Abstract
Background
Experts recommend physical activity (PA) to optimize bariatric surgery (BS) results. However, evidence on the effect of PA before BS is missing. The aim of this study was to assess the impact of adding a Pre-Surgical Exercise Training (PreSET) to an interdisciplinary lifestyle intervention on physical fitness, quality of life, PA barriers, and anthropometric parameters of subjects awaiting BS.
Methods
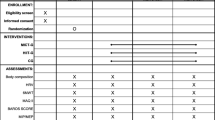
Thirty candidates for BS (43.2 ± 9.2 years, 47.5 ± 8.1 kg/m2) have been randomized in two groups: one group following the PreSET (endurance and strength training) and another receiving usual care. Before and after 12 weeks, we assessed physical fitness with a battery of tests (symptom-limited exercise test, 6-min walk test (6MWT), sit-to-stand test, half-squat test, and arm curl test), quality of life with the laval questionnaire, and PA barriers with the physical exercise belief questionnaire.
Results
One control group subject abandoned the study. Subjects in the PreSET group participated in 60.0 % of the supervised exercise sessions proposed. Results showed significant improvements in the 6MWT (17.4 ± 27.2 vs. −16.4 ± 42.4 m; p = 0.03), half-squat test (17.1 ± 17.9 vs. −0.9 ± 14.5 s; p = 0.05), arm curl repetitions (4.8 ± 2.3 vs. 1.0 ± 4.1; p = 0.01), social interaction score (10.7 ± 12.5 vs. −2.1 ± 11.0 %; p = 0.02), and embarrassment (−15.6 ± 10.2 vs. −3.1 ± 17.8 %; p = 0.02) in completers (n = 8) compared to the non-completers (n = 21). No significant difference between groups in BMI and other outcomes studied was observed after the intervention.
Conclusions
Adding a PreSET to an individual lifestyle counselling intervention improved physical fitness, social interactions, and embarrassment. Post-surgery data would be interesting to confirm these benefits on the long term.

Similar content being viewed by others
References
Sjostrom L. Review of the key results from the Swedish Obese Subjects (SOS) trial—a prospective controlled intervention study of bariatric surgery. J Intern Med. 2013;273(3):219–34.
Mechanick JI, Youdim A, Jones DB, et al. Clinical practice guidelines for the perioperative nutritional, metabolic, and nonsurgical support of the bariatric surgery patient—2013 update: cosponsored by American Association of Clinical Endocrinologists, The Obesity Society, and American Society for Metabolic & Bariatric Surgery. Obesity. 2013;21:S1–27.
King WC, Hsu JY, Belle SH, et al. Pre- to postoperative changes in physical activity: report from the longitudinal assessment of bariatric surgery-2. Surg Obes Relat Dis. 2012;8(5):522–32.
Larsen JK, Geenen R, van Ramshorst B, et al. Binge eating and exercise behavior after surgery for severe obesity: a structural equation model. Int J Eat Disord. 2006;39(5):369–75.
Wiklund M, Olsén MF, Willén C. Physical activity as viewed by adults with severe obesity, awaiting gastric bypass surgery. Physioth Res Int. 2011;16(3):179–86.
Bond DS, Evans RK, DeMaria E, et al. Physical activity and quality of life improvements before obesity surgery. Am J Health Behav. 2006;30(4):422–34.
Wouters EJ, Larsen JK, Zijlstra H, et al. Physical activity after surgery for severe obesity: the role of exercise cognitions. Obes Surg. 2011;21(12):1–6.
Baillot A, Audet M, Baillargeon JP, et al. Impact of physical activity and fitness in class II and III obese individuals: a systematic review. Obes Rev. 2014;15(9):721–39.
Bond DS, Thomas JG, King WC, et al. Exercise improves quality of life in bariatric surgery candidates: results from the Bari-Active trial. Obesity (Silver Spring). 2015;23(3):536–42.
Baillot A, Mampuya WM, Comeau E, et al. Feasibility and impacts of supervised exercise training in subjects with obesity awaiting bariatric surgery: a pilot study. Obes Surg. 2013;23(7):882–91.
Gagnon C, Brown C, Couture C, et al. A cost-effective moderate-intensity interdisciplinary weight-management programme for individuals with prediabetes. Diabetes Metab. 2011;37(5):410–8.
Bruce RA, Blackmon JR, Jones JW, et al. Exercising testing in adult normal subjects and cardiac patients. Pediatrics. 1963;32(SUPPL):742–56.
Gibbons RJ, Balady GJ, Bricker JT, et al. ACC/AHA 2002 guideline update for exercise testing: summary article. A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Update the 1997 Exercise Testing Guidelines). J Am Coll Cardiol. 2002;40(8):1531–40.
