Abstract
Introduction
Safety of exercise training in relationship with the risk of hypoglycemia post-bariatric surgery is unknown.
Objective
To evaluate the safety and magnitude of changes in blood glucose levels during exercise training following bariatric surgery.
Material and Methods
Twenty-nine severely obese patients undergoing either sleeve gastrectomy (SG) (n = 16) or biliopancreatic diversion with duodenal switch (BPD-DS) (n = 13) were prospectively enrolled. Three months after surgery, patients participated in a 12-week supervised exercise training program, (35-min aerobic training with a 25-min resistance exercises) three times a week. Capillary blood glucose (CBG) levels were measured immediately before and after each exercise session.
Results
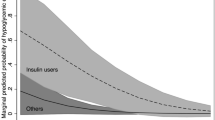
Seven patients (24%) had type 2 diabetes before surgery (mean duration: 10 years); four patients still have type 2 diabetes 3 months post-bariatric surgery. A total of 577 exercise training sessions with CBG monitoring were recorded. Only seven sessions (1.2%) were associated with an episode of asymptomatic hypoglycemia (CBG ≤ 3.9 mmol/L). Patients with type 2 diabetes at baseline showed a larger decrease in CBG with pre-exercise CBG being between 6.1 and 8.0 mmol/L (− 1.6 ± 1.2 vs. − 1.1 ± 0.9 mmol/L, p = 0.02). BPD-DS patients with CBG ≥ 6.1 mmol/L showed higher reduction in CBG following exercise vs. SG patients (− 1.7 ± 1.0 vs. − 1.1 ± 1.1 mmol/L; p < 0.001 and − 4.3 ± 1.0 vs. − 2.2 ± 1.4 mmol/L, p < 0.001, respectively).
Conclusion
Three months after bariatric surgery, exercise training program in patients without and with type 2 diabetes is safe, and is associated with a desirable glycemic profile, with few episodes of asymptomatic hypoglycemia.


Similar content being viewed by others
References
Madsbad S, Dirksen C, Holst JJ. Mechanisms of changes in glucose metabolism and bodyweight after bariatric surgery. Lancet Diabetes Endocrinol. 2014;2(2):152–64.
Hanaire H, Bertrand M, Guerci B, et al. High glycemic variability assessed by continuous glucose monitoring after surgical treatment of obesity by gastric bypass. Diabetes Technol Ther. 2011;13(6):625–30.
Jimenez A, Ceriello A, Casamitjana R, et al. Remission of type 2 diabetes after Roux-en-Y gastric bypass or sleeve gastrectomy is associated with a distinct glycemic profile. Ann Surg. 2015;261(2):316–22.
Kovatchev B, Cobelli C. Glucose variability: timing, risk analysis, and relationship to hypoglycemia in diabetes. Diabetes Care. 2016;39(4):502–10.
Abrahamsson N, Eden EB, Sundbom M, et al. Hypoglycemia in everyday life after gastric bypass and duodenal switch. Eur J Endocrinol. 2015;173(1):91–100.
Marsk R, Jonas E, Rasmussen F, et al. Nationwide cohort study of post-gastric bypass hypoglycaemia including 5,040 patients undergoing surgery for obesity in 1986-2006 in Sweden. Diabetologia. 2010;53(11):2307–11.
Nannipieri M, Belligoli A, Guarino D, et al. Risk factors for spontaneously self-reported postprandial hypoglycemia after bariatric surgery. J Clin Endocrinol Metab. 2016;101(10):3600–7.
Gerstein HC, Miller ME, Byington RP, et al. Effects of intensive glucose lowering in type 2 diabetes. N Engl J Med. 2008;358(24):2545–59.
Whitmer RA, Karter AJ, Yaffe K, et al. Hypoglycemic episodes and risk of dementia in older patients with type 2 diabetes mellitus. JAMA. 2009;301(15):1565–72.
Davis RE, Morrissey M, Peters JR, et al. Impact of hypoglycaemia on quality of life and productivity in type 1 and type 2 diabetes. Curr Med Res Opin. 2005;21(9):1477–83.
Redelmeier DA, Kenshole AB, Ray JG. Motor vehicle crashes in diabetic patients with tight glycemic control: a population-based case control analysis. PLoS Med. 2009;6(12):e1000192.
American Diabetes Association - Standards of Medical Care in Diabetes - 2017. Diabetes Care 40[Supplement 1], S1-S131. 2017.
Coen PM, Goodpaster BH. A role for exercise after bariatric surgery? Diabetes Obes Metab. 2016;18(1):16–23.
