Abstract
Background
Children who present with idiopathic slipped capital femoral epiphysis (SCFE) have an increased risk of developing bilateral disease. Predicting which patients will develop problems with bilateral hips is important for determining treatment algorithms. This is a retrospective observational study that evaluates the relationship and risk between body mass index (BMI)-for-age and unilateral and bilateral SCFE in patients followed until physeal closure.
Methods
This is a retrospective study of all patients with SCFE presenting to one institution from 1998–2005. Using the Center for Disease Control (CDC) references, BMI-for-age was calculated for each patient. The patients were followed up until complete closure of the bilateral proximal femoral physes, which was considered completion of the study. Statistical analysis for significant differences between groups was performed using the Kruskal–Wallis test for equality of populations. A logistic regression, controlling for age and gender, was used to identify BMI-for-age as a risk factor and to determine the significance of the odds ratios (ORs) for the relevant categorical variables—obese, overweight and healthy weight.
Results
Eighty patients (56 male, 24 female) presented to a single institution between 1998 and 2005 with a diagnosis of SCFE. The mean age of patients was 12.2 years at initial presentation (range 8.5–16). Forty-eight patients (32 male, 16 female) presented with unilateral SCFE, with 22 of the 48 patients having a BMI for-age percentile ≥95 %. Thirty-two patients (24 male, 8 female) presented with bilateral SCFE, with 29 of the 32 patients having a BMI-for-age percentile ≥95 %. Patients with a BMI-for-age ≥95 % had a significantly increased risk of presentation with bilateral slips (OR 4.83; relative risk [RR] 3.01; p < 0.05]. All but one patient in this study with bilateral SCFE or unilateral SCFE with subsequent contralateral involvement had a BMI-for-age ≥85 % (44 out of 45 patients). Additionally, the overall risk of developing bilateral SCFE until physeal closure with a BMI-for-age ≥95 % was significantly increased (OR 3.84; RR 2.02; p < 0.05; number needed to treat [NNT] 3.01).
Conclusions
Previous work has established a relationship between BMI and SCFE. The CDC BMI-for-age growth charts more accurately measure obesity in the pediatric population compared to BMI and are therefore a more appropriate reference tool. This study demonstrates an association between obesity measured by BMI-for-age percentiles and SCFE. This study also demonstrates an association between BMI-for-age and risk for bilateral SCFE at presentation as well as overall incidence of developing bilateral SCFE in the obese pediatric population. By defining the at-risk population through BMI-for-age, physicians can screen the pediatric patient population and provide early strategies for therapeutic weight loss which may reduce the incidence of SCFE.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Slipped capital femoral epiphysis (SCFE) is the most common adolescent hip disorder, with an estimated prevalence of 2.13–10.8 per 100,000 in the United States [1, 2]. While most cases of SCFE are idiopathic, the fundamental etiology can be attributed to a combination of mechanical, endocrine and genetic components. Overwhelming shear stress across the physis ultimately results in biomechanical failure characterized by anterior-cranial-lateral movement of the proximal femoral metaphysis relative to the epiphysis [2–4].
Although SCFE may occur in children of healthy weight, the disorder is commonly associated with obesity [1–5]. Cadaver studies have suggested that increased forces may lead to SCFE in these obese children [6]. It has also been hypothesized that SCFE may be due to a failure of the structural integrity of the physis secondary to a genetic or acquired problem, such as that associated with endocrine disorders [7–12].
The preferred treatment for SCFE is generally surgical stabilization of the affected hip. In addition, at many institutions surgeons may choose to perform prophylactic pinning of the asymptomatic contralateral side [13–15]. As with any surgical procedure, internal fixation of SCFE is not without risk and morbidity including possible avascular necrosis and chondrolysis [16, 17]. As a result, prophylactic pinning was traditionally performed only in high-risk patients such as those with younger bone age at presentation, renal failure, or endocrinopathies [18–22]. As more epidemiologic data become available, a number of studies have suggested that prophylactic pinning may be safer and preferable to observation, citing a high prevalence of long-term osteoarthric sequela with missed SCFE [14, 15, 23–26]. Nevertheless, controversy stills exists regarding the advisability of prophylactic pinning of the contralateral hip.
