Abstract
Background
The prevalence of obesity is on a continuous rise worldwide, with major studies clearly correlating obesity with the development of chronic metabolic disorders including type 2 diabetes. Bariatric surgery has proven to be beneficial in the management of this condition; however, a limited number of studies exist on its effect on type 1 diabetes.
Objective
The objective of this study is to evaluate the outcome of laparoscopic sleeve gastrectomy for the management of patients with type 1 diabetes (DM1).
Setting
This is a retrospective cohort study conducted in a university hospital and private practice in Kuwait.
Research Design and Methods
Analysis was conducted on 10 patients diagnosed with type 1 diabetes that underwent bariatric surgery from October 2008 until December 2016 at Amiri Hospital and Royale Hayat Hospital, Kuwait. Primary parameters included body mass index (BMI), % excess weight (%EWL) loss at follow-up, glycosylated hemoglobin (A1C), and basal insulin requirements. Total cholesterol readings and fasting blood glucose (FBS) levels were considered secondary outcomes. Statistical analysis of the data was carried out using Statistical Package for the Social Sciences (SPSS) software.
Results
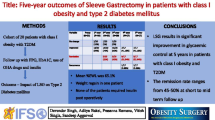
Mean BMI showed a reduction from 41.9 ± 5.4 to 31.4 ± 8.4 kg/m2. Mean %EWL after the follow-up period was 74.4 ± 25.3%. A1C levels failed to show a significant difference 12 months post-op (p = 0.189). Cholesterol levels did not display a significant decrease either (p = 0.447). When it came to insulin requirements, a significant difference was perceived, with the mean number of units of insulin required dropping from 76.6 to 18.2 (p = 0.026). FBS readings also showed a drop from 15.1 ± 3.8 to 7.8 ± 2.9 mmol/L (p = 0.001).
Conclusions
Laparoscopic sleeve gastrectomy resulted in significant weight loss, comorbidity resolution as well as reduction in their insulin doses post-op. However, glycemic control does not seem to show significant improvement in these patients. Larger, more long-term studies are needed to reach a definite conclusion on this topic.

Similar content being viewed by others
References
State of Victoria (1999) Victorian Burden of Disease Study: Morbidity Public Health Division, Department of Human Services Melbourne Victoria, Australia.
Hu FB, Manson JE, Stampfer MJ, et al. Diet, lifestyle, and the risk of type 2 diabetes mellitus in women. N Engl J Med. 2001;345:790–7.
Must A, Spadano J, Coakley EH, et al. The disease burden associated with overweight and obesity. JAMA. 1999;282:1523–9.
Pories WJ, Swanson MS, MacDonald KG, et al. Who would have thought it? An operation proves to be the most effective therapy for adult-onset diabetes mellitus. Ann Surg. 1995;222:339–50. discussion 350-332
Czupryniak L, Wiszniewski M, Szymanski D, et al. Long-term results of gastric bypass surgery in morbidly obese type 1 diabetes patients. Obes Surg. 2010;20:506–8.
Brethauer SA, Aminian A, Rosenthal RJ, et al. Bariatric surgery improves the metabolic profile of morbidly obese patients with type 1 diabetes. Diabet Care. 2014;37:e51–2.
Maraka S, Kudva YC, Kellogg TA, et al. Bariatric surgery and diabetes: implications of type 1 versus insulin-requiring type 2. Obesity. 2015;23(3):552–7. Web
The American Society for Metabolic and Bariatric Surgery.
NDEI.org. Guidelines for Hypoglycemia in Diabetes ADA/Endocrine Society. N.p., n.d. Web. 04 July 2016.
Serban V, Brink S, Timar B, et al. An increasing incidence of type 1 diabetes mellitus in Romanian children aged 0 to 17 years. J Pediatr Endocrinol Metab. 2015;28(3–4):293–8.
Conway B, Miller RG, Costacou T, et al. Adiposity and mortality in type 1 diabetes. Int J Obes. 2009;33:796–805.
Nathan DM. Long-term complications of diabetesmellitus. N Engl JMed. 1993;328:1676–85.
Price SA, Gorelik A, Fourlanos S, et al. Obesity is associated with retinopathy and macrovascular disease in type 1 diabetes. Obes Res Clin Pract. 2014;8:e178–82.
De Block CE, De Leeuw IH, Van Gaal LF. Impact of overweight on chronic microvascular complications in type 1 diabetic patients. Diabetes Care. 2005;28:1649–55.
Kirwan JP, Brethauer SA, Aminian A, et al. Response to comments on Brethauer et al. Bariatric surgery improves the metabolic profile of morbidly obese patients with type 1 diabetes. Diabetes Care. 2014;37:e51–2. Diabetes Care 2014;37:e251
Chillarón JJ, Benaiges D, Mañé L, et al. Obesity and type 1 diabetes mellitus management. Minerva Endocrinol. 2015;40(1):53–60.
Dixon JB, le Roux CW, Rubino F, et al. Bariatric surgery for type 2 diabetes. Lancet. 2012;379:2300–11.