Piche ME, Auclair A, Harvey J, et al. How to choose and use bariatric surgery in 2015. Can J Cardiol. 2015;31(2):153–66.
Pournaras DJ, Osborne A, Hawkins SC, et al. Remission of type 2 diabetes after gastric bypass and banding: mechanisms and 2 year outcomes. Ann Surg. 2010;252(6):966–71.
Mechanick JI, Kushner RF, Sugerman HJ, et al. American Association of Clinical Endocrinologists, The Obesity Society, and American Society for Metabolic & Bariatric Surgery medical guidelines for clinical practice for the perioperative nutritional, metabolic, and nonsurgical support of the bariatric surgery patient. Obesity (Silver Spring). 2009;17(Suppl 1):S1–70.
Gaudet-Savard T, Ferland A, Broderick TL, et al. Safety and magnitude of changes in blood glucose levels following exercise performed in the fasted and the postprandial state in men with type 2 diabetes. Eur J Cardiovasc Prev Rehabil. 2007;14(6):831–6.
Seaquist ER, Anderson J, Childs B, et al. Hypoglycemia and diabetes: a report of a workgroup of the American Diabetes Association and the Endocrine Society. Diabetes Care. 2013;36(5):1384–95.
Imran SA, Rabasa-Lhoret R, Ross S. Targets for glycemic control. Can J Diabetes. 2013;37(Suppl 1):S31–4.
Poirier P, Mawhinney S, Grondin L, et al. Prior meal enhances the plasma glucose lowering effect of exercise in type 2 diabetes. Med Sci Sports Exerc. 2001;33(8):1259–64.
Rossetti L, Giaccari A, Barzilai N, et al. Mechanism by which hyperglycemia inhibits hepatic glucose production in conscious rats. Implications for the pathophysiology of fasting hyperglycemia in diabetes. J Clin Invest. 1993;92(3):1126–34.
Aiston S, Andersen B, Agius L. Glucose 6-phosphate regulates hepatic glycogenolysis through inactivation of phosphorylase. Diabetes. 2003;52(6):1333–9.
Larsen JJ, Dela F, Kjaer M, et al. The effect of moderate exercise on postprandial glucose homeostasis in NIDDM patients. Diabetologia. 1997;40(4):447–53.
Martin IK, Katz A, Wahren J. Splanchnic and muscle metabolism during exercise in NIDDM patients. Am J Phys. 1995;269(3 Pt 1):E583–90.
Minuk HL, Vranic M, Marliss EB, et al. Glucoregulatory and metabolic response to exercise in obese noninsulin-dependent diabetes. Am J Phys. 1981;240(5):E458–64.
Larsen JJ, Dela F, Madsbad S, et al. Interaction of sulfonylureas and exercise on glucose homeostasis in type 2 diabetic patients. Diabetes Care. 1999;22(10):1647–54.
Weir GC. A defective beta-cell glucose sensor as a cause of diabetes. N Engl J Med. 1993;328(10):729–31.
Postic C, Shiota M, Magnuson MA. Cell-specific roles of glucokinase in glucose homeostasis. Recent Prog Horm Res. 2001;56:195–217.
Poirier P, Tremblay A, Catellier C, et al. Impact of time interval from the last meal on glucose response to exercise in subjects with type 2 diabetes. J Clin Endocrinol Metab. 2000;85(8):2860–4.
Camastra S, Manco M, Mari A, et al. Beta-cell function in morbidly obese subjects during free living: long-term effects of weight loss. Diabetes. 2005;54(8):2382–9.
Hanefeld M, Fischer S, Julius U, et al. Risk factors for myocardial infarction and death in newly detected NIDDM: the Diabetes Intervention Study, 11-year follow-up. Diabetologia. 1996;39(12):1577–83.
Oberlin DJ, Mikus CR, Kearney ML, et al. One bout of exercise alters free-living postprandial glycemia in type 2 diabetes. Med Sci Sports Exerc. 2014;46(2):232–8.
Lee CJ, Brown TT, Schweitzer M, et al. The incidence and risk factors associated with developing symptoms of hypoglycemia after bariatric surgery. Surg Obes Relat Dis. 2018;14(6):797–802.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Statement of Human Rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Proulx, É., Auclair, A., Piché, ME. et al. Safety of Blood Glucose Response Following Exercise Training After Bariatric Surgery. OBES SURG 28, 3976–3983 (2018). https://doi.org/10.1007/s11695-018-3449-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-018-3449-8