Abstract
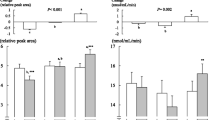
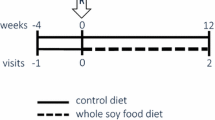
Studies examining the effect of soy protein on cardiovascular disease (CVD) risk factors have not taken advantage of the postprandial state as an adjunct to the fasting lipid profile. The American Heart Association has acknowledged the efficacy of soy protein in reducing CVD risk factors to be limited. We hypothesized that the postprandial state would be more sensitive to any favorable changes associated with consuming soy protein compared with the fasting lipid profile. Furthermore, the presence of isoflavones in soy would enhance this effect. Thirty sedentary males aged 18–30 years were randomly assigned to milk protein (Milk), isoflavone-poor soy (Soy−), or isoflavone-rich soy (Soy+). Usual diets were supplemented with 25 g/day of protein for 28 days. Serum samples were collected before and after supplementation in a fasted state and postprandially at 30, 60, 120, 240, and 360 min after a high-fat, 1,000 kcal shake. Triacylglycerol (TAG), total cholesterol, non-esterified fatty acids, apolipoproteins B-100 and A-I and glucose concentrations were quantified. Fasting concentrations were not different after any protein supplementation. Postprandial TAG and TAG AUC increased after Soy-consumption supporting the postprandial state as a more sensitive indicator of soy ingestion effects on CVD risk factors compared with the fasting lipid profile. Furthermore, the absence of isoflavones in soy protein may have deleterious consequences on purported cardio-protective effects.



Similar content being viewed by others
Abbreviations
- CVD:
-
Cardiovascular disease
- Milk:
-
Milk protein
- Soy−:
-
Isoflavone-poor soy
- Soy+:
-
Isoflavone-rich soy
- TC:
-
Total cholesterol
- TAG:
-
Triacylglycerol
- Apo B-100:
-
Apolipoprotein B-100
- Apo A-I:
-
Apolipoprotein A-I
- FDA:
-
Food and Drug Administration
- VLDL:
-
Very-low density lipoprotein
- AUC:
-
Area under the curve
- BMI:
-
Body mass index
- HDL-C:
-
High density lipoprotein cholesterol constituent
- NEFA:
-
Non-esterified fatty acids
- ANOVA:
-
Analysis of variance
- LDL-C:
-
Low density lipoprotein cholesterol constituent
- RLP-C:
-
Remnant-like particle-cholesterol
- TRL:
-
Triacylglycerol rich lipoprotein
- LDL:
-
Low density lipoprotein
- HDL:
-
High density lipoprotein
- LCAT:
-
Lecithin:cholesterol acyltransferase
References
(2002) National Cholesterol Education Program (NCEP) Expert Panel on detection, evaluation, and treatment of high blood cholesterol in adults (Adult Treatment Panel III). Third report of the national cholesterol education program (NCEP) Expert Panel on detection, evaluation, and treatment of high blood cholesterol in adults (Adult Treatment Panel III) final report. Circulation 106:3143–3421
Adiels M, Packard C, Caslake MJ, Stewart P, Soro A, Westerbacka J, Wennberg B, Olofsson S-O, Taskinen M-R, Borén J (2005) A new combined multicompartmental model for apolipoprotein B-100 and triglyceride metabolism in VLDL subfractions. J Lipid Res 46:58–67
Allen JK, Becker DM, Kwiterovich PO, Lindenstruth KA, Curtis C (2007) Effect of soy protein-containing isoflavones on lipoproteins in postmenopausal women. Menopause 14:106–114
Anderson JW, O’Neal DS, Riddell-Mason S, Floore TM, Dillom DW, Oeltgen PR (1995) Postprandial serum glucose, insulin, and lipoprotein responses to high- and low-fiber diets. Metabolism 44:848–854
Bansal S, Buring JE, Rifai N, Mora S, Sacks FM, Ridker PM (2007) Fasting compared with nonfasting triglycerides and risk of cardiovascular events in women. J Am Med Assoc 298:309–316
