Abstract
Background
Evidence suggests obesity-related social stigma and impairment in work function may be the two most detrimental quality of life (QOL) factors to overall well-being among patients seeking weight loss surgery (WLS); whether the relative importance of QOL factors varies across patient sex and race/ethnicity is unclear.
Methods
We interviewed 574 patients seeking WLS at two centers. We measured patient’s health utility (preference-based well-being measure) as determined via standard gamble scenarios assessing patients’ willingness to risk death to achieve weight loss or perfect health. Multivariable models assessed associations between patients’ utility and five weight-related QOL domains stratified by gender and race: social stigma, self-esteem, physical function, public distress (weight stigma), and work life.
Results
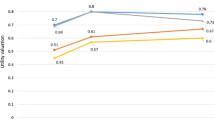
Depending on patients’ sex and race/ethnicity, mean utilities ranged from 0.85 to 0.91, reflecting an average willingness to assume a 9–15 % risk of death to achieve their most desired health/weight state. After adjustment, African Americans (AAs) reported higher utility than Caucasians (+0.054, p = 0.03), but utilities did not vary significantly by sex. Among Caucasian and AA men, impairment in physical functioning was the most important factor associated with diminished utility; social stigma was also a leading factor for Caucasian men. Among Caucasian women, self-esteem and work function appeared equally important. Social stigma was the leading contributor to utility among AA women; QOL factors did not appear as important among Hispanic patients.
Conclusion
AAs reported higher utilities than Caucasian patients. Individual QOL domains that drive diminished well-being varied across race/ethnicity and sex.


Similar content being viewed by others
References
Clinical guidelines on the identification, evaluation, and treatment of overweight and obesity in adults—the evidence report. National Institutes of Health. Obes Res. 1998;6 Suppl 2:51S-209S.
Calle EE, Rodriguez C, Walker-Thurmond K, et al. Overweight, obesity, and mortality from cancer in a prospectively studied cohort of U.S. adults. N Engl J Med. 2003;348(17):1625–38.
Resnick HE, Valsania P, Halter JB, et al. Differential effects of BMI on diabetes risk among black and white Americans. Diabetes Care. 1998;21(11):1828–35.
Stevens J. Impact of age on associations between weight and mortality. Nutr Rev. 2000;58(5):129–37.
Puhl R, Brownell KD. Bias, discrimination, and obesity. Obes Res. 2001;9(12):788–805.
White MA, O'Neil PM, Kolotkin RL, et al. Gender, race, and obesity-related quality of life at extreme levels of obesity. Obes Res. 2004;12(6):949–55.
Gerland P, Masquelier B, Helleringer S, et al. Maternal mortality estimates. Lancet. 2014;384(9961):2211.
The medium and the message of Ebola. Lancet. 2014;384(9955):1641.
Shepard DS. Cost-effectiveness in health and medicine. By M.R. Gold, J.E. Siegel, L.B. Russell, and M.C. Weinstein (eds). New York: Oxford University Press, 1996. J Ment Health Policy Econ. 1999;2(2):91–2.
Wee CC, Hamel MB, Apovian CM, et al. Expectations for weight loss and willingness to accept risk among patients seeking weight loss surgery. JAMA Surg. 2013;148(3):264–71.
Wee CC, Davis RB, Huskey KW, et al. Quality of life among obese patients seeking weight loss surgery: the importance of obesity-related social stigma and functional status. J Gen Intern Med. 2013;28(2):231–8. PMCID: 3614124.
Wee CC, Jones DB, Davis RB, et al. Understanding patients' value of weight loss and expectations for bariatric surgery. Obes Surg. 2006;16(4):496–500.
Kolotkin RL, Crosby RD, Kosloski KD, et al. Development of a brief measure to assess quality of life in obesity. Obes Res. 2001;9(2):102–11.
Kolotkin RL, Head S, Hamilton M, et al. Assessing impact of weight on quality of life. Obes Res. 1995;3(1):49–56.
Wee CC, Davis RB, Huskey KW, Jones DB, Hamel MB. Quality of life among obese patients seeking weight loss surgery: the role of obesity-related social stigma and functional status. J Gen Intern Med. 2012.
Tengs TO, Wallace A. One thousand health-related quality-of-life estimates. Med Care. 2000;38(6):583–637.
Consequences of a competitive research culture. Lancet. 2014;384(9960):2084.
Nguyen NT, Paya M, Stevens CM, et al. The relationship between hospital volume and outcome in bariatric surgery at academic medical centers. Ann Surg. 2004;240(4):586–93. discussion 93–4.
Santry HP, Gillen DL, Lauderdale DS. Trends in bariatric surgical procedures. JAMA. 2005;294(15):1909–17.
Fettich KC, Chen EY. Coping with obesity stigma affects depressed mood in African-American and white candidates for bariatric surgery. Obesity. 2012;20(5):1118–21.
Acknowledgments
The study was funded by a grant from the National Institutes of Health (R01DK073302, PI Wee). Dr. Wee is also supported by a NIH Midcareer Mentorship Award (K24DK087932). The funder had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; and preparation, review, or approval of the manuscript. Ms. Huskey had full access to the data and takes responsibility for the integrity and accuracy of the data.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The study was funded by a grant from the National Institutes of Health (R01DK073302, PI Wee). Dr. Wee is also supported by a NIH Midcareer Mentorship Award (K24DK087932).
Conflict of Interest
Dr. Apovian reports grants from National Institutes of Health, from Myos, from Aspire Bariatrics, and from GI Dynamics; grants and personal fees from Amylin, from Sanofi-Aventis, from Orexigen, and from Takeda; personal fees from Merck, from Johnson & Johnson, from Arena, from Nutrisystem, from Zafgen, from EnteroMedics, and from NovoNordisk for work unrelated to the current project. All other authors declare they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Wee, C.C., Davis, R.B., Jones, D.B. et al. Sex, Race, and the Quality of Life Factors Most Important to Patients’ Well-Being Among Those Seeking Bariatric Surgery. OBES SURG 26, 1308–1316 (2016). https://doi.org/10.1007/s11695-015-1956-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-015-1956-4