Abstract
Background
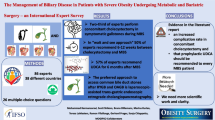
Bariatric surgery is currently the treatment of choice for those patients with severe obesity, but the procedure of choice is not clearly established. We describe weight loss and nutritional parameters in severely obese patients after biliopancreatic diversion for 10 years of follow-up.
Methods
Patients were followed by the same multidisciplinary team, and data are shown for 10 years. Bariatric Analysis and Reporting Outcome System (BAROS) questionnaire, data regarding the evolution of obesity-related diseases, and nutritional parameters are reported.
Results
Two hundred ninety-nine patients underwent biliopancreatic diversion, 76.1 % women, initial BMI 50.1 kg/m2 (7.2). Weight loss was maintained throughout 10 years with EWL% around 65 % and EBMIL% around 70 %. More than 80 % of the patients showed EWL higher than 50 %. Blood pressure, glucose metabolism, and lipid profile clearly improved after surgery. Mean nutritional parameters remained within the normal range during follow-up. Protein malnutrition affected less than 4 % and anemia up to 16 %. Fat-soluble vitamin levels decreased along the time, with vitamin D deficiency in 61.5 % of patients. No significant differences were found either in nutritional parameters or weight loss regarding gastrectomy or gastric preservation, or common limb length longer or shorter than 55 cm
Conclusions
Biliopancreatic diversion is an effective surgical procedure in terms of weight loss, quality of life, and evolution of obesity-related diseases. Nutritional deficiencies are less frequent than feared for a malabsorptive procedure, but must be taken into account, especially for fat-soluble vitamins.
Similar content being viewed by others
References
Buchwald H, Estok R, Fahrbach K, et al. Weight and type 2 diabetes after bariatric surgery: systematic review and meta-analysis. Am J Med. 2009;122(3):248–56. doi:10.1016/j.amjmed.2008.09.041.
Topart P, Becouarn G, Salle A. Five-year follow-up after biliopancreatic diversion with duodenal switch. Surg Obes Relat Dis. 2011;7(2):199–205.
Gracia JA, Martínez M, Elia M, et al. Obesity surgery results depending on technique performed: long-term outcome. Obes Surg. 2009;19(4):432–8. doi:10.1007/s11695-008-9762-x.
Skroubis G, Kouri N, Mead N, et al. Long-term results of a prospective comparison of Roux-en-Y gastric bypass versus a variant of biliopancreatic diversion in a non-superobese population (BMI 35-50 kg/m(2)). Obes Surg. 2014;24(2):197–204. doi:10.1007/s11695-013-1081-1.
Mechanick JI, Youdim A, Jones DB, et al. American Association of Clinical Endocrinologists; Obesity Society, American Society for Metabolic & Bariatric Surgery. Clinical practice guidelines for the perioperative nutritional, metabolic, and nonsurgical support of the bariatric surgery patient—2013 update: cosponsored by American Association of Clinical Endocrinologists, The Obesity Society, and American Society for Metabolic & Bariatric Surgery. Obesity (Silver Spring). 2013;21 Suppl 1:S1–27. doi:10.1002/oby.20461.
Mann JP, Jakes AD, Hayden JD et al. Systematic review of definitions of failure in revisional bariatric surgery. Obes Surg. 2014.
Oria HE, Moorehead MK. Bariatric Analysis and Reporting Outcome System (BAROS). Obes Surg. 1998;8:487–99.
Moorehead MK, Ardelt-Gattinger E, Lechner H, et al. The validation of the Moorehead–Ardelt–Gattinger quality of life questionnaire II. Obes Surg. 2003;13:684–92.
Thumham DI, Davies JA, Crump BJ, et al. The use 01 different lipids to express serum tocopherol:lipid ratios for the measurement of vitamin E status. Ann Clin Biochem. 1986;23:514–20.
Ford L, Farr J, Morris P, et al. The value of measuring serum cholesterol-adjusted vitamin E in routine practice. Ann Clin Biochem. 2006;43:130–4.
Ascaso JF, Romero P, Real JT, et al. Insulin resistance quantification by fasting insulin plasma values and HOMA index in a non-diabetic population. Med Clin (Barc). 2001;117(14):530–3.
Marceau P, Biron S, Hould FS, et al. Duodenal switch: long-term results. Obes Surg. 2007;17(11):1421–30.
