunogold field emission scanning and transmission electron microscopy. J Allergy Clin Immunol 2000, 105:1140–1145.
Schappi GF, Taylor PE, Pain MCF, et al.: Concentrations of major grass group 5 allergens in pollen grains and atmospheric particles: implications for hay fever and allergic asthma sufferers sensitized to grass pollen allergens. Clin Exper Allergy 1999, 29:633–641.This study investigated grass pollen asthma by comparing levels of grass pollen allergens with airborne pollen concentrations. On dry days, the allergen levels were correlated with pollen levels, but following rain, 57% of the allergen was detected in respirable-sized particles not intact pollen grains.
D’Amato G, Noschese P, Russo M, et al.: Pollen asthma in the deep. J Allergy Clin Immunol 1999, 104:710.
O’Rourke MK, Quackenboss JJ, Lebowitz MD: An epidemiological approach investigating respiratory disease response in sensitive individuals to indoor and outdoor pollen exposure in Tucson, Arizona. Aerobiologia 1989, 5:104–110.
Rogers C, Levetin E: Evidence of long-distance transport of mountain cedar pollen into Tulsa, Oklahoma. Int J Biometeorol 1998, 42:65–72.
Levetin E, Van de Water P, Main CE: Aerobiology of Juniperus ashei pollen. J Allergy Clin Immunol 2000, 105:S230.
Monn C, Fuchs A, Hogger D, et al.: Particulate matter less than 10 mm (PM10) and fine particles less than 2.5 mm (PM2.5): relationships between indoor, outdoor and personal concentrations. Sci Total Environ 1997, 208:15–21.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Levetin, E., Van de Water, P. Environmental contributions to allergic disease. Curr Allergy Asthma Rep 1, 506–514 (2001). https://doi.org/10.1007/s11882-001-0059-6
Issue Date:
DOI: https://doi.org/10.1007/s11882-001-0059-6