Abstract
Background
Obesity is a worldwide prevalent disease and is an underlying factor of non-alcoholic fatty liver disease (NAFLD). It has been understood as a chronic inflammatory state, being associated with the production of adipokines. The aim of this study was to analyze the levels of adipokines in the serum, visceral, and subcutaneous fat and to compare them with hepatic histopathology in morbidly obese patients.
Methods
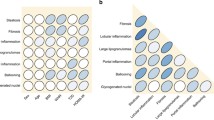
This is a cross-sectional observational study, which analyzed the findings of liver biopsy in patients undergoing bariatric surgery and who had performed analysis of adipokines mRNA expression (adiponectin—ADIPOQ, leptin—LEP, and resistin—RETN) in subcutaneous and visceral adipose tissue and circulating adipokines in serum. Liver biopsies performed were evaluated according to Kleiner criteria.
Results
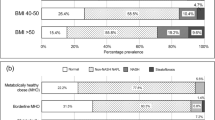
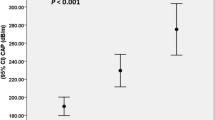
The study analyzed 25 patients undergoing bariatric surgery. The sample was composed exclusively of women. There was a predominance of NAFLD, with 21 patients (84%) with intrahepatic fat accumulation. Twelve patients presented non-alcoholic steatohepatitis (NASH). Glycated hemoglobin levels (HbA1c) were elevated in NASH patients. ADIPOQ levels were directly correlated with high-density lipoprotein (HDL) cholesterol levels and inversely correlated with triglycerides and total cholesterol. LEP levels showed an inverse relationship with the degree of steatosis, and RETN levels showed an inverse relationship with fibrosis stages.
Conclusion
Serum LEP levels were reduced in the presence of increased levels of intrahepatic fat, and serum levels of RETN were diminished in the presence of NASH. HbA1c levels were higher in the presence of NASH, indirectly reflecting insulin resistance. Moreover, ADIPOQ levels were related to blood lipid profile.


Similar content being viewed by others
References
Lau DCW, Douketis JD, Morrison KM, et al. 2006 Canadian clinical practice guidelines on the management and prevention of obesity in adults and children. Can Med Assoc J. 2007;176(8):S1–13.
Vernon G, Baranova A, Younossi ZM. Systematic review: the epidemiology and natural history of non-alcoholic fatty liver disease and non-alcoholic steatohepatitis in adults. Aliment Pharmacol Ther. 2011;34(3):274–85.
WGO Global Guidelines. Nonalcoholic fatty liver disease and nonalcoholic steatohepatitis. World Gastroenterol Organ Guidel. 2012.
Losekann A, Weston A, de Mattos A, et al. Non-alcoholic steatohepatitis (NASH): risk factors in morbidly obese patients. Int J Mol Sci. 2015;16(10):25552–9.
Losekann A, Weston AC, Carli LA, et al. Nonalcoholic fatty liver disease in severe obese patients, subjected to bariatric surgery. Arq Gastroenterol. 2013;50(4):285–9.
Rinella ME. Nonalcoholic fatty liver disease a systematic review. JAMA. 2015;169(2):170.
Frayn KN, Arner P, Yki-Jarvinen H. Fatty acid metabolism in adipose tissue, muscle and liver in health and disease. Essays Biochem. 2006;42:89–103.
Deng Y, Scherer PE. Adipokines as novel biomarkers and regulators of the metabolic syndrome. Ann N Y Acad Sci. 2010;1212:1–25.
Petta S, Gastaldelli A, Rebelos E, et al. Pathophysiology of non alcoholic fatty liver disease. Int J Mol Sci. 2016;17(12):2082.
Li X-L, Sui J-Q, Lu L-L, et al. Gene polymorphisms associated with non-alcoholic fatty liver disease and coronary artery disease: a concise review. Lipids Health Dis Lipids in Health and Disease. 2016;15(1):53.
Jarrar MH, Baranova A, Collantes R, et al. Adipokines and cytokines in non-alcoholic fatty liver disease. Aliment Pharmacol Ther. 2008;27(5):412–21.
Abenavoli L, Peta V. Role of adipokines and cytokines in non-alcoholic fatty liver disease. Rev Recent Clin Trials. 2014;9(3):134–40.
