Abstract
Objective
Ex vivo lung perfusion (EVLP) has been used not only for graft evaluation but also for graft reconditioning prior to lung transplantation. Inflammatory cells such as neutrophils may cause additional graft injury during EVLP. Neutrophil elastase inhibitors protect lungs against neutrophil-induced lung injury, such as acute respiratory distress syndrome. This study aimed to investigate the effect of a neutrophil elastase inhibitor during EVLP.
Methods
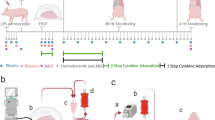
EVLP was performed for 4 h in bilateral pig lungs that had previously experienced warm ischemia for 2 h with or without a neutrophil elastase inhibitor (treated and control groups, respectively; n = 6). Following EVLP, the left lung was transplanted into a recipient pig, and this was followed by observation for 4 h. Pulmonary functions were observed both during EVLP and during the early post-transplant stage.
Results
During EVLP, decreases in neutrophil elastase levels (P < 0.001), the wet–dry weight ratio (P < 0.05), and pulmonary vascular resistance (P < 0.01) and increases in the PaO2/FiO2 ratio (P < 0.01) and pulmonary compliance (P < 0.05) were observed in the treated group. After transplantation, decreased pulmonary vascular resistance (P < 0.05) was observed in the treated group.
Conclusions
A neutrophil elastase inhibitor attenuated the inflammatory response during EVLP and may decrease the incidence of lung reperfusion injury after transplantation.




Similar content being viewed by others
References
Oto T, Okada Y, Bando T, Minami M, Shiraishi T, Nagayasu T, et al. Registry of the Japanese Society of Lung and Heart-Lung Transplantation: the official Japanese lung transplantation report 2012. Gen Thorac Cardiovasc Surg. 2013;61:208–11.
Kakishita T, Oto T, Hori S, Miyoshi K, Otani S, Yamamoto S, et al. Suppression of inflammatory cytokines during ex vivo lung perfusion with an adsorbent membrane. Ann Thorac Surg. 2010;89:1773–9.
Otani S, Oto T, Kakishita T, Miyoshi K, Hori S, Yamane M, et al. Early effects of the ex vivo evaluation system on graft function after swine lung transplantation. Eur J Cardiothorac Surg. 2011;40:956–61.
Sadaria MR, Smith PD, Fullerton DA, Justison GA, Lee JH, Puskas F, et al. Cytokine expression profile in human lungs undergoing normothermic ex vivo lung perfusion. Ann Thorac Surg. 2011;92:478–84.
Barletta KE, Cagnina RE, Wallace KL, Ramos SI, Mehrad B, Linden J. Leukocyte compartments in the mouse lung: distinguishing between marginated, interstitial, and alveolar cells in response to injury. J Immunol Methods. 2012;375:100–10.
Zeiher BG, Matsuoka S, Kawabata K, Repine JE. Neutrophil elastase and acute lung injury: prospects for sivelestat and other neutrophil elastase inhibitors as therapeutics. Crit Care Med. 2002;30:S281–7.
Hayakawa M, Katabami K, Wada T, Minami Y, Sugano M, Shimojima H, et al. Sivelestat (selective neutrophil elastase inhibitor) improves the mortality rate of sepsis associated with both acute respiratory distress syndrome and disseminated intravascular coagulation patients. Shock. 2010;33:14–8.
Fujino N, Kubo H, Suzuki T, He M, Suzuki T, Yamada M, et al. Administration of a specific inhibitor of neutrophil elastase attenuates pulmonary fibrosis after acute lung injury in mice. Exp Lung Res. 2012;38:28–36.
Hagio T, Nakao S, Matsuoka H, Matsumoto S, Kawabata K, Ohno H, et al. Inhibition of neutrophil elastase activity attenuates complement-mediated lung injury in the hamster. Eur J Pharmacol. 2001;426:131–8.
Steen S, Sjoberg T, Pierre L, Liao Q, Eriksson L, Algotsson L, et al. Transplantation of lungs from a non-heart-beating donor. Lancet. 2001;357:825–9.
Steen S, Liao Q, Wierup PN, Bolys R, Pierre L, Sjoberg T. Transplantation of lungs from non–heart-beating donors after functional assessment ex vivo. Ann Thorac Surg. 2003;76:244–52.
Cypel M, Yeung JC, Keshavjee S. Novel approaches to expanding the lung donor pool: donation after cardiac death and ex vivo conditioning. Clin Chest Med. 2011;32:233–44.
Cypel M, Yeung JC, Liu M, Anraku M, Chen F, Karolak W, et al. Normothermic ex vivo lung perfusion in clinical lung transplantation. N Engl J Med. 2011;364:1431–40.
Erasmus ME, Fernhout MH, Elstrodt JM, Rakhorst G. Normothermic ex vivo lung perfusion of non-heart-beating donor lungs in pigs: from pretransplant function analysis towards a 6-h machine preservation. Transpl Int. 2006;19:589–93.
Cypel M, Yeung JC, Hirayama S, Rubacha M, Fischer S, Anraku M, et al. Technique for prolonged normothermic ex vivo lung perfusion. J Heart Lung Transplant. 2008;27:1319–25.
Aoki T, Tsuchida M, Takekubo M, Saito M, Sato K, Hayashi J. Neutrophil elastase inhibitor ameliorates reperfusion injury in a canine model of lung transplantation. Eur Surg Res. 2005;37:274–80.
Eppinger MJ, Deeb GM, Bolling SF, Ward PA. Mediators of ischemia-reperfusion injury of rat lung. Am J Pathol. 1997;150:1773–84.
Fiser SM, Tribble CG, Long SM, Kaza AK, Cope JT, Laubach VE, et al. Lung transplant reperfusion injury involves pulmonary macrophages and circulating leukocytes in a biphasic response. J Thorac Cardiovasc Surg. 2001;121:1069–75.
Lee WL, Downey GP. Leukocyte elastase: physiological functions and role in acute lung injury. Am J Respir Crit Care Med. 2001;164:896–904.
Kawabata K, Hagio T, Matsuoka S. The role of neutrophil elastase in acute lung injury. Eur J Pharmacol. 2002;451:1–10.
Acknowledgments
The authors gratefully thank Mr. Tetsuo Kawakami for his technical assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Masaaki Harada and other co-authors have no conflict of interest.
Rights and permissions
About this article
Cite this article
Harada, M., Oto, T., Otani, S. et al. A neutrophil elastase inhibitor improves lung function during ex vivo lung perfusion. Gen Thorac Cardiovasc Surg 63, 645–651 (2015). https://doi.org/10.1007/s11748-015-0585-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11748-015-0585-0