Abstract
Background
The present study aimed to identify the implications for the mother and the newborn in pregnancies occurring after the bariatric surgery.
Methods
The present retrospective, exploratory cohort study was conducted to analyze the implications for the mother and the newborn in women of childbearing age (10 to 49 years) who became pregnant after undergoing bariatric surgery in Maringá, Paraná, Brazil, during the period from 1999 through 2008.
Results
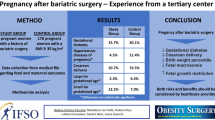
The study identified 32 women with the following characteristics: the majority of the women were Caucasian, slightly more than half were living with a partner, had some higher education, and most of them were without surgical complications. In addition, the mean weight loss post-surgery was 44.09 lbs, with an average interval of 40 months between the surgery and the pregnancy, with improvement of various comorbidities post-surgery. Conversely, they presented more neuropsychiatric disorders, post-surgery anemia, and higher prevalence of cesarean delivery. The majority of children were born at term with normal birth weight and no history of anemia. Hospitalization was required for 36.58% of the post-surgery pregnant women, while 17.07% of such cases required blood transfusion due to anemia. Lastly, there were fewer pregnancy-related hypertension cases than before the surgery.
Conclusions
Pregnancy after bariatric surgery has proven to be safe for both the mother and the newborn. The newborn birth weight was not compromised even though some of the pregnant women were anemic.
Similar content being viewed by others
References
Allison DB, Fontaine KR, Manson JE, et al. Annual deaths attributable to obesity in the United States. JAMA. 1999;282:1530–8.
World Health Organization. Obesity and overweight. Fac Sheet n. 311. Update February 2011. Available at: http://www.who.int/mediacentre/factsheets/fs311/en/. Accessed 2011 (Feb 06).
Ogden CL, Carroll MD, Curtin LR, et al. Prevalence of overweight and obesity in the United States. 1999–2004. JAMA. 2006;295:1549–55.
American College of Obstetricians and Gynecologists. ACOG Committee Opinion 315: obesity in pregnancy. Obstet Gynecol. 2005;106:671–5.
Dao T, Kuhn J, Ehmer D, et al. Pregnancy outcomes after gastric-bypass surgery. Am J Surg. 2006;192:762–6.
Geloneze B, Pareja JC. Cirurgia bariátrica no paciente diabético. Rev da ABESO. 2006;28. Available at: http://www.abeso.org.br/pagina/127/cirurgia-bariatrica-i-%E2%80%93-dr.-bruno-geloneze.shtml. Accessed 2008 (Mar 10).
Lima JG, Nobrega LHC, Mesquita JB, et al. Gestação após gastroplastia para tratamento de obesidade mórbida: série de casos e revisão da literatura. Rev Bras Ginecol Obstet. 2006;28(2):107–11.
Buchwald H. Consensus conference statement bariatric surgery for morbid obesity: health implications for patients, health professionals, and third-party payers. Surg Obes Relat Dis. 2005;1:271–381.
Buchwald H, Avidor Y, Braunwald E, et al. Bariatric surgery: a systematic review and meta-analysis. JAMA. 2004;292:1724–37.
Pope GD, Birkmeyer JD, Finlayson SR. National trends in utilization and in-hospital outcomes of bariatric surgery. J Gastrointest Surg. 2002;6:855–60.
Beard JH, Bell RL, Dufty AJ. Reproductive considerations and pregnancy after bariatric surgery: current evidence and recommendations. Obes Surg. 2008;8:1023–7.
WHO. World Health Organization. Global database on body mass index. BMI classification. Available at: http://apps.who.int/bmi/index.jsp?introPage=intro_3.html. Accessed 2009 (Aug 24).
Halls SB. About arithmetic formulas for calculating ideal body weight. Disponível em www.halls.md/ideal-weight/devine.htm. Accessed 2009 (Aug 24).