Buechler C, Wanninger J, Neumeier M. Adiponectin, a key adipokine in obesity related liver diseases. World J Gastroenterol. 2011;17(23):2801–11.
Stojsavljević S, Gomerčić Palčić M, Virović Jukić L, et al. Adipokines and proinflammatory cytokines, the key mediators in the pathogenesis of nonalcoholic fatty liver disease. World J Gastroenterol. 2014;20(48):18070–91.
Tsochatzis EA, Papatheodoridis GV, Archimandritis AJ. Adipokines in nonalcoholic steatohepatitis: from pathogenesis to implications in diagnosis and therapy. Mediat Inflamm. 2009;2009:831670.
Kleiner DE, Brunt EM, Van Natta M, et al. Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology. 2005;41(6):1313–21.
Targher G, Bertolini L, Rodella S, et al. Associations between plasma adiponectin concentrations and liver histology in patients with nonalcoholic fatty liver disease. Clin Endocrinol. 2006;64(6):679–83.
Karbowska J, Kochan Z. Role of adiponectin in the regulation of carbohydrate and lipid metabolism. In: J Physiol Pharmacol. 2006. p. 103–13.
Lee B, Shao J. Adiponectin and lipid metabolism in skeletal muscle. Acta Pharm Sin B. 2012;2(4):335–40.
Baratta R, Amato S, Degano C, Farina MG, Patanè G, Vigneri R, et al. Adiponectin relationship with lipid metabolism is independent of body fat mass: evidence from both cross-sectional and intervention studies. In: J Clin Endocrinol Metabol. 2004. p. 2665–71.
Bugianesi E, Pagotto U, Manini R, et al. Plasma adiponectin in nonalcoholic fatty liver is related to hepatic insulin resistance and hepatic fat content, not to liver disease severity. J Clin Endocrinol Metab. 2005;90(6):3498–504.
Pagano C, Soardo G, Esposito W, et al. Plasma adiponectin is decreased in nonalcoholic fatty liver disease. Eur J Endocrinol. 2005;152(1):113–8.
Polyzos SA, Mantzoros CS. Adiponectin as a target for the treatment of nonalcoholic steatohepatitis with thiazolidinediones: a systematic review. Metabolism. 2016;65(9):1297–306.
Spranger J, Kroke A, Möhlig M, et al. Adiponectin and protection against type 2 diabetes mellitus. Lancet. 2003;361(9353):226–8.
Argentou M, Tiniakos DG, Karanikolas M, et al. Adipokine serum levels are related to liver histology in severely obese patients undergoing bariatric surgery. Obes Surg. 2009;19(9):1313–23.
Abenavoli L, DI Renzo L, Guzzi PH, et al. Non-alcoholic fatty liver disease severity, central fat mass and adinopectin: a close relationship. Clujul Med. 2015;88(4):489–93.
Baranova A, Gowder SJ, Schlauch K, et al. Gene expression of leptin, resistin, and adiponectin in the white adipose tissue of obese patients with non-alcoholic fatty liver disease and insulin resistance. Obes Surg. 2006;16(9):1118–25.
Jamali R, Arj A, Razavizade M, et al. Prediction of nonalcoholic fatty liver disease via a novel panel of serum adipokines. Medicine (Baltimore). 2016a;95(5):e2630.
Considine RV, Sinha MK, Heiman ML, et al. Serum immunoreactive-leptin concentrations in normal-weight and obese humans. N Engl J Med. 1996;334(5):292–5.
Lönnqvist F, Arner P, Nordfors L, et al. Overexpression of the obese (Ob) gene in adipose tissue of human obese subjects. Nat Med. 1995;1(9):950–3.
Tsochatzis E, Papatheodoridis GV, Archimandritis AJ. The evolving role of leptin and adiponectin in chronic liver diseases. Am J Gastroenterol. 2006;101(11):2629–40.
Ikejima K, Takei Y, Honda H, et al. Leptin receptor-mediated signaling regulates hepatic fibrogenesis and remodeling of extracellular matrix in the rat. Gastroenterology. 2002;122(5):1399–410.
