Abstract
Background
Recent studies have suggested that metabolic surgery reduces cancer risk. This study aims to determine if incident cancer is associated with the extent of weight loss after Roux-en-Y gastric bypass (RYGB).
Methods
Patients at a large tertiary bariatric surgery center were retrospectively reviewed to identify patients with no history of cancer at the time of RYGB. Diagnoses in the electronic health record, a tumor registry, and chart review were used to identify postoperative incident solid organ cancer. The overall incidence of organ cancer was estimated using Kaplan-Meier analysis. The percent total body weight loss (%TWL) in the 48 months after surgery but prior to cancer was compared between those that developed organ cancer versus those that did not using repeated measures linear regression.
Results
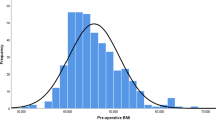
The 2943 patients had a mean age of 45.6 years (SD = 11.1), 81 % were female, and a mean baseline body mass index (BMI) of 47.2 kg/m2 (SD = 7.9). Median follow-up after surgery was 3.8 years (range = [<1, 12]). Incident organ cancer developed and was verified in 54 of the 2943 patients (1.8 %). Kaplan-Meier estimates for cancer at 3, 5, and 10 years postsurgery were 1.3, 2.5, and 4.2 %. After adjusting for age, BMI, sex, diabetes, hypertension, and dyslipidemia, patients that developed organ cancer achieved less weight loss (−1.5 % TWL, 95 % CI = [−2.9 %, −0.1 %], p = 0.034).
Conclusions
Greater weight loss after metabolic surgery may be associated with lower organ cancer risk.



Similar content being viewed by others
References
American Institute of Cancer Research [Internet]. Washington DC: The American Institute of Cancer Research; c1982-2015 [updated 2014; cited 2015 Jan 5]. Available: http://www.aicr.org/cancer-research-update/2014/january_08/cru-report-billion-overweight-obese.html.
Division of Nutrition, Physical Activity, and Obesity [Internet]. Georgia: National Center for Chronic Disease Prevention and Health Promotion, Centers for Disease Control and Prevention; c 2009–2015 [updated 2012; cited 2015 Jan 5]. Available: http://www.cdc.gov/nccdphp/dnpa/obesity/economic_consequences.htm.
Fontaine K, Redden DT, Wang C, et al. Years of life lost due to obesity. JAMA. 2003;289:187–93.
American Institute of Cancer Research [Internet]. Washington DC: The American Institute of Cancer Research; c 1982–2015 [updated 2012; cited 2015 Jan 5]. Available: http://www.aicr.org/assets/docs/pdf/education/aicr-cancer-awareness-report-2012.pdf .
International Agency for Research on Cancer [Internet]. France: International Agency for Research on Cancer; c1965-2015 [updated 2014; cited 2015 Jan 5]. Available: http://www.iarc.fr/en/media-centre/pr/2014/pdfs/pr224_E.pdf .
American Institute of Cancer Research [Internet]. Washington DC: The American Institute of Cancer Research; c 1982–2015 [updated 2012; cited 2015 Jan 5]. Available: http://www.aicr.org/reduce-your-cancer-risk/cancer-prevention/reduce_cancer_by_numbers.html.
Renehan A, Tyson M, Egger M, et al. Body-mass index and incidence of cancer: a systematic review and meta-analysis of prospective observational studies. Lancet. 2008;371:569–78.
Calle E, Rodriguez C, Walker-Thurmond K, et al. Overweight, obesity and mortality from cancer in a prospectively studied cohort of U.S. adults. N Engl J Med. 2003;348:1625–38.
Wolin KY, Carson K, Colditz GA. Obesity and cancer. Oncologist. 2010;15(6):556–65.
Reeves GK, Pirie K, Beral V, et al. Cancer incidence and mortality in relation to body mass index in the million women study: cohort study. BMJ. 2007;335(7630):1134.
DePergola G, Sivestris F. Obesity as a major risk factor for cancer. J Obes. 2013;2013:291546.
Arnold M, Pandeya N, Byrnes G, et al. Global burden of cancer attributable to high body-mass index in 2012: a population-based study. Lancet Oncol. 2014 Nov 26 [cited 2015 Jan 10]: [13 p.]. Available from: http://press.thelancet.com/BMIcancer.pdf .
Whitlock G, Lewington S, Sherliker P, et al. Body-mass index and cause-specific mortality in 900,000 adults: collaborative analyses of 57 prospective studies. Lancet. 2009;373:083–1096.