Moroshko I, Brennan L, O'Brien P. Predictors of attrition in bariatric after care: a systematic review of the literature. Obes Surg. 2012;22(10):1640–7. doi:10.1007/s11695-012-0691-3.
Buchwald H, Estok R, Fahrbach K, et al. Weight and type 2 diabetes after bariatric surgery: systematic review and meta-analysis. Am J Med. 2009;122(3):248-256.e5. doi:10.1016/j.amjmed.2008.09.041.
Skroubis G, Kouri N, Mead N, et al. Long-term results of a prospective comparison of Roux-en-Y gastric bypass versus a variant of biliopancreatic diversion in a non-superobese population (BMI 35-50 kg/m(2)). Obes Surg. 2014;24(2):197–204. doi:10.1007/s11695-013-1081-1.
Marinari GM, Murelli F, Camerini G, et al. A 15-year evaluation of biliopancreatic diversion according to the Bariatric Analysis Reporting Outcome System (BAROS). Obes Surg. 2004;14:325–8.
Dalcanale L, Oliveira CP, Faintuch J, et al. Long-term nutritional outcome after gastric bypass. Obes Surg. 2010;20(2):181–7. doi:10.1007/s11695-009-9916-5.
Mason EE, Hesson WW. Informed consent for obesity surgery. Obes Surg. 1998;8:419–28.
Scopinaro N. Thirty-five years of biliopancreatic diversion: notes on gastrointestinal physiology to complete the published information useful for a better understanding and clinical use of the operation. Obes Surg. 2012;22(3):427–32. doi:10.1007/s11695-011-0554-3.
Avinoah E, Ovnat A, Charuzi I. Nutritional status years after Roux-En-Y gastric bypass surgery. Surgery. 1992;111:137–42.
Buffington C, Walker B, Cowan Jr GS, et al. Vitamin D deficiency in the morbidly obese. Obes Surg. 1993;3:421–4.
Chapin BL, LeMar HJ, Knodel DH, et al. Secondary hyperparathyroidism following biliopancreatic diversion. Arch Surg. 1996;131:1048–52.
Marceau P, Hould FS, Simard S, et al. Biliopancreatic diversion with duodenal switch. World J Surg. 1998;22:947–54.
Alvarez-Leite JI. Nutrient deficiencies secondary to bariatric surgery. Curr Opin Clin Nutr Metab Care. 2004;7:569–75.
Vazquez C, Morejon E, Muñoz C, et al. Repercusión nutricional de la cirugía bariátrica segúntécnica de Scopinaro: análisis de 40 casos. Nutr Hosp. 2003;18:189–93.
Berger JR. The neurological complications of bariatric surgery. Arch Neurol. 2004;61:1185–9.
Brolin RE, Gorman JH, Gorman RC, et al. Are vitamin B12 and folate deficiencies clinically important after Roux-en-Y gastric bypass? J Gastrointest Surg. 1998;2:436–42.
Crea N, Pata G, Di Betta E, et al. Long-term results of biliopancreatic diversion with or without gastric preservation for morbid obesity. Obes Surg. 2011;21(2):139–45. doi:10.1007/s11695-010-0333-6.
Vidal P, Ramón JM, Goday A, et al. Lack of adherence to follow-up visits after bariatric surgery: reasons and outcome. Obes Surg. 2014;24(2):179–83. doi:10.1007/s11695-013-1094-9.
Topart P, Becouarn G, Sallé A, et al. Biliopancreatic diversion requires multiple vitamin and micronutrient adjustments within 2 years of surgery. Surg Obes Relat Dis. 2014. doi:10.1016/j.soard.2014.02.007.
Conflict of Interest
Ballesteros-Pomar MD, González de Francisco T, Urioste-Fondo A, González-Herraez L, Calleja-Fernández A, Vidal-Casariego A, Simó-Fernández V, and Cano-Rodríguez I declare no conflict of interest. For this type of study formal consent is not required
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ballesteros-Pomar, M.D., González de Francisco, T., Urioste-Fondo, A. et al. Biliopancreatic Diversion for Severe Obesity: Long-Term Effectiveness and Nutritional Complications. OBES SURG 26, 38–44 (2016). https://doi.org/10.1007/s11695-015-1719-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-015-1719-2