Rubino F, Schauer PR, Kaplan LM, et al. Metabolic surgery to treat type 2 diabetes: clinical outcomes and mechanisms of action. Annu Rev Med. 2010;61:393–411.
Thaler JP, Cummings DE. Minireview: hormonal and metabolic mechanisms of diabetes remission after gastrointestinal surgery. Endocrinology. 2009;150:2518–25.
Blanco J, Jiménez A, Casamitjana R, et al. Relevance of beta-cell function for improved glycemic control after gastric bypass surgery. Surg Obes Relat Dis. 2014;10(1):9–13. quiz 189–90
Chuang J, Zeller MH, Inge T, et al. Bariatric surgery for severe obesity in two adolescents with type 1 diabetes. Pediatrics. 2013;132(4):e1031–4.
Dirksen C, Jacobsen SH, Bojsen-Møller KN, et al. Reduction in cardiovascular risk factors and insulin dose, but no beta-cell regeneration 1 year after Roux-en-Y gastric bypass in an obese patient with type 1 diabetes: a case report. Obes Res Clin Pract. 2013;7(4):e269–74.
Pozzilli P, Guglielmi C, Pronina E, et al. Double or hybrid diabetes associated with an increase in type 1 and type 2 diabetes in children and youths. Pediatr Diabetes. 2007;8(Suppl 9):88–95.
Pozzilli P, Guglielmi C, Caprio S, et al. Obesity, autoimmunity, and double diabetes in youth. Diabetes Care. 2011;34(Suppl 2):S166–70.
Golomb I, Ben David M, Glass A, et al. Long-term metabolic effects of laparoscopic sleeve gastrectomy. JAMA Surg. 2015;150(11):1051. Web.
Robert M, Belanger P, Hould FS, et al. Shouldmetabolic surgery be offered in morbidly obese patients with type I diabetes? Surg Obes Relat Dis. 2014; doi:10.1016/j.soard.2014.12.016.
Buchwald H, Estok R, Fahrbach K, et al. Weight and type 2 diabetes after bariatric surgery: systematic review and meta-analysis. Am J Med. 2009;122:248–56. e245
Sjostrom L, Lindroos AK, Peltonen M, et al. Swedish obese subjects study scientific group. Lifestyle, diabetes, and cardiovascular risk factors 10 years after bariatric surgery. N Engl J Med. 2004;351:2683–93.
Aminian A, Zelisko A, Kirwan JP, et al. Exploring the impact of bariatric surgery on high density lipoprotein. Surg Obes Relat Dis. 2015;11:238–47.
Schauer PR, Bhatt DL, Kirwan JP, et al. STAMPEDE investigators. Bariatric surgery versus intensive medical therapy for diabetes—3-year outcomes. N Engl J Med. 2014;370:2002–13.
Mingrone G, Panunzi S, De Gaetano A, et al. Bariatric surgery versus conventional medical therapy for type 2 diabetes. N Engl J Med. 2012;366:1577–85.
Ikramuddin S, Korner J, Lee WJ, et al. Rouxen-Y gastric bypass vs intensive medical management for the control of type 2 diabetes, hypertension, and hyperlipidemia: the diabetes surgery study randomized clinical trial. JAMA. 2013;309:2240–9.
Dixon JB, O’Brien PE, Playfair J, et al. Adjustable gastric banding and conventional therapy for type 2 diabetes: a randomized controlled trial. JAMA. 2008;299:316–23.
Adams TD, Davidson LE, Litwin SE, et al. Health benefits of gastric bypass surgery after 6 years. JAMA. 2012;308:1122–31.
Brethauer SA, Aminian A, Romero-Talamás H, et al. Can diabetes be surgically cured? Long-term metabolic effects of bariatric surgery in obese patients with type 2 diabetes mellitus. Ann Surg. 2013;258:628–36. discussion 636–637
Aminian A, Daigle CR, Romero-Talamás H, et al. Risk prediction of complications of metabolic syndrome before and 6 years after gastric bypass. Surg Obes Relat Dis. 2014;10:576–82.
Romero-Talamás H, Aminian A, Corcelles R, et al. Psoriasis improvement after bariatric surgery. Surg Obes Relat Dis. 2014;10:1155–9.
Romero-Talamás H, Daigle CR, Aminian A, et al. The effect of bariatric surgery on gout: a comparative study. Surg Obes Relat Dis. 2014;10:1161–5.
Hussain A, Mahmood H, El-Hasani S. Can Roux-en-Y gastric bypass provide a lifelong solution for diabetes mellitus? Can J Surg. 2009;52(6):E269–75.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study. Additional informed consent does not apply.
Rights and permissions
About this article
Cite this article
Al Sabah, S., Al Haddad, E., Muzaffar, T.H. et al. Laparoscopic Sleeve Gastrectomy for the Management of Type 1 Diabetes Mellitus. OBES SURG 27, 3187–3193 (2017). https://doi.org/10.1007/s11695-017-2777-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-017-2777-4