Body mass index (BMI) has also been suggested as a risk factor for SCFE [5, 27, 28]. It has been consistently demonstrated that patients presenting with SCFE have a higher than average BMI, and that children with bilateral SCFE have a higher BMI than children with unilateral SCFE [1, 2, 6, 29–31]. Patients who present with unilateral SCFE and progress to bilateral disease have also been previously found to have a significantly greater BMI than patients with unilateral SCFE who did not progress [28].
The recently developed BMI-for-age percentile has been shown to more effectively evaluate obesity in the pediatric population [29]. Although BMI is calculated in the same way for children and adults, the criteria used to interpret the meaning of BMI in children is different than adults as the amount of body fat changes with age [30] (Fig. 1). For example, a 10-year-old boy with a BMI of 23 would be considered obese (≥95th percentile) while a 15-year-old boy with a BMI of 23 would be considered healthy (5th–85th percentile) [31]. Methods for evaluating obesity also depend on regional population disparities as demonstrated by differences in BMI calculations between data collection references such as Must, Dallal and Dietz, Cole et al., and Kuczmarski et al. [32–35]. Additionally, studies such as those by Loder and colleagues demonstrate that ethnicity differences must be considered when evaluating certain patient populations [36, 37].
Body mass index-for-age percentiles [31]
The purpose of this study was to examine the relationship between BMI-for-age and unilateral versus bilateral presentation of SCFE as well to clinically follow these patients until radiographic physeal closure to ascertain their risk for future contralateral slip.
Materials and methods
This was a retrospective study of all patients with SCFE presenting to one institution from 1998–2005. All charts and radiographs were available for review. Height and weight at presentation were used to calculate BMI using the formula BMI = weight (kg)/height2 (m2). The Center for Disease Control (CDC) 2000 BMI-for-age growth charts were used to calculate individual BMI-for-age percentiles. According to the CDC growth charts, children with BMI-for-age levels ≥95th percentile are considered obese and those between the 85th and 95th percentiles are considered overweight [29]. Patients were divided into one of three groups—unilateral presentation, bilateral presentation, or unilateral presentation with subsequent contralateral slip. BMI-for-age percentile was calculated for each presentation.
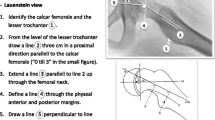
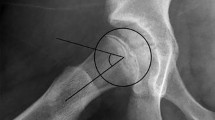
The presence of SCFE was determined radiographically. All radiographs were evaluated by both a board-certified pediatric orthopedic surgeon as well as a board-certified radiologist. In correlation with the physical examination and history, criteria for diagnosis of slips were based on (1) widening and irregularity of the physis, (2) evaluation of Klein’s line or a Trethowan sign, and (3) discrepancy between the head-shaft angle of the hips as seen on anteroposterior and frog-leg lateral views of the pelvis. The patients were followed up until complete closure of the bilateral proximal femoral physes, which was considered completion of the study. Statistical analysis for significant differences between groups was performed using the Kruskal–Wallis test for equality of populations. The level of significance was set at 5 %. A logistic regression, controlling for age and gender, was used to identify BMI-for-age as a risk factor and to determine the significance of the odds ratios (ORs) for the relevant categorical variables—obese, overweight and healthy weight.
Results
Eighty patients (56 male, 24 female) presented to a single institution between 1998 and 2005 with a diagnosis of SCFE. The mean age of patients was 12.2 years at initial presentation (range 8.5–16). The males were significantly older with a mean age of 13.1 years (range 8.5–16) compared to a mean age of 11.7 years (range 9–14) for females (p < 0.01). None of the children showed evidence of endocrinopathy or renal failure. The mean duration of follow-up was 2.2 years.
The mean BMI for all patients included in the study was 29.7 kg/m2 (range 19.0–47.5 kg/m2). Forty-eight patients (32 male, 16 female) presented with unilateral SCFE, with 22 of the 48 patients having a BMI-for-age percentile ≥95 %. Thirty-two patients (24 male, 8 female) presented with bilateral SCFE, with 29 of the 32 patients having a BMI-for-age percentile ≥95 %. Thirteen patients (7 male, 6 female) developed a subsequent contralateral slip, with 10 of the 13 patients having a BMI-for-age percentile ≥95 % (Fig. 2).
