Abstract
Objectives
Silicone airway stents are used to manage central airway stenosis or obstruction, although their impact on long-term survival remains unknown in patients with central airway stenosis or obstruction due to thoracic malignancy. In this study, we retrospectively analyzed the impact of silicone stents on survival.
Methods
We retrospectively analyzed clinical data of 106 patients with central airway stenosis or obstruction due to thoracic malignancy treated by stenting at Toho University Omori Medical Center between 1998 and 2018.
Results
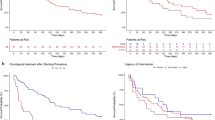
Patients treated with silicone stents had significantly higher survival rates than patients treated with metallic stents (p = 0.0173). Silicone stents patients also had significantly more additional treatments for thoracic malignancy after stenting than metallic stents patients (p = 0.0007). Notably, significantly more silicone stents patients underwent chemoradiotherapy or radiotherapy (p = 0.0268, p = 0.0300). During multivariate analyses, the additional treatment, including chemoradiotherapy or radiotherapy, was an independent optimal prognostic factor.
Conclusions
Silicone stents patients had significantly higher survival rates than metallic stents patients. Although stenting for airway stenosis or obstruction due to thoracic malignancy may be mainly palliative, additional treatments after stenting should be considered to improve the prognoses of patients with airway stenosis or obstruction due to thoracic malignancy.

Similar content being viewed by others
References
Iyoda A, Azuma Y, Sano A, Sakai T, Koezuka S, Otsuka H, et al. Long-term outcomes in patients with benign central airway stenosis or obstruction after stenting. World Acad Sci J. 2020;2:20.
Oviatt PL, Stather DR, Michaud G, Maceachern P, Tremblay A. Exercise capacity, lung function, and quality of life after interventional bronchoscopy. J Thorac Oncol. 2011;6:38–42.
Ferrell B, Koczywas M, Grannis F, Harrington A. Palliative care in lung cancer. Surg Clin North Am. 2011;91:403–17.
Folch E, Keyes C. Airway stents Ann Cardiothorac Surg. 2018;7:273–83.
Ost DE, Shah AM, Lei X, Godoy MCB, Jimenez CA, Eapen GA, et al. Respiratory infections increase the risk of granulation tissue formation following airway stenting in patients with malignant airway obstruction. Chest. 2012;141:1473–81.
Oki M, Saka H. Temporary use of silicone stents for severe airway stenosis in untreated malignant lymphoma. J Bronchology Interv Pulmonol. 2013;20:21–7.
Kim JH, Shin JH, Song HY, Ohm JY, Lee JM, Lee DH, et al. Palliative treatment of inoperable malignant tracheobronchial obstruction: temporary stenting combined with radiation therapy and/or chemotherapy. AJR Am J Roentgenol. 2009;193:W38-42.
Miyazawa T, Miyazu Y, Iwamoto Y, Ishida A, Kanoh K, Sumiyoshi H, et al. Stenting at the flow-limiting segment in tracheobronchial stenosis due to lung cancer. Am J Respir Crit Care Med. 2004;169:1096–102.
Saad CP, Murthy S, Krizmanich G, Mehta AC. Self-expandable metallic airway stents and flexible bronchoscopy: long-term outcomes analysis. Chest. 2003;124:1993–9.
Furukawa K, Ishida J, Yamaguchi G, Usuda J, Tsutsui H, Saito M, et al. The role of airway stent placement in the management of tracheobronchial stenosis caused by inoperable advanced lung cancer. Surg Today. 2010;40:315–20.
Husain SA, Finch D, Ahmed M, Morgan A, Hetzel MR. Long-term follow-up of ultraflex metallic stents in benign and malignant central airway obstruction. Ann Thorac Surg. 2007;83:1251–6.
Oki M, Saka H. Airway stenting for patients with airway stenosis because of small cell lung cancer. Clin Respir J. 2018;12:2257–63.
Saji H, Furukawa K, Tsutsui H, Tsuboi M, Ichinose S, Usuda J, et al. Outcomes of airway stenting for advanced lung cancer with central airway obstruction. Interact Cardiovasc Thorac Surg. 2010;11:425–8.
Bolliger CT, Probst R, Tschopp K, Solèr M, Perruchoud AP. Silicone stents in the management of inoperable tracheobronchial stenosis. Indications and limitations. Chest. 1993;104:1653–9.
Lemaire A, Burfeind WR, Toloza E, Balderson S, Petersen RP, Harpole DH Jr, et al. Outcomes of tracheobronchial stents in patients with malignant airway disease. Ann Thorac Surg. 2005;80:434–7.
Iyoda A, Azuma Y, Sano A, Sakai T, Koezuka S, Otsuka H, , et al. Contributions of Airway Stent for Long-term Outcome in Patients With Malignant Central Airway Stenosis or Obstruction. J Bronchology Interv Pulmonol. 2021; https://doi.org/https://doi.org/10.1097/LBR.0000000000000749..
Tsuji Y, Yoshimura H, Uto F, Tamada T, Iwata K, Tamamoto T, et al. Physical and histopathological assessment of the effects of metallic stents on radiation therapy. J Radiat Res. 2007;48:477–83.
Nishimura Y, Nagata K, Katano S, Hirota S, Nakamura K, Higuchi F, et al. Severe complications in advanced esophageal cancer treated with radiotherapy after intubation of esophageal stents: a questionnaire survey of the Japanese Society for Esophageal Diseases. Int J Radiat Oncol Biol Phys. 2003;56:1327–32.
Acknowledgments
Not applicable
Funding
This research did not receive any grants from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
YA, AS, TS, SK, HO, KI, SS, KT, and AI have been involved in the conception and design of the study. AI wrote the manuscript. YA, AS, TS, SK, and HO collected data. KI, SS, and KT supervised this study. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
We have no conflicts of interest in this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Iyoda, A., Azuma, Y., Sano, A. et al. Long-term survival of airway silicone stents in patients with central airway stenosis or obstruction due to thoracic malignancy. Gen Thorac Cardiovasc Surg 69, 1303–1307 (2021). https://doi.org/10.1007/s11748-021-01634-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11748-021-01634-0