Caldwell CR, Britz SJ, Mirecki RM (2005) Effect of temperature, elevated carbon dioxide, and draught during seed development on the isoflavone content of dwarf soybean [Glycine max (L.) Merrill] grown in controlled environments. J Agric Food Chem 53:1125–1129
Cederroth CR, Nef S (2009) Soy, phytoestrogens and metabolism: a review. Mol Cell Endocrinol 304:30–42
Cohn JS (2006) Postprandial lipemia and remnant lipoproteins. Clin Lab Med 26:773–786
Cohn JS, McNamara JR, Cohn SD, Ordovas JM, Schaefer EJ (1988) Postprandial plasma lipoprotein changes in human subjects of different ages. J Lipid Res 29:469–479
Collaboration APCS (2004) Serum triglycerides as a risk factor for cardiovascular diseases in the Asia-Pacific Region. Circulation 110:2678–2686
Coward L, Smith M, Kirk M, Barnes S (1998) Chemical modification of isoflavones in soy foods during cooking and processing. Am J Clin Nutr 68:1486s–1491s
De Bruin TWA, Brouwer B, Trip ML, Jansen H, Erkelens DW (1993) Different postprandial metabolism of olive oil and soybean oil: a possible mechanism of the high-density lipoprotein conserving effect of olive oil. Am J Clin Nutr 58:477–483
Dewell A, Hollenbeck PL, Hollenbeck CB (2006) Clinical review: a critical evaluation of the role of soy protein and isoflavone supplementation in the control of plasma cholesterol concentrations. J Clin Endocrinol Metab 91:772–780
Freiberg JJ, Tybjaerg-Hansen A, Jensen JS, Nordestgaard BG (2008) Nonfasting triglycerides and risk of ischemic stroke in the general population. J Am Med Assoc 300:2142–2152
Friedman M, Brandon DL (2001) Nutritional and health benefits of soy proteins. J Agric Food Chem 49:1069–1086
Gardner CD, Messina M, Kiazand A, Morris JL, Franke AA (2007) Effect of two types of soy milk and dairy milk on plasma lipids in hypercholesterolemic adults: a randomized trial. J Am Coll Nutr 26:669–677
Ginsberg HN, Jones J, Blaner WS, Thomas A, Karmally W, Fields L, Blood D, Beg MD (1995) Association of postprandial triglyceride and retinyl palmitate responses with newly diagnosed exercise-induced myocardial ischemia in middle-aged men and women. Arterioscler Thromb Vasc Biol 15:1829–1838
Hanson LN, Engelman HM, Alekel DL, Schalinske KL, Kohut ML, Reddy MB (2006) Effects of soy isoflavones and phytate on homocysteine, C-reactive protein, and iron status in postmenopausal women. Am J Clin Nutr 84:774–780
Harris WS, Connor WE, Alam N, Illingworth DR (1988) Reduction of postprandial triglyceridemia in humans by dietary n-3 fatty acids. J Lipid Res 29:1451–1460
Ho SC, Chen YM, Ho SS, Woo JL (2007) Soy isoflavone supplementation and fasting serum glucose and lipid profile among postmenopausal Chinese women: a double-blind, randomized, placebo-controlled trial. Menopause 14:905–912
Hooper L, Kroon PA, Rimm EB, Cohn JS, Harvey I, Le Cornu KA, Ryder JJ, Hall WL, Cassidy A (2008) Flavonoids, flavonoid-rich foods, and cardiovascular risk: a meta-analysis of randomized controlled trials. Am J Clin Nutr 88:38–50
Kannel WB, Vasan RS (2009) Triglycerides as vascular risk factors: new epidemiologic insights. Curr Opin Cardiol 24:345–350
Karpe F, Steiner G, Uffelman K, Olivecrona T, Hamsten A (1994) Postprandial lipoprotein and progression of coronary atherosclerosis. Atherosclerosis 106:83–97
Kolovou GD, Anagnostopoulou KK, Daskalopoulou SS, Mikhailidis DP, Cokkinos DV (2005) Clinical relevance of postprandial lipaemia. Curr Med Chem 12:1931–1945
Langsted A, Freiberg JJ, Nordestgaard GB (2008) Fasting and nonfasting lipid levels: influence of normal food intake on lipids, lipoproteins, apolipoproteins, and cardiovascular risk prediction. Circulation 118:2047–2056
Le N-A, Walter MF (2007) The role of hypertriglyceridemia in atherosclerosis. Curr Atheroscler Rep 9:110–115