Patients with a BMI-for-age ≥95 % represented 63 % of patients with unilateral SCFE (22/35), 91 % of patients with bilateral SCFE (29/32), and 77 % of patients who developed a contralateral slip (10/13). Patients with a BMI-for-age between 85 and 95 % represented 23 % of patients with unilateral SCFE (8/35), 9 % of patients with bilateral SCFE (3/32), and 15 % of patients who developed a contralateral slip (2/13) (Table 1).
Sixty-three percent of patients with a BMI-for-age ≥95 % presented with a bilateral SCFE or presented with unilateral SCFE and developed a subsequent contralateral SCFE. All but one patient in this study with bilateral SCFE or unilateral SCFE with subsequent contralateral involvement had a BMI-for-age ≥85 % (44 out of 45 patients).
Patients with a BMI-for-age ≥95 % had a significantly increased risk of presentation with bilateral slips (OR 4.83; RR 3.01; p < 0.05]. There was no significant difference in the development of future contralateral slip (OR 1.97; RR 1.67; p = 0.38) when isolating patients who presented with unilateral SCFE and went on to develop bilateral pathology. The overall risk of developing bilateral SCFE until physeal closure with a BMI-for-age ≥95 %, however, was significantly increased (OR 3.84; RR 2.02; p < 0.05). The number to be treated (NNT) was 3.01, suggesting that pinning all hips in patients with a BMI-for-age >95 % would mean pinning three hips in order to prevent one hip from progression to bilateral slips. Patients with a BMI-for-age between 85 and 95 % did not have a significantly increased risk of presentation with bilateral slips (OR 4.33; RR 3.50; p = 0.36) or development of future contralateral slip (OR 1.25; RR 1.20; NNT 30; p = 0.87) compared to individuals with a BMI-for-age < 85 %.
Discussion and conclusion
Although the exact etiology of SCFE remains unproven, many previous investigators have suggested an association with obesity and possible increased shear stress across the physis leading to an increased incidence of SCFE in this population [6, 7, 10]. The results of this study support this hypothesis as the majority of patients in this study were classified as overweight or obese. Previous work has established a relationship between BMI and SCFE [1, 27, 28, 38]. This study uses the CDC BMI-for-age growth charts to more accurately measure obesity in the pediatric population compared to BMI. However, the CDC reference is just one way of calculating BMI-for-age; although it covers a large sampling of representative populations, it is not all-inclusive. The CDC references for the United States were based on data collected from European Americans, African Americans and Mexican Americans sampled between 1988 and 1994 in the NHANES III study. When compared to other models it demonstartes an increased proportion of the population in the overweight and obesity categories [35, 39].
This study demonstrates an association between obesity as measured by BMI-for-age percentiles and SCFE. This study also elucidates an association between BMI-for-age and risk for bilateral SCFE both at initial presentation and throughout the remaining growth period. While there was no significant association between BMI-for-age and subsequent contralateral slip after initial presentation, our study was likely underpowered to prove this given the smaller sub-group size. If the assumption was made that all patients with bilateral SCFE at initial presentation at some point in their clinical history had unilateral SCFE and then developed bilateral pathology, the adjusted calculations would then indicate a statistically signficant correlation between BMI and SCFE.
In addition to larger long-term prospective studies, further work is needed to establish the effect of weight reduction on the incidence of future contralateral slips in this population. As suggested by Loder et al., physiologic or bone age is less variable than the chronologic age when discussing risk for SCFE and this may be one of the limitations of our study [40]. Furthermore, as this is an observational study continuous variables, such as age at onset and relation to peak height velocity, are possible cofounding factors during OR analysis.
The prevalence of bilateral involvement in this study is also consistent with previously published reports of an 18–63 % prevalence of bilateral disease, with 40 % (32/80) of patients presenting with bilateral SCFE in this study [23, 37, 41]. This study also demonstrates that patients with bilateral SCFE had a significantly higher BMI-for-age than children with unilateral SCFE. Patients who presented with unilateral SCFE who progressed to bilateral disease also had a significantly higher BMI-for-age than patients with unilateral disease who did not progress.