Ashrafian H, Ahmed K, Rowland SP. Metabolic Surgery and Cancer. Cancer. 2011;117(9):1788–99.
Adams TD, Gress MA, Smith SC, et al. Long-term mortality after gastric bypass surgery. NEJM. 2007;357:753–61.
Christou NV, Sampali JS, Liberman M, et al. Surgery decreases long-term mortality, morbidity, and health care use in morbidly obese patients. Ann Surg. 2004;240(3):416–23.
Sjostrom L, Narbro K, Sjostrom CD, et al. Effects of bariatric surgery on mortality in Swedish obese subjects. N Engl J Med. 2007;357(8):741–52.
Christou N, Lieberman M, Sampalis F, et al. Bariatric surgery reduces cancer risk in morbidly obese patients. Surg Obes Relat Dis. 2008;4(6):691–5.
Adams TD, Stroup AM, Gress RE, et al. Cancer incidence and mortality after gastric bypass surgery. Obesity. 2009;17(4):796–802.
Sjostrom L, Gummesson A, Sjostrom CD, et al. Effects of bariatric surgery on cancer incidence in obese patients in Sweden (Swedish obese study subjects): a prospective, controlled intervention trial. Lancet. 2009;10(7):653–62.
Still CD, Wood GC, Chu X, et al. Clinical factors associated with weight loss outcomes after Roux-en-Y gastric bypass surgery. Obesity. 2014;22(3):888–94.
Wood GC, Chu X, Manney C, et al. An electronic health record-enabled obesity database. BMC Med Inform Decis Mak. 2012;12:45.
International Agency for Research on Cancer [Internet]. France: International Agency for Research on Cancer; c1965-2015 [cited 2015 Jan 10]. Available: http://www.iarc.fr/en/publications/pdfs-online/prev/handbook6.
American Institute of Cancer Research [Internet]. Washington DC: The American Institute of Cancer Research; c 1982–2015 [updated 2007; cited 2015 Jan 10]. Available: http://www.aicr.org/research/research_science_expert_report.html .
Berger NA. Obesity-associated gastrointestinal tract cancer: from beginning to end. Cancer. 2014;120(7):935–9.
Harwood J. The adipocyte as an endocrine organ in the regulation of metabolic homeostasis. Neuropharmacology. 2012;63(1):57–75.
Musso G, Gambino R, Cassader M. Obesity, diabetes, and gut microbiota: the hygiene hypothesis expanded. Diabetes Care. 2010;33:2277–84.
Iyenegar N, Hudis C, Dannenberg A. Obesity and cancer: local and systemic mechanisms. Annu Rev Med. 2015;66:297–309.
Ostlund MP, Lu YL, Lagergren J. Risk of obesity-related cancer after obesity surgery in a population-based cohort study. Ann Surg. 2010;252(6):972–6.
Derogar M, Hull MA, Kant P, et al. Increased risk of colorectal cancer after obesity surgery. Ann Surg. 2013;258(6):983–8.
Tee MC, Cao Y, Warnock G, et al. Effects of bariatric surgery on oncologic outcomes: a systematic review and meta-analysis. Surg Endosc. 2013;27(12):4449–56.
Afshar S, Kelly SB, Seymour K, Lara J, Woodcock S, Mathers JC. The effects of bariatric surgery on colorectal cancer risk: systematic review and meta-analysis. Obes Surg. 2014;24(10):1793–9.
Van de Laar A, de Caluwe L, Dillemans B. Relative outcome measures for bariatric surgery. Evidence against excess weight loss and excess body mass index loss from a series of laparoscopic Roux-en-Y gastric bypass patients. Obes Surg. 2011;6:763–7.
Renehan A. Bariatric surgery, weight reduction, and cancer prevention. Lancet Oncol. 2009;10(7):640–1.
Acknowledgments
This research was supported by research funds from the Geisinger Health System and the National Institutes of Health (grant no. DK072488 to C. D. Still and G.C. Wood).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors. For this type of study, formal consent is not required.
Informed Consent
Does not apply.
Rights and permissions
About this article
Cite this article
Hunsinger, M.A., Wood, G.C., Still, C. et al. Maximizing Weight Loss After Roux-en-Y Gastric Bypass May Decrease Risk of Incident Organ Cancer. OBES SURG 26, 2856–2861 (2016). https://doi.org/10.1007/s11695-016-2206-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-016-2206-0