Levy E, Roy CC, Goldstein R, Bar-On H, Ziv E (1991) Metabolic fate of chylomicrons obtained from rats maintained on diets varying in fatty acid composition. J Am Coll Nutr 10:69–78
Lovati MR, Manzoni C, Corsini A, Granata A, Frattinin R, Fumagalli R, Sirtori CR (1992) Low density lipoprotein receptor activity is modulated by soybean globulins in cell culture. J Nutr 122:1971–1978
Lu LW, Anderson K (1998) Sex and long-term soy diets affect the metabolism and excretion of soy isoflavones in humans. Am J Clin Nutr 68:1500s–1504s
Ma Y, Chiriboga D, Olendzki BC, Nicolosi R, Merriam PA, Ockene IS (2005) Effect of soy protein containing isoflavones on blood lipids in moderately hypercholesterolemic adults: a randomized controlled trial. J Am Coll Nutr 24:275–285
Matthan NR, Jalbert SM, Ausman LM, Kuvin JT, Karas RH, Lichenstein AH (2007) Effect of soy protein from differently processed products on cardiovascular disease risk factors and vascular endothelial function in hypercholesterolemic subjects. Am J Clin Nutr 85:960–966
McVeigh BL, Dillingham BL, Lampe JW, Duncan AM (2006) Effect of soy protein varying in isoflavone content on serum lipids in healthy young men. Am J Clin Nutr 83:244–251
Mora S, Rifai N, Buring JE, Ridker PM (2008) Fasting compared with nonfasting lipids and apolipoproteins for predicting incident cardiovascular events. Circulation 118:993–1001
Muesing RA, Griffin P, Mitchell P (1995) Corn oil and beef tallow elicit different postprandial responses in triglycerides and cholesterol, but similar changes in constituents of high-density lipoprotein. J Am Coll Nutr 14:53–60
Nordestgaard BG, Benn M, Schnohr P, Tybjaerg-Hansen A (2007) Nonfasting triglycerides and risk of myocardial infarction, ischemic heart disease, and death in men and women. J Am Med Assoc 298:299–308
O’Keefe JH, Bell DSH (2007) Postprandial hyperglycemia/hyperlipidemia (postprandial dysmetabolism) is a cardiovascular risk factor. Am J Cardiol 100:899–904
Otvos JD, Jeyarajah EJ, Cromwell WC (2002) Measurement issues related to lipoprotein heterogeneity. Am J Cardiol 90:22i–29i
Parks EJ (2001) Recent findings in the study of postprandial lipemia. Curr Atheroscler Rep 3:462–470
Patsch JR, Miesenbock G, Hopferwieser T, Muhlberger V, Knapp E, Dunn JK, Gotto AM, Patsch W (1992) Relation of triglyceride metabolism and coronary disease. Arterioscler Thromb 12:1336–1345
Pischon T, Girman CJ, Sacks FM, Rifai N, Stampfer MJ, Rimm EB (2005) Non-high-density lipoprotein cholesterol and apolipoprotein B in the prediction of coronary heart disease in men. Circulation 112:3375–3383
Potter SM (1998) Soy protein and cardiovascular disease: the impact of bioactive components in soy. Nutr Rev 56:231–235
Reynolds K, Chin A, Lees KA, Nguyen A, Bujnowski D, He J (2006) A meta-analysis of the effect of soy protein supplementation on serum lipids. Am J Cardiol 98:633–640
Sacks FM (2006) The apolipoprotein story. Atheroscler Suppl 7:23–27
Sacks FM, Lichenstein A, Horn LV, Harris W, Kris-Etherton P, Winston M (2006) Soy protein, isoflavones, and cardiovascular health: an American Heart Association Science Advisory for health professionals from the Nutrition Committee. Circulation 113:1034–1044
Santo AS, Cunningham AM, Alhassan S, Browne RW, Burton H, Leddy JJ, Grandjean PW, Horvath SM, Horvath PJ (2008) NMR analysis of lipoprotein particle size does not increase sensitivity to the effect of soy protein on CVD risk when compared with the traditional lipid profile. Appl Physiol Nutr Metab 33:489–500
Setchell K (1998) Phytoestrogens: the biochemistry, physiology, and implications for human health of soy isoflavones. Am J Clin Nutr 68:1333–1346