Institute of Medicine. National Academy of Sciences. Subcommittee on Nutritional Status and Weight Gain During Pregnancy. Nutrition during Pregnancy. Part I: Weight gain. Washington: National Academy Press. 1990;5 p.
Organizacion Panamericana de la Salud. Manual de la classificación estadística internacional de enfermedadestraumatismos causas de defunción9ª revisión. 1975;1:835–1978 (OMS—Publicación Científica no 353).
Ramos JLA. Avaliação do crescimento intra-uterino por medidas antropométricas do recém-nascido. São Paulo Tese (Doutorado) Faculdade de Medicina, Universidade de São Paulo. 1983. 180 p.
IBGE—Instituto Brasileiro de Geografia e Estatística. Censo Demográfico 2000. MINISTÉRIO DO PLANEJAMENTO, ORÇAMENTO E GESTÃO. Características gerais da amostra: cor ou raça. Disponível em: http://www.ibge.gov.br/home/estatistica/populacao/censo2000/populacao/cor_raca_Censo2000.pdf. Accessed 2009 (Oct 10).
Sociedade Brasileira de Cirurgia Bariátrica e Metabólica. Índice de Penetração de Obesidade no Brasil, 2007. Disponivel em http://www.sbcb.org.br/asbcbm_pesquisa_obesidade_2007.php. Accessed 2009 (Aug 13).
Costa MCO, Santos CAST, Sobrinho CN, et al. Gravidez na adolescência: associação de variáveis sociodemográficas e biomédicas materna com resultado neonatal. feira de santana—Bahia. Rev Baiana de Saude Pública. 2005;29(2):300–12.
Garrido Junior AB. Cirurgia em obesos mórbidos: experiência pessoal. Arq Bras Endocrinol Metabol. 2000;44:106–10.
Melo SMD'A, Vasconcelos FAR, Melo VA, et al. Cirurgia bariátrica: existe necessidade de internação em unidade de terapia intensiva? Rev bras ter intensiva. 2009;21:162–8.
Cendan JC, Abu-aouf D, Gabrielli A, et al. Utilization of intensive care resources in bariatric surgery. Obes Surg. 2005;15:1247–51.
Sheiner E, Balaban E, Dreiher J, et al. Pregnancy in patients following different types of bariatric surgeries. Obes Surg. 2009;19:1286–92.
Fantuch J, Dias CGD, Fazio ES. Pregnancy nutritional indices and birth weight after Roux-en-Y gastric bypass. Obes Surg. 2009;19:583–9.
Wittgrove AC, Jester L, Wittgrove P, Clark GW. Pregnancy following gastric bypass for morbid obesity. Obes Surg. 1998;8:461–6.
Poitou BC, Ciangura C, Coupaye M, et al. Nutritional deficiency after gastric bypass: diagnosis, prevention, treatment. Diab Metab. 2007;33:13–24.
Sakala C. Medically unnecessary cesarean section births: introduction to a symposium. Soc Sci Med. 1993;37(10):1117–98.
Sheiner E, Levy A, Silverberg D, et al. Pregnancy after bariatric surgery is not associated with adverse perinatal outcome. Am J Obstet Gynecol. 2004;190:1335–40.
Antonio MARGM, Zanolli ML, Carniel EF, et al. Fatores associados ao peso insuficiente ao nascimento. Rev Assoc Méd Bras. 2009;55(2):153–7.
Marceau P, Kaufman D, Biron S, et al. Outcome of pregnancies after biliopancreatic diversion. Obes Surg. 2004;14(3):318–24.
Wax JR, Cartin A, Wolff R, et al. Pregnancy following gastric bypass surgery for morbid obesity: maternal and neonatal outcomes. Obes Surg. 2008;18:540–4.
Conflicts of Interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Millene Dell’Agnolo, C., Dalva de Barros Carvalho, M. & Marisa Pelloso, S. Pregnancy After Bariatric Surgery: Implications for Mother and Newborn. OBES SURG 21, 699–706 (2011). https://doi.org/10.1007/s11695-011-0363-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-011-0363-8