Abstract
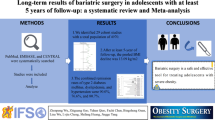
Predisposing factors of new-onset orthostatic intolerance (OI) after bariatric surgery (BS) are unknown. The purpose of this study is to summarize current existing data on new-onset OI after BS. Materials and methods were considered for a search of articles that were published by the 30th of July 2020. A systematic review in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines and in line with the protocol agreed by all authors was conducted. Of the 604 initially identified articles, four studies were found to match the established criteria and were extracted for eligibility. 83.3% were female. Hypertension, type 2 diabetes mellitus, and obstructive sleep apnea syndrome were the most frequently reported comorbidities. Surgical intervention such as revision, conversion, or reversal was not documented in these studies. Awareness of this issue must be raised due to the possibility of reduced quality of life and the risk of syncope.

Similar content being viewed by others
References
Adams TD, Gress RE, Smith SC, et al. Long-term mortality after gastric bypass surgery. N Engl J Med. 2007;357(8):753–61.
Schauer PR, Bhatt DL, Kirwan JP, et al. Bariatric surgery versus intensive medical therapy for diabetes - 5-year outcomes. N Engl J Med. 2017;376(7):641–51.
Gagner M, Deitel M, Erickson AL, et al. Survey on laparoscopic sleeve gastrectomy (LSG) at the Fourth International Consensus Summit on Sleeve Gastrectomy. Obes Surg. 2013;23(12):2013–7.
Kumar N. Obesity surgery: a word of neurologic caution. Neurology. 2007;68:36–8.
Berger JR. The neurological complications of bariatric surgery. Arch Neurol. 2004;61:1185–9.
Juhasz-Pocsine K, Rudnicki SA, Archer RL, et al. Neurologic complications of gastric bypass surgery for morbid obesity. Neurology. 2007;68:1843–50.
Freeman R, Wieling W, Axelrod FB, et al. Consensus statement on the definition of orthostatic hypotension, neurally mediated syncope and the postural tachycardia syndrome. Auton Neurisci. 2011;161:46–8.
Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ. 2009;339:b2700. https://doi.org/10.1136/bmj.b2700.
Zhang JB, Tamboli RA, Albaugh VL, et al. The incidence of orthostatic intolerance after bariatric surgery. Obes Sci Pract. 2019;6(1):76–83.
Rubinshtein R, Ciubotaru M, Elad H, et al. Severe orthostatic hypotension following weight reduction surgery. Arch Intern Med. 2001;161(17):2145–7.
Billakanty SR, Kligman MD, Kanjwal YM, et al. New-onset orthostatic intolerance following bariatric surgery. Pacing Clin Electrophysiol. 2008;31(7):884–8.
Lascano CA, Szomstein S, Zundel N, et al. Diabetes mellitus-associated diffuse autonomic dysfunction causing debilitating hypotension manifested after rapid weight loss in a morbidly obese patient: case report and review of the literature. Surg Obes Relat Dis. 2005;1(4):443–6.
Welbourn R, Hollyman M, Kinsman R, et al. Bariatric surgery worldwide: baseline demographic description and one-year outcomes from the Fourth IFSO Global Registry Report 2018. Obes Surg. 2019;29(3):782–95.
Lambert E, Sari CI, Dawood T, et al. Sympathetic nervous system activity is associated with obesity-induced subclinical organ damage in young adults. Hypertension. 2010;56(3):351–8.
Scarpellini E, Arts J, Karamanolis G, et al. International consensus on the diagnosis and management of dumping syndrome. Nat Rev Endocrinol. 2020;16(8):448–66.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix. Search Strategy
Appendix. Search Strategy
Our search strategy was performed by utilizing the below words:
Summation of #1-8: #1 ((bariatric [MeSH Terms]) OR (bariatric [Title/Abstract])) AND (((((orthostatic[MeSH Terms]) OR (orthostatic [Title/Abstract])) OR (syncope [MeSH Terms])) OR (syncope [Title/Abstract])) OR (tilt test [Title/Abstract])), #2 ((Neurologic complication [Title/Abstract])) AND ((((((bariatric [MeSH Terms]) OR (bariatric [Title/Abstract])) OR (weight loss [MeSH Terms])) OR (weight loss [Title/Abstract])) OR (gastric bypass [Title/Abstract])) OR (sleeve gastrectomy [Title/Abstract])), #3 ((weight loss [MeSH Terms]) OR (weight loss [Title/Abstract])) AND (((((orthostatic [MeSH Terms]) OR (orthostatic [Title/Abstract])) OR (syncope [MeSH Terms])) OR (syncope [Title/Abstract])) OR (tilt test [Title/Abstract])), #4 ((Sleeve gastrectomy [Title/Abstract])) AND (((((orthostatic [MeSH Terms]) OR (orthostatic [Title/Abstract])) OR (syncope [MeSH Terms])) OR (syncope [Title/Abstract])) OR (tilt test [Title/Abstract])), #5 ((Metabolic surgery [Title/Abstract])) AND (((((orthostatic [MeSH Terms]) OR (orthostatic [Title/Abstract])) OR (syncope [MeSH Terms])) OR (syncope [Title/Abstract])) OR (tilt test [Title/Abstract])), #6 ((gastric bypass [MeSH Terms]) OR (gastric bypass [Title/Abstract])) AND (((((orthostatic [MeSH Terms]) OR (orthostatic [Title/Abstract])) OR (syncope [MeSH Terms])) OR (syncope [Title/Abstract])) OR (tilt test [Title/Abstract])), #7 ((body mass index [MeSH Terms]) OR (body mass index [Title/Abstract])) AND (((((orthostatic [MeSH Terms]) OR (orthostatic [Title/Abstract])) OR (syncope [MeSH Terms])) OR (syncope [Title/Abstract])) OR (tilt test [Title/Abstract])), #8 ((obesity [MeSH Terms]) OR (obesity [Title/Abstract])) AND (((((orthostatic [MeSH Terms]) OR (orthostatic [Title/Abstract])) OR (syncope [MeSH Terms])) OR (syncope [Title/Abstract])) OR (tilt test [Title/Abstract]))
Rights and permissions
About this article
Cite this article
Kermansaravi, M., Chiappetta, S., Lainas, P. et al. Orthostatic Intolerance after Bariatric Surgery: a Systematic Review. OBES SURG 31, 2250–2254 (2021). https://doi.org/10.1007/s11695-021-05266-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-021-05266-4