Patients with a BMI-for-age ≥95 % are at a significantly increased risk of developing SCFE. If clinically correlated, obese patients warrant a high index of suspicion for bilateral disease given their increased presentation with bilateral SCFE and propensity for future development of a contralateral slip. This study suggests that strong consideration should be given to prophylactic stabilization of the contralateral hip in patients with SCFE presenting with a BMI-for-age ≥95 %. In addition, by defining the at-risk population through BMI-for-age, physicians can screen the pediatric patient population and provide early strategies for therapeutic weight loss which may reduce the incidence of SCFE.
References
Manoff EM, Banffy MB, Winell JJ (2005) Relationship between body mass index and slipped capital femoral epiphysis. J Pediatr Orthop 25:744–746
Kelsey JL, Acheson RM, Keggi KJ (1972) The body build of patients with slipped capital femoral epiphysis. Am J Dis Child 124:276–281
Fidler MW, Brook CDK (1974) Slipped capital femoral epiphysis following treatment with human growth hormone. J Bone Jt Surg Am 56:1719–1722
Burrows HJ (1957) Slipped upper femoral epiphysis. J Bone Jt Surg Br 39:641–658
Murray AW, Wilson NI (2008) Changing incidence of slipped capital femoral epiphysis: a relationship with obesity? J Bone Jt Surg Br 90:92–94
Chung SMK, Batterman SC, Brighton CT (1976) Shear strength of the human femoral capital epiphyseal plate. J Bone Jt Surg Am 58:94–103
Prichett JW, Perdue KD (1988) Mechanical factors in slipped capital femoral epiphysis. J Pediatr Orthop 8:385–388
Brenkel IJ, Dias JJ, Davies TG et al (1989) Hormone status in patients with slipped capital femoral epiphysis. J Bone Jt Surg Br 71:33–38
Loder RT, Aronson DD, Jacobs MB et al (2000) Slipped capital femoral epiphysis. J Bone Jt Surg Am 82:1170–1188
Weiner D (1996) Pathogenesis of slipped capital femoral epiphysis: current concepts. J Pediatr Orthop B 5:67–73
Floman Y, Yosipovitch Z, Licht A et al (1975) Bilateral slipped upper femoral epiphysis: a rare manifestation of renal osteodystrophy. Isr J Med Sci 11:15–20
Moorefield WG Jr, Urbaniak JR, Ogden WS et al (1976) Acquired hypothyroidism and slipped capital femoral epiphysis. Report of three cases. J Bone Jt Surg Am 58:705–708
Emery RJ, Todd RC, Dunn DM (1990) Prophylactic pinning in slipped upper femoral epiphysis. Prevention of complications. J Bone Jt Surg Br 72:217–219
Hagglund G (1996) The contralateral hip in slipped capital femoral epiphysis. J Pediatr Orthop B 5:158–161
Hagglund G, Hansson LI, Ordeberg G et al (1988) Bilaterality in slipped upper femoral epiphysis. J Bone Jt Surg Br 70:179–181
Maurer RC, Larsen IJ (1970) Acute necrosis of cartilage in slipped capital femoral epiphysis. J Bone Jt Surg Am 52:39–50
Vrettos BC, Hoffman EB (1993) Chondrolysis in slipped upper femoral epiphysis. Long term study of the etiology and natural history. J Bone Jt Surg Br 75:956–961
Busch MT, Morrissy RT (1987) Slipped capital femoral epiphysis. Orthop Clin N Am 18:637–647
Castro FP, Bennett JT, Doulens K (2000) Epidemiological perspective on prophylactic pinning in patients with unilateral slipped capital femoral epiphysis. J Pediatr Orthop 20:745–758
Crawford AH, Steel HH (1990) Operative versus nonoperative treatment of slipped capital femoral epiphysis. Orthopedics 13:99–111
Loder RT, Aronson DD, Greenfield ML (1993) The epidemiology of bilateral slipped capital femoral epiphysis. A study of children in Michigan. J Bone Jt Surg Am 75:1141–1147
Wilson PD, Jacobs B, Schecter L (1965) Slipped capital femoral epiphysis. An end-result study. J Bone Jt Surg Am 47:1128–1145
Hagglund G, Hannson LI, Ordeberg G (1984) Epidemiology of slipped capital femoral epiphysis in southern Sweden. Clin Orthop 191:82–94
Baghdadi YMK, Larson AN, Sierra RJ, Peterson HA, Stans AA (2013) The fate of hips that are not prophylactically pinned after unilateral slipped capital femoral epiphysis. Clin Orthop Relat Res 471(7):2124–2131
Yildirim Y, Bautista S, Davidson RS (2008) Chondrolysis, osteonecrosis, and slip severity in patients with subsequent contralateral slipped capital femoral epiphysis. J Bone Jt Surg Am 90(A):485–492