Sharret AR, Chambless LE, Heiss G, Paton CC, Patsch W (1995) Association of postprandial triglyceride and retinyl palmitate responses with asymptomatic carotid artery atherosclerosis in middle-aged men and women. Arterioscler Thromb Vasc Biol 15:2122–2129
Shige H, Ishikawa T, Higashi K, Yamashita T, Tomiyasu K, Yoshida H, Hosoai H, Ito T, Nakajima K, Ayaori M, Yonemura A, Suzukawa M, Nakamura H (1998) Effects of soy protein isolate (SPI) and casein on the postprandial lipemia in normolipidemic men. J Nutr Sci Vitaminol 44:113–127
Sirtori CR, Calabresi L, Franceschini G (1999) Recombinant apolipoproteins for the treatment of vascular diseases. Atherosclerosis 142:29–40
Slavin JL, Karr SC, Hutchins AM, Lampe JW (1998) Influence of soybean processing, habitual diet, and soy dose on urinary isoflavonoid excretion. Am J Clin Nutr 68:1492s–1495s
Sniderman AD, Furberg CD, Keech A, JERv Lennep, Frohlich J, Jungner I, Walldius G (2003) Apolipoproteins versus lipids as indices of coronary risk and as targets for statin treatment. Lancet 361:777–780
Stalenhoef AFH, Graaf Jd (2008) Association of fasting and nonfasting serum triglycerides with cardiovascular disease and the role of remnant-like lipoproteins and small dense LDL. Curr Opin Lipidol 19:355–361
Taku K, Umegaki K, Sato Y, Endoh K, Watanabe S (2007) Soy isoflavones lower serum total and LDL cholesterol in humans: a meta-analysis of 11 randomized controlled trials. Am J Clin Nutr 85:1148–1156
Thorp A, Howe PRC, Mori TA, Coates AM, Buckley JD, Hodgson J, Mansour J, Meyer BJ (2008) Soy food consumption does not lower LDL cholesterol in either equol or nonequol producers. Am J Clin Nutr 88:298–304
Torres N, Torre-Villalvazo I, Tovar AR (2006) Regulation of lipid metabolism by soy protein and its implication in diseases mediated by lipid disorders. J Nutr Biochem 17:365–373
Van Heek M, Zilversmit DB (1990) Postprandial lipemia and lipoprotein lipase in the rabbit are modified by olive and coconut oil. Arteriosclerosis 10:421–429
Wangen KE, Duncan AM, Xu X, Kurzer MS (2001) Soy isoflavones improve plasma lipids in normocholesterolemic and mildly hypercholesterolemic postmenopausal women. Am J Clin Nutr 73:225–231
Weintraub MS, Zechner R, Brown A, Eisenberg S, Breslow JL (1988) Dietary polyunsaturated fats of the w-6 and w-3 series reduce postprandial lipoproteins levels. J Clin Invest 82:1884–1893
Weissberg PL, Rudd JH (eds) (2002) Atherosclerotic biology and epidemiology of disease textbook of cardiovascular medicine. Lippincott Williams & Wilkins, Philadelphia
Yu KC-W, Cooper AD (2001) Postprandial lipoproteins and atherosclerosis. Front Biosci 6:d332–d354
Zhan S, Ho SC (2005) Meta-analysis of the effects of soy protein containing isoflavones on the lipid profile. Am J Clin Nutr 81:397–408
Zhuo X-G, Melby MK, Watanabe S (2004) Soy isoflavone intake lowers serum LDL cholesterol: a meta-analysis of 8 randomized controlled trials in humans. J Nutr 134:2395–2400
Zilversmit DB (1979) Atherogenesis: a postprandial phenomenon. Circulation 60:473–485
Acknowledgments
The authors would like to thank The Solae Company (St. Louis, MO, USA) for donating the protein supplements used in this study. Special gratitude is warranted to our colleagues Amy Miracle and Jack Young for their input in the final review of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
S. M. Horvath: deceased.
About this article
Cite this article
Santo, A.S., Santo, A.M., Browne, R.W. et al. Postprandial Lipemia Detects the Effect of Soy Protein on Cardiovascular Disease Risk Compared with the Fasting Lipid Profile. Lipids 45, 1127–1138 (2010). https://doi.org/10.1007/s11745-010-3487-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11745-010-3487-z