Ikejima K, Honda H, Yoshikawa M, et al. Leptin augments inflammatory and profibrogenic responses in the murine liver induced by hepatotoxic chemicals. Hepatology. 2001;34(2):288–97.
Chitturi S, Farrell G, Frost L, et al. Serum leptin in NASH correlates with hepatic steatosis but not fibrosis: a manifestation of lipotoxicity? Hepatology. 2002;36(2):403–9.
Tsochatzis E, Papatheodoridis GV, Hadziyannis E, et al. Serum adipokine levels in chronic liver diseases: association of resistin levels with fibrosis severity. Scand J Gastroenterol. 2008;43(9):1128–36.
Polyzos SA, Aronis KN, Kountouras J, et al. Circulating leptin in non-alcoholic fatty liver disease: a systematic review and meta-analysis. Diabetologia. 2016;59(1):30–43.
Polyzos SA, Kountouras J, Mantzoros CS. Leptin in nonalcoholic fatty liver disease: a narrative review. Metab Clin Exp. 2015;64:60–78.
Steppan CM, Bailey ST, Bhat S, et al. The hormone resistin links obesity to diabetes. Nature. 2001;409(6818):307–12.
De Luis DA, Terroba MC, Cuellar L, et al. Resistin levels in morbid obese patients following the biliopancreatic diversion surgery. Horm Metab Res. 2011;43(3):205–8.
Aller R, de Luis D, Fernandez L, et al. Influence of insulin resistance and adipokines in the grade of steatosis of nonalcoholic fatty liver disease. Dig Dis Sci. 2008;53(4):1088–92.
Pagano C, Soardo G, Pilon C, et al. Increased serum resistin in nonalcoholic fatty liver disease is related to liver disease severity and not to insulin resistance. J Clin Endocrinol Metab. 2006;91(3):1081–6.
Senates E, Çolak Y, Yesil A, et al. Circulating resistin is elevated in patients with non-alcoholic fatty liver disease and its associated with steatosis, portal inflammation, insulin resistance and no alcoholic steatohepatitis scores. Minerva Med. 2012;53(9):1689–99.
Cengiz C, Ardicoglu Y, Bulut S, et al. Serum retinol-binding protein 4 in patients with nonalcoholic fatty liver disease: does it have a significant impact on pathogenesis? Eur J Gastroenterol Hepatol. 2010;22(7):813–9.
Jamali R, Razavizade M, Arj A, et al. Serum adipokines might predict liver histology findings in non-alcoholic fatty liver disease. World J Gastroenterol. 2016b;22(21):5096–103.
Perseghin G, Lattuada G, De Cobelli F, et al. Serum resistin and hepatic fat content in nondiabetic individuals. J Clin Endocrinol Metab. 2006;91(12):5122–5.
Bekaert M, Verhelst X, Geerts A, et al. Association of recently described adipokines with liver histology in biopsy-proven non-alcoholic fatty liver disease: a systematic review. Obes Rev. 2016;17(1):68–80.
Samaras K, Botelho NK, Chisholm DJ, et al. Subcutaneous and visceral adipose tissue gene expression of serum adipokines that predict type 2 diabetes. Obesity (silver spring). Nat Publ Group. 2010;18(5):884–9.
Blüher M, Fasshauer M, Kralisch S, et al. Regulation of adiponectin receptor R1 and R2 gene expression in adipocytes of C57BL/6 mice. Biochem Biophys Res Commun. 2005;329(3):1127–32.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Statement
This study was submitted to and approved by the Research Ethics Committee of Universidade Federal de Ciências da Saúde de Porto Alegre (UFCSPA) and of Hospital Nossa Senhora da Conceição (HNSC). All participants signed an inform consent form authorizing adipose tissue and blood sample collection previous to surgery procedures and their storage for further studies. These samples were collected for a previous larger study, and their utilization in the present study and collection of information from routine liver biopsies performed during surgery from their medical records was authorized by both institutions.
Rights and permissions
About this article
Cite this article
D’Incao, R.B., Tovo, C.V., Mattevi, V.S. et al. Adipokine Levels Versus Hepatic Histopathology in Bariatric Surgery Patients. OBES SURG 27, 2151–2158 (2017). https://doi.org/10.1007/s11695-017-2627-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-017-2627-4