Schultz WR, Weinstein JN, Weinstein SL, Smith BG (2002) Prophylactic pinning of the contralateral hip in slipped capital femoral epiphysis: evaluation of long-term outcome for the contralateral hip with use of decision analysis. J Bone Jt Surg Am 84(A):1305–1314
Poussa M, Schlenzka D, Yrjonen T (2003) Body mass index and slipped capital femoral epiphysis. J Pediatr Orthop B 12:369–371
Bhatia NN, Pirpiris M, Otsuka NY (2006) Body mass index in patients with slipped capital femoral epiphysis. J Pediatr Orthop 26:197–199
Ogden CL, Carroll MD, Flegal KM (2008) High body mass index for age among US children and adolescents, 2003–2006. J Am Med Assoc 299:2401–2405
Freedman DS, Wang J, Thornton JC et al (2009) Classification of body fatness by body mass index–for-age categories among children. Arch Pediatr Adolesc Med 16:805–811
Division of Nutrition, Physical Activity and Obesity, National Center for Chronic Disease Prevention and Health Promotion (2014) About BMI for children and teens. Centers for Disease Control and Prevention. http://www.cdc.gov/healthyweight/assessing/bmi/childrens_bmi/about_childrens_bmi.html#interpreted%20the%20same%20way. Accessed 30 April 2015
Must A, Dallal GE, Dietz WH (1991) Reference data for obesity: 85th and 95th percentiles of body mass index and triceps skinfold thickness. Am J Clin Nutr 53:839–846
Cole TJ, Bellizzi MC, Flegal KM, Dietz WH (2000) Establishing a standard definition for child overweight and obesity worldwide: international survey. Br Med J 320:1240–1243
Kuczmarski RJ (2002) 2000 CDC growth charts for the United States: methods and development. Vital Health Stat 246:17–27
Jackson RT, Rashed M, Al-Hamad N, Hwalla N, Al-Somaie M (2007) Comparison of BMI-for-age in adolescent girls in 3 countries of the Eastern Mediterranean Region. East Mediterr Health J 13(2): 430–440
Loder RT (1996) The demographics of slipped capital femoral epiphysis. An international multicenter study. Clin Orthop Relat Res 322:8–27
Loder RT, Aronson DD, Bollinger RO (1990) Seasonal variation in slipped capital femoral epiphysis. J Bone Jt Surg Am 72:378–381
Wisemandle WMA, Maynard LM, Guo SS et al (2000) Childhood weight, stature, and body mass index never overweight, early onset overweight, and late-onset overweight groups. Pediatrics 106:E14
National Center for Health Statistics (NCHS), Centers of Disease Control and Prevention, US Department of Health and Human Services (1996) Third National Health and Nutrition Examination Survey, 1988–1994, NHANES III Analytic and reporting guidelines. Cent Dis Control Prev, Hyattsville
Loder RT, Skopelja EN (2011) The epidemiology and demographics of slipped capital femoral epiphysis. Orthopedics 2011:1–19
Jerre R, Billing L, Hansson G et al (1996) Bilaterality in slipped capital femoral epiphysis: importance of a reliable radiographic method. J Pediatr Orthop B 5:80–84
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Michael W. Aversano, Payam Moazzaz, Anthony A. Scaduto and Norman Y. Otsuka declare that they have no conflict of interest.
Funding
No grants or funding sources were utilized.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
For this type of study formal consent is not required.
Rights and permissions
This article is published under an open access license. Please check the 'Copyright Information' section either on this page or in the PDF for details of this license and what re-use is permitted. If your intended use exceeds what is permitted by the license or if you are unable to locate the licence and re-use information, please contact the Rights and Permissions team.
About this article
Cite this article
Aversano, M.W., Moazzaz, P., Scaduto, A.A. et al. Association between body mass index-for-age and slipped capital femoral epiphysis: the long-term risk for subsequent slip in patients followed until physeal closure. J Child Orthop 10, 209–213 (2016). https://doi.org/10.1007/s11832-016-0731-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11832-016-0731-y