American College of Sports Medicine. Guidelines for exercise testing and prescription. 8th ed Baltimore Williams & Wilkinson. 2010.
Stegen S, Derave W, Calders P, et al. Physical fitness in morbidly obese patients: effect of gastric bypass surgery and exercise training. Obes Surg. 2011;21(1):61–70.
ATS statement: guidelines for the six-minute walk test. Am J Respir Crit Care Med. 2002;166(1):111-7.
Borg G. Perceived exertion as an indicator of somatic stress. Scand J Rehabil Med. 1970;2(2):92–8.
Therrien F, Marceau P, Turgeon N, et al. The laval questionnaire: a new instrument to measure quality of life in morbid obesity. Health Qual Life Outcomes. 2011;9:66.
US Department of Health and Human Services Barriers to Being Physically Active Quiz 1999 http://www.cdc.gov/diabetes/ndep/pdfs/8-road-to-health-barriers-quiz-508pdf Accessed January 30, 2015.
Craig CL, Marshall AL, Sjostrom M, et al. International physical activity questionnaire: 12-country reliability and validity. Med Sci Sports Exerc. 2003;35(8):1381–95.
Boneva-Asiova Z, Boyanov MA. Body composition analysis by leg-to-leg bioelectrical impedance and dual-energy X-ray absorptiometry in non-obese and obese individuals. Diabetes Obes Metab. 2008;10(11):1012–8.
Waldburger R, Wilms B, Ernst B, et al. Cardio-respiratory fitness is independently associated with cardio-metabolic risk markers in severely obese women. Exp Clin Endocrinol Diabetes. 2014;122(3):190–4.
Hennis PJ, Meale PM, Hurst RA, et al. Cardiopulmonary exercise testing predicts postoperative outcome in patients undergoing gastric bypass surgery. Br J Anaesth. 2012;109(4):566–71.
Baillot A, Asselin M, Comeau E, et al. Impact of excess skin from massive weight loss on the practice of physical activity in women. Obes Surg. 2013;23(11):1826–34.
Speck RM, Bond DS, Sarwer DB, et al. A systematic review of musculoskeletal pain among bariatric surgery patients: implications for physical activity and exercise. Surg Obes Relat Dis. 2014;10(1):161–70.
Baillot A, Romain AJ, Boisvert-Vigneault K, et al. Effects of lifestyle interventions that include a physical activity component in class II and III obese individuals: a systematic review and meta-analysis. PLoS One. 2015;10(4):e0119017.
Catenacci VA, Wyatt HR. The role of physical activity in producing and maintaining weight loss. Nat Clin Pract Endocrinol Metab. 2007;3(7):518–29.
King NA, Horner K, Hills AP, et al. Exercise, appetite and weight management: understanding the compensatory responses in eating behaviour and how they contribute to variability in exercise-induced weight loss. Br J Sports Med. 2012;46(5):315–22.
Evans EM, Saunders MJ, Spano MA, et al. Body-composition changes with diet and exercise in obese women: a comparison of estimates from clinical methods and a 4-component model. Am J Clin Nutr. 1999;70(1):5–12.
Rosa Fortin MM, Brown C, Ball GD, et al. Weight management in Canada: an environmental scan of health services for adults with obesity. BMC Health Serv Res. 2014;14:69.
Acknowledgments
The investigators would like to thank Vicki Lebrun and Anouk Landry, kinesiologists; Marie-Michèle Rosa-Fortin, researcher assistant; and the students of Université de Sherbrooke (Canada) involved in the project (Gabrielle Lebel, Rachel Lapointe, Alexandrine Boucher, Sofia Vasquez) for help with the supervised exercise training and data collection.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Informed consent was obtained from all individual participants included in the study. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Conflict of Interest
The authors declare that they have no conflict of interest.
Grant Information
This study was funded by the Canadian Institutes of Health Research (CIHR, Grant No. OPB-131592). AB is the recipient of a scholarship from the Department of Medicine of Université de Sherbrooke. MFL is the recipient of salary awards from the Fonds de recherche du Québec-Santé (FRQ-S). The Research Center of the Centre hospitalier universitaire de Sherbrooke is a FRQ-S-funded research center.
Rights and permissions
About this article
Cite this article
Baillot, A., Mampuya, W.M., Dionne, I.J. et al. Impacts of Supervised Exercise Training in Addition to Interdisciplinary Lifestyle Management in Subjects Awaiting Bariatric Surgery: a Randomized Controlled Study. OBES SURG 26, 2602–2610 (2016). https://doi.org/10.1007/s11695-016-2153-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-016-2153-9